User login
Flexibility, innovation key to practice management during pandemic
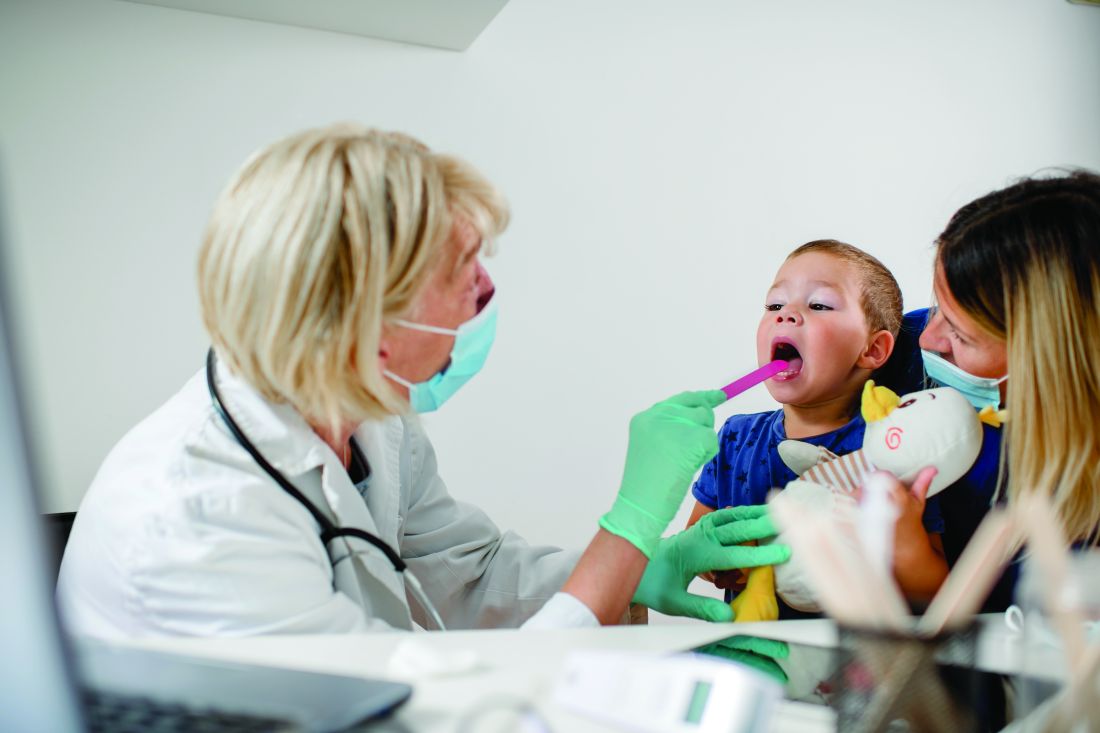
Practice management is the responsibility of every pediatrician, and leadership is more important than ever in a crisis like the COVID-19 pandemic.
“Ultimately you have a critical role in ensuring that your practice remains sustainable so that you can continue to deliver great care,” Sue Kressly, MD, a retired pediatrician from Warrington, Pa., said at the virtual annual meeting of the American Academy of Pediatrics. “None of us escaped some impact of the COVID crisis, and many of us are going to experience lasting change.”
Dr. Kressly and Suzanne Berman, MD, a pediatrician in central Tennessee, presented a live online session on how the pandemic is affecting practices and how pediatricians can effectively address those challenges.
Three ways a crisis impacts practices
“When a practice experiences a crisis, it really exposes what your practice is made of, for better or for worse,” Dr. Berman said. “The COVID crisis has been profound and broad and long enough to really stress the core tensile strength of practices along at least three axes.” Those are staffing, financial health, and partnerships.
It’s a normal human response to enter survival mode during a crisis, so staff management becomes more important than ever. Some things to consider are whether you have a truly collaborative team culture in your practice and whether you’re really listening to the staff’s struggles and suggestions.
“Staffing challenges can be very difficult,” Dr. Berman said. “Permitting staff to work from home is the single biggest thing you can do when staff needs to self-isolate.”
Financially, most medical practices have adequate cash on hand not to have to pay close attention to the numbers, Dr. Kressly said, but if physicians are looking at their books for the first time during a crisis, they have no way of knowing what their baseline expectations should be or how much to worry about their finances. It’s important to understand your practice’s or department’s budget.
Jesse Hackell, MD, a private practice pediatrician in a suburb of New York City and vice president of the New York AAP Chapter 3, attended the session and appreciated this point on finances.
“In order to provide good quality care to kids, you need to be financially successful because otherwise you’ll close your doors,” Dr. Hackell said in an interview. “It’s making yourself available to be able to provide care.”
Stressors among partners during a crisis arise from responding to the challenges of the crisis, such as who should be impacted by pay cuts or furloughs, how to account for overhead, how to distribute revenue and how to divide the work equitably. Other issues include how to protect higher risk providers fairly and how to shift schedules or case load based on unforeseen events, including quarantining.
“There is no ‘fair’ in a crisis,” Dr. Berman said. “We must use the equity paradigm to be sure everyone has what they need to survive and have the best outcome possible.”
The speakers also discussed the importance of a practice’s situation before the pandemic began, a point that resonated with attendee Jason Terk, MD, a pediatrician who practices in a large pediatric health care system near Fort Worth, Texas.
“Just like the pandemic impacts the health of people in different ways based upon their baseline health, the pandemic impacts practices in different ways based on the practice’s baseline health,” he said in an interview. “If you had good operations, a good culture, good communication and all those other good indicators of practice health before, then you stood a much better chance of surviving the pandemic as a practice than practices that had weaknesses before.”
The size of a practice did not necessarily predict the impact of the crisis, Dr. Berman said. Rather, practices with good patient engagement, active recall programs, and good fiscal planning did better.
Dr. Hackell said. “We had never seen anything like this before,” he said in an interview. “From the start we had no idea what was going to work. Try something and see if it works. If it fails, try something else. We were all operating blind here.”
The focus of most practices in the spring was on well visits, chronic care follow-up, and telehealth. Going into fall and winter, innovation will be necessary to provide appropriate care for all children while keeping in mind that the choices pediatricians make will have long-lasting implications for their staff and patients. The speakers stressed the importance of communication and transparency within the office team and to patients and the community.
Dr. Hackell appreciated the speakers’ point that kids need care, and pediatricians need to meet that need.
“Kids need well care and immunizations, and kids get sick and need sick care,” he said. “Parents need a lot more reassurance during times like this. We need to be able to provide that care and be sure that we do it safely. To give the right care at the right time in the right location is key.”
Making practice adaptations
In balancing risk and access to care, Dr. Kressly described the importance of multiple interventions, including managing some patients out of the office and making physical changes, such as putting in physical barriers and eliminating waiting rooms.
“Many practices are highly focused on PPE [personal protective equipment],” Dr. Kressly said, but even Centers for Disease Control and Prevention guidance emphasizes that PPE is the last line of defense. “There are many things we can do to protect our teams and our patients, and we know that not one single adaption is going to be 100% effective. But like the Swiss cheese model indicates, when you layer all of these efforts on top of one another, many defenses allow for the protection of the majority of people.”
Other changes include restricting office visitors to one per patient, implementing social distancing, requiring visitors to wear masks, and considering alternate locations for visits, including car and parking lot visits.
“No idea is too crazy, and some of the best ideas come from your staff,” Dr. Kressly said. She also recommended asking families where they feel most comfortable meeting.
“Don’t make any assumptions about where they want to be seen, but ask and together decide where the patient can most safely and effectively be given appropriate care,” she said.
Dr. Kressly also noted the new CPT code, 99072, that can be used to bill for “additional supplies, materials, and clinical staff time over and above those usually included in an office visit or other nonfacility service(s), when performed during a public health emergency as defined by law, due to respiratory-transmitted infectious disease.”
Pediatricians should think of ways they can remove barriers to access, such as adjusting no-show cancellation penalties and adjusting practice policies as needed when things change. “Avoid creating a culture where families do not disclose all information for fear of not being seen,” Dr. Kressly said.
A slower pace because of delays and hiccups is also normal at this time, Dr. Berman said. “If you feel like you’re just not as efficient as you were prior to COVID, it’s not just you,” she said. “It’s true. Everyone has to grapple with new things now. It takes longer.”
Things that add time include remote check-in and paperwork, more time to don and doff PPE and disinfect, dealing with technology failures, adjusting to new procedures or policies, and the general mental fatigue of adhering to PPE best practices. Patience is vital during this time, Dr. Berman said.
Several ways to improve efficiency include cutting out unnecessary steps, using standing orders and Advance Beneficiary Notice of Noncoverage (ABNs) for flu vaccinations, keeping credit card numbers on file for contactless payment, and considering the clinical and financial value of lab testing before ordering it.
“Effective triage helps patient satisfaction, access to care, and efficiency of your office workload,” Dr. Kressly said. “Use technology where it’s appropriate, but then add people where it’s needed. Connections to caring people matter even more in a time of crisis.”
The speakers also highlighted the importance of early flu vaccinations.
“One of the single biggest things you can do for value in COVID is to get your flu vaccine numbers up,” Dr. Berman said. “Severely reducing the burden of influenza will help flatten the curve, it will reduce febrile respiratory illness, and it will protect your most fragile patients.”
Two ways to do that include flu clinics and making a strong push for immunizations during the first 8 weeks after getting the vaccines. Dr Berman shared numbers from two practices showing how many more total immunizations were done in the practice that began vaccinating in early August versus early September.
A crisis is an opportunity
The speakers closed on an optimistic note that emphasized the opportunities that can grow out of the challenges presented by the pandemic, a point Dr Terk elaborated on.
“One of the most important things is realizing how we can potentially use a crisis to transform our practices,” Dr. Terk said in the interview. “As had been said before, a crisis is a terrible thing to waste. Those practices that have the gumption to innovate and find different ways to improve the way they provide care are probably going to be in better shape as we go forward.”
Critical to that success is taking risks, he added.
“When you’re innovating, failure has to be something you are permissive of because if you’re risk-averse and failure-averse, you’re not going to have the opportunity to grow and innovate, and this is another opportunity to innovate,” Dr. Terk said.
He also stressed the value of learning from one another. “We need to help each other by sharing our good practices, and on the flip side, be open to learning from each other,” he said. “Those pediatricians who are struggling need to be open-minded and open-hearted to understanding how we can operate our practices better and know that the things we think are barriers we can’t change are probably things we probably haven’t allowed ourselves to think about changing.”
Dr. Kressly and Dr. Berman recommended several specific actions for pediatricians to take:
- Creating a SWOT (Strengths, Weaknesses, Opportunities, and Threats) analysis regarding your practice management response to the pandemic.
- Articulating three goals for improving your understanding or the implementation of management in your practice.
- Creating a working group to identify and implement ways to improve clinical work flow and communication strategies.
“Now is the time to meaningfully address disparities of access to appropriate health care and the impact of social determinants of health,” Dr. Kressly said. It’s also an opportunity to build meaningful relationships with patient families based on trust, science, and “true shared decision-making with health literacy in mind.”
Dr Kressly is the medical director of and owns shares in Office Practicum. Dr. Berman is the assistant medical director of and owns shares in Office Practicum, and is the owner of Script Doctor LLC. Dr. Terk and Dr. Hackell had no relevant financial disclosures.
Practice management is the responsibility of every pediatrician, and leadership is more important than ever in a crisis like the COVID-19 pandemic.
“Ultimately you have a critical role in ensuring that your practice remains sustainable so that you can continue to deliver great care,” Sue Kressly, MD, a retired pediatrician from Warrington, Pa., said at the virtual annual meeting of the American Academy of Pediatrics. “None of us escaped some impact of the COVID crisis, and many of us are going to experience lasting change.”
Dr. Kressly and Suzanne Berman, MD, a pediatrician in central Tennessee, presented a live online session on how the pandemic is affecting practices and how pediatricians can effectively address those challenges.
Three ways a crisis impacts practices
“When a practice experiences a crisis, it really exposes what your practice is made of, for better or for worse,” Dr. Berman said. “The COVID crisis has been profound and broad and long enough to really stress the core tensile strength of practices along at least three axes.” Those are staffing, financial health, and partnerships.
It’s a normal human response to enter survival mode during a crisis, so staff management becomes more important than ever. Some things to consider are whether you have a truly collaborative team culture in your practice and whether you’re really listening to the staff’s struggles and suggestions.
“Staffing challenges can be very difficult,” Dr. Berman said. “Permitting staff to work from home is the single biggest thing you can do when staff needs to self-isolate.”
Financially, most medical practices have adequate cash on hand not to have to pay close attention to the numbers, Dr. Kressly said, but if physicians are looking at their books for the first time during a crisis, they have no way of knowing what their baseline expectations should be or how much to worry about their finances. It’s important to understand your practice’s or department’s budget.
Jesse Hackell, MD, a private practice pediatrician in a suburb of New York City and vice president of the New York AAP Chapter 3, attended the session and appreciated this point on finances.
“In order to provide good quality care to kids, you need to be financially successful because otherwise you’ll close your doors,” Dr. Hackell said in an interview. “It’s making yourself available to be able to provide care.”
Stressors among partners during a crisis arise from responding to the challenges of the crisis, such as who should be impacted by pay cuts or furloughs, how to account for overhead, how to distribute revenue and how to divide the work equitably. Other issues include how to protect higher risk providers fairly and how to shift schedules or case load based on unforeseen events, including quarantining.
“There is no ‘fair’ in a crisis,” Dr. Berman said. “We must use the equity paradigm to be sure everyone has what they need to survive and have the best outcome possible.”
The speakers also discussed the importance of a practice’s situation before the pandemic began, a point that resonated with attendee Jason Terk, MD, a pediatrician who practices in a large pediatric health care system near Fort Worth, Texas.
“Just like the pandemic impacts the health of people in different ways based upon their baseline health, the pandemic impacts practices in different ways based on the practice’s baseline health,” he said in an interview. “If you had good operations, a good culture, good communication and all those other good indicators of practice health before, then you stood a much better chance of surviving the pandemic as a practice than practices that had weaknesses before.”
The size of a practice did not necessarily predict the impact of the crisis, Dr. Berman said. Rather, practices with good patient engagement, active recall programs, and good fiscal planning did better.
Dr. Hackell said. “We had never seen anything like this before,” he said in an interview. “From the start we had no idea what was going to work. Try something and see if it works. If it fails, try something else. We were all operating blind here.”
The focus of most practices in the spring was on well visits, chronic care follow-up, and telehealth. Going into fall and winter, innovation will be necessary to provide appropriate care for all children while keeping in mind that the choices pediatricians make will have long-lasting implications for their staff and patients. The speakers stressed the importance of communication and transparency within the office team and to patients and the community.
Dr. Hackell appreciated the speakers’ point that kids need care, and pediatricians need to meet that need.
“Kids need well care and immunizations, and kids get sick and need sick care,” he said. “Parents need a lot more reassurance during times like this. We need to be able to provide that care and be sure that we do it safely. To give the right care at the right time in the right location is key.”
Making practice adaptations
In balancing risk and access to care, Dr. Kressly described the importance of multiple interventions, including managing some patients out of the office and making physical changes, such as putting in physical barriers and eliminating waiting rooms.
“Many practices are highly focused on PPE [personal protective equipment],” Dr. Kressly said, but even Centers for Disease Control and Prevention guidance emphasizes that PPE is the last line of defense. “There are many things we can do to protect our teams and our patients, and we know that not one single adaption is going to be 100% effective. But like the Swiss cheese model indicates, when you layer all of these efforts on top of one another, many defenses allow for the protection of the majority of people.”
Other changes include restricting office visitors to one per patient, implementing social distancing, requiring visitors to wear masks, and considering alternate locations for visits, including car and parking lot visits.
“No idea is too crazy, and some of the best ideas come from your staff,” Dr. Kressly said. She also recommended asking families where they feel most comfortable meeting.
“Don’t make any assumptions about where they want to be seen, but ask and together decide where the patient can most safely and effectively be given appropriate care,” she said.
Dr. Kressly also noted the new CPT code, 99072, that can be used to bill for “additional supplies, materials, and clinical staff time over and above those usually included in an office visit or other nonfacility service(s), when performed during a public health emergency as defined by law, due to respiratory-transmitted infectious disease.”
Pediatricians should think of ways they can remove barriers to access, such as adjusting no-show cancellation penalties and adjusting practice policies as needed when things change. “Avoid creating a culture where families do not disclose all information for fear of not being seen,” Dr. Kressly said.
A slower pace because of delays and hiccups is also normal at this time, Dr. Berman said. “If you feel like you’re just not as efficient as you were prior to COVID, it’s not just you,” she said. “It’s true. Everyone has to grapple with new things now. It takes longer.”
Things that add time include remote check-in and paperwork, more time to don and doff PPE and disinfect, dealing with technology failures, adjusting to new procedures or policies, and the general mental fatigue of adhering to PPE best practices. Patience is vital during this time, Dr. Berman said.
Several ways to improve efficiency include cutting out unnecessary steps, using standing orders and Advance Beneficiary Notice of Noncoverage (ABNs) for flu vaccinations, keeping credit card numbers on file for contactless payment, and considering the clinical and financial value of lab testing before ordering it.
“Effective triage helps patient satisfaction, access to care, and efficiency of your office workload,” Dr. Kressly said. “Use technology where it’s appropriate, but then add people where it’s needed. Connections to caring people matter even more in a time of crisis.”
The speakers also highlighted the importance of early flu vaccinations.
“One of the single biggest things you can do for value in COVID is to get your flu vaccine numbers up,” Dr. Berman said. “Severely reducing the burden of influenza will help flatten the curve, it will reduce febrile respiratory illness, and it will protect your most fragile patients.”
Two ways to do that include flu clinics and making a strong push for immunizations during the first 8 weeks after getting the vaccines. Dr Berman shared numbers from two practices showing how many more total immunizations were done in the practice that began vaccinating in early August versus early September.
A crisis is an opportunity
The speakers closed on an optimistic note that emphasized the opportunities that can grow out of the challenges presented by the pandemic, a point Dr Terk elaborated on.
“One of the most important things is realizing how we can potentially use a crisis to transform our practices,” Dr. Terk said in the interview. “As had been said before, a crisis is a terrible thing to waste. Those practices that have the gumption to innovate and find different ways to improve the way they provide care are probably going to be in better shape as we go forward.”
Critical to that success is taking risks, he added.
“When you’re innovating, failure has to be something you are permissive of because if you’re risk-averse and failure-averse, you’re not going to have the opportunity to grow and innovate, and this is another opportunity to innovate,” Dr. Terk said.
He also stressed the value of learning from one another. “We need to help each other by sharing our good practices, and on the flip side, be open to learning from each other,” he said. “Those pediatricians who are struggling need to be open-minded and open-hearted to understanding how we can operate our practices better and know that the things we think are barriers we can’t change are probably things we probably haven’t allowed ourselves to think about changing.”
Dr. Kressly and Dr. Berman recommended several specific actions for pediatricians to take:
- Creating a SWOT (Strengths, Weaknesses, Opportunities, and Threats) analysis regarding your practice management response to the pandemic.
- Articulating three goals for improving your understanding or the implementation of management in your practice.
- Creating a working group to identify and implement ways to improve clinical work flow and communication strategies.
“Now is the time to meaningfully address disparities of access to appropriate health care and the impact of social determinants of health,” Dr. Kressly said. It’s also an opportunity to build meaningful relationships with patient families based on trust, science, and “true shared decision-making with health literacy in mind.”
Dr Kressly is the medical director of and owns shares in Office Practicum. Dr. Berman is the assistant medical director of and owns shares in Office Practicum, and is the owner of Script Doctor LLC. Dr. Terk and Dr. Hackell had no relevant financial disclosures.
Practice management is the responsibility of every pediatrician, and leadership is more important than ever in a crisis like the COVID-19 pandemic.
“Ultimately you have a critical role in ensuring that your practice remains sustainable so that you can continue to deliver great care,” Sue Kressly, MD, a retired pediatrician from Warrington, Pa., said at the virtual annual meeting of the American Academy of Pediatrics. “None of us escaped some impact of the COVID crisis, and many of us are going to experience lasting change.”
Dr. Kressly and Suzanne Berman, MD, a pediatrician in central Tennessee, presented a live online session on how the pandemic is affecting practices and how pediatricians can effectively address those challenges.
Three ways a crisis impacts practices
“When a practice experiences a crisis, it really exposes what your practice is made of, for better or for worse,” Dr. Berman said. “The COVID crisis has been profound and broad and long enough to really stress the core tensile strength of practices along at least three axes.” Those are staffing, financial health, and partnerships.
It’s a normal human response to enter survival mode during a crisis, so staff management becomes more important than ever. Some things to consider are whether you have a truly collaborative team culture in your practice and whether you’re really listening to the staff’s struggles and suggestions.
“Staffing challenges can be very difficult,” Dr. Berman said. “Permitting staff to work from home is the single biggest thing you can do when staff needs to self-isolate.”
Financially, most medical practices have adequate cash on hand not to have to pay close attention to the numbers, Dr. Kressly said, but if physicians are looking at their books for the first time during a crisis, they have no way of knowing what their baseline expectations should be or how much to worry about their finances. It’s important to understand your practice’s or department’s budget.
Jesse Hackell, MD, a private practice pediatrician in a suburb of New York City and vice president of the New York AAP Chapter 3, attended the session and appreciated this point on finances.
“In order to provide good quality care to kids, you need to be financially successful because otherwise you’ll close your doors,” Dr. Hackell said in an interview. “It’s making yourself available to be able to provide care.”
Stressors among partners during a crisis arise from responding to the challenges of the crisis, such as who should be impacted by pay cuts or furloughs, how to account for overhead, how to distribute revenue and how to divide the work equitably. Other issues include how to protect higher risk providers fairly and how to shift schedules or case load based on unforeseen events, including quarantining.
“There is no ‘fair’ in a crisis,” Dr. Berman said. “We must use the equity paradigm to be sure everyone has what they need to survive and have the best outcome possible.”
The speakers also discussed the importance of a practice’s situation before the pandemic began, a point that resonated with attendee Jason Terk, MD, a pediatrician who practices in a large pediatric health care system near Fort Worth, Texas.
“Just like the pandemic impacts the health of people in different ways based upon their baseline health, the pandemic impacts practices in different ways based on the practice’s baseline health,” he said in an interview. “If you had good operations, a good culture, good communication and all those other good indicators of practice health before, then you stood a much better chance of surviving the pandemic as a practice than practices that had weaknesses before.”
The size of a practice did not necessarily predict the impact of the crisis, Dr. Berman said. Rather, practices with good patient engagement, active recall programs, and good fiscal planning did better.
Dr. Hackell said. “We had never seen anything like this before,” he said in an interview. “From the start we had no idea what was going to work. Try something and see if it works. If it fails, try something else. We were all operating blind here.”
The focus of most practices in the spring was on well visits, chronic care follow-up, and telehealth. Going into fall and winter, innovation will be necessary to provide appropriate care for all children while keeping in mind that the choices pediatricians make will have long-lasting implications for their staff and patients. The speakers stressed the importance of communication and transparency within the office team and to patients and the community.
Dr. Hackell appreciated the speakers’ point that kids need care, and pediatricians need to meet that need.
“Kids need well care and immunizations, and kids get sick and need sick care,” he said. “Parents need a lot more reassurance during times like this. We need to be able to provide that care and be sure that we do it safely. To give the right care at the right time in the right location is key.”
Making practice adaptations
In balancing risk and access to care, Dr. Kressly described the importance of multiple interventions, including managing some patients out of the office and making physical changes, such as putting in physical barriers and eliminating waiting rooms.
“Many practices are highly focused on PPE [personal protective equipment],” Dr. Kressly said, but even Centers for Disease Control and Prevention guidance emphasizes that PPE is the last line of defense. “There are many things we can do to protect our teams and our patients, and we know that not one single adaption is going to be 100% effective. But like the Swiss cheese model indicates, when you layer all of these efforts on top of one another, many defenses allow for the protection of the majority of people.”
Other changes include restricting office visitors to one per patient, implementing social distancing, requiring visitors to wear masks, and considering alternate locations for visits, including car and parking lot visits.
“No idea is too crazy, and some of the best ideas come from your staff,” Dr. Kressly said. She also recommended asking families where they feel most comfortable meeting.
“Don’t make any assumptions about where they want to be seen, but ask and together decide where the patient can most safely and effectively be given appropriate care,” she said.
Dr. Kressly also noted the new CPT code, 99072, that can be used to bill for “additional supplies, materials, and clinical staff time over and above those usually included in an office visit or other nonfacility service(s), when performed during a public health emergency as defined by law, due to respiratory-transmitted infectious disease.”
Pediatricians should think of ways they can remove barriers to access, such as adjusting no-show cancellation penalties and adjusting practice policies as needed when things change. “Avoid creating a culture where families do not disclose all information for fear of not being seen,” Dr. Kressly said.
A slower pace because of delays and hiccups is also normal at this time, Dr. Berman said. “If you feel like you’re just not as efficient as you were prior to COVID, it’s not just you,” she said. “It’s true. Everyone has to grapple with new things now. It takes longer.”
Things that add time include remote check-in and paperwork, more time to don and doff PPE and disinfect, dealing with technology failures, adjusting to new procedures or policies, and the general mental fatigue of adhering to PPE best practices. Patience is vital during this time, Dr. Berman said.
Several ways to improve efficiency include cutting out unnecessary steps, using standing orders and Advance Beneficiary Notice of Noncoverage (ABNs) for flu vaccinations, keeping credit card numbers on file for contactless payment, and considering the clinical and financial value of lab testing before ordering it.
“Effective triage helps patient satisfaction, access to care, and efficiency of your office workload,” Dr. Kressly said. “Use technology where it’s appropriate, but then add people where it’s needed. Connections to caring people matter even more in a time of crisis.”
The speakers also highlighted the importance of early flu vaccinations.
“One of the single biggest things you can do for value in COVID is to get your flu vaccine numbers up,” Dr. Berman said. “Severely reducing the burden of influenza will help flatten the curve, it will reduce febrile respiratory illness, and it will protect your most fragile patients.”
Two ways to do that include flu clinics and making a strong push for immunizations during the first 8 weeks after getting the vaccines. Dr Berman shared numbers from two practices showing how many more total immunizations were done in the practice that began vaccinating in early August versus early September.
A crisis is an opportunity
The speakers closed on an optimistic note that emphasized the opportunities that can grow out of the challenges presented by the pandemic, a point Dr Terk elaborated on.
“One of the most important things is realizing how we can potentially use a crisis to transform our practices,” Dr. Terk said in the interview. “As had been said before, a crisis is a terrible thing to waste. Those practices that have the gumption to innovate and find different ways to improve the way they provide care are probably going to be in better shape as we go forward.”
Critical to that success is taking risks, he added.
“When you’re innovating, failure has to be something you are permissive of because if you’re risk-averse and failure-averse, you’re not going to have the opportunity to grow and innovate, and this is another opportunity to innovate,” Dr. Terk said.
He also stressed the value of learning from one another. “We need to help each other by sharing our good practices, and on the flip side, be open to learning from each other,” he said. “Those pediatricians who are struggling need to be open-minded and open-hearted to understanding how we can operate our practices better and know that the things we think are barriers we can’t change are probably things we probably haven’t allowed ourselves to think about changing.”
Dr. Kressly and Dr. Berman recommended several specific actions for pediatricians to take:
- Creating a SWOT (Strengths, Weaknesses, Opportunities, and Threats) analysis regarding your practice management response to the pandemic.
- Articulating three goals for improving your understanding or the implementation of management in your practice.
- Creating a working group to identify and implement ways to improve clinical work flow and communication strategies.
