User login
Group produces malaria vaccine candidate from algae
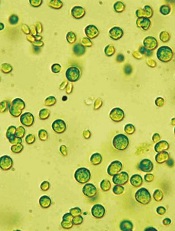
Image from Bielefeld University
A vaccine candidate generated using algae may be able to prevent the transmission of malaria from infected hosts to mosquitoes, preclinical research suggests.
Researchers used Chlamydomonas reinhardtii microalgae to produce recombinant Pfs25 protein.
When paired with human-compatible adjuvants—glucopyranosal lipid A (GLA) plus squalene oil-in-water emulsion—the protein generated antibodies that nearly eliminated malaria infection in mosquitoes.
The researchers reported these results in Infection and Immunity.
“Most malaria vaccine approaches are aimed at preventing humans from becoming infected when bitten by mosquitoes that carry the parasite,” said study author Joseph Vinetz, MD, of the University of California, San Diego.
“Our approach is to prevent transmission of the malaria parasite from infected humans to mosquitoes. This approach is similar to that of the current measles vaccine, which is such a hot topic of discussion these days, because the goal is to generate herd immunity in a population. We think that this approach is key to global malaria elimination too.”
Dr Vinetz and his colleagues wanted to produce a large quantity of properly folded Pfs25, a protein found on the surface of the malaria parasite’s reproductive cells, which are only present within the mosquito’s gut after it feeds on a malaria-infected blood meal.
Since antibodies against Pfs25 can halt the parasite’s lifecycle in the mosquito, they might also block transmission of the parasite to the next host. However, properly folded Pfs25 that induces transmission-blocking antibodies has been difficult to produce in the lab.
To overcome this problem, the researchers turned to Chlamydomonas reinhardtii. They introduced the Pfs25 gene into the algae by shooting the DNA into the plant cell’s nucleus.
After they let the algae do the work of replicating, building, and folding the protein, the team was able to purify enough functional Pfs25 for testing.
They also tested different adjuvants, which help stimulate the immune system’s response to Pfs25. They tested alum alone, GLA plus alum, squalene oil-in-water emulsion, and GLA plus squalene oil-in-water emulsion.
The best Pfs25/adjuvant combination—GLA plus squalene oil-in-water emulsion—elicited a uniquely robust antibody response in mice with high affinity and avidity—antibodies that specifically and strongly reacted with the malaria parasite’s reproductive cells.
The researchers then fed mosquitoes malaria parasites in the presence of control serum or immune serum collected from mice vaccinated with algae-produced Pfs25 in the presence of the adjuvants.
Eight days later, the team examined the mosquitoes’ guts for the presence of the malaria parasite. And they found that 4.2% (1/24) of mosquitoes that consumed the Pfs25/adjuvant-treated mouse serum were positive for the malaria parasite, compared to 70% (28/40) of control mosquitoes.
“We are really excited to see that Pfs25 produced by algae can effectively prevent malaria parasites from developing within the mosquito,” said study author Stephen Mayfield, PhD, of the University of California, San Diego.
“With the low cost of algal production, this may be the only system that can make an economic malaria vaccine. Now, we’re looking forward to comparing algae-produced Pfs25 and adjuvant head-to-head against other approaches to malaria vaccine production and administration.” ![]()

Image from Bielefeld University
A vaccine candidate generated using algae may be able to prevent the transmission of malaria from infected hosts to mosquitoes, preclinical research suggests.
Researchers used Chlamydomonas reinhardtii microalgae to produce recombinant Pfs25 protein.
When paired with human-compatible adjuvants—glucopyranosal lipid A (GLA) plus squalene oil-in-water emulsion—the protein generated antibodies that nearly eliminated malaria infection in mosquitoes.
The researchers reported these results in Infection and Immunity.
“Most malaria vaccine approaches are aimed at preventing humans from becoming infected when bitten by mosquitoes that carry the parasite,” said study author Joseph Vinetz, MD, of the University of California, San Diego.
“Our approach is to prevent transmission of the malaria parasite from infected humans to mosquitoes. This approach is similar to that of the current measles vaccine, which is such a hot topic of discussion these days, because the goal is to generate herd immunity in a population. We think that this approach is key to global malaria elimination too.”