“Now is the time to meaningfully address disparities of access to appropriate health care and the impact of social determinants of health,” Dr. Kressly said. It’s also an opportunity to build meaningful relationships with patient families based on trust, science, and “true shared decision-making with health literacy in mind.”
Dr Kressly is the medical director of and owns shares in Office Practicum. Dr. Berman is the assistant medical director of and owns shares in Office Practicum, and is the owner of Script Doctor LLC. Dr. Terk and Dr. Hackell had no relevant financial disclosures.
FROM AAP 2020
New nonhormonal hot flash treatments on the way
researchers told attendees at the virtual North American Menopause Society 2020 Annual Meeting.
“The KNDy [kisspeptin/neurokinin B/dynorphin] neuron manipulation is really exciting and holds great promise for rapid and highly effective amelioration of hot flashes, up to 80%, and improvement in other menopausal symptoms, though we’re still looking at the safety in phase 3 trials,” reported Susan D. Reed, MD, MPH, director of the Women’s Reproductive Health Research Program at the University of Washington, Seattle.
“If we continue to see good safety data, these are going to be the greatest things since sliced bread,” Dr. Reed said in an interview. “I don’t think we’ve seen anything like this in menopause therapeutics in a long time.”
While several nonhormonal drugs are already used to treat vasomotor symptoms in menopausal women with and without breast cancer, none are as effective as hormone treatments.
“For now, the SSRIs, SNRIs [serotonin norepinephrine reuptake inhibitors], and GABAergics are the best frontline nonhormonal options with a moderate effect, and clonidine and oxybutynin are effective, but we see more side effects with these,” Dr. Reed said. She noted the importance of considering patients’ mood, sleep, pain, sexual function, weight gain, overactive bladder, blood pressure, and individual quality of life (QOL) goals in tailoring those therapies.
But women still need more nonhormonal options that are at least as effective as hormonal options, Dr. Reed said. Some women are unable to take hormonal options because they are at risk for blood clots or breast cancer.
“Then there’s preference,” she said. “Sometimes people don’t like the way they feel when they take hormones, or they just don’t want hormones in their body. It’s absolutely critical to have these options available for women.”
Nanette F. Santoro, MD, a professor of ob.gyn. at the University of Colorado at Denver, Aurora, who was not involved in the presentation, said in an interview that physicians may not always realize the extent to which vasomotor symptoms interfere with women’s daily lives.
“They have an eroding effect on QOL that is not appreciated sometimes,” she said. Though hot flashes eventually subside in most women, others may continue to experience them into their 70s, when hormonal therapies can begin causing more harm than benefit.
“It goes underappreciated that, for a proportion of women, hot flashes will never go away, and they’re just as bad [as] when they were in their 50s,” Dr. Santoro said. “They need to be treated, and the nonhormonal treatments do not work for everybody.”
Promising KNDy therapeutics
Autopsy studies of postmenopausal women revealed that a complex of neurons in the hypothalamus was “massively hypertrophied” and sits right next to the thermoregulatory center of the brain, Dr. Reed explained.
The complex produces three types of molecules: kisspeptin (a neuropeptide), neurokinin B (a neuropeptide), and dynorphin (a kappa opioid), collectively referred to as the KNDy. The KNDy neural complex is located in the same place as the majority of hormone receptors in the arcuate nucleus, a collection of nerve cells in the hypothalamus.
The current hypothesis is that the KNDy neurons, which communicate with each other, become hyperactivated and cause hot flashes by spilling over to and triggering the thermoregulatory center next door. NKB (kisspeptin and neurokinin B) agonists activate KNDy neurons and dynorphin agonists inactivate KNDy, so the expectation is that NKB antagonists or dynorphin agonists would stop hot flashes.
Indeed, research published in 2015 showed that women taking kappa agonists experienced fewer hot flashes than women in the placebo group. However, no peripherally restricted kappa agonists are currently in clinical trials, so their future as therapeutics is unclear.
Right now, three different NK antagonists are in the pipeline for reducing vasomotor symptoms: MLE 4901 (pavinetant) and ESN364 (fezolinetant) are both NK3R antagonists, and NT-814 is a dual NK1R/NK3R antagonist. All three of these drugs were originally developed to treat schizophrenia.
Phase 2 clinical trials of pavinetant were discontinued in November 2017 by Millendo Therapeutics because 3 of 28 women experienced abnormal liver function, which normalized within 90 days. However, the study had shown an 80% decrease in hot flashes in women taking pavinetant, compared with a 30% decrease in the placebo group.
Fezolinetant, currently in phase 3 trials with Astellas, showed a dose response effect on reproductive hormones in phase 1 studies and a short half-life (4-6 hours) in women. It also showed no concerning side effects.
“There was, in fact, a decrease in the endometrial thickness, a delayed or impeded ovulation and a prolonged cycle duration,” Reed said.
The subsequent phase 2a study showed a reduction of five hot flashes a day (93% decrease), compared with placebo (54% decrease, P <.001) “with an abrupt return to baseline hot flash frequency after cessation,” she said. Improvements also occurred in sleep quality, quality of life, disability, and interference of hot flashes in daily life.
The phase 2b study found no difference in effects between once-daily versus twice-daily doses. However, two severe adverse events occurred: a drug-induced liver injury in one woman and cholelithiasis in another, both on the 60-mg, once-daily dose. Additionally, five women on varying doses had transient increases (above 1000 U/L) in creatinine kinase, though apparently without dose response.
A 52-week, three-arm, phase 3 trial of fezolinetant is currently under way with a goal of enrolling 1,740 participants, and plans to be completed by December 2021. Participants will undergo regular adverse event screening first biweekly, then monthly, with vital signs, blood, and urine monitoring.
Meanwhile, NT-814 from KaNDy Therapeutics, has completed phase 2a and phase 2b trials with phase 3 slated to begin in 2021. Adverse events in phase 1 included sleepiness and headache, and it had a long half-life (about 26 hours) and rapid absorption (an hour).
The phase 2a trial found a reduction of five hot flashes a day, compared with placebo, with main side effects again being sleepiness and headache. No events of abnormal liver function occurred. Phase 2b results have not been published.
So far, existing research suggests that KNDy interventions will involve a single daily oral dose that begins taking effect within 3 days and is fully in effect within 1-2 weeks. The reduction in hot flashes, about five fewer a day, is more effective than any other currently used nonhormonal medications for vasomotor symptoms. SSRIs and SNRIs tend to result in 1.5-2 fewer hot flashes a day, and gabapentin results in about 3 fewer per day. It will take longer-term studies, however, and paying attention to liver concerns for the NK3R antagonists to move into clinic.
“We want to keep our eye on the [luteinizing hormone] because if it decreases too much, it could adversely affect sexual function, and this does appear to be a dose-response finding,” Dr. Reed said. It would also be ideal, she said, to target only the KNDy neurons with NK3 antagonists without effects on the NK3 receptors in the liver.
Other nonhormonal options
Oxybutynin is another a nonhormonal agent under investigation for vasomotor symptoms. It’s an anticholinergic that resulted in 80% fewer hot flashes, compared with 30% with placebo in a 2016 trial, but 52% of women complained of dry mouth. A more recent study similarly found high efficacy – a 60%-80% drop in hot flashes, compared with 30% with placebo – but also side effects of dry mouth, difficulty urinating, and abdominal pain.
Finally, Dr. Reed mentioned three other agents under investigation as possible nonhormonal therapeutics, though she has little information about them. They include MT-8554 by Mitsubishi Tanabe; FP-101 by Fervent Pharmaceuticals; and Q-122 by QUE Oncology with Emory University, Atlanta, and the University of Queensland, Brisbane, Australia.
None of the currently available nonhormonal options provide as high efficacy as hormones, but they do reduce symptoms:
Clonidine is an off-label option some physicians already use as a nonhormonal treatment for vasomotor symptoms, but again, the side effects are problematic: dry mouth, constipation, drowsiness, postural hypotension, and poor sleep.
Paroxetine, at 7.5-10 mg, is the only FDA-approved nonhormonal treatment for vasomotor symptoms, but she listed other off-label options found effective in evidence reviews: gabapentin (100-2,400 mg), venlafaxine (37.5-75 mg), citalopram (10 mg), desvenlafaxine (150 mg), and escitalopram (10 mg).
“I want you to take note of the lower doses in all of these products that are efficacious above those doses that might be used for mood,” Dr. Reed added.
Dr. Reed receives royalties from UpToDate and research funding from Bayer. Dr. Santoro owns stock in MenoGeniX and serves as a consultant or advisor to Ansh Labs, MenoGeniX, and Ogeda/Astellas.
A version of this article originally appeared on Medscape.com.
researchers told attendees at the virtual North American Menopause Society 2020 Annual Meeting.
“The KNDy [kisspeptin/neurokinin B/dynorphin] neuron manipulation is really exciting and holds great promise for rapid and highly effective amelioration of hot flashes, up to 80%, and improvement in other menopausal symptoms, though we’re still looking at the safety in phase 3 trials,” reported Susan D. Reed, MD, MPH, director of the Women’s Reproductive Health Research Program at the University of Washington, Seattle.
“If we continue to see good safety data, these are going to be the greatest things since sliced bread,” Dr. Reed said in an interview. “I don’t think we’ve seen anything like this in menopause therapeutics in a long time.”
While several nonhormonal drugs are already used to treat vasomotor symptoms in menopausal women with and without breast cancer, none are as effective as hormone treatments.
“For now, the SSRIs, SNRIs [serotonin norepinephrine reuptake inhibitors], and GABAergics are the best frontline nonhormonal options with a moderate effect, and clonidine and oxybutynin are effective, but we see more side effects with these,” Dr. Reed said. She noted the importance of considering patients’ mood, sleep, pain, sexual function, weight gain, overactive bladder, blood pressure, and individual quality of life (QOL) goals in tailoring those therapies.
But women still need more nonhormonal options that are at least as effective as hormonal options, Dr. Reed said. Some women are unable to take hormonal options because they are at risk for blood clots or breast cancer.
“Then there’s preference,” she said. “Sometimes people don’t like the way they feel when they take hormones, or they just don’t want hormones in their body. It’s absolutely critical to have these options available for women.”
Nanette F. Santoro, MD, a professor of ob.gyn. at the University of Colorado at Denver, Aurora, who was not involved in the presentation, said in an interview that physicians may not always realize the extent to which vasomotor symptoms interfere with women’s daily lives.
“They have an eroding effect on QOL that is not appreciated sometimes,” she said. Though hot flashes eventually subside in most women, others may continue to experience them into their 70s, when hormonal therapies can begin causing more harm than benefit.
“It goes underappreciated that, for a proportion of women, hot flashes will never go away, and they’re just as bad [as] when they were in their 50s,” Dr. Santoro said. “They need to be treated, and the nonhormonal treatments do not work for everybody.”
Promising KNDy therapeutics
Autopsy studies of postmenopausal women revealed that a complex of neurons in the hypothalamus was “massively hypertrophied” and sits right next to the thermoregulatory center of the brain, Dr. Reed explained.
The complex produces three types of molecules: kisspeptin (a neuropeptide), neurokinin B (a neuropeptide), and dynorphin (a kappa opioid), collectively referred to as the KNDy. The KNDy neural complex is located in the same place as the majority of hormone receptors in the arcuate nucleus, a collection of nerve cells in the hypothalamus.
The current hypothesis is that the KNDy neurons, which communicate with each other, become hyperactivated and cause hot flashes by spilling over to and triggering the thermoregulatory center next door. NKB (kisspeptin and neurokinin B) agonists activate KNDy neurons and dynorphin agonists inactivate KNDy, so the expectation is that NKB antagonists or dynorphin agonists would stop hot flashes.
Indeed, research published in 2015 showed that women taking kappa agonists experienced fewer hot flashes than women in the placebo group. However, no peripherally restricted kappa agonists are currently in clinical trials, so their future as therapeutics is unclear.
Right now, three different NK antagonists are in the pipeline for reducing vasomotor symptoms: MLE 4901 (pavinetant) and ESN364 (fezolinetant) are both NK3R antagonists, and NT-814 is a dual NK1R/NK3R antagonist. All three of these drugs were originally developed to treat schizophrenia.
Phase 2 clinical trials of pavinetant were discontinued in November 2017 by Millendo Therapeutics because 3 of 28 women experienced abnormal liver function, which normalized within 90 days. However, the study had shown an 80% decrease in hot flashes in women taking pavinetant, compared with a 30% decrease in the placebo group.
Fezolinetant, currently in phase 3 trials with Astellas, showed a dose response effect on reproductive hormones in phase 1 studies and a short half-life (4-6 hours) in women. It also showed no concerning side effects.
“There was, in fact, a decrease in the endometrial thickness, a delayed or impeded ovulation and a prolonged cycle duration,” Reed said.
The subsequent phase 2a study showed a reduction of five hot flashes a day (93% decrease), compared with placebo (54% decrease, P <.001) “with an abrupt return to baseline hot flash frequency after cessation,” she said. Improvements also occurred in sleep quality, quality of life, disability, and interference of hot flashes in daily life.
The phase 2b study found no difference in effects between once-daily versus twice-daily doses. However, two severe adverse events occurred: a drug-induced liver injury in one woman and cholelithiasis in another, both on the 60-mg, once-daily dose. Additionally, five women on varying doses had transient increases (above 1000 U/L) in creatinine kinase, though apparently without dose response.
A 52-week, three-arm, phase 3 trial of fezolinetant is currently under way with a goal of enrolling 1,740 participants, and plans to be completed by December 2021. Participants will undergo regular adverse event screening first biweekly, then monthly, with vital signs, blood, and urine monitoring.
Meanwhile, NT-814 from KaNDy Therapeutics, has completed phase 2a and phase 2b trials with phase 3 slated to begin in 2021. Adverse events in phase 1 included sleepiness and headache, and it had a long half-life (about 26 hours) and rapid absorption (an hour).
The phase 2a trial found a reduction of five hot flashes a day, compared with placebo, with main side effects again being sleepiness and headache. No events of abnormal liver function occurred. Phase 2b results have not been published.
So far, existing research suggests that KNDy interventions will involve a single daily oral dose that begins taking effect within 3 days and is fully in effect within 1-2 weeks. The reduction in hot flashes, about five fewer a day, is more effective than any other currently used nonhormonal medications for vasomotor symptoms. SSRIs and SNRIs tend to result in 1.5-2 fewer hot flashes a day, and gabapentin results in about 3 fewer per day. It will take longer-term studies, however, and paying attention to liver concerns for the NK3R antagonists to move into clinic.
“We want to keep our eye on the [luteinizing hormone] because if it decreases too much, it could adversely affect sexual function, and this does appear to be a dose-response finding,” Dr. Reed said. It would also be ideal, she said, to target only the KNDy neurons with NK3 antagonists without effects on the NK3 receptors in the liver.
Other nonhormonal options
Oxybutynin is another a nonhormonal agent under investigation for vasomotor symptoms. It’s an anticholinergic that resulted in 80% fewer hot flashes, compared with 30% with placebo in a 2016 trial, but 52% of women complained of dry mouth. A more recent study similarly found high efficacy – a 60%-80% drop in hot flashes, compared with 30% with placebo – but also side effects of dry mouth, difficulty urinating, and abdominal pain.
Finally, Dr. Reed mentioned three other agents under investigation as possible nonhormonal therapeutics, though she has little information about them. They include MT-8554 by Mitsubishi Tanabe; FP-101 by Fervent Pharmaceuticals; and Q-122 by QUE Oncology with Emory University, Atlanta, and the University of Queensland, Brisbane, Australia.
None of the currently available nonhormonal options provide as high efficacy as hormones, but they do reduce symptoms:
Clonidine is an off-label option some physicians already use as a nonhormonal treatment for vasomotor symptoms, but again, the side effects are problematic: dry mouth, constipation, drowsiness, postural hypotension, and poor sleep.
Paroxetine, at 7.5-10 mg, is the only FDA-approved nonhormonal treatment for vasomotor symptoms, but she listed other off-label options found effective in evidence reviews: gabapentin (100-2,400 mg), venlafaxine (37.5-75 mg), citalopram (10 mg), desvenlafaxine (150 mg), and escitalopram (10 mg).
“I want you to take note of the lower doses in all of these products that are efficacious above those doses that might be used for mood,” Dr. Reed added.
Dr. Reed receives royalties from UpToDate and research funding from Bayer. Dr. Santoro owns stock in MenoGeniX and serves as a consultant or advisor to Ansh Labs, MenoGeniX, and Ogeda/Astellas.
A version of this article originally appeared on Medscape.com.
researchers told attendees at the virtual North American Menopause Society 2020 Annual Meeting.
“The KNDy [kisspeptin/neurokinin B/dynorphin] neuron manipulation is really exciting and holds great promise for rapid and highly effective amelioration of hot flashes, up to 80%, and improvement in other menopausal symptoms, though we’re still looking at the safety in phase 3 trials,” reported Susan D. Reed, MD, MPH, director of the Women’s Reproductive Health Research Program at the University of Washington, Seattle.
“If we continue to see good safety data, these are going to be the greatest things since sliced bread,” Dr. Reed said in an interview. “I don’t think we’ve seen anything like this in menopause therapeutics in a long time.”
While several nonhormonal drugs are already used to treat vasomotor symptoms in menopausal women with and without breast cancer, none are as effective as hormone treatments.
“For now, the SSRIs, SNRIs [serotonin norepinephrine reuptake inhibitors], and GABAergics are the best frontline nonhormonal options with a moderate effect, and clonidine and oxybutynin are effective, but we see more side effects with these,” Dr. Reed said. She noted the importance of considering patients’ mood, sleep, pain, sexual function, weight gain, overactive bladder, blood pressure, and individual quality of life (QOL) goals in tailoring those therapies.
But women still need more nonhormonal options that are at least as effective as hormonal options, Dr. Reed said. Some women are unable to take hormonal options because they are at risk for blood clots or breast cancer.
“Then there’s preference,” she said. “Sometimes people don’t like the way they feel when they take hormones, or they just don’t want hormones in their body. It’s absolutely critical to have these options available for women.”
Nanette F. Santoro, MD, a professor of ob.gyn. at the University of Colorado at Denver, Aurora, who was not involved in the presentation, said in an interview that physicians may not always realize the extent to which vasomotor symptoms interfere with women’s daily lives.
“They have an eroding effect on QOL that is not appreciated sometimes,” she said. Though hot flashes eventually subside in most women, others may continue to experience them into their 70s, when hormonal therapies can begin causing more harm than benefit.
“It goes underappreciated that, for a proportion of women, hot flashes will never go away, and they’re just as bad [as] when they were in their 50s,” Dr. Santoro said. “They need to be treated, and the nonhormonal treatments do not work for everybody.”
Promising KNDy therapeutics
Autopsy studies of postmenopausal women revealed that a complex of neurons in the hypothalamus was “massively hypertrophied” and sits right next to the thermoregulatory center of the brain, Dr. Reed explained.
The complex produces three types of molecules: kisspeptin (a neuropeptide), neurokinin B (a neuropeptide), and dynorphin (a kappa opioid), collectively referred to as the KNDy. The KNDy neural complex is located in the same place as the majority of hormone receptors in the arcuate nucleus, a collection of nerve cells in the hypothalamus.
The current hypothesis is that the KNDy neurons, which communicate with each other, become hyperactivated and cause hot flashes by spilling over to and triggering the thermoregulatory center next door. NKB (kisspeptin and neurokinin B) agonists activate KNDy neurons and dynorphin agonists inactivate KNDy, so the expectation is that NKB antagonists or dynorphin agonists would stop hot flashes.
Indeed, research published in 2015 showed that women taking kappa agonists experienced fewer hot flashes than women in the placebo group. However, no peripherally restricted kappa agonists are currently in clinical trials, so their future as therapeutics is unclear.
Right now, three different NK antagonists are in the pipeline for reducing vasomotor symptoms: MLE 4901 (pavinetant) and ESN364 (fezolinetant) are both NK3R antagonists, and NT-814 is a dual NK1R/NK3R antagonist. All three of these drugs were originally developed to treat schizophrenia.
Phase 2 clinical trials of pavinetant were discontinued in November 2017 by Millendo Therapeutics because 3 of 28 women experienced abnormal liver function, which normalized within 90 days. However, the study had shown an 80% decrease in hot flashes in women taking pavinetant, compared with a 30% decrease in the placebo group.
Fezolinetant, currently in phase 3 trials with Astellas, showed a dose response effect on reproductive hormones in phase 1 studies and a short half-life (4-6 hours) in women. It also showed no concerning side effects.
“There was, in fact, a decrease in the endometrial thickness, a delayed or impeded ovulation and a prolonged cycle duration,” Reed said.
The subsequent phase 2a study showed a reduction of five hot flashes a day (93% decrease), compared with placebo (54% decrease, P <.001) “with an abrupt return to baseline hot flash frequency after cessation,” she said. Improvements also occurred in sleep quality, quality of life, disability, and interference of hot flashes in daily life.
The phase 2b study found no difference in effects between once-daily versus twice-daily doses. However, two severe adverse events occurred: a drug-induced liver injury in one woman and cholelithiasis in another, both on the 60-mg, once-daily dose. Additionally, five women on varying doses had transient increases (above 1000 U/L) in creatinine kinase, though apparently without dose response.
A 52-week, three-arm, phase 3 trial of fezolinetant is currently under way with a goal of enrolling 1,740 participants, and plans to be completed by December 2021. Participants will undergo regular adverse event screening first biweekly, then monthly, with vital signs, blood, and urine monitoring.
Meanwhile, NT-814 from KaNDy Therapeutics, has completed phase 2a and phase 2b trials with phase 3 slated to begin in 2021. Adverse events in phase 1 included sleepiness and headache, and it had a long half-life (about 26 hours) and rapid absorption (an hour).
The phase 2a trial found a reduction of five hot flashes a day, compared with placebo, with main side effects again being sleepiness and headache. No events of abnormal liver function occurred. Phase 2b results have not been published.
So far, existing research suggests that KNDy interventions will involve a single daily oral dose that begins taking effect within 3 days and is fully in effect within 1-2 weeks. The reduction in hot flashes, about five fewer a day, is more effective than any other currently used nonhormonal medications for vasomotor symptoms. SSRIs and SNRIs tend to result in 1.5-2 fewer hot flashes a day, and gabapentin results in about 3 fewer per day. It will take longer-term studies, however, and paying attention to liver concerns for the NK3R antagonists to move into clinic.
“We want to keep our eye on the [luteinizing hormone] because if it decreases too much, it could adversely affect sexual function, and this does appear to be a dose-response finding,” Dr. Reed said. It would also be ideal, she said, to target only the KNDy neurons with NK3 antagonists without effects on the NK3 receptors in the liver.
Other nonhormonal options
Oxybutynin is another a nonhormonal agent under investigation for vasomotor symptoms. It’s an anticholinergic that resulted in 80% fewer hot flashes, compared with 30% with placebo in a 2016 trial, but 52% of women complained of dry mouth. A more recent study similarly found high efficacy – a 60%-80% drop in hot flashes, compared with 30% with placebo – but also side effects of dry mouth, difficulty urinating, and abdominal pain.
Finally, Dr. Reed mentioned three other agents under investigation as possible nonhormonal therapeutics, though she has little information about them. They include MT-8554 by Mitsubishi Tanabe; FP-101 by Fervent Pharmaceuticals; and Q-122 by QUE Oncology with Emory University, Atlanta, and the University of Queensland, Brisbane, Australia.
None of the currently available nonhormonal options provide as high efficacy as hormones, but they do reduce symptoms:
Clonidine is an off-label option some physicians already use as a nonhormonal treatment for vasomotor symptoms, but again, the side effects are problematic: dry mouth, constipation, drowsiness, postural hypotension, and poor sleep.
Paroxetine, at 7.5-10 mg, is the only FDA-approved nonhormonal treatment for vasomotor symptoms, but she listed other off-label options found effective in evidence reviews: gabapentin (100-2,400 mg), venlafaxine (37.5-75 mg), citalopram (10 mg), desvenlafaxine (150 mg), and escitalopram (10 mg).
“I want you to take note of the lower doses in all of these products that are efficacious above those doses that might be used for mood,” Dr. Reed added.
Dr. Reed receives royalties from UpToDate and research funding from Bayer. Dr. Santoro owns stock in MenoGeniX and serves as a consultant or advisor to Ansh Labs, MenoGeniX, and Ogeda/Astellas.
A version of this article originally appeared on Medscape.com.
Beyond microcephaly: Zika-affected children near school age
In 2020, “the virus” has come to mean one thing: SARS-CoV-2. But just a few years ago, Zika had the world's attention, as one news report after another described children with microcephaly born to women who'd been infected while pregnant.
It can be difficult for physicians to determine whether a birth defect is the result of Zika. Most infections have few or no symptoms, and mothers may not know if they’ve been exposed. Karin Nielsen, MD, remembers one child in particular, a 9-month-old boy born with microcephaly whose parents brought the infant to her in 2018 because he had started having seizures.
The child was born in Mexico in 2017, when the Zika virus was still known to be circulating in the Americas, said Dr. Nielsen, a pediatric infectious disease specialist at the University of California, Los Angeles. Brain imaging revealed calcifications and other signs in the boy’s brain that were consistent with exposure. But his mother said she was never sick during pregnancy.
Because Zika is transmitted not just via mosquito and from mother to fetus but also sexually, Dr. Nielsen thinks the mother probably contracted an asymptomatic infection from her husband, who recalled having a rash when she was 4 months pregnant. When they participated in a research study, both parents tested positive for Zika antibodies.
“The child had the classic symptoms of congenital Zika syndrome,” Dr. Nielsen said. “He was 9 months old, he had microcephaly, and he was having mal seizures.”
Researchers have since learned that children with such classic symptoms represent only a small proportion of those affected by prenatal Zika exposure – about 3%-5%. The virus was at its height during the 2016-2016 epidemic and is not currently causing outbreaks. But as researchers have followed cohorts of children exposed to Zika in utero, they have found many subtler effects physicians will need to monitor as the children grow up.
“When we’re seeing hundreds of kids with microcephaly, we had a lot of people infected,” Dr. Nielsen said. “Microcephaly is only the tip of the iceberg.”
Early evidence
Microcephaly may be the most identifiable symptom of fetal Zika infection, but researchers tracking cohorts of exposed children have begun to build a more complete picture of what long-term effects might look like. But hundreds, if not thousands, of children have been exposed to Zika in the womb – it’s not clear how many, Dr. Nielsen said – and many show a range of effects that don’t officially qualify as congenital Zika syndrome.
Current estimates suggest about one third of exposed children have some type of neurologic or neurodevelopmental problem, even though prevalence of visible effects is much lower. Over time, the incidence of these effects has fluctuated; some developmental delays and sensory deficits began manifesting later in childhood whereas others, at least in a few children, have resolved.
“We’re just beginning to have some of the data that we need to think about the full spectrum of outcomes,” said Cindy Moore, MD, chief medical officer in the Division of Congenital and Developmental Disorders in the Centers for Disease Control and Prevention’s National Center on Birth Defects and Developmental Disabilities.
“As we’re learning more and more, we’re learning the spectrum is expanding to less severe forms,” Dr. Moore said. “We do know that with some infections, there are later onset of problems.”
Studies published in 2018 described cohorts of children whose mothers had confirmed or suspected Zika infections during pregnancy in the French Territories of America (Guadalupe, Martinique, and French Guiana) and in Salvador, Brazil. The research provided valuable early data on the incidence of microcephaly and other severe effects in newborns, but noted the need for long-term follow up.
The U.S. Zika Pregnancy and Infant Registry is one of the largest such cohorts. In August 2018, researchers made their first report on data from the registry They looked at 1450 children age 1 or older who had undergone neuroimaging or screenings (developmental, vision, hearing) or both. In 6%, at least one birth defect was linked to Zika, and 9% had at least one neurodevelopmental abnormality.
As these children age past developmental milestones, more effects will likely manifest – even in those children whose appearance and imaging presented as healthy at birth.
Longer-term follow up
Nielsen at UCLA and M. Elisabeth Lopes Moreira, MD, of the Oswaldo Cruz Foundation in Rio de Janeiro, are following a cohort of more than 100 children born in Rio de Janeiro during Brazil’s 2015-2016 epidemic to mothers with symptomatic, PCR-confirmed Zika infections during pregnancy. In December 2018, their team reported that rates of severe neurodevelopmental delay and sensory dysfunction – 14% of 131 children aged 12-18 months – were higher than those found in earlier studies.
In August 2019, the team described neurodevelopmental, vision, and hearing outcomes in 216 Zika-exposed children 2 years after birth. They used the Bayley-III Scales of Infant and Toddler Development to assess cognitive, language and motor skills in 146 of the children. Forty percent of them were below or very below average in development, more than one third (35%) had language delays, 12% percent had hearing loss, and 7% had abnormal eye anatomy, such as underdeveloped retinas.
In two of the eight children in the cohort with microcephaly, the abnormality unexpectedly resolved. Although that finding received a lot of press, Dr. Nielsen pointed out that “not all microcephalies are created equal.”
In one case, a child born small for gestational age had proportional microcephaly: the baby›s head circumference met the criteria for microcephaly, but the infant›s head was proportional to the body so, as the child grew, the apparent microcephaly disappeared.
In the other case, the child was born with craniosynostosis, in which the skull sutures fuse too early – another effect seen with prenatal Zika exposure, Dr. Nielsen said. After corrective surgery, the child’s head circumference no longer met the definition of microcephaly, but the child still had symptoms related to congenital Zika: a developmental delay and calcifications in the brain. Meanwhile, two other children in the Rio cohort developed secondary microcephaly.
In another follow-up study of children up to age 4, Dr. Nielsen and colleagues found that both clinicians and family may think that Zika-exposed infants without microcephaly are developing normally, but that may not be true. Nearly 70% of children without microcephaly had neurologic abnormalities on physical examination, and more than half had failure to thrive because of poor feeding related to neurologic abnormalities.
Initially, some children may be able to mask subtle problems. A study published in January from Sarah B. Mulkey, MD, PhD, of Children’s National Hospital in Washington, DC, and colleagues described neurodevelopmental outcomes in 70 Colombian children up to 18 months old who had been exposed to Zika in utero. The children had a normal head circumference at birth and a normal fetal MRI, but – compared with typically developing peers – their communication, social cognition, and mobility scores on standardized assessments tended to decline as they got older.
“Especially in a very young child, there’s always going to be a possibility that you can compensate for a deficit, and it appears that at least some of these children are doing so,” said William J. Muller, MD, PhD, associate professor of pediatrics at Northwestern University, Chicago. When the children are older, certain behavioral effects will become easier to assess.
“With these children now approaching school age, understanding the full spectrum of neurodevelopmental abnormalities has important public health and educational system implications,” Dr. Muller and Dr. Mulkey wrote in a commentary about one of Dr. Nielsen’s studies.
Researchers face multiple barriers to understanding the long-term effects of fetal Zika infection. Many infants known to have been exposed in utero never received the recommended early assessments and haven’t been followed long-term. Particularly in Brazil, poverty, poor access to healthcare, and overcrowding all complicate surveillance efforts, Dr. Muller said. Stigma related to children’s neurodevelopmental problems also can potentially reduce a mother’s willingness to attend all follow-ups and assessments.
Some children may have been exposed but were never recognized as such, making it difficult for researchers to track their development and assemble a complete picture of prenatal Zika infection outcomes. Asymptomatic infection occurs in about 80% of Zika infections, though it’s not clear if that number holds for infections during pregnancy as well, according to Dr. Muller and Dr. Mulkey. Because nearly all the current research involves children whose mothers had symptomatic infections, the studies’ generalizability may be limited.
Those likely asymptomatic infections are also a major reason none of the cohorts have comparison groups.
“There are literally hundreds of things that can contribute to or cause developmental problems,” said Dr. Moore of the CDC, who noted that it would be nice to have a comparison group so as to know what Zika may not be responsible for. That said, it would be difficult-to-impossible to create a control group with similar geographic and demographic characteristics as the exposed children, a group who researchers can be certain weren’t exposed.
Neurodevelopmental disabilities occur in about 15% of the general population, making it difficult to determine whether Zika causes any or all long-term, less severe developmental findings in exposed children. The difficulty only compounds with time: the older a child is when a developmental problem is recognized, the harder it is to go back and say the problem is a result of something that occurred before birth, Dr. Moore said. “It’s a challenging field to say, this is what caused that outcome.”
Exposed children need continued evaluation
Interpreting the clinical implications of available studies is also challenging. It can be difficult to distinguish between central nervous system damage and peripheral damage, leaving the true etiology of poor vision or hearing elusive. The Zika virus can attack both the optic nerve and the part of the brain that interprets what a person sees: “Are you not seeing well because that part of your brain is not developed, or is it just a problem with the eye?” Dr. Nielsen said.
When problems can’t be precisely identified, successful interventions are harder. If the cochlea is normal, for instance, but the part of the brain that interprets sound or language has deficits, a hearing aid won’t help.
The services and interventions that children need depend on their specific developmental or cognitive deficits, regardless of the cause. But if clinicians know the cause is likely Zika exposure, they also know to look for other deficits.
Children showing likely effects of congenital Zika infection should be further evaluated for other possible birth defects and referred to a developmental specialist, early intervention services, and family support services. Depending on the child, primary care providers might consider referrals to an infectious disease specialist, clinical geneticist, neurologist, or other specialists.
Even with no confirmed infection or visible signs at birth, clinicians should remain vigilant with children who had possible exposure. A recently published study of 120 children conceived during the Zika outbreak in Paraíba, Brazil, assessed as infants and then again at 2 years old, exemplifies why. Researchers identified adverse neurologic outcomes and developmental delays in several children who had no physical evidence of birth defects as newborns, but whose antibody tests showed possible infection.
“In this post-epidemic period, with decreased Zika transmission and less public awareness,” wrote Dr. Mulkey and a colleague, “follow-up of these children is now more important than ever”.
A version of this article originally appeared on Medscape.com.
In 2020, “the virus” has come to mean one thing: SARS-CoV-2. But just a few years ago, Zika had the world's attention, as one news report after another described children with microcephaly born to women who'd been infected while pregnant.
It can be difficult for physicians to determine whether a birth defect is the result of Zika. Most infections have few or no symptoms, and mothers may not know if they’ve been exposed. Karin Nielsen, MD, remembers one child in particular, a 9-month-old boy born with microcephaly whose parents brought the infant to her in 2018 because he had started having seizures.
The child was born in Mexico in 2017, when the Zika virus was still known to be circulating in the Americas, said Dr. Nielsen, a pediatric infectious disease specialist at the University of California, Los Angeles. Brain imaging revealed calcifications and other signs in the boy’s brain that were consistent with exposure. But his mother said she was never sick during pregnancy.
Because Zika is transmitted not just via mosquito and from mother to fetus but also sexually, Dr. Nielsen thinks the mother probably contracted an asymptomatic infection from her husband, who recalled having a rash when she was 4 months pregnant. When they participated in a research study, both parents tested positive for Zika antibodies.
“The child had the classic symptoms of congenital Zika syndrome,” Dr. Nielsen said. “He was 9 months old, he had microcephaly, and he was having mal seizures.”
Researchers have since learned that children with such classic symptoms represent only a small proportion of those affected by prenatal Zika exposure – about 3%-5%. The virus was at its height during the 2016-2016 epidemic and is not currently causing outbreaks. But as researchers have followed cohorts of children exposed to Zika in utero, they have found many subtler effects physicians will need to monitor as the children grow up.
“When we’re seeing hundreds of kids with microcephaly, we had a lot of people infected,” Dr. Nielsen said. “Microcephaly is only the tip of the iceberg.”
Early evidence
Microcephaly may be the most identifiable symptom of fetal Zika infection, but researchers tracking cohorts of exposed children have begun to build a more complete picture of what long-term effects might look like. But hundreds, if not thousands, of children have been exposed to Zika in the womb – it’s not clear how many, Dr. Nielsen said – and many show a range of effects that don’t officially qualify as congenital Zika syndrome.
Current estimates suggest about one third of exposed children have some type of neurologic or neurodevelopmental problem, even though prevalence of visible effects is much lower. Over time, the incidence of these effects has fluctuated; some developmental delays and sensory deficits began manifesting later in childhood whereas others, at least in a few children, have resolved.
“We’re just beginning to have some of the data that we need to think about the full spectrum of outcomes,” said Cindy Moore, MD, chief medical officer in the Division of Congenital and Developmental Disorders in the Centers for Disease Control and Prevention’s National Center on Birth Defects and Developmental Disabilities.
“As we’re learning more and more, we’re learning the spectrum is expanding to less severe forms,” Dr. Moore said. “We do know that with some infections, there are later onset of problems.”
Studies published in 2018 described cohorts of children whose mothers had confirmed or suspected Zika infections during pregnancy in the French Territories of America (Guadalupe, Martinique, and French Guiana) and in Salvador, Brazil. The research provided valuable early data on the incidence of microcephaly and other severe effects in newborns, but noted the need for long-term follow up.
The U.S. Zika Pregnancy and Infant Registry is one of the largest such cohorts. In August 2018, researchers made their first report on data from the registry They looked at 1450 children age 1 or older who had undergone neuroimaging or screenings (developmental, vision, hearing) or both. In 6%, at least one birth defect was linked to Zika, and 9% had at least one neurodevelopmental abnormality.
As these children age past developmental milestones, more effects will likely manifest – even in those children whose appearance and imaging presented as healthy at birth.
Longer-term follow up
Nielsen at UCLA and M. Elisabeth Lopes Moreira, MD, of the Oswaldo Cruz Foundation in Rio de Janeiro, are following a cohort of more than 100 children born in Rio de Janeiro during Brazil’s 2015-2016 epidemic to mothers with symptomatic, PCR-confirmed Zika infections during pregnancy. In December 2018, their team reported that rates of severe neurodevelopmental delay and sensory dysfunction – 14% of 131 children aged 12-18 months – were higher than those found in earlier studies.
In August 2019, the team described neurodevelopmental, vision, and hearing outcomes in 216 Zika-exposed children 2 years after birth. They used the Bayley-III Scales of Infant and Toddler Development to assess cognitive, language and motor skills in 146 of the children. Forty percent of them were below or very below average in development, more than one third (35%) had language delays, 12% percent had hearing loss, and 7% had abnormal eye anatomy, such as underdeveloped retinas.
In two of the eight children in the cohort with microcephaly, the abnormality unexpectedly resolved. Although that finding received a lot of press, Dr. Nielsen pointed out that “not all microcephalies are created equal.”
In one case, a child born small for gestational age had proportional microcephaly: the baby›s head circumference met the criteria for microcephaly, but the infant›s head was proportional to the body so, as the child grew, the apparent microcephaly disappeared.
In the other case, the child was born with craniosynostosis, in which the skull sutures fuse too early – another effect seen with prenatal Zika exposure, Dr. Nielsen said. After corrective surgery, the child’s head circumference no longer met the definition of microcephaly, but the child still had symptoms related to congenital Zika: a developmental delay and calcifications in the brain. Meanwhile, two other children in the Rio cohort developed secondary microcephaly.
In another follow-up study of children up to age 4, Dr. Nielsen and colleagues found that both clinicians and family may think that Zika-exposed infants without microcephaly are developing normally, but that may not be true. Nearly 70% of children without microcephaly had neurologic abnormalities on physical examination, and more than half had failure to thrive because of poor feeding related to neurologic abnormalities.
Initially, some children may be able to mask subtle problems. A study published in January from Sarah B. Mulkey, MD, PhD, of Children’s National Hospital in Washington, DC, and colleagues described neurodevelopmental outcomes in 70 Colombian children up to 18 months old who had been exposed to Zika in utero. The children had a normal head circumference at birth and a normal fetal MRI, but – compared with typically developing peers – their communication, social cognition, and mobility scores on standardized assessments tended to decline as they got older.
“Especially in a very young child, there’s always going to be a possibility that you can compensate for a deficit, and it appears that at least some of these children are doing so,” said William J. Muller, MD, PhD, associate professor of pediatrics at Northwestern University, Chicago. When the children are older, certain behavioral effects will become easier to assess.
“With these children now approaching school age, understanding the full spectrum of neurodevelopmental abnormalities has important public health and educational system implications,” Dr. Muller and Dr. Mulkey wrote in a commentary about one of Dr. Nielsen’s studies.
Researchers face multiple barriers to understanding the long-term effects of fetal Zika infection. Many infants known to have been exposed in utero never received the recommended early assessments and haven’t been followed long-term. Particularly in Brazil, poverty, poor access to healthcare, and overcrowding all complicate surveillance efforts, Dr. Muller said. Stigma related to children’s neurodevelopmental problems also can potentially reduce a mother’s willingness to attend all follow-ups and assessments.
Some children may have been exposed but were never recognized as such, making it difficult for researchers to track their development and assemble a complete picture of prenatal Zika infection outcomes. Asymptomatic infection occurs in about 80% of Zika infections, though it’s not clear if that number holds for infections during pregnancy as well, according to Dr. Muller and Dr. Mulkey. Because nearly all the current research involves children whose mothers had symptomatic infections, the studies’ generalizability may be limited.
Those likely asymptomatic infections are also a major reason none of the cohorts have comparison groups.
“There are literally hundreds of things that can contribute to or cause developmental problems,” said Dr. Moore of the CDC, who noted that it would be nice to have a comparison group so as to know what Zika may not be responsible for. That said, it would be difficult-to-impossible to create a control group with similar geographic and demographic characteristics as the exposed children, a group who researchers can be certain weren’t exposed.
Neurodevelopmental disabilities occur in about 15% of the general population, making it difficult to determine whether Zika causes any or all long-term, less severe developmental findings in exposed children. The difficulty only compounds with time: the older a child is when a developmental problem is recognized, the harder it is to go back and say the problem is a result of something that occurred before birth, Dr. Moore said. “It’s a challenging field to say, this is what caused that outcome.”
Exposed children need continued evaluation
Interpreting the clinical implications of available studies is also challenging. It can be difficult to distinguish between central nervous system damage and peripheral damage, leaving the true etiology of poor vision or hearing elusive. The Zika virus can attack both the optic nerve and the part of the brain that interprets what a person sees: “Are you not seeing well because that part of your brain is not developed, or is it just a problem with the eye?” Dr. Nielsen said.
When problems can’t be precisely identified, successful interventions are harder. If the cochlea is normal, for instance, but the part of the brain that interprets sound or language has deficits, a hearing aid won’t help.
The services and interventions that children need depend on their specific developmental or cognitive deficits, regardless of the cause. But if clinicians know the cause is likely Zika exposure, they also know to look for other deficits.
Children showing likely effects of congenital Zika infection should be further evaluated for other possible birth defects and referred to a developmental specialist, early intervention services, and family support services. Depending on the child, primary care providers might consider referrals to an infectious disease specialist, clinical geneticist, neurologist, or other specialists.
Even with no confirmed infection or visible signs at birth, clinicians should remain vigilant with children who had possible exposure. A recently published study of 120 children conceived during the Zika outbreak in Paraíba, Brazil, assessed as infants and then again at 2 years old, exemplifies why. Researchers identified adverse neurologic outcomes and developmental delays in several children who had no physical evidence of birth defects as newborns, but whose antibody tests showed possible infection.
“In this post-epidemic period, with decreased Zika transmission and less public awareness,” wrote Dr. Mulkey and a colleague, “follow-up of these children is now more important than ever”.
A version of this article originally appeared on Medscape.com.
In 2020, “the virus” has come to mean one thing: SARS-CoV-2. But just a few years ago, Zika had the world's attention, as one news report after another described children with microcephaly born to women who'd been infected while pregnant.
It can be difficult for physicians to determine whether a birth defect is the result of Zika. Most infections have few or no symptoms, and mothers may not know if they’ve been exposed. Karin Nielsen, MD, remembers one child in particular, a 9-month-old boy born with microcephaly whose parents brought the infant to her in 2018 because he had started having seizures.
The child was born in Mexico in 2017, when the Zika virus was still known to be circulating in the Americas, said Dr. Nielsen, a pediatric infectious disease specialist at the University of California, Los Angeles. Brain imaging revealed calcifications and other signs in the boy’s brain that were consistent with exposure. But his mother said she was never sick during pregnancy.
Because Zika is transmitted not just via mosquito and from mother to fetus but also sexually, Dr. Nielsen thinks the mother probably contracted an asymptomatic infection from her husband, who recalled having a rash when she was 4 months pregnant. When they participated in a research study, both parents tested positive for Zika antibodies.
“The child had the classic symptoms of congenital Zika syndrome,” Dr. Nielsen said. “He was 9 months old, he had microcephaly, and he was having mal seizures.”
Researchers have since learned that children with such classic symptoms represent only a small proportion of those affected by prenatal Zika exposure – about 3%-5%. The virus was at its height during the 2016-2016 epidemic and is not currently causing outbreaks. But as researchers have followed cohorts of children exposed to Zika in utero, they have found many subtler effects physicians will need to monitor as the children grow up.
“When we’re seeing hundreds of kids with microcephaly, we had a lot of people infected,” Dr. Nielsen said. “Microcephaly is only the tip of the iceberg.”
Early evidence
Microcephaly may be the most identifiable symptom of fetal Zika infection, but researchers tracking cohorts of exposed children have begun to build a more complete picture of what long-term effects might look like. But hundreds, if not thousands, of children have been exposed to Zika in the womb – it’s not clear how many, Dr. Nielsen said – and many show a range of effects that don’t officially qualify as congenital Zika syndrome.
Current estimates suggest about one third of exposed children have some type of neurologic or neurodevelopmental problem, even though prevalence of visible effects is much lower. Over time, the incidence of these effects has fluctuated; some developmental delays and sensory deficits began manifesting later in childhood whereas others, at least in a few children, have resolved.
“We’re just beginning to have some of the data that we need to think about the full spectrum of outcomes,” said Cindy Moore, MD, chief medical officer in the Division of Congenital and Developmental Disorders in the Centers for Disease Control and Prevention’s National Center on Birth Defects and Developmental Disabilities.
“As we’re learning more and more, we’re learning the spectrum is expanding to less severe forms,” Dr. Moore said. “We do know that with some infections, there are later onset of problems.”
Studies published in 2018 described cohorts of children whose mothers had confirmed or suspected Zika infections during pregnancy in the French Territories of America (Guadalupe, Martinique, and French Guiana) and in Salvador, Brazil. The research provided valuable early data on the incidence of microcephaly and other severe effects in newborns, but noted the need for long-term follow up.
The U.S. Zika Pregnancy and Infant Registry is one of the largest such cohorts. In August 2018, researchers made their first report on data from the registry They looked at 1450 children age 1 or older who had undergone neuroimaging or screenings (developmental, vision, hearing) or both. In 6%, at least one birth defect was linked to Zika, and 9% had at least one neurodevelopmental abnormality.
As these children age past developmental milestones, more effects will likely manifest – even in those children whose appearance and imaging presented as healthy at birth.
Longer-term follow up
Nielsen at UCLA and M. Elisabeth Lopes Moreira, MD, of the Oswaldo Cruz Foundation in Rio de Janeiro, are following a cohort of more than 100 children born in Rio de Janeiro during Brazil’s 2015-2016 epidemic to mothers with symptomatic, PCR-confirmed Zika infections during pregnancy. In December 2018, their team reported that rates of severe neurodevelopmental delay and sensory dysfunction – 14% of 131 children aged 12-18 months – were higher than those found in earlier studies.
In August 2019, the team described neurodevelopmental, vision, and hearing outcomes in 216 Zika-exposed children 2 years after birth. They used the Bayley-III Scales of Infant and Toddler Development to assess cognitive, language and motor skills in 146 of the children. Forty percent of them were below or very below average in development, more than one third (35%) had language delays, 12% percent had hearing loss, and 7% had abnormal eye anatomy, such as underdeveloped retinas.
In two of the eight children in the cohort with microcephaly, the abnormality unexpectedly resolved. Although that finding received a lot of press, Dr. Nielsen pointed out that “not all microcephalies are created equal.”
In one case, a child born small for gestational age had proportional microcephaly: the baby›s head circumference met the criteria for microcephaly, but the infant›s head was proportional to the body so, as the child grew, the apparent microcephaly disappeared.
In the other case, the child was born with craniosynostosis, in which the skull sutures fuse too early – another effect seen with prenatal Zika exposure, Dr. Nielsen said. After corrective surgery, the child’s head circumference no longer met the definition of microcephaly, but the child still had symptoms related to congenital Zika: a developmental delay and calcifications in the brain. Meanwhile, two other children in the Rio cohort developed secondary microcephaly.
In another follow-up study of children up to age 4, Dr. Nielsen and colleagues found that both clinicians and family may think that Zika-exposed infants without microcephaly are developing normally, but that may not be true. Nearly 70% of children without microcephaly had neurologic abnormalities on physical examination, and more than half had failure to thrive because of poor feeding related to neurologic abnormalities.
Initially, some children may be able to mask subtle problems. A study published in January from Sarah B. Mulkey, MD, PhD, of Children’s National Hospital in Washington, DC, and colleagues described neurodevelopmental outcomes in 70 Colombian children up to 18 months old who had been exposed to Zika in utero. The children had a normal head circumference at birth and a normal fetal MRI, but – compared with typically developing peers – their communication, social cognition, and mobility scores on standardized assessments tended to decline as they got older.
“Especially in a very young child, there’s always going to be a possibility that you can compensate for a deficit, and it appears that at least some of these children are doing so,” said William J. Muller, MD, PhD, associate professor of pediatrics at Northwestern University, Chicago. When the children are older, certain behavioral effects will become easier to assess.
“With these children now approaching school age, understanding the full spectrum of neurodevelopmental abnormalities has important public health and educational system implications,” Dr. Muller and Dr. Mulkey wrote in a commentary about one of Dr. Nielsen’s studies.
Researchers face multiple barriers to understanding the long-term effects of fetal Zika infection. Many infants known to have been exposed in utero never received the recommended early assessments and haven’t been followed long-term. Particularly in Brazil, poverty, poor access to healthcare, and overcrowding all complicate surveillance efforts, Dr. Muller said. Stigma related to children’s neurodevelopmental problems also can potentially reduce a mother’s willingness to attend all follow-ups and assessments.
Some children may have been exposed but were never recognized as such, making it difficult for researchers to track their development and assemble a complete picture of prenatal Zika infection outcomes. Asymptomatic infection occurs in about 80% of Zika infections, though it’s not clear if that number holds for infections during pregnancy as well, according to Dr. Muller and Dr. Mulkey. Because nearly all the current research involves children whose mothers had symptomatic infections, the studies’ generalizability may be limited.
Those likely asymptomatic infections are also a major reason none of the cohorts have comparison groups.
“There are literally hundreds of things that can contribute to or cause developmental problems,” said Dr. Moore of the CDC, who noted that it would be nice to have a comparison group so as to know what Zika may not be responsible for. That said, it would be difficult-to-impossible to create a control group with similar geographic and demographic characteristics as the exposed children, a group who researchers can be certain weren’t exposed.
Neurodevelopmental disabilities occur in about 15% of the general population, making it difficult to determine whether Zika causes any or all long-term, less severe developmental findings in exposed children. The difficulty only compounds with time: the older a child is when a developmental problem is recognized, the harder it is to go back and say the problem is a result of something that occurred before birth, Dr. Moore said. “It’s a challenging field to say, this is what caused that outcome.”
Exposed children need continued evaluation
Interpreting the clinical implications of available studies is also challenging. It can be difficult to distinguish between central nervous system damage and peripheral damage, leaving the true etiology of poor vision or hearing elusive. The Zika virus can attack both the optic nerve and the part of the brain that interprets what a person sees: “Are you not seeing well because that part of your brain is not developed, or is it just a problem with the eye?” Dr. Nielsen said.
When problems can’t be precisely identified, successful interventions are harder. If the cochlea is normal, for instance, but the part of the brain that interprets sound or language has deficits, a hearing aid won’t help.
The services and interventions that children need depend on their specific developmental or cognitive deficits, regardless of the cause. But if clinicians know the cause is likely Zika exposure, they also know to look for other deficits.
Children showing likely effects of congenital Zika infection should be further evaluated for other possible birth defects and referred to a developmental specialist, early intervention services, and family support services. Depending on the child, primary care providers might consider referrals to an infectious disease specialist, clinical geneticist, neurologist, or other specialists.
Even with no confirmed infection or visible signs at birth, clinicians should remain vigilant with children who had possible exposure. A recently published study of 120 children conceived during the Zika outbreak in Paraíba, Brazil, assessed as infants and then again at 2 years old, exemplifies why. Researchers identified adverse neurologic outcomes and developmental delays in several children who had no physical evidence of birth defects as newborns, but whose antibody tests showed possible infection.
“In this post-epidemic period, with decreased Zika transmission and less public awareness,” wrote Dr. Mulkey and a colleague, “follow-up of these children is now more important than ever”.
A version of this article originally appeared on Medscape.com.
ACS disagrees with CDC on HPV vaccination in adults
The ACS has endorsed two recommendations made by the CDC’s Advisory Committee on Immunization Practices, but the ACS does not agree with a third recommendation for older adults.
The ACIP recommends shared clinical decision-making regarding human papillomavirus (HPV) vaccination in some adults aged 27-45 years who are not adequately vaccinated. The ACS does not endorse this recommendation “because of the low effectiveness and low cancer prevention potential of vaccination in this age group, the burden of decision-making on patients and clinicians, and the lack of sufficient guidance on the selection of individuals who might benefit,” wrote Debbie Saslow, PhD, of the ACS’s section on human papillomavirus and gynecologic cancers, and colleagues.
Dr. Saslow and colleagues detailed the ACS recommendations in CA: A Cancer Journal for Clinicians.
The HPV vaccine protects against the virus that can cause cervical, oropharyngeal, anal, vaginal, vulvar, and penile cancers. For younger people, the ACIP recommends routine HPV vaccination of boys and girls aged 9-12 years and catch-up vaccination in everyone up to age 26 who has not been fully immunized against HPV.
The ACS endorses both of these recommendations. It also advises clinicians to tell patients aged 22-26 years who haven’t received the HPV vaccine or completed the series that the vaccine is less effective at reducing the risk of cancer at older ages.
After the Food and Drug Administration approved the HPV vaccine for adults aged 27-45 years, the ACIP updated its recommendations to state that routine catch-up vaccination is not recommended for anyone aged over 26 years. However, the ACIP recommended that these older adults talk with their providers about the risks and benefits of the vaccine to determine whether to get it.
The ACS subsequently conducted a methodological review of the ACIP’s recommendations and published its own adapted guidance, stating that the ACS does not endorse the shared decision-making. Administering the HPV vaccine to adults aged over 26 years would only prevent an estimated 0.5% of additional cancer cases, 0.4% additional cases of cervical precancer, and 0.3% additional cases of genital warts over the next 100 years, compared with vaccination under age 26.
“In addition to the low effectiveness and low cancer prevention potential of vaccination in this age group, other considerations included the burden of decision-making on patients and clinicians and the lack of sufficient guidance on the selection of individuals who might benefit,” according to the guidance. The ACS also expressed concern that these provider-patient discussions could interfere with the public health goal of increasing HPV vaccination in younger people.