Dr Vinetz and his colleagues wanted to produce a large quantity of properly folded Pfs25, a protein found on the surface of the malaria parasite’s reproductive cells, which are only present within the mosquito’s gut after it feeds on a malaria-infected blood meal.
Since antibodies against Pfs25 can halt the parasite’s lifecycle in the mosquito, they might also block transmission of the parasite to the next host. However, properly folded Pfs25 that induces transmission-blocking antibodies has been difficult to produce in the lab.
To overcome this problem, the researchers turned to Chlamydomonas reinhardtii. They introduced the Pfs25 gene into the algae by shooting the DNA into the plant cell’s nucleus.
After they let the algae do the work of replicating, building, and folding the protein, the team was able to purify enough functional Pfs25 for testing.
They also tested different adjuvants, which help stimulate the immune system’s response to Pfs25. They tested alum alone, GLA plus alum, squalene oil-in-water emulsion, and GLA plus squalene oil-in-water emulsion.
The best Pfs25/adjuvant combination—GLA plus squalene oil-in-water emulsion—elicited a uniquely robust antibody response in mice with high affinity and avidity—antibodies that specifically and strongly reacted with the malaria parasite’s reproductive cells.
The researchers then fed mosquitoes malaria parasites in the presence of control serum or immune serum collected from mice vaccinated with algae-produced Pfs25 in the presence of the adjuvants.
Eight days later, the team examined the mosquitoes’ guts for the presence of the malaria parasite. And they found that 4.2% (1/24) of mosquitoes that consumed the Pfs25/adjuvant-treated mouse serum were positive for the malaria parasite, compared to 70% (28/40) of control mosquitoes.
“We are really excited to see that Pfs25 produced by algae can effectively prevent malaria parasites from developing within the mosquito,” said study author Stephen Mayfield, PhD, of the University of California, San Diego.
“With the low cost of algal production, this may be the only system that can make an economic malaria vaccine. Now, we’re looking forward to comparing algae-produced Pfs25 and adjuvant head-to-head against other approaches to malaria vaccine production and administration.” ![]()

Image from Bielefeld University
A vaccine candidate generated using algae may be able to prevent the transmission of malaria from infected hosts to mosquitoes, preclinical research suggests.
Researchers used Chlamydomonas reinhardtii microalgae to produce recombinant Pfs25 protein.
When paired with human-compatible adjuvants—glucopyranosal lipid A (GLA) plus squalene oil-in-water emulsion—the protein generated antibodies that nearly eliminated malaria infection in mosquitoes.
The researchers reported these results in Infection and Immunity.
“Most malaria vaccine approaches are aimed at preventing humans from becoming infected when bitten by mosquitoes that carry the parasite,” said study author Joseph Vinetz, MD, of the University of California, San Diego.
“Our approach is to prevent transmission of the malaria parasite from infected humans to mosquitoes. This approach is similar to that of the current measles vaccine, which is such a hot topic of discussion these days, because the goal is to generate herd immunity in a population. We think that this approach is key to global malaria elimination too.”
Dr Vinetz and his colleagues wanted to produce a large quantity of properly folded Pfs25, a protein found on the surface of the malaria parasite’s reproductive cells, which are only present within the mosquito’s gut after it feeds on a malaria-infected blood meal.
Since antibodies against Pfs25 can halt the parasite’s lifecycle in the mosquito, they might also block transmission of the parasite to the next host. However, properly folded Pfs25 that induces transmission-blocking antibodies has been difficult to produce in the lab.
To overcome this problem, the researchers turned to Chlamydomonas reinhardtii. They introduced the Pfs25 gene into the algae by shooting the DNA into the plant cell’s nucleus.
After they let the algae do the work of replicating, building, and folding the protein, the team was able to purify enough functional Pfs25 for testing.
They also tested different adjuvants, which help stimulate the immune system’s response to Pfs25. They tested alum alone, GLA plus alum, squalene oil-in-water emulsion, and GLA plus squalene oil-in-water emulsion.
The best Pfs25/adjuvant combination—GLA plus squalene oil-in-water emulsion—elicited a uniquely robust antibody response in mice with high affinity and avidity—antibodies that specifically and strongly reacted with the malaria parasite’s reproductive cells.