HPV vaccination rates have lagged substantially behind other routinely recommended childhood vaccinations. Just over half (51%) of U.S. teens aged 13-17 years were up to date with HPV vaccination, and 68% had received one dose of the vaccine in 2018, according to the National Immunization Survey.
It’s very uncommon for a professional medical organization to not endorse recommendations from the CDC, particularly with vaccines, according to Robert A. Bednarczyk, PhD, an assistant professor of public health at Emory University, Atlanta, who specializes in HPV vaccination research but was not involved with the ACS statement or the ACIP recommendations.
“Often, for vaccination recommendations, there is a harmonization between health care provider organizations, such as the American Academy of Pediatrics, American Academy of Family Physicians, etc., when new vaccination schedules are released,” Dr. Bednarczyk said.
He acknowledged the ACS’s reasons for not endorsing the ACIP’s HPV recommendations in older adults: the burden of shared decision-making given the communication issues, the vaccine’s lower effectiveness in this population, and the ongoing HPV vaccine shortage.
But Dr. Bednarczyk also pointed out that the ACIP’s recommendation opens the door to these discussions when they may actually be needed, such as in adults at greater risk for HPV. He cited data suggesting that, in 2015, divorces occurred in 24 out of 1,000 married people aged 25-39 years and 21 out of 1,000 people aged 40-49.
“When you consider these marriages that end, in addition to marriages that end when one spouse dies, there is a potential for individuals who previously had a low risk of HPV acquisition now entering into new potential sexual relationships,” Dr. Bednarczyk said. “Additionally, it has been estimated that approximately 4% of the U.S. population are in open or consensually nonmonogamous relationships, where exposure to more sexual partners may increase their risk for HPV. These are just some examples of where conversations with health care providers, and shared clinical decision-making, can help with a targeted reduction of HPV risk.”
The ACIP recommendation regarding adults aged 27-45 years also provides people in this age group with insurance coverage for the HPV vaccine if they choose to get it, Dr. Bednarczyk pointed out. Insurance companies may not be required to cover HPV vaccination in people aged over 26 years without the CDC’s recommendation, even if it’s not for routine immunization.
Dr. Bednarczyk agreed, however, with how the ACS adapted the CDC’s recommendation for routine vaccination in youth. The CDC’s routine recommendation is at ages 11-12 but can begin at 9 years, according to the ACIP. The ACS guidance qualifies this statement to place more emphasis on encouraging the vaccine earlier.
“Routine HPV vaccination between ages 9-12 is expected to achieve higher on-time vaccination rates, resulting in increased numbers of cancers prevented,” according to the ACS. “Health care providers are encouraged to start offering the HPV vaccine at age 9 or 10.”
Dr. Bednarczyk pointed to some of his past research finding low proportions of teens fully vaccinated against HPV by age 13 years (J Infect Dis. 2019 Jul 31;220[5]:730-4). Therefore, “any efforts to encourage vaccination, including starting the series at ages 9-10 years may help,” he said.
He also agreed that there may be diminished effectiveness with vaccinating adults aged 22-26, “but this should also be considered relative to an individual’s risk of acquiring HPV.”
While an HPV vaccine shortage is a major concern and HPV vaccination efforts should remain most focused on young teens, adults should not necessarily be neglected, Dr. Bednarczyk noted.
“Given how common HPV infection is in the population, open discussion between patients and health care providers can help identify those adults for whom HPV vaccination can be effective,” he said.
The development of the ACS guideline was supported by ACS operational funds. The ACS has received an independent educational grant from Merck Sharp & Dohme for a project intended to increase HPV vaccination rates. Dr. Saslow is the principal investigator for a cooperative agreement between the ACS and the CDC to support the National HPV Vaccination Roundtable and is coprincipal investigator of a cooperative agreement between the ACS and CDC to support initiatives to increase HPV vaccination. The remaining authors and Dr. Bednarczyk reported no relevant disclosures.
SOURCE: Saslow D et al. CA Cancer J Clin. 2020 Jul 8. doi: 10.3322/caac.21616.
The ACS has endorsed two recommendations made by the CDC’s Advisory Committee on Immunization Practices, but the ACS does not agree with a third recommendation for older adults.
The ACIP recommends shared clinical decision-making regarding human papillomavirus (HPV) vaccination in some adults aged 27-45 years who are not adequately vaccinated. The ACS does not endorse this recommendation “because of the low effectiveness and low cancer prevention potential of vaccination in this age group, the burden of decision-making on patients and clinicians, and the lack of sufficient guidance on the selection of individuals who might benefit,” wrote Debbie Saslow, PhD, of the ACS’s section on human papillomavirus and gynecologic cancers, and colleagues.
Dr. Saslow and colleagues detailed the ACS recommendations in CA: A Cancer Journal for Clinicians.
The HPV vaccine protects against the virus that can cause cervical, oropharyngeal, anal, vaginal, vulvar, and penile cancers. For younger people, the ACIP recommends routine HPV vaccination of boys and girls aged 9-12 years and catch-up vaccination in everyone up to age 26 who has not been fully immunized against HPV.
The ACS endorses both of these recommendations. It also advises clinicians to tell patients aged 22-26 years who haven’t received the HPV vaccine or completed the series that the vaccine is less effective at reducing the risk of cancer at older ages.
After the Food and Drug Administration approved the HPV vaccine for adults aged 27-45 years, the ACIP updated its recommendations to state that routine catch-up vaccination is not recommended for anyone aged over 26 years. However, the ACIP recommended that these older adults talk with their providers about the risks and benefits of the vaccine to determine whether to get it.
The ACS subsequently conducted a methodological review of the ACIP’s recommendations and published its own adapted guidance, stating that the ACS does not endorse the shared decision-making. Administering the HPV vaccine to adults aged over 26 years would only prevent an estimated 0.5% of additional cancer cases, 0.4% additional cases of cervical precancer, and 0.3% additional cases of genital warts over the next 100 years, compared with vaccination under age 26.
“In addition to the low effectiveness and low cancer prevention potential of vaccination in this age group, other considerations included the burden of decision-making on patients and clinicians and the lack of sufficient guidance on the selection of individuals who might benefit,” according to the guidance. The ACS also expressed concern that these provider-patient discussions could interfere with the public health goal of increasing HPV vaccination in younger people.
HPV vaccination rates have lagged substantially behind other routinely recommended childhood vaccinations. Just over half (51%) of U.S. teens aged 13-17 years were up to date with HPV vaccination, and 68% had received one dose of the vaccine in 2018, according to the National Immunization Survey.
It’s very uncommon for a professional medical organization to not endorse recommendations from the CDC, particularly with vaccines, according to Robert A. Bednarczyk, PhD, an assistant professor of public health at Emory University, Atlanta, who specializes in HPV vaccination research but was not involved with the ACS statement or the ACIP recommendations.
“Often, for vaccination recommendations, there is a harmonization between health care provider organizations, such as the American Academy of Pediatrics, American Academy of Family Physicians, etc., when new vaccination schedules are released,” Dr. Bednarczyk said.
He acknowledged the ACS’s reasons for not endorsing the ACIP’s HPV recommendations in older adults: the burden of shared decision-making given the communication issues, the vaccine’s lower effectiveness in this population, and the ongoing HPV vaccine shortage.
But Dr. Bednarczyk also pointed out that the ACIP’s recommendation opens the door to these discussions when they may actually be needed, such as in adults at greater risk for HPV. He cited data suggesting that, in 2015, divorces occurred in 24 out of 1,000 married people aged 25-39 years and 21 out of 1,000 people aged 40-49.
“When you consider these marriages that end, in addition to marriages that end when one spouse dies, there is a potential for individuals who previously had a low risk of HPV acquisition now entering into new potential sexual relationships,” Dr. Bednarczyk said. “Additionally, it has been estimated that approximately 4% of the U.S. population are in open or consensually nonmonogamous relationships, where exposure to more sexual partners may increase their risk for HPV. These are just some examples of where conversations with health care providers, and shared clinical decision-making, can help with a targeted reduction of HPV risk.”
The ACIP recommendation regarding adults aged 27-45 years also provides people in this age group with insurance coverage for the HPV vaccine if they choose to get it, Dr. Bednarczyk pointed out. Insurance companies may not be required to cover HPV vaccination in people aged over 26 years without the CDC’s recommendation, even if it’s not for routine immunization.
Dr. Bednarczyk agreed, however, with how the ACS adapted the CDC’s recommendation for routine vaccination in youth. The CDC’s routine recommendation is at ages 11-12 but can begin at 9 years, according to the ACIP. The ACS guidance qualifies this statement to place more emphasis on encouraging the vaccine earlier.
“Routine HPV vaccination between ages 9-12 is expected to achieve higher on-time vaccination rates, resulting in increased numbers of cancers prevented,” according to the ACS. “Health care providers are encouraged to start offering the HPV vaccine at age 9 or 10.”
Dr. Bednarczyk pointed to some of his past research finding low proportions of teens fully vaccinated against HPV by age 13 years (J Infect Dis. 2019 Jul 31;220[5]:730-4). Therefore, “any efforts to encourage vaccination, including starting the series at ages 9-10 years may help,” he said.
He also agreed that there may be diminished effectiveness with vaccinating adults aged 22-26, “but this should also be considered relative to an individual’s risk of acquiring HPV.”
While an HPV vaccine shortage is a major concern and HPV vaccination efforts should remain most focused on young teens, adults should not necessarily be neglected, Dr. Bednarczyk noted.
“Given how common HPV infection is in the population, open discussion between patients and health care providers can help identify those adults for whom HPV vaccination can be effective,” he said.
The development of the ACS guideline was supported by ACS operational funds. The ACS has received an independent educational grant from Merck Sharp & Dohme for a project intended to increase HPV vaccination rates. Dr. Saslow is the principal investigator for a cooperative agreement between the ACS and the CDC to support the National HPV Vaccination Roundtable and is coprincipal investigator of a cooperative agreement between the ACS and CDC to support initiatives to increase HPV vaccination. The remaining authors and Dr. Bednarczyk reported no relevant disclosures.
SOURCE: Saslow D et al. CA Cancer J Clin. 2020 Jul 8. doi: 10.3322/caac.21616.
The ACS has endorsed two recommendations made by the CDC’s Advisory Committee on Immunization Practices, but the ACS does not agree with a third recommendation for older adults.
The ACIP recommends shared clinical decision-making regarding human papillomavirus (HPV) vaccination in some adults aged 27-45 years who are not adequately vaccinated. The ACS does not endorse this recommendation “because of the low effectiveness and low cancer prevention potential of vaccination in this age group, the burden of decision-making on patients and clinicians, and the lack of sufficient guidance on the selection of individuals who might benefit,” wrote Debbie Saslow, PhD, of the ACS’s section on human papillomavirus and gynecologic cancers, and colleagues.
Dr. Saslow and colleagues detailed the ACS recommendations in CA: A Cancer Journal for Clinicians.
The HPV vaccine protects against the virus that can cause cervical, oropharyngeal, anal, vaginal, vulvar, and penile cancers. For younger people, the ACIP recommends routine HPV vaccination of boys and girls aged 9-12 years and catch-up vaccination in everyone up to age 26 who has not been fully immunized against HPV.
The ACS endorses both of these recommendations. It also advises clinicians to tell patients aged 22-26 years who haven’t received the HPV vaccine or completed the series that the vaccine is less effective at reducing the risk of cancer at older ages.
After the Food and Drug Administration approved the HPV vaccine for adults aged 27-45 years, the ACIP updated its recommendations to state that routine catch-up vaccination is not recommended for anyone aged over 26 years. However, the ACIP recommended that these older adults talk with their providers about the risks and benefits of the vaccine to determine whether to get it.
The ACS subsequently conducted a methodological review of the ACIP’s recommendations and published its own adapted guidance, stating that the ACS does not endorse the shared decision-making. Administering the HPV vaccine to adults aged over 26 years would only prevent an estimated 0.5% of additional cancer cases, 0.4% additional cases of cervical precancer, and 0.3% additional cases of genital warts over the next 100 years, compared with vaccination under age 26.
“In addition to the low effectiveness and low cancer prevention potential of vaccination in this age group, other considerations included the burden of decision-making on patients and clinicians and the lack of sufficient guidance on the selection of individuals who might benefit,” according to the guidance. The ACS also expressed concern that these provider-patient discussions could interfere with the public health goal of increasing HPV vaccination in younger people.
HPV vaccination rates have lagged substantially behind other routinely recommended childhood vaccinations. Just over half (51%) of U.S. teens aged 13-17 years were up to date with HPV vaccination, and 68% had received one dose of the vaccine in 2018, according to the National Immunization Survey.
It’s very uncommon for a professional medical organization to not endorse recommendations from the CDC, particularly with vaccines, according to Robert A. Bednarczyk, PhD, an assistant professor of public health at Emory University, Atlanta, who specializes in HPV vaccination research but was not involved with the ACS statement or the ACIP recommendations.
“Often, for vaccination recommendations, there is a harmonization between health care provider organizations, such as the American Academy of Pediatrics, American Academy of Family Physicians, etc., when new vaccination schedules are released,” Dr. Bednarczyk said.
He acknowledged the ACS’s reasons for not endorsing the ACIP’s HPV recommendations in older adults: the burden of shared decision-making given the communication issues, the vaccine’s lower effectiveness in this population, and the ongoing HPV vaccine shortage.
But Dr. Bednarczyk also pointed out that the ACIP’s recommendation opens the door to these discussions when they may actually be needed, such as in adults at greater risk for HPV. He cited data suggesting that, in 2015, divorces occurred in 24 out of 1,000 married people aged 25-39 years and 21 out of 1,000 people aged 40-49.
“When you consider these marriages that end, in addition to marriages that end when one spouse dies, there is a potential for individuals who previously had a low risk of HPV acquisition now entering into new potential sexual relationships,” Dr. Bednarczyk said. “Additionally, it has been estimated that approximately 4% of the U.S. population are in open or consensually nonmonogamous relationships, where exposure to more sexual partners may increase their risk for HPV. These are just some examples of where conversations with health care providers, and shared clinical decision-making, can help with a targeted reduction of HPV risk.”
The ACIP recommendation regarding adults aged 27-45 years also provides people in this age group with insurance coverage for the HPV vaccine if they choose to get it, Dr. Bednarczyk pointed out. Insurance companies may not be required to cover HPV vaccination in people aged over 26 years without the CDC’s recommendation, even if it’s not for routine immunization.
Dr. Bednarczyk agreed, however, with how the ACS adapted the CDC’s recommendation for routine vaccination in youth. The CDC’s routine recommendation is at ages 11-12 but can begin at 9 years, according to the ACIP. The ACS guidance qualifies this statement to place more emphasis on encouraging the vaccine earlier.
“Routine HPV vaccination between ages 9-12 is expected to achieve higher on-time vaccination rates, resulting in increased numbers of cancers prevented,” according to the ACS. “Health care providers are encouraged to start offering the HPV vaccine at age 9 or 10.”
Dr. Bednarczyk pointed to some of his past research finding low proportions of teens fully vaccinated against HPV by age 13 years (J Infect Dis. 2019 Jul 31;220[5]:730-4). Therefore, “any efforts to encourage vaccination, including starting the series at ages 9-10 years may help,” he said.
He also agreed that there may be diminished effectiveness with vaccinating adults aged 22-26, “but this should also be considered relative to an individual’s risk of acquiring HPV.”
While an HPV vaccine shortage is a major concern and HPV vaccination efforts should remain most focused on young teens, adults should not necessarily be neglected, Dr. Bednarczyk noted.
“Given how common HPV infection is in the population, open discussion between patients and health care providers can help identify those adults for whom HPV vaccination can be effective,” he said.
The development of the ACS guideline was supported by ACS operational funds. The ACS has received an independent educational grant from Merck Sharp & Dohme for a project intended to increase HPV vaccination rates. Dr. Saslow is the principal investigator for a cooperative agreement between the ACS and the CDC to support the National HPV Vaccination Roundtable and is coprincipal investigator of a cooperative agreement between the ACS and CDC to support initiatives to increase HPV vaccination. The remaining authors and Dr. Bednarczyk reported no relevant disclosures.
SOURCE: Saslow D et al. CA Cancer J Clin. 2020 Jul 8. doi: 10.3322/caac.21616.
FROM CA: A CANCER JOURNAL FOR CLINICIANS
One-week postsurgical interval for voiding trial increases pass rate
Women who underwent vaginal prolapse surgery and did not immediately have a successful voiding trial were seven times more likely to pass their second voiding trial if their follow-up was 7 days after surgery instead of 4 days, according to a study in the American Journal of Obstetrics and Gynecology.
“This information is useful for setting expectations and for counseling patients on when it might be best to repeat a voiding trial in those with transient incomplete bladder emptying on the day of surgery, especially for those who may not live close to their surgeon, or for those who have difficulty traveling to the office,” said Jeffrey S. Schachar, MD, of Wake Forest Baptist Health in Winston-Salem, N.C., and colleagues. “Despite a higher rate of initial unsuccessful office voiding trials, however, the early group did have significantly fewer days with an indwelling transurethral catheter, as well as total catheterization days,” including self-catheterization.
The researchers note that rates of temporary use of catheters after surgery vary widely, from 12% to 83%, likely because no consensus exists on how long to wait for voiding trials and what constitutes a successful trial.
“It is critical to identify patients with incomplete bladder emptying in order to prevent pain, myogenic and neurogenic damage, ureteral reflux and bladder overdistension that may further impair voiding function,” the authors wrote. “However, extending bladder drainage beyond the necessary recovery period may be associated with higher rates of urinary tract infection (UTI) and patient bother.”
To learn more about the best duration for postoperative catheter use, the researchers enrolled 102 patients before they underwent vaginal prolapse surgery at Wake Forest Baptist Health and Cleveland Clinic Florida from February 2017 to November 2019. The 29 patients with a successful voiding trial within 6 hours after surgery left the study, and 5 others were excluded for needing longer vaginal packing.
The voiding trial involved helping the patient stand to drain the bladder via the catheter, backfilling the bladder with 300 mL of saline solution through the catheter, removing the catheter to give women 1 hour to urinate, and then measuring the postvoid residual with a catheter or ultrasound. At least 100 mL postvoid residual was considered persistent incomplete bladder emptying.
The 60 remaining patients who did not pass the initial voiding trial and opted to remain in the study received a transurethral indwelling catheter and were randomly assigned to return for a second voiding trial either 2-4 days after surgery (depending on day of the week) or 7 days after surgery. The groups were demographically and clinically similar, with predominantly white postmenopausal, non-smoking women with stage II or III multicompartment pelvic organ prolapse.
Women without successful trials could continue with the transurethral catheter or give themselves intermittent catheterizations with a follow-up schedule determined by their surgeon. The researchers then tracked the women for 6 weeks to determine the rate of unsuccessful repeat voiding trials.
Among the women who returned 2-4 days post surgery, 23% had unsuccessful follow-up voiding trials, compared with 3% in the group returning 7 days after surgery (relative risk = 7; P = .02). The researchers calculated that one case of persistent postoperative incomplete bladder emptying was prevented for every five patients who used a catheter for 7 days after surgery.
Kevin A. Ault, MD, professor of obstetrics and gynecology at the University of Kansas Medical Center in Kansas City, said the study was well done, although the findings were unsurprising. He said the clinical implication is straightforward – to wait a week before doing a second voiding trial.
“I suspect these findings match the clinical experience of many surgeons. It is always good to see a well-done clinical trial on a topic,” Dr Ault said in an interview. “The most notable finding is how this impacts patient counseling. Gynecologists should tell their patients that it will take a week with a catheter when this problem arises.”
“The main limitation is whether this finding can be extrapolated to other gynecological surgeries, such as hysterectomy,” said Dr. Ault, who was not involved in the study. “Urinary retention is likely less common after that surgery, but it is still bothersome to patients.”
Dr. Schachar and associates also reported that patients in the earlier group “used significantly more morphine dose equivalents within 24 hours of the office voiding trial than the late-voiding trial group, which was expected given the proximity to surgery” (3 vs. 0.38; P = .005). However, new postoperative pain medication prescriptions and refills were similar in both groups.
Secondary endpoints included UTI rates, total days with a catheter, and patient experience of discomfort with the catheter. The two groups of women reported similar levels of catheter bother, but there was a nonsignificant difference in UTI rates: 23% in the earlier group, compared with 7% in the later group (P = .07).
The early-voiding trial group had an average 5 days with an indwelling transurethral catheter, compared with a significantly different 7 days in the later group (P = .0007). The early group also had fewer total days with an indwelling transurethral catheter and self-catheterization (6 days), compared with the late group (7 days; P = .0013). No patients had persistent incomplete bladder emptying after 17 days post surgery.
“Being able to adequately predict which patients are more likely to have unsuccessful postoperative voiding trials allows surgeons to better counsel their patients and may guide clinical decisions,” Dr. Schachar and associates said. They acknowledged, however, that their study’s biggest weakness is the small enrollment, which led to larger confidence intervals related to relative risk differences between the groups.
The study did not use external funding. Four of the investigators received grant, research funding, or honoraria from one or many medical device or pharmaceutical companies. The remaining researchers had no disclosures. Dr. Ault said he had no relevant financial disclosures.
SOURCE: Schachar JS et al. Am J Obstet Gynecol. 2020 Jun. doi: 10.1016/j.ajog.2020.06.001.
Women who underwent vaginal prolapse surgery and did not immediately have a successful voiding trial were seven times more likely to pass their second voiding trial if their follow-up was 7 days after surgery instead of 4 days, according to a study in the American Journal of Obstetrics and Gynecology.
“This information is useful for setting expectations and for counseling patients on when it might be best to repeat a voiding trial in those with transient incomplete bladder emptying on the day of surgery, especially for those who may not live close to their surgeon, or for those who have difficulty traveling to the office,” said Jeffrey S. Schachar, MD, of Wake Forest Baptist Health in Winston-Salem, N.C., and colleagues. “Despite a higher rate of initial unsuccessful office voiding trials, however, the early group did have significantly fewer days with an indwelling transurethral catheter, as well as total catheterization days,” including self-catheterization.
The researchers note that rates of temporary use of catheters after surgery vary widely, from 12% to 83%, likely because no consensus exists on how long to wait for voiding trials and what constitutes a successful trial.
“It is critical to identify patients with incomplete bladder emptying in order to prevent pain, myogenic and neurogenic damage, ureteral reflux and bladder overdistension that may further impair voiding function,” the authors wrote. “However, extending bladder drainage beyond the necessary recovery period may be associated with higher rates of urinary tract infection (UTI) and patient bother.”
To learn more about the best duration for postoperative catheter use, the researchers enrolled 102 patients before they underwent vaginal prolapse surgery at Wake Forest Baptist Health and Cleveland Clinic Florida from February 2017 to November 2019. The 29 patients with a successful voiding trial within 6 hours after surgery left the study, and 5 others were excluded for needing longer vaginal packing.
The voiding trial involved helping the patient stand to drain the bladder via the catheter, backfilling the bladder with 300 mL of saline solution through the catheter, removing the catheter to give women 1 hour to urinate, and then measuring the postvoid residual with a catheter or ultrasound. At least 100 mL postvoid residual was considered persistent incomplete bladder emptying.
The 60 remaining patients who did not pass the initial voiding trial and opted to remain in the study received a transurethral indwelling catheter and were randomly assigned to return for a second voiding trial either 2-4 days after surgery (depending on day of the week) or 7 days after surgery. The groups were demographically and clinically similar, with predominantly white postmenopausal, non-smoking women with stage II or III multicompartment pelvic organ prolapse.
Women without successful trials could continue with the transurethral catheter or give themselves intermittent catheterizations with a follow-up schedule determined by their surgeon. The researchers then tracked the women for 6 weeks to determine the rate of unsuccessful repeat voiding trials.
Among the women who returned 2-4 days post surgery, 23% had unsuccessful follow-up voiding trials, compared with 3% in the group returning 7 days after surgery (relative risk = 7; P = .02). The researchers calculated that one case of persistent postoperative incomplete bladder emptying was prevented for every five patients who used a catheter for 7 days after surgery.
Kevin A. Ault, MD, professor of obstetrics and gynecology at the University of Kansas Medical Center in Kansas City, said the study was well done, although the findings were unsurprising. He said the clinical implication is straightforward – to wait a week before doing a second voiding trial.
“I suspect these findings match the clinical experience of many surgeons. It is always good to see a well-done clinical trial on a topic,” Dr Ault said in an interview. “The most notable finding is how this impacts patient counseling. Gynecologists should tell their patients that it will take a week with a catheter when this problem arises.”
“The main limitation is whether this finding can be extrapolated to other gynecological surgeries, such as hysterectomy,” said Dr. Ault, who was not involved in the study. “Urinary retention is likely less common after that surgery, but it is still bothersome to patients.”
Dr. Schachar and associates also reported that patients in the earlier group “used significantly more morphine dose equivalents within 24 hours of the office voiding trial than the late-voiding trial group, which was expected given the proximity to surgery” (3 vs. 0.38; P = .005). However, new postoperative pain medication prescriptions and refills were similar in both groups.
Secondary endpoints included UTI rates, total days with a catheter, and patient experience of discomfort with the catheter. The two groups of women reported similar levels of catheter bother, but there was a nonsignificant difference in UTI rates: 23% in the earlier group, compared with 7% in the later group (P = .07).
The early-voiding trial group had an average 5 days with an indwelling transurethral catheter, compared with a significantly different 7 days in the later group (P = .0007). The early group also had fewer total days with an indwelling transurethral catheter and self-catheterization (6 days), compared with the late group (7 days; P = .0013). No patients had persistent incomplete bladder emptying after 17 days post surgery.
“Being able to adequately predict which patients are more likely to have unsuccessful postoperative voiding trials allows surgeons to better counsel their patients and may guide clinical decisions,” Dr. Schachar and associates said. They acknowledged, however, that their study’s biggest weakness is the small enrollment, which led to larger confidence intervals related to relative risk differences between the groups.
The study did not use external funding. Four of the investigators received grant, research funding, or honoraria from one or many medical device or pharmaceutical companies. The remaining researchers had no disclosures. Dr. Ault said he had no relevant financial disclosures.
SOURCE: Schachar JS et al. Am J Obstet Gynecol. 2020 Jun. doi: 10.1016/j.ajog.2020.06.001.
Women who underwent vaginal prolapse surgery and did not immediately have a successful voiding trial were seven times more likely to pass their second voiding trial if their follow-up was 7 days after surgery instead of 4 days, according to a study in the American Journal of Obstetrics and Gynecology.
“This information is useful for setting expectations and for counseling patients on when it might be best to repeat a voiding trial in those with transient incomplete bladder emptying on the day of surgery, especially for those who may not live close to their surgeon, or for those who have difficulty traveling to the office,” said Jeffrey S. Schachar, MD, of Wake Forest Baptist Health in Winston-Salem, N.C., and colleagues. “Despite a higher rate of initial unsuccessful office voiding trials, however, the early group did have significantly fewer days with an indwelling transurethral catheter, as well as total catheterization days,” including self-catheterization.
The researchers note that rates of temporary use of catheters after surgery vary widely, from 12% to 83%, likely because no consensus exists on how long to wait for voiding trials and what constitutes a successful trial.
“It is critical to identify patients with incomplete bladder emptying in order to prevent pain, myogenic and neurogenic damage, ureteral reflux and bladder overdistension that may further impair voiding function,” the authors wrote. “However, extending bladder drainage beyond the necessary recovery period may be associated with higher rates of urinary tract infection (UTI) and patient bother.”
To learn more about the best duration for postoperative catheter use, the researchers enrolled 102 patients before they underwent vaginal prolapse surgery at Wake Forest Baptist Health and Cleveland Clinic Florida from February 2017 to November 2019. The 29 patients with a successful voiding trial within 6 hours after surgery left the study, and 5 others were excluded for needing longer vaginal packing.