The researchers then fed mosquitoes malaria parasites in the presence of control serum or immune serum collected from mice vaccinated with algae-produced Pfs25 in the presence of the adjuvants.
Eight days later, the team examined the mosquitoes’ guts for the presence of the malaria parasite. And they found that 4.2% (1/24) of mosquitoes that consumed the Pfs25/adjuvant-treated mouse serum were positive for the malaria parasite, compared to 70% (28/40) of control mosquitoes.
“We are really excited to see that Pfs25 produced by algae can effectively prevent malaria parasites from developing within the mosquito,” said study author Stephen Mayfield, PhD, of the University of California, San Diego.
“With the low cost of algal production, this may be the only system that can make an economic malaria vaccine. Now, we’re looking forward to comparing algae-produced Pfs25 and adjuvant head-to-head against other approaches to malaria vaccine production and administration.” ![]()
Silk-based bone marrow system produces functional platelets

proplatelets (green) that will
become mature platelets
Image from Tufts University
Researchers say they’ve developed a 3-dimensional system that reproduces the structure and physiology of human bone marrow.
Using this silk-based bone marrow niche tissue system, the team was able to manufacture functional human platelets.
The system might also prove useful for studying platelet-related diseases and predicting the efficacy of new drugs, according to the researchers, who said the new system could be a more precise and cheaper alternative to animal models.
“There are many diseases where platelet production or function is impaired,” said Alessandra Balduini, MD, of Tufts University in Medford, Massachusetts.
“New insight into the formation of platelets would have a major impact on patients and healthcare. In this tissue system, we can culture patient-derived megakaryocytes—the bone marrow cells that make platelets—and also endothelial cells, which are found in bone marrow and promote platelet production, to design patient-specific drug administration regimens.”
Dr Balduini and her colleagues described the system in Blood.
The system combined microtubes spun of silk, collagen, and fibronectin surrounded by a porous silk sponge. Megakaryocytes—some derived from patients—were seeded into the engineered microvasculature.
The researchers were able to increase platelet production in the bioreactor by embedding the silk with active endothelial cells and endothelial-related molecular proteins that support platelet formation.
The special properties of silk protein were essential to successfully mimicking the bone marrow microenvironment, said study author David Kaplan, PhD, of Tufts University.
“Silk protein possesses a unique molecular structure that enables it to be modeled in a wide variety of forms and stiffnesses, characteristics that have been shown to affect platelet formation and release,” Dr Kaplan said.
“Furthermore, silk is biocompatible and has the ability to stabilize bioactive agents at normal temperatures. Therefore, we can ‘functionalize’ it by adding such agents.”
In addition, the silk is nonactivating to platelets, which allowed the researchers to collect functional platelets from the bioreactor. Tests showed the platelets were able to aggregate and clot.
Although the number of platelets produced per megakaryocyte was lower than normally made in the body, the researchers said the system represents a significant advance over previous models. The scalable nature of the bioreactor system provides engineering options to increase the yield of platelets in ongoing studies.
In addition to providing a platform for studying the processes that regulate platelet production and related diseases, the researchers hope the platelets produced can be used as a source of growth factors for wound healing in regenerative medicine.
“The need for platelet production systems to treat patients with related diseases is significant,” Dr Kaplan said. “This patient-specific system could provide new insight and options for clinical treatments.”
“Further, the platelets can be generated on demand, avoiding the complications of storage problems, and in greater quantities and with better quality and control in terms of morphology and function.” ![]()

proplatelets (green) that will
become mature platelets
Image from Tufts University
Researchers say they’ve developed a 3-dimensional system that reproduces the structure and physiology of human bone marrow.
Using this silk-based bone marrow niche tissue system, the team was able to manufacture functional human platelets.
The system might also prove useful for studying platelet-related diseases and predicting the efficacy of new drugs, according to the researchers, who said the new system could be a more precise and cheaper alternative to animal models.
“There are many diseases where platelet production or function is impaired,” said Alessandra Balduini, MD, of Tufts University in Medford, Massachusetts.
“New insight into the formation of platelets would have a major impact on patients and healthcare. In this tissue system, we can culture patient-derived megakaryocytes—the bone marrow cells that make platelets—and also endothelial cells, which are found in bone marrow and promote platelet production, to design patient-specific drug administration regimens.”
Dr Balduini and her colleagues described the system in Blood.
The system combined microtubes spun of silk, collagen, and fibronectin surrounded by a porous silk sponge. Megakaryocytes—some derived from patients—were seeded into the engineered microvasculature.
The researchers were able to increase platelet production in the bioreactor by embedding the silk with active endothelial cells and endothelial-related molecular proteins that support platelet formation.
The special properties of silk protein were essential to successfully mimicking the bone marrow microenvironment, said study author David Kaplan, PhD, of Tufts University.
“Silk protein possesses a unique molecular structure that enables it to be modeled in a wide variety of forms and stiffnesses, characteristics that have been shown to affect platelet formation and release,” Dr Kaplan said.
“Furthermore, silk is biocompatible and has the ability to stabilize bioactive agents at normal temperatures. Therefore, we can ‘functionalize’ it by adding such agents.”
In addition, the silk is nonactivating to platelets, which allowed the researchers to collect functional platelets from the bioreactor. Tests showed the platelets were able to aggregate and clot.
Although the number of platelets produced per megakaryocyte was lower than normally made in the body, the researchers said the system represents a significant advance over previous models. The scalable nature of the bioreactor system provides engineering options to increase the yield of platelets in ongoing studies.
In addition to providing a platform for studying the processes that regulate platelet production and related diseases, the researchers hope the platelets produced can be used as a source of growth factors for wound healing in regenerative medicine.
“The need for platelet production systems to treat patients with related diseases is significant,” Dr Kaplan said. “This patient-specific system could provide new insight and options for clinical treatments.”
“Further, the platelets can be generated on demand, avoiding the complications of storage problems, and in greater quantities and with better quality and control in terms of morphology and function.” ![]()

proplatelets (green) that will
become mature platelets
Image from Tufts University
Researchers say they’ve developed a 3-dimensional system that reproduces the structure and physiology of human bone marrow.
Using this silk-based bone marrow niche tissue system, the team was able to manufacture functional human platelets.
The system might also prove useful for studying platelet-related diseases and predicting the efficacy of new drugs, according to the researchers, who said the new system could be a more precise and cheaper alternative to animal models.
“There are many diseases where platelet production or function is impaired,” said Alessandra Balduini, MD, of Tufts University in Medford, Massachusetts.
“New insight into the formation of platelets would have a major impact on patients and healthcare. In this tissue system, we can culture patient-derived megakaryocytes—the bone marrow cells that make platelets—and also endothelial cells, which are found in bone marrow and promote platelet production, to design patient-specific drug administration regimens.”
Dr Balduini and her colleagues described the system in Blood.
The system combined microtubes spun of silk, collagen, and fibronectin surrounded by a porous silk sponge. Megakaryocytes—some derived from patients—were seeded into the engineered microvasculature.
The researchers were able to increase platelet production in the bioreactor by embedding the silk with active endothelial cells and endothelial-related molecular proteins that support platelet formation.
The special properties of silk protein were essential to successfully mimicking the bone marrow microenvironment, said study author David Kaplan, PhD, of Tufts University.
“Silk protein possesses a unique molecular structure that enables it to be modeled in a wide variety of forms and stiffnesses, characteristics that have been shown to affect platelet formation and release,” Dr Kaplan said.
“Furthermore, silk is biocompatible and has the ability to stabilize bioactive agents at normal temperatures. Therefore, we can ‘functionalize’ it by adding such agents.”
In addition, the silk is nonactivating to platelets, which allowed the researchers to collect functional platelets from the bioreactor. Tests showed the platelets were able to aggregate and clot.
Although the number of platelets produced per megakaryocyte was lower than normally made in the body, the researchers said the system represents a significant advance over previous models. The scalable nature of the bioreactor system provides engineering options to increase the yield of platelets in ongoing studies.
In addition to providing a platform for studying the processes that regulate platelet production and related diseases, the researchers hope the platelets produced can be used as a source of growth factors for wound healing in regenerative medicine.