The voiding trial involved helping the patient stand to drain the bladder via the catheter, backfilling the bladder with 300 mL of saline solution through the catheter, removing the catheter to give women 1 hour to urinate, and then measuring the postvoid residual with a catheter or ultrasound. At least 100 mL postvoid residual was considered persistent incomplete bladder emptying.
The 60 remaining patients who did not pass the initial voiding trial and opted to remain in the study received a transurethral indwelling catheter and were randomly assigned to return for a second voiding trial either 2-4 days after surgery (depending on day of the week) or 7 days after surgery. The groups were demographically and clinically similar, with predominantly white postmenopausal, non-smoking women with stage II or III multicompartment pelvic organ prolapse.
Women without successful trials could continue with the transurethral catheter or give themselves intermittent catheterizations with a follow-up schedule determined by their surgeon. The researchers then tracked the women for 6 weeks to determine the rate of unsuccessful repeat voiding trials.
Among the women who returned 2-4 days post surgery, 23% had unsuccessful follow-up voiding trials, compared with 3% in the group returning 7 days after surgery (relative risk = 7; P = .02). The researchers calculated that one case of persistent postoperative incomplete bladder emptying was prevented for every five patients who used a catheter for 7 days after surgery.
Kevin A. Ault, MD, professor of obstetrics and gynecology at the University of Kansas Medical Center in Kansas City, said the study was well done, although the findings were unsurprising. He said the clinical implication is straightforward – to wait a week before doing a second voiding trial.
“I suspect these findings match the clinical experience of many surgeons. It is always good to see a well-done clinical trial on a topic,” Dr Ault said in an interview. “The most notable finding is how this impacts patient counseling. Gynecologists should tell their patients that it will take a week with a catheter when this problem arises.”
“The main limitation is whether this finding can be extrapolated to other gynecological surgeries, such as hysterectomy,” said Dr. Ault, who was not involved in the study. “Urinary retention is likely less common after that surgery, but it is still bothersome to patients.”
Dr. Schachar and associates also reported that patients in the earlier group “used significantly more morphine dose equivalents within 24 hours of the office voiding trial than the late-voiding trial group, which was expected given the proximity to surgery” (3 vs. 0.38; P = .005). However, new postoperative pain medication prescriptions and refills were similar in both groups.
Secondary endpoints included UTI rates, total days with a catheter, and patient experience of discomfort with the catheter. The two groups of women reported similar levels of catheter bother, but there was a nonsignificant difference in UTI rates: 23% in the earlier group, compared with 7% in the later group (P = .07).
The early-voiding trial group had an average 5 days with an indwelling transurethral catheter, compared with a significantly different 7 days in the later group (P = .0007). The early group also had fewer total days with an indwelling transurethral catheter and self-catheterization (6 days), compared with the late group (7 days; P = .0013). No patients had persistent incomplete bladder emptying after 17 days post surgery.
“Being able to adequately predict which patients are more likely to have unsuccessful postoperative voiding trials allows surgeons to better counsel their patients and may guide clinical decisions,” Dr. Schachar and associates said. They acknowledged, however, that their study’s biggest weakness is the small enrollment, which led to larger confidence intervals related to relative risk differences between the groups.
The study did not use external funding. Four of the investigators received grant, research funding, or honoraria from one or many medical device or pharmaceutical companies. The remaining researchers had no disclosures. Dr. Ault said he had no relevant financial disclosures.
SOURCE: Schachar JS et al. Am J Obstet Gynecol. 2020 Jun. doi: 10.1016/j.ajog.2020.06.001.
FROM AMERICAN JOURNAL OF OBSTETRICS & GYNECOLOGY
Sepsis readmissions risk linked to residence in a poor neighborhoods
according to a study published in Critical Care Medicine.
The association between living in a disadvantaged neighborhood and 30-day readmission remained significant even after adjustment for “individual demographic variables, active tobacco use, length of index hospitalization, severity of acute and chronic morbidity, and place of initial discharge,” wrote Panagis Galiatsatos, MD, of Johns Hopkins University in Baltimore, and colleagues.
“Our findings suggest the need for interventions that emphasize neighborhood-level socioeconomic variables in addition to individual-level efforts in an effort to promote and achieve health equity for patients who survive a hospitalization due to sepsis,” the authors wrote. “With a third of our cohort rehospitalized with infections, and other studies emphasizing that the most common readmission diagnosis was infection, attention toward both anticipating and attenuating the risk of infection in sepsis survivors, especially among those who live in higher risk neighborhoods, must be a priority for the prevention of readmissions.”
Although she did not find the study results surprising, Eva DuGoff, PhD, a senior managing consultant with the Berkeley Research Group and a visiting assistant professor at University of Maryland School of Public Health, College Park, said in an interview that she was impressed with how clinically rigorous the analysis was, both in confirming an accurate sepsis diagnosis and in using the more refined measure of the Area Deprivation Index (ADI) to assess neighborhood disadvantage.
“I think it makes sense that people who have less means and are in neighborhoods with fewer resources would run into more issues and would need to return to the hospital, above and beyond the clinical risk factors, such as smoking and chronic conditions,” said Dr. DuGoff, who studies health disparities but was not involved in this study.
Shayla N.M. Durfey MD, ScM, a pediatric resident at Hasbro Children’s Hospital in Providence, R.I., said in an interview she was similarly unsurprised by the findings.
“People who live in disadvantaged neighborhoods may have less access to walking spaces, healthy food, and safe housing and more exposure to poor air quality, toxic stress, and violence – any of which can negatively impact health or recovery from illness through stress responses, nutritional deficiencies, or comorbidities, such as reactive airway disease, obesity, hypertension, and diabetes,” said Dr. Durfey, who studies health disparities but was not involved in this study. “Our research has found these neighborhood-level factors often matter above and beyond individual social determinants of health.”
Dr. Galiatsatos and associates conducted a retrospective study in Baltimore that compared readmission rates in 2017 at Johns Hopkins Bayview Medical Center among patients discharged after a hospitalization for sepsis, coded via ICD-10. They relied on the ADI to categorize the neighborhoods of patients’ residential addresses. The ADI rates various socioeconomic components, including income, education, employment, and housing characteristics, on a scale of 1-100 in geographic blocks, with higher score indicating a greater level of disadvantage.
Among 647 hospitalized patients with an ICD-10 code of sepsis who also met criteria for sepsis or septic shock per the Sepsis-3 definition, 17.9% were excluded from the analysis because they died or were transferred to hospice care. The other 531 patients had an average age of 61, and just under one-third (30.9%) were active smokers. Their average length of stay was 6.9 days, with a mean Charlson Comorbidity Index of 4.2 and a mean Sequential Organ Failure Assessment score of 4.9.
The average ADI for all the patients was 54.2, but the average score was 63 for the 22% of patients who were readmitted within 30 days of initial discharge, compared with an average 51.8 for patients not readmitted (P < .001).
Among those 117 readmitted, “39 patients had a reinfection, 68 had an exacerbation of their chronic conditions, and 10 were admitted for ‘concerning symptoms’ without a primary admitting diagnosis,” the investigators reported. Because “a third of our cohort was readmitted with an infection, it is possible that more disadvantaged neighborhoods created more challenges for a person’s immune system, which may be compromised after recovering from sepsis.”
Dr. DuGoff further noted that health literacy may be lower among people living in less advantaged neighborhoods.
“A number of studies suggest when patients leave the hospital, they’re not sure what they need to do. The language is complicated, and it’s hard to know what kind of medication to take when, and when you’re supposed to return to the doctor or the hospital,” Dr. DuGoff said. “Managing all of that can be pretty scary for people, particularly after a traumatic experience with sepsis at the hospital.”
Most patients had been discharged home (67.3%), but the 31.6% discharged to a skilled nursing facility had a greater likelihood of readmission, compared with those discharged home (P < .01); 1% were discharged to acute rehabilitation. The average length of stay during the index hospitalization was also greater for those readmitted (8.7 days) than for those not readmitted (6.4 days). The groups did not differ in terms of their acute organ dysfunction or severity of their comorbidities.
However, even after adjustment for these factors, “neighborhood disadvantage remained significantly associated with 30-day rehospitalization in patients who were discharged with sepsis,” the authors said. Specifically, each additional standard deviation greater in patients’ ADI was associated with increased risk of 30-day readmission (P < .001).
“Given that the ADI is a composite score, we cannot identify which component is the predominant driver of rehospitalizations for patients who survive sepsis,” the authors wrote. “However, all components that make up the index are intertwined, and policy efforts targeting one (i.e., unemployment) will likely impact others (i.e., housing).”
Dr. Durfey said that medical schools have not traditionally provided training related to management of social risk factors, although this is changing in more recent curricula. But the findings still have clinical relevance for practitioners.
“Certainly, the first step is awareness of where and how patients live and being mindful of how treatment plans may be impacted by social factors at both the individual and community levels,” Dr. Durfey said. “An important part of this is working in partnership with social workers and case managers. Importantly, clinicians can also partner with disadvantaged communities to advocate for improved conditions through policy change and act as expert witnesses to how neighborhood level factors impact health.”
Dr. DuGoff also wondered what implications these findings might have currently, with regards to COVID-19.
“People living in disadvantaged neighborhoods are already at higher risk for getting the disease, and this study raises really good questions about how we should be monitoring discharge now in anticipation of these types of issues,” she said.
The authors noted that their study is cross-sectional and cannot indicate causation, and the findings of a single urban institution may not be generalizable elsewhere. They also did not consider what interventions individual patients had during their index hospitalization that could have increased frailty.
The study did not note external funding. One coauthor of the study, Suchi Saria, PhD, reported receiving honoraria and travel reimbursement from two dozen biotechnology companies for keynotes and advisory board service; she also holds equity in Patient Ping and Bayesian Health. The other authors reported no industry disclosures. In addition to consulting for Berkeley Research Group, Dr. DuGoff has received a past honorarium from Zimmer Biomet. Dr. Durfey has no disclosures.
SOURCE: Galiatsatos P et al. Crit Care Med. 2020 Jun;48(6):808-14.
according to a study published in Critical Care Medicine.
The association between living in a disadvantaged neighborhood and 30-day readmission remained significant even after adjustment for “individual demographic variables, active tobacco use, length of index hospitalization, severity of acute and chronic morbidity, and place of initial discharge,” wrote Panagis Galiatsatos, MD, of Johns Hopkins University in Baltimore, and colleagues.
“Our findings suggest the need for interventions that emphasize neighborhood-level socioeconomic variables in addition to individual-level efforts in an effort to promote and achieve health equity for patients who survive a hospitalization due to sepsis,” the authors wrote. “With a third of our cohort rehospitalized with infections, and other studies emphasizing that the most common readmission diagnosis was infection, attention toward both anticipating and attenuating the risk of infection in sepsis survivors, especially among those who live in higher risk neighborhoods, must be a priority for the prevention of readmissions.”
Although she did not find the study results surprising, Eva DuGoff, PhD, a senior managing consultant with the Berkeley Research Group and a visiting assistant professor at University of Maryland School of Public Health, College Park, said in an interview that she was impressed with how clinically rigorous the analysis was, both in confirming an accurate sepsis diagnosis and in using the more refined measure of the Area Deprivation Index (ADI) to assess neighborhood disadvantage.
“I think it makes sense that people who have less means and are in neighborhoods with fewer resources would run into more issues and would need to return to the hospital, above and beyond the clinical risk factors, such as smoking and chronic conditions,” said Dr. DuGoff, who studies health disparities but was not involved in this study.
Shayla N.M. Durfey MD, ScM, a pediatric resident at Hasbro Children’s Hospital in Providence, R.I., said in an interview she was similarly unsurprised by the findings.
“People who live in disadvantaged neighborhoods may have less access to walking spaces, healthy food, and safe housing and more exposure to poor air quality, toxic stress, and violence – any of which can negatively impact health or recovery from illness through stress responses, nutritional deficiencies, or comorbidities, such as reactive airway disease, obesity, hypertension, and diabetes,” said Dr. Durfey, who studies health disparities but was not involved in this study. “Our research has found these neighborhood-level factors often matter above and beyond individual social determinants of health.”
Dr. Galiatsatos and associates conducted a retrospective study in Baltimore that compared readmission rates in 2017 at Johns Hopkins Bayview Medical Center among patients discharged after a hospitalization for sepsis, coded via ICD-10. They relied on the ADI to categorize the neighborhoods of patients’ residential addresses. The ADI rates various socioeconomic components, including income, education, employment, and housing characteristics, on a scale of 1-100 in geographic blocks, with higher score indicating a greater level of disadvantage.
Among 647 hospitalized patients with an ICD-10 code of sepsis who also met criteria for sepsis or septic shock per the Sepsis-3 definition, 17.9% were excluded from the analysis because they died or were transferred to hospice care. The other 531 patients had an average age of 61, and just under one-third (30.9%) were active smokers. Their average length of stay was 6.9 days, with a mean Charlson Comorbidity Index of 4.2 and a mean Sequential Organ Failure Assessment score of 4.9.
The average ADI for all the patients was 54.2, but the average score was 63 for the 22% of patients who were readmitted within 30 days of initial discharge, compared with an average 51.8 for patients not readmitted (P < .001).
Among those 117 readmitted, “39 patients had a reinfection, 68 had an exacerbation of their chronic conditions, and 10 were admitted for ‘concerning symptoms’ without a primary admitting diagnosis,” the investigators reported. Because “a third of our cohort was readmitted with an infection, it is possible that more disadvantaged neighborhoods created more challenges for a person’s immune system, which may be compromised after recovering from sepsis.”
Dr. DuGoff further noted that health literacy may be lower among people living in less advantaged neighborhoods.
“A number of studies suggest when patients leave the hospital, they’re not sure what they need to do. The language is complicated, and it’s hard to know what kind of medication to take when, and when you’re supposed to return to the doctor or the hospital,” Dr. DuGoff said. “Managing all of that can be pretty scary for people, particularly after a traumatic experience with sepsis at the hospital.”
Most patients had been discharged home (67.3%), but the 31.6% discharged to a skilled nursing facility had a greater likelihood of readmission, compared with those discharged home (P < .01); 1% were discharged to acute rehabilitation. The average length of stay during the index hospitalization was also greater for those readmitted (8.7 days) than for those not readmitted (6.4 days). The groups did not differ in terms of their acute organ dysfunction or severity of their comorbidities.
However, even after adjustment for these factors, “neighborhood disadvantage remained significantly associated with 30-day rehospitalization in patients who were discharged with sepsis,” the authors said. Specifically, each additional standard deviation greater in patients’ ADI was associated with increased risk of 30-day readmission (P < .001).
“Given that the ADI is a composite score, we cannot identify which component is the predominant driver of rehospitalizations for patients who survive sepsis,” the authors wrote. “However, all components that make up the index are intertwined, and policy efforts targeting one (i.e., unemployment) will likely impact others (i.e., housing).”
Dr. Durfey said that medical schools have not traditionally provided training related to management of social risk factors, although this is changing in more recent curricula. But the findings still have clinical relevance for practitioners.
“Certainly, the first step is awareness of where and how patients live and being mindful of how treatment plans may be impacted by social factors at both the individual and community levels,” Dr. Durfey said. “An important part of this is working in partnership with social workers and case managers. Importantly, clinicians can also partner with disadvantaged communities to advocate for improved conditions through policy change and act as expert witnesses to how neighborhood level factors impact health.”
Dr. DuGoff also wondered what implications these findings might have currently, with regards to COVID-19.
“People living in disadvantaged neighborhoods are already at higher risk for getting the disease, and this study raises really good questions about how we should be monitoring discharge now in anticipation of these types of issues,” she said.
The authors noted that their study is cross-sectional and cannot indicate causation, and the findings of a single urban institution may not be generalizable elsewhere. They also did not consider what interventions individual patients had during their index hospitalization that could have increased frailty.
The study did not note external funding. One coauthor of the study, Suchi Saria, PhD, reported receiving honoraria and travel reimbursement from two dozen biotechnology companies for keynotes and advisory board service; she also holds equity in Patient Ping and Bayesian Health. The other authors reported no industry disclosures. In addition to consulting for Berkeley Research Group, Dr. DuGoff has received a past honorarium from Zimmer Biomet. Dr. Durfey has no disclosures.
SOURCE: Galiatsatos P et al. Crit Care Med. 2020 Jun;48(6):808-14.
according to a study published in Critical Care Medicine.
The association between living in a disadvantaged neighborhood and 30-day readmission remained significant even after adjustment for “individual demographic variables, active tobacco use, length of index hospitalization, severity of acute and chronic morbidity, and place of initial discharge,” wrote Panagis Galiatsatos, MD, of Johns Hopkins University in Baltimore, and colleagues.
“Our findings suggest the need for interventions that emphasize neighborhood-level socioeconomic variables in addition to individual-level efforts in an effort to promote and achieve health equity for patients who survive a hospitalization due to sepsis,” the authors wrote. “With a third of our cohort rehospitalized with infections, and other studies emphasizing that the most common readmission diagnosis was infection, attention toward both anticipating and attenuating the risk of infection in sepsis survivors, especially among those who live in higher risk neighborhoods, must be a priority for the prevention of readmissions.”
Although she did not find the study results surprising, Eva DuGoff, PhD, a senior managing consultant with the Berkeley Research Group and a visiting assistant professor at University of Maryland School of Public Health, College Park, said in an interview that she was impressed with how clinically rigorous the analysis was, both in confirming an accurate sepsis diagnosis and in using the more refined measure of the Area Deprivation Index (ADI) to assess neighborhood disadvantage.
“I think it makes sense that people who have less means and are in neighborhoods with fewer resources would run into more issues and would need to return to the hospital, above and beyond the clinical risk factors, such as smoking and chronic conditions,” said Dr. DuGoff, who studies health disparities but was not involved in this study.
Shayla N.M. Durfey MD, ScM, a pediatric resident at Hasbro Children’s Hospital in Providence, R.I., said in an interview she was similarly unsurprised by the findings.
“People who live in disadvantaged neighborhoods may have less access to walking spaces, healthy food, and safe housing and more exposure to poor air quality, toxic stress, and violence – any of which can negatively impact health or recovery from illness through stress responses, nutritional deficiencies, or comorbidities, such as reactive airway disease, obesity, hypertension, and diabetes,” said Dr. Durfey, who studies health disparities but was not involved in this study. “Our research has found these neighborhood-level factors often matter above and beyond individual social determinants of health.”
Dr. Galiatsatos and associates conducted a retrospective study in Baltimore that compared readmission rates in 2017 at Johns Hopkins Bayview Medical Center among patients discharged after a hospitalization for sepsis, coded via ICD-10. They relied on the ADI to categorize the neighborhoods of patients’ residential addresses. The ADI rates various socioeconomic components, including income, education, employment, and housing characteristics, on a scale of 1-100 in geographic blocks, with higher score indicating a greater level of disadvantage.
Among 647 hospitalized patients with an ICD-10 code of sepsis who also met criteria for sepsis or septic shock per the Sepsis-3 definition, 17.9% were excluded from the analysis because they died or were transferred to hospice care. The other 531 patients had an average age of 61, and just under one-third (30.9%) were active smokers. Their average length of stay was 6.9 days, with a mean Charlson Comorbidity Index of 4.2 and a mean Sequential Organ Failure Assessment score of 4.9.
The average ADI for all the patients was 54.2, but the average score was 63 for the 22% of patients who were readmitted within 30 days of initial discharge, compared with an average 51.8 for patients not readmitted (P < .001).
Among those 117 readmitted, “39 patients had a reinfection, 68 had an exacerbation of their chronic conditions, and 10 were admitted for ‘concerning symptoms’ without a primary admitting diagnosis,” the investigators reported. Because “a third of our cohort was readmitted with an infection, it is possible that more disadvantaged neighborhoods created more challenges for a person’s immune system, which may be compromised after recovering from sepsis.”
Dr. DuGoff further noted that health literacy may be lower among people living in less advantaged neighborhoods.
“A number of studies suggest when patients leave the hospital, they’re not sure what they need to do. The language is complicated, and it’s hard to know what kind of medication to take when, and when you’re supposed to return to the doctor or the hospital,” Dr. DuGoff said. “Managing all of that can be pretty scary for people, particularly after a traumatic experience with sepsis at the hospital.”
Most patients had been discharged home (67.3%), but the 31.6% discharged to a skilled nursing facility had a greater likelihood of readmission, compared with those discharged home (P < .01); 1% were discharged to acute rehabilitation. The average length of stay during the index hospitalization was also greater for those readmitted (8.7 days) than for those not readmitted (6.4 days). The groups did not differ in terms of their acute organ dysfunction or severity of their comorbidities.
However, even after adjustment for these factors, “neighborhood disadvantage remained significantly associated with 30-day rehospitalization in patients who were discharged with sepsis,” the authors said. Specifically, each additional standard deviation greater in patients’ ADI was associated with increased risk of 30-day readmission (P < .001).
“Given that the ADI is a composite score, we cannot identify which component is the predominant driver of rehospitalizations for patients who survive sepsis,” the authors wrote. “However, all components that make up the index are intertwined, and policy efforts targeting one (i.e., unemployment) will likely impact others (i.e., housing).”
Dr. Durfey said that medical schools have not traditionally provided training related to management of social risk factors, although this is changing in more recent curricula. But the findings still have clinical relevance for practitioners.
“Certainly, the first step is awareness of where and how patients live and being mindful of how treatment plans may be impacted by social factors at both the individual and community levels,” Dr. Durfey said. “An important part of this is working in partnership with social workers and case managers. Importantly, clinicians can also partner with disadvantaged communities to advocate for improved conditions through policy change and act as expert witnesses to how neighborhood level factors impact health.”
Dr. DuGoff also wondered what implications these findings might have currently, with regards to COVID-19.
“People living in disadvantaged neighborhoods are already at higher risk for getting the disease, and this study raises really good questions about how we should be monitoring discharge now in anticipation of these types of issues,” she said.
The authors noted that their study is cross-sectional and cannot indicate causation, and the findings of a single urban institution may not be generalizable elsewhere. They also did not consider what interventions individual patients had during their index hospitalization that could have increased frailty.
The study did not note external funding. One coauthor of the study, Suchi Saria, PhD, reported receiving honoraria and travel reimbursement from two dozen biotechnology companies for keynotes and advisory board service; she also holds equity in Patient Ping and Bayesian Health. The other authors reported no industry disclosures. In addition to consulting for Berkeley Research Group, Dr. DuGoff has received a past honorarium from Zimmer Biomet. Dr. Durfey has no disclosures.
SOURCE: Galiatsatos P et al. Crit Care Med. 2020 Jun;48(6):808-14.
FROM CRITICAL CARE MEDICINE
ACR issues guidances for MIS-C and pediatric rheumatic disease during pandemic
Two new clinical guidance documents from the American College of Rheumatology provide evidence-based recommendations for managing pediatric rheumatic disease during the COVID-19 pandemic as well as diagnostic and treatment recommendations for multisystem inflammatory syndrome in children (MIS-C) associated with COVID-19 infection.
Although several children’s hospitals have published their treatment protocols for MIS-C since the condition’s initial discovery, the ACR appears to be the first medical organization to review all the most current evidence to issue interim guidance with the expectations that it will change as more data become available.
“It is challenging having to make recommendations not having a lot of scientific evidence, but we still felt we had to use whatever’s out there to the best of our ability and use our experience to put together these recommendations,” Dawn M. Wahezi, MD, chief of pediatric rheumatology at Children’s Hospital at Montefiore and an associate professor of pediatrics at Albert Einstein College of Medicine, New York, said in an interview.
“We wanted to be mindful of the fact that there are things we know and things we don’t know, and we have to be careful about what we’re recommending,” said Dr. Wahezi, a member of the ACR working group that assembled the recommendations for pediatric rheumatic disease management during the pandemic. “We’re recommending the best we can at this moment, but if there are new studies that come out and suggest otherwise, we will definitely have to go back and amend the document.”
The foremost priority of the pediatric rheumatic disease guidance focuses on maintaining control of the disease and avoiding flares that may put children at greater risk of infection. Dr. Wahezi said the ACR has received many calls from patients and clinicians asking whether patients should continue their immunosuppressant medications. Fear of the coronavirus infection, medication shortages, difficulty getting to the pharmacy, uneasiness about going to the clinic or hospital for infusions, and other barriers may have led to gaps in medication.
“We didn’t want people to be too quick to hold patients’ medications just because they were scared of COVID,” Dr. Wahezi said. “If they did have medication stopped for one reason or another and their disease flared, having active disease, regardless of which disease it is, actually puts you at higher risk for infection. By controlling their disease, that would be the way to protect them the most.”
A key takeaway in the guidance on MIS-C, meanwhile, is an emphasis on its rarity lest physicians be too quick to diagnose it and miss another serious condition with overlapping symptoms, explained Lauren Henderson, MD, an attending rheumatologist at Boston Children’s Hospital and assistant professor of pediatrics at Harvard Medical School, Boston. Dr. Henderson participated in the ACR group that wrote the MIS-C guidance.
“The first thing we want to be thoughtful about clinically is to recognize that children in general with the acute infectious phase of SARS-CoV-2 have mild symptoms and generally do well,” Dr. Henderson said. “From what we can tell from all the data, MIS-C is rare. That really needs to be considered when clinicians on the ground are doing the diagnostic evaluation” because of concerns that clinicians “could rush to diagnose and treat patients with MIS-C and miss important diagnoses like malignancies and infections.”
Management of pediatric rheumatic disease during the pandemic
The COVID-19 clinical guidance for managing pediatric rheumatic disease grew from the work of the North American Pediatric Rheumatology Clinical Guidance Task Force, which included seven pediatric rheumatologists, two pediatric infectious disease physicians, one adult rheumatologist, and one pediatric nurse practitioner. The general guidance covers usual preventive measures for reducing risk for COVID-19 infection, the recommendation that children continue to receive recommended vaccines unless contraindicated by medication, and routine in-person visits for ophthalmologic surveillance of those with a history of uveitis or at high risk for chronic uveitis. The guidance also notes the risk of mental health concerns, such as depression and anxiety, related to quarantine and the pandemic.
The top recommendation is initiation or continuation of all medications necessary to control underlying disease, including NSAIDs, hydroxychloroquine, ACE inhibitors/angiotensin II receptor blockers, colchicine, conventional disease-modifying antirheumatic drugs (cDMARDs), biologic DMARDs, and targeted synthetic DMARDs. Even patients who may have had exposure to COVID-19 or who have an asymptomatic COVID-19 infection should continue to take these medications with the exception of ACEi/ARBs.
In those with pediatric rheumatic disease who have a symptomatic COVID-19 infection, “NSAIDs, HCQ, and colchicine may be continued, if necessary, to control underlying disease,” as can interleukin (IL)-1 and IL-6 inhibitors, but “cDMARDs, bDMARDs [except IL-1 and IL-6 inhibitors] and tsDMARDs should be temporarily delayed or withheld,” according to the guidance. Glucocorticoids can be continued at the lowest possible dose to control disease.
“There’s nothing in the literature that suggests people who have rheumatic disease, especially children, and people who are on these medications, really are at increased risk for COVID-19,” Dr. Wahezi said. “That’s why we didn’t want people to be overcautious in stopping medications when the main priority is to control their disease.”
She noted some experts’ speculations that these medications may actually benefit patients with rheumatic disease who develop a COVID-19 infection because the medications keep the immune response in check. “If you allow them to have this dysregulated immune response and have active disease, you’re potentially putting them at greater risk,” Dr. Wahezi said, although she stressed that inadequate evidence exists to support these speculations right now.
Lack of evidence has been the biggest challenge all around with developing this guidance, she said.