“The need for platelet production systems to treat patients with related diseases is significant,” Dr Kaplan said. “This patient-specific system could provide new insight and options for clinical treatments.”
“Further, the platelets can be generated on demand, avoiding the complications of storage problems, and in greater quantities and with better quality and control in terms of morphology and function.” ![]()
Researchers map the human epigenome
to the Epigenome Roadmap
Image by Nik Spencer/Nature
Scientists have created new maps of the human epigenome that may help unravel the complex links between DNA and disease.
Researchers supported by the Common Fund’s Epigenomics Program have mapped the epigenomes of more than 100 types of cells and tissues, providing new insight into which parts of the genome are used to make a particular type of cell.
The group published an article describing the epigenome maps in the journal Nature.
Twenty-three additional papers in Nature Publishing Group journals show how these maps can be used to study human biology.
The papers are available on Nature’s Epigenome Roadmap site.
For the Roadmap Epigenomics Project, scientists compared epigenomic signatures and established their differences across a variety of cell types. The resulting information may help us understand how changes to the genome and epigenome can lead to cancers and other conditions.
“These 111 reference epigenome maps are essentially a vocabulary book that helps us decipher each DNA segment in distinct cell and tissue types,” said Bing Ren, PhD, of the University of California, San Diego.
For cancer research, the new data will hasten a merging of genomic and epigenomic perspectives that was already underway, according to Joseph F. Costello, PhD, of the University of California, San Francisco.
“You’ve had cancer researchers studying the genome—the role of mutations, deletions, and so on—and others studying epigenomes,” Dr Costello said. “They’ve almost been working on parallel tracks, and they didn’t talk to each other all that much.”
“Over the past 5 or 6 years, there’s been a reframing of the discussion, because the most recurrent mutations in cancer affect epigenomic regulators. So the way mutations in the genome play out is through epigenomic mechanisms, and major pharmaceutical companies now view epigenomes as an important target.” ![]()

to the Epigenome Roadmap
Image by Nik Spencer/Nature
Scientists have created new maps of the human epigenome that may help unravel the complex links between DNA and disease.
Researchers supported by the Common Fund’s Epigenomics Program have mapped the epigenomes of more than 100 types of cells and tissues, providing new insight into which parts of the genome are used to make a particular type of cell.
The group published an article describing the epigenome maps in the journal Nature.
Twenty-three additional papers in Nature Publishing Group journals show how these maps can be used to study human biology.
The papers are available on Nature’s Epigenome Roadmap site.
For the Roadmap Epigenomics Project, scientists compared epigenomic signatures and established their differences across a variety of cell types. The resulting information may help us understand how changes to the genome and epigenome can lead to cancers and other conditions.
“These 111 reference epigenome maps are essentially a vocabulary book that helps us decipher each DNA segment in distinct cell and tissue types,” said Bing Ren, PhD, of the University of California, San Diego.
For cancer research, the new data will hasten a merging of genomic and epigenomic perspectives that was already underway, according to Joseph F. Costello, PhD, of the University of California, San Francisco.
“You’ve had cancer researchers studying the genome—the role of mutations, deletions, and so on—and others studying epigenomes,” Dr Costello said. “They’ve almost been working on parallel tracks, and they didn’t talk to each other all that much.”
“Over the past 5 or 6 years, there’s been a reframing of the discussion, because the most recurrent mutations in cancer affect epigenomic regulators. So the way mutations in the genome play out is through epigenomic mechanisms, and major pharmaceutical companies now view epigenomes as an important target.” ![]()

to the Epigenome Roadmap
Image by Nik Spencer/Nature
Scientists have created new maps of the human epigenome that may help unravel the complex links between DNA and disease.
Researchers supported by the Common Fund’s Epigenomics Program have mapped the epigenomes of more than 100 types of cells and tissues, providing new insight into which parts of the genome are used to make a particular type of cell.
The group published an article describing the epigenome maps in the journal Nature.
Twenty-three additional papers in Nature Publishing Group journals show how these maps can be used to study human biology.
The papers are available on Nature’s Epigenome Roadmap site.