“Because this is such an unprecedented situation and because people are so desperate to find treatments both for the illness and to protect those at risk for it, there are lots of people trying to put evidence out there, but it may not be the best-quality evidence,” Dr. Wahezi said.
Insufficient evidence also drove the group’s determination that “SARS-CoV-2 antibody testing is not useful in informing on the history of infection or risk of reinfection,” as the guidance states. Too much variability in the assays exist, Dr. Wahezi said, and, further, it’s unclear what the clinical significance of a positive test would be.
“We didn’t want anyone to feel they had to make clinical decisions based on the results of that antibody testing,” she said. “Even if the test is accurate, we don’t know how to interpret it because it’s so new.”
The guidance also notes that patients with stable disease and previously stable lab markers on stable doses of their medication may be able to extend the interval for medication toxicity lab testing a few months if there is concern about exposure to COVID-19 to get the blood work.
“If you’re just starting a medicine or there’s someone who’s had abnormalities with the medicine in the past or you’re making medication adjustments, you wouldn’t do it in those scenarios, but if there’s someone who’s been on the drug for a long time and are nervous to get [blood] drawn, it’s probably okay to delay it,” Dr. Wahezi said. Lab work for disease activity measures, on the other hand, remain particularly important, especially since telemedicine visits may require clinicians to rely on lab results more than previously.
Management of MIS-C associated with COVID-19
The task force that developed guidance for the new inflammatory condition recently linked to SARS-CoV-2 infections in children included nine pediatric rheumatologists, two adult rheumatologists, two pediatric cardiologists, two pediatric infectious disease specialists, and one pediatric critical care physician.
The guidance includes a figure for the diagnostic pathway in evaluating children suspected of having MIS-C and extensive detail on diagnostic work-up, but the task force intentionally avoided providing a case definition for the condition. Existing case definitions from the Centers for Disease Control and Prevention, World Health Organization, and the United Kingdom’s Royal College of Paediatrics and Child Health differ from one another and are based on unclear evidence, Dr. Henderson noted. “We really don’t have enough data to know the sensitivity and specificity of each parameter, and until that’s available, we didn’t want to add to the confusion,” she said.
The guidance also stresses that MIS-C is a rare complication, so patients suspected of having the condition who do not have “life-threatening manifestations should undergo diagnostic evaluation for MIS-C as well as other possible infectious and noninfectious etiologies before immunomodulatory treatment is initiated,” the guidance states.
Unless a child is in shock or otherwise requires urgent care, physicians should take the time to complete the diagnostic work-up while monitoring the child, Dr. Henderson said. If the child does have MIS-C, the guidance currently recommends intravenous immunoglobulin (IVIG) and/or glucocorticoids to prevent coronary artery aneurysms, the same treatment other institutions have been recommending.
“We don’t have rigorous comparative studies looking at different types of treatments,” Dr. Henderson said, noting that the vast majority of children in the literature received IVIG and/or glucocorticoid treatment. “Often children really responded quite forcefully to those treatments, but we don’t have high-quality data yet to know that this treatment is better than supportive care or another medication.”
Dr. Henderson also stressed the importance of children receiving care at a facility with the necessary expertise to manage MIS-C and receiving long-term follow-up care from a multidisciplinary clinical team that includes a rheumatologist, an infectious disease doctor, a cardiologist, and possibly a hematologist.
“Making sure children are admitted to a hospital that has the resources and are followed by physicians with expertise or understanding of the intricacies of MIS-C is really important,” she said, particularly for children with cardiac involvement. “We don’t know if all the kids presenting with left ventricular dysfunction and shock are at risk for having myocardial fibrosis down the line,” she noted. “There is so much we do not understand and very little data to guide us on what to do, so these children really need to be under the care of a cardiologist and rheumatologist to make sure that their care is tailored to them.”
Although MIS-C shares overlapping symptoms with Kawasaki disease, it’s still unclear how similar or different the two conditions are, Dr. Henderson said.
“We can definitely say that when we look at MIS-C and compare it to historical groups of Kawasaki disease before the pandemic, there are definitely different features in the MIS-C group,” she said. Kawasaki disease generally only affects children under age 5, whereas MIS-C patients run the gamut from age 1-17. Racial demographics are also different, with a higher proportion of black children affected by MIS-C.
It’s possible that the pathophysiology of both conditions will turn out to be similar, particularly given the hypothesis that Kawasaki disease is triggered by infections in genetically predisposed people. However, the severity of symptoms and risk of aneurysms appear greater with MIS-C so far.
“The degree to which these patients are presenting with left ventricular dysfunction and shock is much higher than what we’ve seen previously,” Dr. Henderson said. “Children can have aneurysms even if they don’t meet all the Kawasaki disease features, which makes it feel that this is somehow clinically different from what we’ve seen before. It’s not just the kids who have the rash and the conjunctivitis and the extremity changes and oral changes who have the aneurysms.”
The reason for including both IVIG and glucocorticoids as possible first-line drugs to prevent aneurysms is that some evidence suggests children with MIS-C may have higher levels of IVIG resistance, she said.
Like Dr. Wahezi, Dr. Henderson emphasized the necessarily transient nature of these recommendations.
“These recommendations will almost certainly change based on evolving understanding of MIS-C and the data,” Dr. Henderson said, adding that this new, unique condition highlights the importance of including children in allocating funding for research and in clinical trials.
“Children are not always identical to adults, and it’s really important that we have high-quality data to inform our decisions about how to care for them,” she said.
Dr. Wahezi had no disclosures. Dr. Henderson has consulted for Sobi and Adaptive Technologies. The guidelines did not note other disclosures for members of the ACR groups.
SOURCES: COVID-19 Clinical Guidance for Pediatric Patients with Rheumatic Disease and Clinical Guidance for Pediatric Patients with Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with SARS-CoV-2 and Hyperinflammation in COVID-19
Two new clinical guidance documents from the American College of Rheumatology provide evidence-based recommendations for managing pediatric rheumatic disease during the COVID-19 pandemic as well as diagnostic and treatment recommendations for multisystem inflammatory syndrome in children (MIS-C) associated with COVID-19 infection.
Although several children’s hospitals have published their treatment protocols for MIS-C since the condition’s initial discovery, the ACR appears to be the first medical organization to review all the most current evidence to issue interim guidance with the expectations that it will change as more data become available.
“It is challenging having to make recommendations not having a lot of scientific evidence, but we still felt we had to use whatever’s out there to the best of our ability and use our experience to put together these recommendations,” Dawn M. Wahezi, MD, chief of pediatric rheumatology at Children’s Hospital at Montefiore and an associate professor of pediatrics at Albert Einstein College of Medicine, New York, said in an interview.
“We wanted to be mindful of the fact that there are things we know and things we don’t know, and we have to be careful about what we’re recommending,” said Dr. Wahezi, a member of the ACR working group that assembled the recommendations for pediatric rheumatic disease management during the pandemic. “We’re recommending the best we can at this moment, but if there are new studies that come out and suggest otherwise, we will definitely have to go back and amend the document.”
The foremost priority of the pediatric rheumatic disease guidance focuses on maintaining control of the disease and avoiding flares that may put children at greater risk of infection. Dr. Wahezi said the ACR has received many calls from patients and clinicians asking whether patients should continue their immunosuppressant medications. Fear of the coronavirus infection, medication shortages, difficulty getting to the pharmacy, uneasiness about going to the clinic or hospital for infusions, and other barriers may have led to gaps in medication.
“We didn’t want people to be too quick to hold patients’ medications just because they were scared of COVID,” Dr. Wahezi said. “If they did have medication stopped for one reason or another and their disease flared, having active disease, regardless of which disease it is, actually puts you at higher risk for infection. By controlling their disease, that would be the way to protect them the most.”
A key takeaway in the guidance on MIS-C, meanwhile, is an emphasis on its rarity lest physicians be too quick to diagnose it and miss another serious condition with overlapping symptoms, explained Lauren Henderson, MD, an attending rheumatologist at Boston Children’s Hospital and assistant professor of pediatrics at Harvard Medical School, Boston. Dr. Henderson participated in the ACR group that wrote the MIS-C guidance.
“The first thing we want to be thoughtful about clinically is to recognize that children in general with the acute infectious phase of SARS-CoV-2 have mild symptoms and generally do well,” Dr. Henderson said. “From what we can tell from all the data, MIS-C is rare. That really needs to be considered when clinicians on the ground are doing the diagnostic evaluation” because of concerns that clinicians “could rush to diagnose and treat patients with MIS-C and miss important diagnoses like malignancies and infections.”
Management of pediatric rheumatic disease during the pandemic
The COVID-19 clinical guidance for managing pediatric rheumatic disease grew from the work of the North American Pediatric Rheumatology Clinical Guidance Task Force, which included seven pediatric rheumatologists, two pediatric infectious disease physicians, one adult rheumatologist, and one pediatric nurse practitioner. The general guidance covers usual preventive measures for reducing risk for COVID-19 infection, the recommendation that children continue to receive recommended vaccines unless contraindicated by medication, and routine in-person visits for ophthalmologic surveillance of those with a history of uveitis or at high risk for chronic uveitis. The guidance also notes the risk of mental health concerns, such as depression and anxiety, related to quarantine and the pandemic.
The top recommendation is initiation or continuation of all medications necessary to control underlying disease, including NSAIDs, hydroxychloroquine, ACE inhibitors/angiotensin II receptor blockers, colchicine, conventional disease-modifying antirheumatic drugs (cDMARDs), biologic DMARDs, and targeted synthetic DMARDs. Even patients who may have had exposure to COVID-19 or who have an asymptomatic COVID-19 infection should continue to take these medications with the exception of ACEi/ARBs.
In those with pediatric rheumatic disease who have a symptomatic COVID-19 infection, “NSAIDs, HCQ, and colchicine may be continued, if necessary, to control underlying disease,” as can interleukin (IL)-1 and IL-6 inhibitors, but “cDMARDs, bDMARDs [except IL-1 and IL-6 inhibitors] and tsDMARDs should be temporarily delayed or withheld,” according to the guidance. Glucocorticoids can be continued at the lowest possible dose to control disease.
“There’s nothing in the literature that suggests people who have rheumatic disease, especially children, and people who are on these medications, really are at increased risk for COVID-19,” Dr. Wahezi said. “That’s why we didn’t want people to be overcautious in stopping medications when the main priority is to control their disease.”
She noted some experts’ speculations that these medications may actually benefit patients with rheumatic disease who develop a COVID-19 infection because the medications keep the immune response in check. “If you allow them to have this dysregulated immune response and have active disease, you’re potentially putting them at greater risk,” Dr. Wahezi said, although she stressed that inadequate evidence exists to support these speculations right now.
Lack of evidence has been the biggest challenge all around with developing this guidance, she said.
“Because this is such an unprecedented situation and because people are so desperate to find treatments both for the illness and to protect those at risk for it, there are lots of people trying to put evidence out there, but it may not be the best-quality evidence,” Dr. Wahezi said.
Insufficient evidence also drove the group’s determination that “SARS-CoV-2 antibody testing is not useful in informing on the history of infection or risk of reinfection,” as the guidance states. Too much variability in the assays exist, Dr. Wahezi said, and, further, it’s unclear what the clinical significance of a positive test would be.
“We didn’t want anyone to feel they had to make clinical decisions based on the results of that antibody testing,” she said. “Even if the test is accurate, we don’t know how to interpret it because it’s so new.”
The guidance also notes that patients with stable disease and previously stable lab markers on stable doses of their medication may be able to extend the interval for medication toxicity lab testing a few months if there is concern about exposure to COVID-19 to get the blood work.
“If you’re just starting a medicine or there’s someone who’s had abnormalities with the medicine in the past or you’re making medication adjustments, you wouldn’t do it in those scenarios, but if there’s someone who’s been on the drug for a long time and are nervous to get [blood] drawn, it’s probably okay to delay it,” Dr. Wahezi said. Lab work for disease activity measures, on the other hand, remain particularly important, especially since telemedicine visits may require clinicians to rely on lab results more than previously.
Management of MIS-C associated with COVID-19
The task force that developed guidance for the new inflammatory condition recently linked to SARS-CoV-2 infections in children included nine pediatric rheumatologists, two adult rheumatologists, two pediatric cardiologists, two pediatric infectious disease specialists, and one pediatric critical care physician.
The guidance includes a figure for the diagnostic pathway in evaluating children suspected of having MIS-C and extensive detail on diagnostic work-up, but the task force intentionally avoided providing a case definition for the condition. Existing case definitions from the Centers for Disease Control and Prevention, World Health Organization, and the United Kingdom’s Royal College of Paediatrics and Child Health differ from one another and are based on unclear evidence, Dr. Henderson noted. “We really don’t have enough data to know the sensitivity and specificity of each parameter, and until that’s available, we didn’t want to add to the confusion,” she said.
The guidance also stresses that MIS-C is a rare complication, so patients suspected of having the condition who do not have “life-threatening manifestations should undergo diagnostic evaluation for MIS-C as well as other possible infectious and noninfectious etiologies before immunomodulatory treatment is initiated,” the guidance states.
Unless a child is in shock or otherwise requires urgent care, physicians should take the time to complete the diagnostic work-up while monitoring the child, Dr. Henderson said. If the child does have MIS-C, the guidance currently recommends intravenous immunoglobulin (IVIG) and/or glucocorticoids to prevent coronary artery aneurysms, the same treatment other institutions have been recommending.
“We don’t have rigorous comparative studies looking at different types of treatments,” Dr. Henderson said, noting that the vast majority of children in the literature received IVIG and/or glucocorticoid treatment. “Often children really responded quite forcefully to those treatments, but we don’t have high-quality data yet to know that this treatment is better than supportive care or another medication.”
Dr. Henderson also stressed the importance of children receiving care at a facility with the necessary expertise to manage MIS-C and receiving long-term follow-up care from a multidisciplinary clinical team that includes a rheumatologist, an infectious disease doctor, a cardiologist, and possibly a hematologist.
“Making sure children are admitted to a hospital that has the resources and are followed by physicians with expertise or understanding of the intricacies of MIS-C is really important,” she said, particularly for children with cardiac involvement. “We don’t know if all the kids presenting with left ventricular dysfunction and shock are at risk for having myocardial fibrosis down the line,” she noted. “There is so much we do not understand and very little data to guide us on what to do, so these children really need to be under the care of a cardiologist and rheumatologist to make sure that their care is tailored to them.”
Although MIS-C shares overlapping symptoms with Kawasaki disease, it’s still unclear how similar or different the two conditions are, Dr. Henderson said.
“We can definitely say that when we look at MIS-C and compare it to historical groups of Kawasaki disease before the pandemic, there are definitely different features in the MIS-C group,” she said. Kawasaki disease generally only affects children under age 5, whereas MIS-C patients run the gamut from age 1-17. Racial demographics are also different, with a higher proportion of black children affected by MIS-C.
It’s possible that the pathophysiology of both conditions will turn out to be similar, particularly given the hypothesis that Kawasaki disease is triggered by infections in genetically predisposed people. However, the severity of symptoms and risk of aneurysms appear greater with MIS-C so far.
“The degree to which these patients are presenting with left ventricular dysfunction and shock is much higher than what we’ve seen previously,” Dr. Henderson said. “Children can have aneurysms even if they don’t meet all the Kawasaki disease features, which makes it feel that this is somehow clinically different from what we’ve seen before. It’s not just the kids who have the rash and the conjunctivitis and the extremity changes and oral changes who have the aneurysms.”
The reason for including both IVIG and glucocorticoids as possible first-line drugs to prevent aneurysms is that some evidence suggests children with MIS-C may have higher levels of IVIG resistance, she said.
Like Dr. Wahezi, Dr. Henderson emphasized the necessarily transient nature of these recommendations.
“These recommendations will almost certainly change based on evolving understanding of MIS-C and the data,” Dr. Henderson said, adding that this new, unique condition highlights the importance of including children in allocating funding for research and in clinical trials.
“Children are not always identical to adults, and it’s really important that we have high-quality data to inform our decisions about how to care for them,” she said.
Dr. Wahezi had no disclosures. Dr. Henderson has consulted for Sobi and Adaptive Technologies. The guidelines did not note other disclosures for members of the ACR groups.
SOURCES: COVID-19 Clinical Guidance for Pediatric Patients with Rheumatic Disease and Clinical Guidance for Pediatric Patients with Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with SARS-CoV-2 and Hyperinflammation in COVID-19
Two new clinical guidance documents from the American College of Rheumatology provide evidence-based recommendations for managing pediatric rheumatic disease during the COVID-19 pandemic as well as diagnostic and treatment recommendations for multisystem inflammatory syndrome in children (MIS-C) associated with COVID-19 infection.
Although several children’s hospitals have published their treatment protocols for MIS-C since the condition’s initial discovery, the ACR appears to be the first medical organization to review all the most current evidence to issue interim guidance with the expectations that it will change as more data become available.
“It is challenging having to make recommendations not having a lot of scientific evidence, but we still felt we had to use whatever’s out there to the best of our ability and use our experience to put together these recommendations,” Dawn M. Wahezi, MD, chief of pediatric rheumatology at Children’s Hospital at Montefiore and an associate professor of pediatrics at Albert Einstein College of Medicine, New York, said in an interview.
“We wanted to be mindful of the fact that there are things we know and things we don’t know, and we have to be careful about what we’re recommending,” said Dr. Wahezi, a member of the ACR working group that assembled the recommendations for pediatric rheumatic disease management during the pandemic. “We’re recommending the best we can at this moment, but if there are new studies that come out and suggest otherwise, we will definitely have to go back and amend the document.”
The foremost priority of the pediatric rheumatic disease guidance focuses on maintaining control of the disease and avoiding flares that may put children at greater risk of infection. Dr. Wahezi said the ACR has received many calls from patients and clinicians asking whether patients should continue their immunosuppressant medications. Fear of the coronavirus infection, medication shortages, difficulty getting to the pharmacy, uneasiness about going to the clinic or hospital for infusions, and other barriers may have led to gaps in medication.
“We didn’t want people to be too quick to hold patients’ medications just because they were scared of COVID,” Dr. Wahezi said. “If they did have medication stopped for one reason or another and their disease flared, having active disease, regardless of which disease it is, actually puts you at higher risk for infection. By controlling their disease, that would be the way to protect them the most.”
A key takeaway in the guidance on MIS-C, meanwhile, is an emphasis on its rarity lest physicians be too quick to diagnose it and miss another serious condition with overlapping symptoms, explained Lauren Henderson, MD, an attending rheumatologist at Boston Children’s Hospital and assistant professor of pediatrics at Harvard Medical School, Boston. Dr. Henderson participated in the ACR group that wrote the MIS-C guidance.
“The first thing we want to be thoughtful about clinically is to recognize that children in general with the acute infectious phase of SARS-CoV-2 have mild symptoms and generally do well,” Dr. Henderson said. “From what we can tell from all the data, MIS-C is rare. That really needs to be considered when clinicians on the ground are doing the diagnostic evaluation” because of concerns that clinicians “could rush to diagnose and treat patients with MIS-C and miss important diagnoses like malignancies and infections.”
Management of pediatric rheumatic disease during the pandemic
The COVID-19 clinical guidance for managing pediatric rheumatic disease grew from the work of the North American Pediatric Rheumatology Clinical Guidance Task Force, which included seven pediatric rheumatologists, two pediatric infectious disease physicians, one adult rheumatologist, and one pediatric nurse practitioner. The general guidance covers usual preventive measures for reducing risk for COVID-19 infection, the recommendation that children continue to receive recommended vaccines unless contraindicated by medication, and routine in-person visits for ophthalmologic surveillance of those with a history of uveitis or at high risk for chronic uveitis. The guidance also notes the risk of mental health concerns, such as depression and anxiety, related to quarantine and the pandemic.
The top recommendation is initiation or continuation of all medications necessary to control underlying disease, including NSAIDs, hydroxychloroquine, ACE inhibitors/angiotensin II receptor blockers, colchicine, conventional disease-modifying antirheumatic drugs (cDMARDs), biologic DMARDs, and targeted synthetic DMARDs. Even patients who may have had exposure to COVID-19 or who have an asymptomatic COVID-19 infection should continue to take these medications with the exception of ACEi/ARBs.
In those with pediatric rheumatic disease who have a symptomatic COVID-19 infection, “NSAIDs, HCQ, and colchicine may be continued, if necessary, to control underlying disease,” as can interleukin (IL)-1 and IL-6 inhibitors, but “cDMARDs, bDMARDs [except IL-1 and IL-6 inhibitors] and tsDMARDs should be temporarily delayed or withheld,” according to the guidance. Glucocorticoids can be continued at the lowest possible dose to control disease.
“There’s nothing in the literature that suggests people who have rheumatic disease, especially children, and people who are on these medications, really are at increased risk for COVID-19,” Dr. Wahezi said. “That’s why we didn’t want people to be overcautious in stopping medications when the main priority is to control their disease.”
She noted some experts’ speculations that these medications may actually benefit patients with rheumatic disease who develop a COVID-19 infection because the medications keep the immune response in check. “If you allow them to have this dysregulated immune response and have active disease, you’re potentially putting them at greater risk,” Dr. Wahezi said, although she stressed that inadequate evidence exists to support these speculations right now.
Lack of evidence has been the biggest challenge all around with developing this guidance, she said.
“Because this is such an unprecedented situation and because people are so desperate to find treatments both for the illness and to protect those at risk for it, there are lots of people trying to put evidence out there, but it may not be the best-quality evidence,” Dr. Wahezi said.
Insufficient evidence also drove the group’s determination that “SARS-CoV-2 antibody testing is not useful in informing on the history of infection or risk of reinfection,” as the guidance states. Too much variability in the assays exist, Dr. Wahezi said, and, further, it’s unclear what the clinical significance of a positive test would be.
“We didn’t want anyone to feel they had to make clinical decisions based on the results of that antibody testing,” she said. “Even if the test is accurate, we don’t know how to interpret it because it’s so new.”
The guidance also notes that patients with stable disease and previously stable lab markers on stable doses of their medication may be able to extend the interval for medication toxicity lab testing a few months if there is concern about exposure to COVID-19 to get the blood work.
“If you’re just starting a medicine or there’s someone who’s had abnormalities with the medicine in the past or you’re making medication adjustments, you wouldn’t do it in those scenarios, but if there’s someone who’s been on the drug for a long time and are nervous to get [blood] drawn, it’s probably okay to delay it,” Dr. Wahezi said. Lab work for disease activity measures, on the other hand, remain particularly important, especially since telemedicine visits may require clinicians to rely on lab results more than previously.
Management of MIS-C associated with COVID-19
The task force that developed guidance for the new inflammatory condition recently linked to SARS-CoV-2 infections in children included nine pediatric rheumatologists, two adult rheumatologists, two pediatric cardiologists, two pediatric infectious disease specialists, and one pediatric critical care physician.
The guidance includes a figure for the diagnostic pathway in evaluating children suspected of having MIS-C and extensive detail on diagnostic work-up, but the task force intentionally avoided providing a case definition for the condition. Existing case definitions from the Centers for Disease Control and Prevention, World Health Organization, and the United Kingdom’s Royal College of Paediatrics and Child Health differ from one another and are based on unclear evidence, Dr. Henderson noted. “We really don’t have enough data to know the sensitivity and specificity of each parameter, and until that’s available, we didn’t want to add to the confusion,” she said.
The guidance also stresses that MIS-C is a rare complication, so patients suspected of having the condition who do not have “life-threatening manifestations should undergo diagnostic evaluation for MIS-C as well as other possible infectious and noninfectious etiologies before immunomodulatory treatment is initiated,” the guidance states.
Unless a child is in shock or otherwise requires urgent care, physicians should take the time to complete the diagnostic work-up while monitoring the child, Dr. Henderson said. If the child does have MIS-C, the guidance currently recommends intravenous immunoglobulin (IVIG) and/or glucocorticoids to prevent coronary artery aneurysms, the same treatment other institutions have been recommending.
“We don’t have rigorous comparative studies looking at different types of treatments,” Dr. Henderson said, noting that the vast majority of children in the literature received IVIG and/or glucocorticoid treatment. “Often children really responded quite forcefully to those treatments, but we don’t have high-quality data yet to know that this treatment is better than supportive care or another medication.”
Dr. Henderson also stressed the importance of children receiving care at a facility with the necessary expertise to manage MIS-C and receiving long-term follow-up care from a multidisciplinary clinical team that includes a rheumatologist, an infectious disease doctor, a cardiologist, and possibly a hematologist.
“Making sure children are admitted to a hospital that has the resources and are followed by physicians with expertise or understanding of the intricacies of MIS-C is really important,” she said, particularly for children with cardiac involvement. “We don’t know if all the kids presenting with left ventricular dysfunction and shock are at risk for having myocardial fibrosis down the line,” she noted. “There is so much we do not understand and very little data to guide us on what to do, so these children really need to be under the care of a cardiologist and rheumatologist to make sure that their care is tailored to them.”
Although MIS-C shares overlapping symptoms with Kawasaki disease, it’s still unclear how similar or different the two conditions are, Dr. Henderson said.
“We can definitely say that when we look at MIS-C and compare it to historical groups of Kawasaki disease before the pandemic, there are definitely different features in the MIS-C group,” she said. Kawasaki disease generally only affects children under age 5, whereas MIS-C patients run the gamut from age 1-17. Racial demographics are also different, with a higher proportion of black children affected by MIS-C.
It’s possible that the pathophysiology of both conditions will turn out to be similar, particularly given the hypothesis that Kawasaki disease is triggered by infections in genetically predisposed people. However, the severity of symptoms and risk of aneurysms appear greater with MIS-C so far.
“The degree to which these patients are presenting with left ventricular dysfunction and shock is much higher than what we’ve seen previously,” Dr. Henderson said. “Children can have aneurysms even if they don’t meet all the Kawasaki disease features, which makes it feel that this is somehow clinically different from what we’ve seen before. It’s not just the kids who have the rash and the conjunctivitis and the extremity changes and oral changes who have the aneurysms.”
The reason for including both IVIG and glucocorticoids as possible first-line drugs to prevent aneurysms is that some evidence suggests children with MIS-C may have higher levels of IVIG resistance, she said.
Like Dr. Wahezi, Dr. Henderson emphasized the necessarily transient nature of these recommendations.
“These recommendations will almost certainly change based on evolving understanding of MIS-C and the data,” Dr. Henderson said, adding that this new, unique condition highlights the importance of including children in allocating funding for research and in clinical trials.
“Children are not always identical to adults, and it’s really important that we have high-quality data to inform our decisions about how to care for them,” she said.
Dr. Wahezi had no disclosures. Dr. Henderson has consulted for Sobi and Adaptive Technologies. The guidelines did not note other disclosures for members of the ACR groups.
SOURCES: COVID-19 Clinical Guidance for Pediatric Patients with Rheumatic Disease and Clinical Guidance for Pediatric Patients with Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with SARS-CoV-2 and Hyperinflammation in COVID-19
Food deserts linked to greater pregnancy morbidity
according to a retrospective observational study published in Obstetrics & Gynecology.
Previous research has linked so-called “food deserts” to higher systolic blood pressure and an increased risk of cardiovascular events in people with coronary artery disease, the authors note.
“Research on populations in the United States confirm that increased access to supermarkets is associated with lower prevalence of overweight and obesity, and improved fruit and vegetable consumption,” said Matthew J. Tipton, MD, of Loyola University Medical Center in Chicago, and colleagues.
“With our study showing an association between living in a food desert and increased pregnancy morbidity, it is our hope that with future work, an unhealthy food environment could prove to be a modifiable factor that does contribute to disparities in pregnancy morbidity,” the authors said. “Perhaps then, one could question whether greater access to healthier foods could reduce unexplained pregnancy morbidity for this population of patients,” paving the way toward developing interventions that can then improve vulnerable women’s health.
The researchers reviewed the electronic medical records of all the pregnant patients who delivered at Loyola University Medical Center in 2014. To determine who lived in a food desert, the authors relied on data about grocery food availability within Census tracts from the U.S. Department of Agriculture Food Access Research Atlas.
Dr. Tipton and associates defined living in a food desert as living in a low-income Census tract “where at least 33% of the population is more than half a mile from the nearest large grocery store for an urban area or more than 10 miles for a rural area.” Low-income Census tracts are those where “at least 20% of the population has a median family income at or below 80% of the metropolitan area or state median income.”
The authors compared women’s residence within a food desert (or not) with six different pregnancy morbidities: preeclampsia, gestational hypertension, gestational diabetes, prelabor rupture of membranes, preterm labor, and intrauterine growth restriction.
Among 1,001 deliveries, about 1 in 5 women (20%) lived in a food desert. These women tended to be slightly younger than those not living in a food desert (28 vs. 30 years old), and a higher proportion of women in food deserts were black (44%) rather than white (32%). They also had a lower average income ($44,694) than those not living in food deserts ($67,005).
After adjustment for age, race, and medical insurance type (private, Medicaid, other), the researchers found that women who lived in a food desert had 1.6 times greater odds of pregnancy comorbidity than if they did not (odds ratio, 1.64; P = .004). Nearly half the women living in food deserts had any type of comorbidity (47%), compared with just over a third of women who did not (36%).
Among the six comorbidities studied, preterm rupture of membranes was significantly different before adjustment between those who lived in food deserts (16%) and those who did not (10%) (P = .015). An association with preeclampsia had borderline significance before adjustment: 13% of women in food deserts had preeclampsia, compared with 9% of women not (P = .049). After adjustment for age, race, and medical insurance, however, neither of these associations retained statistically significant differences.
The study was limited by leaving out consideration of other factors besides local food access that might influence pregnancy health, including “quality of patient-doctor communication, implicit bias, structural racism, and stress owing to concern for neighborhood safety,” Dr. Tipton and associates said.
“An additional, albeit less obvious factor that may be unique to patients suffering disproportionately from obstetric morbidity is exposure to toxic elements,” the researchers add. “It has been shown in a previous study that low-income, predominately black communities of pregnant women may suffer disproportionately from lead or arsenic exposure.”
The study did not note external funding, and the authors reported no relevant financial disclosures.
SOURCE: Tipton MJ et al. Obstet Gynecol. 2020. doi: 10.1097/AOG.0000000000003868.
according to a retrospective observational study published in Obstetrics & Gynecology.
Previous research has linked so-called “food deserts” to higher systolic blood pressure and an increased risk of cardiovascular events in people with coronary artery disease, the authors note.
“Research on populations in the United States confirm that increased access to supermarkets is associated with lower prevalence of overweight and obesity, and improved fruit and vegetable consumption,” said Matthew J. Tipton, MD, of Loyola University Medical Center in Chicago, and colleagues.
“With our study showing an association between living in a food desert and increased pregnancy morbidity, it is our hope that with future work, an unhealthy food environment could prove to be a modifiable factor that does contribute to disparities in pregnancy morbidity,” the authors said. “Perhaps then, one could question whether greater access to healthier foods could reduce unexplained pregnancy morbidity for this population of patients,” paving the way toward developing interventions that can then improve vulnerable women’s health.
The researchers reviewed the electronic medical records of all the pregnant patients who delivered at Loyola University Medical Center in 2014. To determine who lived in a food desert, the authors relied on data about grocery food availability within Census tracts from the U.S. Department of Agriculture Food Access Research Atlas.
Dr. Tipton and associates defined living in a food desert as living in a low-income Census tract “where at least 33% of the population is more than half a mile from the nearest large grocery store for an urban area or more than 10 miles for a rural area.” Low-income Census tracts are those where “at least 20% of the population has a median family income at or below 80% of the metropolitan area or state median income.”
The authors compared women’s residence within a food desert (or not) with six different pregnancy morbidities: preeclampsia, gestational hypertension, gestational diabetes, prelabor rupture of membranes, preterm labor, and intrauterine growth restriction.
Among 1,001 deliveries, about 1 in 5 women (20%) lived in a food desert. These women tended to be slightly younger than those not living in a food desert (28 vs. 30 years old), and a higher proportion of women in food deserts were black (44%) rather than white (32%). They also had a lower average income ($44,694) than those not living in food deserts ($67,005).
After adjustment for age, race, and medical insurance type (private, Medicaid, other), the researchers found that women who lived in a food desert had 1.6 times greater odds of pregnancy comorbidity than if they did not (odds ratio, 1.64; P = .004). Nearly half the women living in food deserts had any type of comorbidity (47%), compared with just over a third of women who did not (36%).
Among the six comorbidities studied, preterm rupture of membranes was significantly different before adjustment between those who lived in food deserts (16%) and those who did not (10%) (P = .015). An association with preeclampsia had borderline significance before adjustment: 13% of women in food deserts had preeclampsia, compared with 9% of women not (P = .049). After adjustment for age, race, and medical insurance, however, neither of these associations retained statistically significant differences.
The study was limited by leaving out consideration of other factors besides local food access that might influence pregnancy health, including “quality of patient-doctor communication, implicit bias, structural racism, and stress owing to concern for neighborhood safety,” Dr. Tipton and associates said.
“An additional, albeit less obvious factor that may be unique to patients suffering disproportionately from obstetric morbidity is exposure to toxic elements,” the researchers add. “It has been shown in a previous study that low-income, predominately black communities of pregnant women may suffer disproportionately from lead or arsenic exposure.”
The study did not note external funding, and the authors reported no relevant financial disclosures.
SOURCE: Tipton MJ et al. Obstet Gynecol. 2020. doi: 10.1097/AOG.0000000000003868.
according to a retrospective observational study published in Obstetrics & Gynecology.
Previous research has linked so-called “food deserts” to higher systolic blood pressure and an increased risk of cardiovascular events in people with coronary artery disease, the authors note.
“Research on populations in the United States confirm that increased access to supermarkets is associated with lower prevalence of overweight and obesity, and improved fruit and vegetable consumption,” said Matthew J. Tipton, MD, of Loyola University Medical Center in Chicago, and colleagues.
“With our study showing an association between living in a food desert and increased pregnancy morbidity, it is our hope that with future work, an unhealthy food environment could prove to be a modifiable factor that does contribute to disparities in pregnancy morbidity,” the authors said. “Perhaps then, one could question whether greater access to healthier foods could reduce unexplained pregnancy morbidity for this population of patients,” paving the way toward developing interventions that can then improve vulnerable women’s health.
The researchers reviewed the electronic medical records of all the pregnant patients who delivered at Loyola University Medical Center in 2014. To determine who lived in a food desert, the authors relied on data about grocery food availability within Census tracts from the U.S. Department of Agriculture Food Access Research Atlas.
Dr. Tipton and associates defined living in a food desert as living in a low-income Census tract “where at least 33% of the population is more than half a mile from the nearest large grocery store for an urban area or more than 10 miles for a rural area.” Low-income Census tracts are those where “at least 20% of the population has a median family income at or below 80% of the metropolitan area or state median income.”
The authors compared women’s residence within a food desert (or not) with six different pregnancy morbidities: preeclampsia, gestational hypertension, gestational diabetes, prelabor rupture of membranes, preterm labor, and intrauterine growth restriction.
Among 1,001 deliveries, about 1 in 5 women (20%) lived in a food desert. These women tended to be slightly younger than those not living in a food desert (28 vs. 30 years old), and a higher proportion of women in food deserts were black (44%) rather than white (32%). They also had a lower average income ($44,694) than those not living in food deserts ($67,005).
After adjustment for age, race, and medical insurance type (private, Medicaid, other), the researchers found that women who lived in a food desert had 1.6 times greater odds of pregnancy comorbidity than if they did not (odds ratio, 1.64; P = .004). Nearly half the women living in food deserts had any type of comorbidity (47%), compared with just over a third of women who did not (36%).
Among the six comorbidities studied, preterm rupture of membranes was significantly different before adjustment between those who lived in food deserts (16%) and those who did not (10%) (P = .015). An association with preeclampsia had borderline significance before adjustment: 13% of women in food deserts had preeclampsia, compared with 9% of women not (P = .049). After adjustment for age, race, and medical insurance, however, neither of these associations retained statistically significant differences.
The study was limited by leaving out consideration of other factors besides local food access that might influence pregnancy health, including “quality of patient-doctor communication, implicit bias, structural racism, and stress owing to concern for neighborhood safety,” Dr. Tipton and associates said.
“An additional, albeit less obvious factor that may be unique to patients suffering disproportionately from obstetric morbidity is exposure to toxic elements,” the researchers add. “It has been shown in a previous study that low-income, predominately black communities of pregnant women may suffer disproportionately from lead or arsenic exposure.”
The study did not note external funding, and the authors reported no relevant financial disclosures.
SOURCE: Tipton MJ et al. Obstet Gynecol. 2020. doi: 10.1097/AOG.0000000000003868.
FROM OBSTETRICS & GYNECOLOGY
COVID-19-related inflammatory condition more common in black children in small study
More evidence has linked the Kawasaki-like multisystem inflammatory syndrome in children to COVID-19 and suggests that black children have a greater risk of the condition, according to a study published in the BMJ.
A small observational study in Paris found more than half of the 21 children who were admitted for the condition at the city’s pediatric hospital for COVID-19 patients were of African ancestry.
“The observation of a higher proportion of patients of African ancestry is consistent with recent findings, suggesting an effect of either social and living conditions or genetic susceptibility,” wrote Julie Toubiana, MD, PhD, of the University of Paris and the Pasteur Institute, and colleagues.
The findings did not surprise Edward M. Behrens, MD, chief of the division of rheumatology at Children’s Hospital of Philadelphia, whose institution has seen similar disparities that he attributes to social disadvantages.
“Infection rate will be higher in vulnerable populations that are less able to socially distance, have disproportionate numbers of essential workers, and have less access to health care and other resources,” Dr. Behrens said in an interview. “While there may be a role for genetics, environment – including social disparities – is almost certainly playing a role.”
Although the study’s small size is a limitation, he said, “the features described seem to mirror the experience of our center and what has been discussed more broadly amongst U.S. physicians.”
Byron Whyte, MD, a pediatrician in private practice in southeast Washington, found the differences in race interesting, but said the study was too small to draw any conclusions or generalize to the United States. But social disparities related to race are likely similar in France as they are in the United States, he said.
The prospective observational study assessed the clinical and demographic characteristics of all patients under age 18 who met the criteria for Kawasaki disease and were admitted between April 27 and May 20 to the Necker Hospital for Sick Children in Paris.
The 21 children had an average age of 8 years (ranging from 3 to 16), and 57% had at least one parent from sub-Saharan Africa or a Caribbean island; 14% had parents from Asia (two from China and one from Sri Lanka). The authors noted in their discussion that past U.S. and U.K. studies of Kawasaki disease have found a 2.5 times greater risk in Asian-American children and 1.5 times greater risk in African-American children compared with children with European ancestry.
Most of the patients (81%) needed intensive care, with 57% presenting with Kawasaki disease shock syndrome and 67% with myocarditis. Dr. Toubiana and associates also noted that “gastrointestinal symptoms were also unusually common, affecting all of our 21 patients.”
Only nine of the children reported having symptoms of a viral-like illness when they were admitted, primarily headache, cough, coryza, and fever, plus anosmia in one child. Among those children, the Kawasaki symptoms began a median 45 days after onset of the viral symptoms (range 18-79 days).
Only two children showed no positive test result for current COVID-19 infection or antibodies. Eight (38%) of the children had positive PCR tests for SARS-CoV2, and 19 (90%) had positive tests for IgG antibodies. The two patients with both negative tests did not require intensive care and did not have myocarditis.
About half the patients (52%) met all the criteria of Kawasaki disease, and the other 10 had “incomplete Kawasaki disease.” The most common Kawasaki symptoms were the polymorphous skin rash, occurring in 76% of the patients, changes to the lips and oral cavity (76%), and bilateral bulbar conjunctival injection (81%). Three patients (14%) had pleural effusion, and 10 of them (48%) had pericardial effusion, Dr. Toubiana and associates reported.
But Dr. Behrens said he disagrees with the assertion that the illness described in the paper and what he is seeing at Children’s Hospital of Philadelphia is related to Kawasaki disease.
“Most experts here in the U.S. seem to agree this is not Kawasaki disease, but a distinct clinical syndrome called multisystem inflammatory syndrome in children, or MIS-C, that seems to have some overlap with the most nonspecific features of Kawasaki disease,” said Dr. Behrens, who is the Joseph Lee Hollander Chair in Pediatric Rheumatology at Children’s Hospital of Philadelphia. He has coauthored a study currently under review and available as a preprint soon that examines the biologic mechanisms underlying MIS-C.
Neither Dr. Behrens nor Dr. Whyte believed the findings had clinical implications that might change practice, but Dr. Whyte said he will be paying closer attention to the black children he treats – 99% of his practice – who are recovering from COVID-19.
“And, because we know that the concerns of African Americans are often overlooked in health care,” Dr. Whyte said, physicians should “pay a little more attention to symptom reporting on those kids, since there is a possibility that those kids would need hospitalization.”
All the patients in the study were treated with intravenous immunoglobulin, and corticosteroids were administered to 10 of them (48%). Their median hospital stay was 8 days (5 days in intensive care), and all were discharged without any deaths.
“Only one patient had symptoms suggestive of acute covid-19 and most had positive serum test results for IgG antibodies, suggesting that the development of Kawasaki disease in these patients is more likely to be the result of a postviral immunological reaction,” Dr. Toubiana and associates said.
The research received no external funding, and neither the authors nor other quoted physicians had any relevant financial disclosures.
SOURCE: Toubiana J et al. BMJ. 2020 Jun 3, doi: 10.1136 bmj.m2094.
More evidence has linked the Kawasaki-like multisystem inflammatory syndrome in children to COVID-19 and suggests that black children have a greater risk of the condition, according to a study published in the BMJ.
A small observational study in Paris found more than half of the 21 children who were admitted for the condition at the city’s pediatric hospital for COVID-19 patients were of African ancestry.
“The observation of a higher proportion of patients of African ancestry is consistent with recent findings, suggesting an effect of either social and living conditions or genetic susceptibility,” wrote Julie Toubiana, MD, PhD, of the University of Paris and the Pasteur Institute, and colleagues.
The findings did not surprise Edward M. Behrens, MD, chief of the division of rheumatology at Children’s Hospital of Philadelphia, whose institution has seen similar disparities that he attributes to social disadvantages.
“Infection rate will be higher in vulnerable populations that are less able to socially distance, have disproportionate numbers of essential workers, and have less access to health care and other resources,” Dr. Behrens said in an interview. “While there may be a role for genetics, environment – including social disparities – is almost certainly playing a role.”
Although the study’s small size is a limitation, he said, “the features described seem to mirror the experience of our center and what has been discussed more broadly amongst U.S. physicians.”
Byron Whyte, MD, a pediatrician in private practice in southeast Washington, found the differences in race interesting, but said the study was too small to draw any conclusions or generalize to the United States. But social disparities related to race are likely similar in France as they are in the United States, he said.
The prospective observational study assessed the clinical and demographic characteristics of all patients under age 18 who met the criteria for Kawasaki disease and were admitted between April 27 and May 20 to the Necker Hospital for Sick Children in Paris.
The 21 children had an average age of 8 years (ranging from 3 to 16), and 57% had at least one parent from sub-Saharan Africa or a Caribbean island; 14% had parents from Asia (two from China and one from Sri Lanka). The authors noted in their discussion that past U.S. and U.K. studies of Kawasaki disease have found a 2.5 times greater risk in Asian-American children and 1.5 times greater risk in African-American children compared with children with European ancestry.
Most of the patients (81%) needed intensive care, with 57% presenting with Kawasaki disease shock syndrome and 67% with myocarditis. Dr. Toubiana and associates also noted that “gastrointestinal symptoms were also unusually common, affecting all of our 21 patients.”
Only nine of the children reported having symptoms of a viral-like illness when they were admitted, primarily headache, cough, coryza, and fever, plus anosmia in one child. Among those children, the Kawasaki symptoms began a median 45 days after onset of the viral symptoms (range 18-79 days).
Only two children showed no positive test result for current COVID-19 infection or antibodies. Eight (38%) of the children had positive PCR tests for SARS-CoV2, and 19 (90%) had positive tests for IgG antibodies. The two patients with both negative tests did not require intensive care and did not have myocarditis.
About half the patients (52%) met all the criteria of Kawasaki disease, and the other 10 had “incomplete Kawasaki disease.” The most common Kawasaki symptoms were the polymorphous skin rash, occurring in 76% of the patients, changes to the lips and oral cavity (76%), and bilateral bulbar conjunctival injection (81%). Three patients (14%) had pleural effusion, and 10 of them (48%) had pericardial effusion, Dr. Toubiana and associates reported.
But Dr. Behrens said he disagrees with the assertion that the illness described in the paper and what he is seeing at Children’s Hospital of Philadelphia is related to Kawasaki disease.
“Most experts here in the U.S. seem to agree this is not Kawasaki disease, but a distinct clinical syndrome called multisystem inflammatory syndrome in children, or MIS-C, that seems to have some overlap with the most nonspecific features of Kawasaki disease,” said Dr. Behrens, who is the Joseph Lee Hollander Chair in Pediatric Rheumatology at Children’s Hospital of Philadelphia. He has coauthored a study currently under review and available as a preprint soon that examines the biologic mechanisms underlying MIS-C.
Neither Dr. Behrens nor Dr. Whyte believed the findings had clinical implications that might change practice, but Dr. Whyte said he will be paying closer attention to the black children he treats – 99% of his practice – who are recovering from COVID-19.
“And, because we know that the concerns of African Americans are often overlooked in health care,” Dr. Whyte said, physicians should “pay a little more attention to symptom reporting on those kids, since there is a possibility that those kids would need hospitalization.”
All the patients in the study were treated with intravenous immunoglobulin, and corticosteroids were administered to 10 of them (48%). Their median hospital stay was 8 days (5 days in intensive care), and all were discharged without any deaths.
“Only one patient had symptoms suggestive of acute covid-19 and most had positive serum test results for IgG antibodies, suggesting that the development of Kawasaki disease in these patients is more likely to be the result of a postviral immunological reaction,” Dr. Toubiana and associates said.
The research received no external funding, and neither the authors nor other quoted physicians had any relevant financial disclosures.
SOURCE: Toubiana J et al. BMJ. 2020 Jun 3, doi: 10.1136 bmj.m2094.
More evidence has linked the Kawasaki-like multisystem inflammatory syndrome in children to COVID-19 and suggests that black children have a greater risk of the condition, according to a study published in the BMJ.
A small observational study in Paris found more than half of the 21 children who were admitted for the condition at the city’s pediatric hospital for COVID-19 patients were of African ancestry.
“The observation of a higher proportion of patients of African ancestry is consistent with recent findings, suggesting an effect of either social and living conditions or genetic susceptibility,” wrote Julie Toubiana, MD, PhD, of the University of Paris and the Pasteur Institute, and colleagues.
The findings did not surprise Edward M. Behrens, MD, chief of the division of rheumatology at Children’s Hospital of Philadelphia, whose institution has seen similar disparities that he attributes to social disadvantages.
“Infection rate will be higher in vulnerable populations that are less able to socially distance, have disproportionate numbers of essential workers, and have less access to health care and other resources,” Dr. Behrens said in an interview. “While there may be a role for genetics, environment – including social disparities – is almost certainly playing a role.”
Although the study’s small size is a limitation, he said, “the features described seem to mirror the experience of our center and what has been discussed more broadly amongst U.S. physicians.”
Byron Whyte, MD, a pediatrician in private practice in southeast Washington, found the differences in race interesting, but said the study was too small to draw any conclusions or generalize to the United States. But social disparities related to race are likely similar in France as they are in the United States, he said.
The prospective observational study assessed the clinical and demographic characteristics of all patients under age 18 who met the criteria for Kawasaki disease and were admitted between April 27 and May 20 to the Necker Hospital for Sick Children in Paris.
The 21 children had an average age of 8 years (ranging from 3 to 16), and 57% had at least one parent from sub-Saharan Africa or a Caribbean island; 14% had parents from Asia (two from China and one from Sri Lanka). The authors noted in their discussion that past U.S. and U.K. studies of Kawasaki disease have found a 2.5 times greater risk in Asian-American children and 1.5 times greater risk in African-American children compared with children with European ancestry.
Most of the patients (81%) needed intensive care, with 57% presenting with Kawasaki disease shock syndrome and 67% with myocarditis. Dr. Toubiana and associates also noted that “gastrointestinal symptoms were also unusually common, affecting all of our 21 patients.”
Only nine of the children reported having symptoms of a viral-like illness when they were admitted, primarily headache, cough, coryza, and fever, plus anosmia in one child. Among those children, the Kawasaki symptoms began a median 45 days after onset of the viral symptoms (range 18-79 days).
Only two children showed no positive test result for current COVID-19 infection or antibodies. Eight (38%) of the children had positive PCR tests for SARS-CoV2, and 19 (90%) had positive tests for IgG antibodies. The two patients with both negative tests did not require intensive care and did not have myocarditis.
About half the patients (52%) met all the criteria of Kawasaki disease, and the other 10 had “incomplete Kawasaki disease.” The most common Kawasaki symptoms were the polymorphous skin rash, occurring in 76% of the patients, changes to the lips and oral cavity (76%), and bilateral bulbar conjunctival injection (81%). Three patients (14%) had pleural effusion, and 10 of them (48%) had pericardial effusion, Dr. Toubiana and associates reported.
But Dr. Behrens said he disagrees with the assertion that the illness described in the paper and what he is seeing at Children’s Hospital of Philadelphia is related to Kawasaki disease.
“Most experts here in the U.S. seem to agree this is not Kawasaki disease, but a distinct clinical syndrome called multisystem inflammatory syndrome in children, or MIS-C, that seems to have some overlap with the most nonspecific features of Kawasaki disease,” said Dr. Behrens, who is the Joseph Lee Hollander Chair in Pediatric Rheumatology at Children’s Hospital of Philadelphia. He has coauthored a study currently under review and available as a preprint soon that examines the biologic mechanisms underlying MIS-C.
Neither Dr. Behrens nor Dr. Whyte believed the findings had clinical implications that might change practice, but Dr. Whyte said he will be paying closer attention to the black children he treats – 99% of his practice – who are recovering from COVID-19.
“And, because we know that the concerns of African Americans are often overlooked in health care,” Dr. Whyte said, physicians should “pay a little more attention to symptom reporting on those kids, since there is a possibility that those kids would need hospitalization.”
All the patients in the study were treated with intravenous immunoglobulin, and corticosteroids were administered to 10 of them (48%). Their median hospital stay was 8 days (5 days in intensive care), and all were discharged without any deaths.
“Only one patient had symptoms suggestive of acute covid-19 and most had positive serum test results for IgG antibodies, suggesting that the development of Kawasaki disease in these patients is more likely to be the result of a postviral immunological reaction,” Dr. Toubiana and associates said.
The research received no external funding, and neither the authors nor other quoted physicians had any relevant financial disclosures.
SOURCE: Toubiana J et al. BMJ. 2020 Jun 3, doi: 10.1136 bmj.m2094.
FROM BMJ
COVID-19: Problematic gambling could worsen
The confluence of isolation, excess available time, and anxiety about illness or finances as a result of the COVID-19 pandemic have the potential to increase problem gambling behaviors during this public health emergency, so it’s essential to gather data and supply guidance on this issue, according to a call to action published May 18 in the Journal of Addiction Medicine.
“When facing an unforeseen situation with confinement, fear of disease, and financial uncertainty for the future, problem gambling may be an important health hazard to monitor and prevent during and following the COVID-19 crisis, especially given current online gambling availability,” wrote Anders Håkansson, PhD, of Lund University in Sweden and coauthors.
Both stress and trauma have been linked to gambling problems, and both are occurring during the pandemic, said coauthor Marc N. Potenza, MD, PhD, of Yale University, New Haven, Conn., in an interview.
“People are likely to be experiencing stress at levels they haven’t experienced previously,” Dr. Potenza said. While multiple factors can contribute to addictive behaviors, “with respect to the pandemic, one concern is that so-called negative reinforcement motivations – engaging in an addictive behavior to escape from depressed or negative mood states – may be a driving motivation for a significant number of people during this time,” he said.
David Hodgins, PhD, CPsych, a professor of psychology at the University of Calgary in Alberta, who was not involved with the commentary, noted that gambling relapse is triggered by “negative emotional states, interpersonal stress, and financial stress” – all three of which the pandemic contributes to.
Financial stress can especially “inflame erroneous gambling-related cognitions,” he said in an interview, including “beliefs such as the idea that gambling can solve financial problems, even when this is statistically almost impossible as debt increases, and that debt has been caused by gambling.”
Increased social isolation also is particularly problematic, pointed out Shane W. Kraus, PhD, from the University of Nevada, Las Vegas. Dr. Kraus also was not involved with the paper.
“If someone is already struggling with already negative emotions, negative feelings, thoughts, and depression, and you’re now isolating them quite a bit, that’s not going to be a recipe for success,” Dr. Kraus said in an interview.
Dr. Potenza said.
“We should be mindful of ways in which people develop addictions in these settings,” he said. “One of the aspects of the pandemic is that many people are at home for longer periods of time, and they use digital technologies more frequently.”
The use of digital technologies can include interaction on social media platforms and on meeting applications such as Zoom, but such use also offers opportunities for problematic gambling, gaming, and pornography use. The World Health Organization recognizes addiction disorders for gambling and for gaming, and online gaming platforms and pornography sites have reported substantial increases in their traffic during the pandemic, Dr. Potenza said.
The increase in frequency is unsurprising and not necessarily a concern by itself, Dr. Kraus said.
“It’s all about loss of control or difficulty engaging or disengaging,” Dr. Kraus said. “When you can’t stop doing something even if you like it or love it, when it interferes with your day-to-day activities and relationships, that’s when it’s a problem.”
Gambling online: Easy, available
The authors note that past research has identified increased gambling problems during economic crises in other countries.
“While currently speculative, financial hardships may promote gambling as individuals may be motivated to gamble to try to win money,” the authors suggested. “Although presently limited, existing data suggest that COVID-19–related financial concerns may increase gambling-related harms, and this possibility merits systematic research.”
But trends and characteristics of the gambling market, including direct effects from the pandemic, can potentially influence behaviors, too. Most casinos have closed during the pandemic, and most of the sports that people bet on have been canceled or postponed.
“Fewer people are gambling on sports, but they turn then to other areas,” Dr. Potenza said. “If they can’t bet on major league type sports, they might gamble on more local sporting events, or they may bet on other activities going on in society during the pandemic.”
But online gambling poses greater risk.
“Properties of online gambling may constitute a particular health hazard when many people are confined to their homes and have had rapid changes in working conditions, psychosocial stress, anxiety, and depression, as has been described in China,” the paper’s authors wrote. “Online gambling may be particularly concerning due to its availability and velocity” and association with higher debt levels.
In addition to online gaming’s ease and availability, past research has found patients report boredom and escapism as reasons they turned to it.
Again, boredom on its own is not necessarily a problem, but for those who already struggle with addictive behaviors, it can be a trigger, Dr. Kraus said.
“Boredom is very tough for them because it’s often associated with negative emotions,” such as dwelling on things not going well in their lives, he said. “In a pandemic, people are by themselves quite a bit, socially isolated, so for those who are struggling already with some depression or anxiety, it’s only going to be increased.”