For the Roadmap Epigenomics Project, scientists compared epigenomic signatures and established their differences across a variety of cell types. The resulting information may help us understand how changes to the genome and epigenome can lead to cancers and other conditions.
“These 111 reference epigenome maps are essentially a vocabulary book that helps us decipher each DNA segment in distinct cell and tissue types,” said Bing Ren, PhD, of the University of California, San Diego.
For cancer research, the new data will hasten a merging of genomic and epigenomic perspectives that was already underway, according to Joseph F. Costello, PhD, of the University of California, San Francisco.
“You’ve had cancer researchers studying the genome—the role of mutations, deletions, and so on—and others studying epigenomes,” Dr Costello said. “They’ve almost been working on parallel tracks, and they didn’t talk to each other all that much.”
“Over the past 5 or 6 years, there’s been a reframing of the discussion, because the most recurrent mutations in cancer affect epigenomic regulators. So the way mutations in the genome play out is through epigenomic mechanisms, and major pharmaceutical companies now view epigenomes as an important target.” ![]()
FDA issues documents on drug compounding

Photo by Rhoda Baer
The US Food and Drug Administration (FDA) has issued 5 draft documents related to drug compounding and repackaging that aim to help entities comply with public health provisions.
The agency said these draft documents are applicable to pharmacies, federal facilities, outsourcing facilities, and physicians.
The new category of outsourcing facilities was created under the Drug Quality and Security Act (DQSA), which was enacted by Congress in November 2013.
It was enacted in response to a deadly fungal meningitis outbreak that was linked to contaminated sterile compounded drug products.
Drugs compounded in an outsourcing facility that meet certain conditions may be entitled to exemptions from certain provisions of the Federal Food, Drug, and Cosmetic Act (FD&C Act), including the new drug approval requirements and the requirement to label drug products with adequate directions for use.
Outsourcing facilities are subject to current good manufacturing practice requirements and inspections by the FDA according to a risk-based schedule.
Drugs produced by compounders that are not registered as outsourcing facilities must meet certain other conditions described in the FD&C Act, or they will be subject to all of the requirements applicable to drugs produced by conventional drug manufacturers.
“The draft guidance documents provide information to pharmacies, outsourcing facilities, healthcare entities, and others about these FDA-proposed policies, which are critical to protecting the public health,” said Janet Woodcock, MD, director of the FDA’s Center for Drug Evaluation and Research.
Descriptions of these documents follow.
This draft guidance provides an entity considering whether to register with the FDA as an outsourcing facility with information about the regulatory impact of registering.
For example, it explains that a facility engaged in only certain activities, including repackaging human drugs and compounding non-sterile drugs, should not register as an outsourcing facility because its drug products will not qualify for the exemptions provided in section 503B, including the exemption from the new drug approval requirements.
This draft guidance describes the conditions under which the FDA does not intend to take action for certain violations of the law when state-licensed pharmacies, federal facilities, or outsourcing facilities repackage certain drug products.
Repackaged drug products are generally not exempt from any of the provisions of the FD&C Act related to the production of drugs, and the compounding provisions of the FD&C Act do not address repackaging. Therefore, the FDA is issuing guidance to describe how it intends to address repackaging when done in a state-licensed pharmacy, federal facility, or outsourcing facility.
This draft guidance describes the conditions under which the FDA does not intend to take action for violations of certain sections of the Public Health Service Act (PHS Act) and the FD&C Act when state-licensed pharmacies, federal facilities, or outsourcing facilities mix, dilute, or repackage specific biological products without an approved BLA, or when such facilities or physicians prepare prescription sets of allergenic extracts without an approved BLA.
The draft guidance notes that a biological product that is mixed, diluted, or repackaged outside the scope of an approved BLA is an unlicensed biological product under section 351 of the PHS Act and may not be legally marketed without an approved BLA.
Additionally, the compounding provisions of the FD&C Act do not address biological products subject to licensure under section 351 of the PHS Act. Therefore, the FDA is issuing the guidance to describe how it intends to address these practices.
Entities registered as outsourcing facilities are required to report adverse events to the FDA. This draft guidance explains adverse event reporting for such facilities.