Online gaming trends may vary with demographics, however. Dr. Kraus noted that his former clinic at the Veterans Administration has been seeing lower gambling in patients with addictive disorders, but those patients are also older and primarily frequented casinos.
“It’s going to depend on age and familiarity with technology,” he said, but even if older problem gamblers are not going to the Internet now, “let’s wait and see what happens in the next 2 or 3 months.”
The authors noted results from a small survey of patients in treatment for gambling addiction at the Bellvitge University Hospital in Barcelona, Spain, where two of the coauthors work. They conducted telephone surveys with 26 patients about the first 4 weeks of sheltering in place because of the coronavirus. All but four of the patients were male, and their average age was 45 years.
“Most presented worries about increased uncertainties, such as the negative impact on their work, risk of COVID-19 infection of themselves or their loved ones and their treatment,” the authors reported.
Although 19% were completely abstinent, an additional 12% (n = 3) reported worsened gambling. In addition, almost half (46%) reported anxiety symptoms and more than a quarter (27%) had depressive symptoms.
Appropriate care
A particularly complicating factor of the pandemic is how it has disrupted traditional ways of seeking health care, particularly with how much mental health and other medical care has shifted to telehealth and online delivery, Dr. Potenza pointed out.
“This is a change for many people, and it’s important for both caretakers and people in treatment to be mindful of this and to try to ensure that appropriate services are maintained for people during this time,” he said.
For example, 12-step programs traditionally meet in person, which is largely impossible during the pandemic. Some have moved meetings online, and other programs have turned to apps, such as the Addiction Policy Forum’s app Connections, an empirically validated digital therapy platform that lets patients and clinicians remain connected with remote check-ins.
The move to more telehealth may actually increase access, suggested Dr. Hodgins.
“There is no evidence that this is less effective, and in fact, its convenience might be an advantage in reaching more people,” he said. “More challenging is offering group therapies remotely, but this is also feasible.”
The treatment with the strongest evidence remains cognitive-behavioral therapy (CBT), Dr. Hodgins said.
“This therapy, in part, helps people become aware of their erroneous cognitions and to challenge them, but also helps people restructure their activities to change their habits,” he said. He also noted the rise of online therapy, whether supported by a therapist or entirely self-directed, such as Gambling Self-help.
“These programs typically provide cognitive behavior content but also content that comes from studying how people recover from gambling problems,” he said. “The challenge of completely self-directed approaches is follow-through. Like most online content, people tend to flit around more than they might in therapy.” Still, he added, research has shown good outcomes from these programs.
Dr. Potenza also noted that several organizations, including the International Society of Addiction Medicine and Children and Screens, have been hosting webinars related to COVID-19 coping and/or addiction that clinicians and patients might find helpful.
Identification of problematic behaviors
One challenge in watching for problematic gambling behaviors during the pandemic is the set of unusual living circumstances for most people right now. At almost no other time in history have people been primarily confined to their homes, many unable to go to work or working from home, with extra leisure time and nowhere to go.
“With the COVID-19 pandemic, a lot of daily life has changed,” Dr. Potenza said. “It’s unclear whether certain behaviors that have become habitual during the pandemic, such as gaming or online gambling, will then interfere with daily life when the pandemic subsides.”
“The problem is, a small proportion of people who are very vulnerable will develop a disorder and might maintain it,” Dr. Kraus said. Those who already struggle with mental health and may be out of work have greater potential for problematic behaviors.
Dr. Potenza collaborated with other psychiatrists in drafting consensus guidelines on maintaining healthy use of the Internet specifically during the pandemic (Compr Psychiatry. 2020 Jul. doi: 10.10161/comppsych.2020.152180).
“It’s important to think about where one draws the line between normative everyday behaviors – behaviors that are not interfering with life functioning – and those that do interfere with life functioning,” Dr. Potenza said. “If someone is having difficulty making work or family or school obligations, these are important signs that the behavior may be problematic.”
He offered suggestions for things people can do to promote their health during the pandemic, such as having regular routines that include getting physical exercise and social interaction, dining with family if isolating together, and making time for self-care. He also recommended setting limits on the use of digital devices and aiming for a healthy balance in keeping up with the news. The idea is to stay aware of what’s happening without getting burned out or traumatized by news coverage.
Guidance for clinicians
An urgent need for research and guidelines related to gambling and the pandemic exists, the authors argued.
In the meantime, aside from various validated screeners available, Dr. Kraus offered some practical advice for clinicians checking in with their patients: “Ask your patients what they have been doing to cope with this difficult time.”
Some might mention their faith, family, or friends, and others might not have an answer or mention drinking, gaming, or engaging in other activities. “We all do things to cope. Sometimes you use healthy coping and sometimes you use unhealthy coping,” Dr. Kraus said. “I would have a dialogue with my patients around, ‘How are you getting through? What’s helping you? What are some things you’ve tried that are tripping you up?’ ”
If gambling in particular is a possible concern, he encouraged clinicians to ask their patients whether they have tried to quit or what would happen if they stopped gambling.
“What we’d expect is the problem gamblers will have more irritability, crankiness, difficulty with quitting,” he said.
Dr. Hodgins agreed that checking in on how patients’ lives and activities have changed, and their emotion reactions to those changes, is prudent.
“The change in activities might be healthy or might include increased addictive behaviors, including increased use of substances, gaming, pornography, food, and gambling,” he said.
In addition, the paper authors list several examples of guidelines that might be considered in drafting guidance for clinicians, including the following:
- Limiting the extent of gambling
- Not gambling to regulate negative emotions
- Not gambling in order to try to solve financial problems or financial concerns
- Not gambling under the influence of alcohol or drugs
- Carefully monitoring gambling-related time and financial expenditures
- Maintaining and establishing daily routines involving activities other than gambling
- Minding gambling-related attitudes and behaviors in the presence of minors
- Not starting to gamble because of stressors
The research did not receive external funding. Dr. Håkansson has received research funding from the Swedish Sport Foundation, the Swedish alcohol monopoly Systembolaget, and the Swedish state-owned gambling operator AB Svenska Spel. He is working with the company Kontigo Care on devices for gambling addiction follow-up care. Dr. Potenza has received consulting or advisory compensation from several entities, including the Addiction Policy Forum, AXA Gaming, Idorsia, Opiant, and RiverMend Health. Dr. Potenza has received research funding from Mohegan Sun casino and the National Center for Responsible Gaming. No other authors or outside sources had industry-related disclosures.
SOURCE: Håkansson A et al. J Addict Med. 2020 May 18. doi: 10.1097/ADM.0000000000000690.
The confluence of isolation, excess available time, and anxiety about illness or finances as a result of the COVID-19 pandemic have the potential to increase problem gambling behaviors during this public health emergency, so it’s essential to gather data and supply guidance on this issue, according to a call to action published May 18 in the Journal of Addiction Medicine.
“When facing an unforeseen situation with confinement, fear of disease, and financial uncertainty for the future, problem gambling may be an important health hazard to monitor and prevent during and following the COVID-19 crisis, especially given current online gambling availability,” wrote Anders Håkansson, PhD, of Lund University in Sweden and coauthors.
Both stress and trauma have been linked to gambling problems, and both are occurring during the pandemic, said coauthor Marc N. Potenza, MD, PhD, of Yale University, New Haven, Conn., in an interview.
“People are likely to be experiencing stress at levels they haven’t experienced previously,” Dr. Potenza said. While multiple factors can contribute to addictive behaviors, “with respect to the pandemic, one concern is that so-called negative reinforcement motivations – engaging in an addictive behavior to escape from depressed or negative mood states – may be a driving motivation for a significant number of people during this time,” he said.
David Hodgins, PhD, CPsych, a professor of psychology at the University of Calgary in Alberta, who was not involved with the commentary, noted that gambling relapse is triggered by “negative emotional states, interpersonal stress, and financial stress” – all three of which the pandemic contributes to.
Financial stress can especially “inflame erroneous gambling-related cognitions,” he said in an interview, including “beliefs such as the idea that gambling can solve financial problems, even when this is statistically almost impossible as debt increases, and that debt has been caused by gambling.”
Increased social isolation also is particularly problematic, pointed out Shane W. Kraus, PhD, from the University of Nevada, Las Vegas. Dr. Kraus also was not involved with the paper.
“If someone is already struggling with already negative emotions, negative feelings, thoughts, and depression, and you’re now isolating them quite a bit, that’s not going to be a recipe for success,” Dr. Kraus said in an interview.
Dr. Potenza said.
“We should be mindful of ways in which people develop addictions in these settings,” he said. “One of the aspects of the pandemic is that many people are at home for longer periods of time, and they use digital technologies more frequently.”
The use of digital technologies can include interaction on social media platforms and on meeting applications such as Zoom, but such use also offers opportunities for problematic gambling, gaming, and pornography use. The World Health Organization recognizes addiction disorders for gambling and for gaming, and online gaming platforms and pornography sites have reported substantial increases in their traffic during the pandemic, Dr. Potenza said.
The increase in frequency is unsurprising and not necessarily a concern by itself, Dr. Kraus said.
“It’s all about loss of control or difficulty engaging or disengaging,” Dr. Kraus said. “When you can’t stop doing something even if you like it or love it, when it interferes with your day-to-day activities and relationships, that’s when it’s a problem.”
Gambling online: Easy, available
The authors note that past research has identified increased gambling problems during economic crises in other countries.
“While currently speculative, financial hardships may promote gambling as individuals may be motivated to gamble to try to win money,” the authors suggested. “Although presently limited, existing data suggest that COVID-19–related financial concerns may increase gambling-related harms, and this possibility merits systematic research.”
But trends and characteristics of the gambling market, including direct effects from the pandemic, can potentially influence behaviors, too. Most casinos have closed during the pandemic, and most of the sports that people bet on have been canceled or postponed.
“Fewer people are gambling on sports, but they turn then to other areas,” Dr. Potenza said. “If they can’t bet on major league type sports, they might gamble on more local sporting events, or they may bet on other activities going on in society during the pandemic.”
But online gambling poses greater risk.
“Properties of online gambling may constitute a particular health hazard when many people are confined to their homes and have had rapid changes in working conditions, psychosocial stress, anxiety, and depression, as has been described in China,” the paper’s authors wrote. “Online gambling may be particularly concerning due to its availability and velocity” and association with higher debt levels.
In addition to online gaming’s ease and availability, past research has found patients report boredom and escapism as reasons they turned to it.
Again, boredom on its own is not necessarily a problem, but for those who already struggle with addictive behaviors, it can be a trigger, Dr. Kraus said.
“Boredom is very tough for them because it’s often associated with negative emotions,” such as dwelling on things not going well in their lives, he said. “In a pandemic, people are by themselves quite a bit, socially isolated, so for those who are struggling already with some depression or anxiety, it’s only going to be increased.”
Online gaming trends may vary with demographics, however. Dr. Kraus noted that his former clinic at the Veterans Administration has been seeing lower gambling in patients with addictive disorders, but those patients are also older and primarily frequented casinos.
“It’s going to depend on age and familiarity with technology,” he said, but even if older problem gamblers are not going to the Internet now, “let’s wait and see what happens in the next 2 or 3 months.”
The authors noted results from a small survey of patients in treatment for gambling addiction at the Bellvitge University Hospital in Barcelona, Spain, where two of the coauthors work. They conducted telephone surveys with 26 patients about the first 4 weeks of sheltering in place because of the coronavirus. All but four of the patients were male, and their average age was 45 years.
“Most presented worries about increased uncertainties, such as the negative impact on their work, risk of COVID-19 infection of themselves or their loved ones and their treatment,” the authors reported.
Although 19% were completely abstinent, an additional 12% (n = 3) reported worsened gambling. In addition, almost half (46%) reported anxiety symptoms and more than a quarter (27%) had depressive symptoms.
Appropriate care
A particularly complicating factor of the pandemic is how it has disrupted traditional ways of seeking health care, particularly with how much mental health and other medical care has shifted to telehealth and online delivery, Dr. Potenza pointed out.
“This is a change for many people, and it’s important for both caretakers and people in treatment to be mindful of this and to try to ensure that appropriate services are maintained for people during this time,” he said.
For example, 12-step programs traditionally meet in person, which is largely impossible during the pandemic. Some have moved meetings online, and other programs have turned to apps, such as the Addiction Policy Forum’s app Connections, an empirically validated digital therapy platform that lets patients and clinicians remain connected with remote check-ins.
The move to more telehealth may actually increase access, suggested Dr. Hodgins.
“There is no evidence that this is less effective, and in fact, its convenience might be an advantage in reaching more people,” he said. “More challenging is offering group therapies remotely, but this is also feasible.”
The treatment with the strongest evidence remains cognitive-behavioral therapy (CBT), Dr. Hodgins said.
“This therapy, in part, helps people become aware of their erroneous cognitions and to challenge them, but also helps people restructure their activities to change their habits,” he said. He also noted the rise of online therapy, whether supported by a therapist or entirely self-directed, such as Gambling Self-help.
“These programs typically provide cognitive behavior content but also content that comes from studying how people recover from gambling problems,” he said. “The challenge of completely self-directed approaches is follow-through. Like most online content, people tend to flit around more than they might in therapy.” Still, he added, research has shown good outcomes from these programs.
Dr. Potenza also noted that several organizations, including the International Society of Addiction Medicine and Children and Screens, have been hosting webinars related to COVID-19 coping and/or addiction that clinicians and patients might find helpful.
Identification of problematic behaviors
One challenge in watching for problematic gambling behaviors during the pandemic is the set of unusual living circumstances for most people right now. At almost no other time in history have people been primarily confined to their homes, many unable to go to work or working from home, with extra leisure time and nowhere to go.
“With the COVID-19 pandemic, a lot of daily life has changed,” Dr. Potenza said. “It’s unclear whether certain behaviors that have become habitual during the pandemic, such as gaming or online gambling, will then interfere with daily life when the pandemic subsides.”
“The problem is, a small proportion of people who are very vulnerable will develop a disorder and might maintain it,” Dr. Kraus said. Those who already struggle with mental health and may be out of work have greater potential for problematic behaviors.
Dr. Potenza collaborated with other psychiatrists in drafting consensus guidelines on maintaining healthy use of the Internet specifically during the pandemic (Compr Psychiatry. 2020 Jul. doi: 10.10161/comppsych.2020.152180).
“It’s important to think about where one draws the line between normative everyday behaviors – behaviors that are not interfering with life functioning – and those that do interfere with life functioning,” Dr. Potenza said. “If someone is having difficulty making work or family or school obligations, these are important signs that the behavior may be problematic.”
He offered suggestions for things people can do to promote their health during the pandemic, such as having regular routines that include getting physical exercise and social interaction, dining with family if isolating together, and making time for self-care. He also recommended setting limits on the use of digital devices and aiming for a healthy balance in keeping up with the news. The idea is to stay aware of what’s happening without getting burned out or traumatized by news coverage.
Guidance for clinicians
An urgent need for research and guidelines related to gambling and the pandemic exists, the authors argued.
In the meantime, aside from various validated screeners available, Dr. Kraus offered some practical advice for clinicians checking in with their patients: “Ask your patients what they have been doing to cope with this difficult time.”
Some might mention their faith, family, or friends, and others might not have an answer or mention drinking, gaming, or engaging in other activities. “We all do things to cope. Sometimes you use healthy coping and sometimes you use unhealthy coping,” Dr. Kraus said. “I would have a dialogue with my patients around, ‘How are you getting through? What’s helping you? What are some things you’ve tried that are tripping you up?’ ”
If gambling in particular is a possible concern, he encouraged clinicians to ask their patients whether they have tried to quit or what would happen if they stopped gambling.
“What we’d expect is the problem gamblers will have more irritability, crankiness, difficulty with quitting,” he said.
Dr. Hodgins agreed that checking in on how patients’ lives and activities have changed, and their emotion reactions to those changes, is prudent.
“The change in activities might be healthy or might include increased addictive behaviors, including increased use of substances, gaming, pornography, food, and gambling,” he said.
In addition, the paper authors list several examples of guidelines that might be considered in drafting guidance for clinicians, including the following:
- Limiting the extent of gambling
- Not gambling to regulate negative emotions
- Not gambling in order to try to solve financial problems or financial concerns
- Not gambling under the influence of alcohol or drugs
- Carefully monitoring gambling-related time and financial expenditures
- Maintaining and establishing daily routines involving activities other than gambling
- Minding gambling-related attitudes and behaviors in the presence of minors
- Not starting to gamble because of stressors
The research did not receive external funding. Dr. Håkansson has received research funding from the Swedish Sport Foundation, the Swedish alcohol monopoly Systembolaget, and the Swedish state-owned gambling operator AB Svenska Spel. He is working with the company Kontigo Care on devices for gambling addiction follow-up care. Dr. Potenza has received consulting or advisory compensation from several entities, including the Addiction Policy Forum, AXA Gaming, Idorsia, Opiant, and RiverMend Health. Dr. Potenza has received research funding from Mohegan Sun casino and the National Center for Responsible Gaming. No other authors or outside sources had industry-related disclosures.
SOURCE: Håkansson A et al. J Addict Med. 2020 May 18. doi: 10.1097/ADM.0000000000000690.
The confluence of isolation, excess available time, and anxiety about illness or finances as a result of the COVID-19 pandemic have the potential to increase problem gambling behaviors during this public health emergency, so it’s essential to gather data and supply guidance on this issue, according to a call to action published May 18 in the Journal of Addiction Medicine.
“When facing an unforeseen situation with confinement, fear of disease, and financial uncertainty for the future, problem gambling may be an important health hazard to monitor and prevent during and following the COVID-19 crisis, especially given current online gambling availability,” wrote Anders Håkansson, PhD, of Lund University in Sweden and coauthors.
Both stress and trauma have been linked to gambling problems, and both are occurring during the pandemic, said coauthor Marc N. Potenza, MD, PhD, of Yale University, New Haven, Conn., in an interview.
“People are likely to be experiencing stress at levels they haven’t experienced previously,” Dr. Potenza said. While multiple factors can contribute to addictive behaviors, “with respect to the pandemic, one concern is that so-called negative reinforcement motivations – engaging in an addictive behavior to escape from depressed or negative mood states – may be a driving motivation for a significant number of people during this time,” he said.
David Hodgins, PhD, CPsych, a professor of psychology at the University of Calgary in Alberta, who was not involved with the commentary, noted that gambling relapse is triggered by “negative emotional states, interpersonal stress, and financial stress” – all three of which the pandemic contributes to.
Financial stress can especially “inflame erroneous gambling-related cognitions,” he said in an interview, including “beliefs such as the idea that gambling can solve financial problems, even when this is statistically almost impossible as debt increases, and that debt has been caused by gambling.”
Increased social isolation also is particularly problematic, pointed out Shane W. Kraus, PhD, from the University of Nevada, Las Vegas. Dr. Kraus also was not involved with the paper.
“If someone is already struggling with already negative emotions, negative feelings, thoughts, and depression, and you’re now isolating them quite a bit, that’s not going to be a recipe for success,” Dr. Kraus said in an interview.
Dr. Potenza said.
“We should be mindful of ways in which people develop addictions in these settings,” he said. “One of the aspects of the pandemic is that many people are at home for longer periods of time, and they use digital technologies more frequently.”
The use of digital technologies can include interaction on social media platforms and on meeting applications such as Zoom, but such use also offers opportunities for problematic gambling, gaming, and pornography use. The World Health Organization recognizes addiction disorders for gambling and for gaming, and online gaming platforms and pornography sites have reported substantial increases in their traffic during the pandemic, Dr. Potenza said.
The increase in frequency is unsurprising and not necessarily a concern by itself, Dr. Kraus said.
“It’s all about loss of control or difficulty engaging or disengaging,” Dr. Kraus said. “When you can’t stop doing something even if you like it or love it, when it interferes with your day-to-day activities and relationships, that’s when it’s a problem.”
Gambling online: Easy, available
The authors note that past research has identified increased gambling problems during economic crises in other countries.
“While currently speculative, financial hardships may promote gambling as individuals may be motivated to gamble to try to win money,” the authors suggested. “Although presently limited, existing data suggest that COVID-19–related financial concerns may increase gambling-related harms, and this possibility merits systematic research.”
But trends and characteristics of the gambling market, including direct effects from the pandemic, can potentially influence behaviors, too. Most casinos have closed during the pandemic, and most of the sports that people bet on have been canceled or postponed.
“Fewer people are gambling on sports, but they turn then to other areas,” Dr. Potenza said. “If they can’t bet on major league type sports, they might gamble on more local sporting events, or they may bet on other activities going on in society during the pandemic.”
But online gambling poses greater risk.
“Properties of online gambling may constitute a particular health hazard when many people are confined to their homes and have had rapid changes in working conditions, psychosocial stress, anxiety, and depression, as has been described in China,” the paper’s authors wrote. “Online gambling may be particularly concerning due to its availability and velocity” and association with higher debt levels.
In addition to online gaming’s ease and availability, past research has found patients report boredom and escapism as reasons they turned to it.
Again, boredom on its own is not necessarily a problem, but for those who already struggle with addictive behaviors, it can be a trigger, Dr. Kraus said.
“Boredom is very tough for them because it’s often associated with negative emotions,” such as dwelling on things not going well in their lives, he said. “In a pandemic, people are by themselves quite a bit, socially isolated, so for those who are struggling already with some depression or anxiety, it’s only going to be increased.”
Online gaming trends may vary with demographics, however. Dr. Kraus noted that his former clinic at the Veterans Administration has been seeing lower gambling in patients with addictive disorders, but those patients are also older and primarily frequented casinos.
“It’s going to depend on age and familiarity with technology,” he said, but even if older problem gamblers are not going to the Internet now, “let’s wait and see what happens in the next 2 or 3 months.”
The authors noted results from a small survey of patients in treatment for gambling addiction at the Bellvitge University Hospital in Barcelona, Spain, where two of the coauthors work. They conducted telephone surveys with 26 patients about the first 4 weeks of sheltering in place because of the coronavirus. All but four of the patients were male, and their average age was 45 years.
“Most presented worries about increased uncertainties, such as the negative impact on their work, risk of COVID-19 infection of themselves or their loved ones and their treatment,” the authors reported.
Although 19% were completely abstinent, an additional 12% (n = 3) reported worsened gambling. In addition, almost half (46%) reported anxiety symptoms and more than a quarter (27%) had depressive symptoms.
Appropriate care
A particularly complicating factor of the pandemic is how it has disrupted traditional ways of seeking health care, particularly with how much mental health and other medical care has shifted to telehealth and online delivery, Dr. Potenza pointed out.
“This is a change for many people, and it’s important for both caretakers and people in treatment to be mindful of this and to try to ensure that appropriate services are maintained for people during this time,” he said.
For example, 12-step programs traditionally meet in person, which is largely impossible during the pandemic. Some have moved meetings online, and other programs have turned to apps, such as the Addiction Policy Forum’s app Connections, an empirically validated digital therapy platform that lets patients and clinicians remain connected with remote check-ins.
The move to more telehealth may actually increase access, suggested Dr. Hodgins.
“There is no evidence that this is less effective, and in fact, its convenience might be an advantage in reaching more people,” he said. “More challenging is offering group therapies remotely, but this is also feasible.”
The treatment with the strongest evidence remains cognitive-behavioral therapy (CBT), Dr. Hodgins said.
“This therapy, in part, helps people become aware of their erroneous cognitions and to challenge them, but also helps people restructure their activities to change their habits,” he said. He also noted the rise of online therapy, whether supported by a therapist or entirely self-directed, such as Gambling Self-help.
“These programs typically provide cognitive behavior content but also content that comes from studying how people recover from gambling problems,” he said. “The challenge of completely self-directed approaches is follow-through. Like most online content, people tend to flit around more than they might in therapy.” Still, he added, research has shown good outcomes from these programs.
Dr. Potenza also noted that several organizations, including the International Society of Addiction Medicine and Children and Screens, have been hosting webinars related to COVID-19 coping and/or addiction that clinicians and patients might find helpful.
Identification of problematic behaviors
One challenge in watching for problematic gambling behaviors during the pandemic is the set of unusual living circumstances for most people right now. At almost no other time in history have people been primarily confined to their homes, many unable to go to work or working from home, with extra leisure time and nowhere to go.
“With the COVID-19 pandemic, a lot of daily life has changed,” Dr. Potenza said. “It’s unclear whether certain behaviors that have become habitual during the pandemic, such as gaming or online gambling, will then interfere with daily life when the pandemic subsides.”
“The problem is, a small proportion of people who are very vulnerable will develop a disorder and might maintain it,” Dr. Kraus said. Those who already struggle with mental health and may be out of work have greater potential for problematic behaviors.
Dr. Potenza collaborated with other psychiatrists in drafting consensus guidelines on maintaining healthy use of the Internet specifically during the pandemic (Compr Psychiatry. 2020 Jul. doi: 10.10161/comppsych.2020.152180).
“It’s important to think about where one draws the line between normative everyday behaviors – behaviors that are not interfering with life functioning – and those that do interfere with life functioning,” Dr. Potenza said. “If someone is having difficulty making work or family or school obligations, these are important signs that the behavior may be problematic.”
He offered suggestions for things people can do to promote their health during the pandemic, such as having regular routines that include getting physical exercise and social interaction, dining with family if isolating together, and making time for self-care. He also recommended setting limits on the use of digital devices and aiming for a healthy balance in keeping up with the news. The idea is to stay aware of what’s happening without getting burned out or traumatized by news coverage.
Guidance for clinicians
An urgent need for research and guidelines related to gambling and the pandemic exists, the authors argued.
In the meantime, aside from various validated screeners available, Dr. Kraus offered some practical advice for clinicians checking in with their patients: “Ask your patients what they have been doing to cope with this difficult time.”
Some might mention their faith, family, or friends, and others might not have an answer or mention drinking, gaming, or engaging in other activities. “We all do things to cope. Sometimes you use healthy coping and sometimes you use unhealthy coping,” Dr. Kraus said. “I would have a dialogue with my patients around, ‘How are you getting through? What’s helping you? What are some things you’ve tried that are tripping you up?’ ”
If gambling in particular is a possible concern, he encouraged clinicians to ask their patients whether they have tried to quit or what would happen if they stopped gambling.
“What we’d expect is the problem gamblers will have more irritability, crankiness, difficulty with quitting,” he said.
Dr. Hodgins agreed that checking in on how patients’ lives and activities have changed, and their emotion reactions to those changes, is prudent.
“The change in activities might be healthy or might include increased addictive behaviors, including increased use of substances, gaming, pornography, food, and gambling,” he said.
In addition, the paper authors list several examples of guidelines that might be considered in drafting guidance for clinicians, including the following:
- Limiting the extent of gambling
- Not gambling to regulate negative emotions
- Not gambling in order to try to solve financial problems or financial concerns
- Not gambling under the influence of alcohol or drugs
- Carefully monitoring gambling-related time and financial expenditures
- Maintaining and establishing daily routines involving activities other than gambling
- Minding gambling-related attitudes and behaviors in the presence of minors
- Not starting to gamble because of stressors
The research did not receive external funding. Dr. Håkansson has received research funding from the Swedish Sport Foundation, the Swedish alcohol monopoly Systembolaget, and the Swedish state-owned gambling operator AB Svenska Spel. He is working with the company Kontigo Care on devices for gambling addiction follow-up care. Dr. Potenza has received consulting or advisory compensation from several entities, including the Addiction Policy Forum, AXA Gaming, Idorsia, Opiant, and RiverMend Health. Dr. Potenza has received research funding from Mohegan Sun casino and the National Center for Responsible Gaming. No other authors or outside sources had industry-related disclosures.
SOURCE: Håkansson A et al. J Addict Med. 2020 May 18. doi: 10.1097/ADM.0000000000000690.
FROM THE JOURNAL OF ADDICTION MEDICINE