The draft memorandum of understanding (MOU) under section 503A of the FD&C Act describes the responsibilities of a state that chooses to sign the MOU in investigating and responding to complaints related to compounded human drug products distributed outside the state, and in addressing the interstate distribution of “inordinate amounts” of compounded human drug products.
These documents are the latest in a series of policy documents related to FDA oversight of drugs produced by state-licensed pharmacies, federal facilities, and outsourcing facilities.
The draft guidance documents are available for public comment for 90 days. The public has 120 days to comment on the draft MOU between the states and the FDA. ![]()

Photo by Rhoda Baer
The US Food and Drug Administration (FDA) has issued 5 draft documents related to drug compounding and repackaging that aim to help entities comply with public health provisions.
The agency said these draft documents are applicable to pharmacies, federal facilities, outsourcing facilities, and physicians.
The new category of outsourcing facilities was created under the Drug Quality and Security Act (DQSA), which was enacted by Congress in November 2013.
It was enacted in response to a deadly fungal meningitis outbreak that was linked to contaminated sterile compounded drug products.
Drugs compounded in an outsourcing facility that meet certain conditions may be entitled to exemptions from certain provisions of the Federal Food, Drug, and Cosmetic Act (FD&C Act), including the new drug approval requirements and the requirement to label drug products with adequate directions for use.
Outsourcing facilities are subject to current good manufacturing practice requirements and inspections by the FDA according to a risk-based schedule.
Drugs produced by compounders that are not registered as outsourcing facilities must meet certain other conditions described in the FD&C Act, or they will be subject to all of the requirements applicable to drugs produced by conventional drug manufacturers.
“The draft guidance documents provide information to pharmacies, outsourcing facilities, healthcare entities, and others about these FDA-proposed policies, which are critical to protecting the public health,” said Janet Woodcock, MD, director of the FDA’s Center for Drug Evaluation and Research.
Descriptions of these documents follow.
This draft guidance provides an entity considering whether to register with the FDA as an outsourcing facility with information about the regulatory impact of registering.
For example, it explains that a facility engaged in only certain activities, including repackaging human drugs and compounding non-sterile drugs, should not register as an outsourcing facility because its drug products will not qualify for the exemptions provided in section 503B, including the exemption from the new drug approval requirements.
This draft guidance describes the conditions under which the FDA does not intend to take action for certain violations of the law when state-licensed pharmacies, federal facilities, or outsourcing facilities repackage certain drug products.
Repackaged drug products are generally not exempt from any of the provisions of the FD&C Act related to the production of drugs, and the compounding provisions of the FD&C Act do not address repackaging. Therefore, the FDA is issuing guidance to describe how it intends to address repackaging when done in a state-licensed pharmacy, federal facility, or outsourcing facility.
This draft guidance describes the conditions under which the FDA does not intend to take action for violations of certain sections of the Public Health Service Act (PHS Act) and the FD&C Act when state-licensed pharmacies, federal facilities, or outsourcing facilities mix, dilute, or repackage specific biological products without an approved BLA, or when such facilities or physicians prepare prescription sets of allergenic extracts without an approved BLA.
The draft guidance notes that a biological product that is mixed, diluted, or repackaged outside the scope of an approved BLA is an unlicensed biological product under section 351 of the PHS Act and may not be legally marketed without an approved BLA.
Additionally, the compounding provisions of the FD&C Act do not address biological products subject to licensure under section 351 of the PHS Act. Therefore, the FDA is issuing the guidance to describe how it intends to address these practices.
Entities registered as outsourcing facilities are required to report adverse events to the FDA. This draft guidance explains adverse event reporting for such facilities.
The draft memorandum of understanding (MOU) under section 503A of the FD&C Act describes the responsibilities of a state that chooses to sign the MOU in investigating and responding to complaints related to compounded human drug products distributed outside the state, and in addressing the interstate distribution of “inordinate amounts” of compounded human drug products.
These documents are the latest in a series of policy documents related to FDA oversight of drugs produced by state-licensed pharmacies, federal facilities, and outsourcing facilities.
The draft guidance documents are available for public comment for 90 days. The public has 120 days to comment on the draft MOU between the states and the FDA. ![]()

Photo by Rhoda Baer
The US Food and Drug Administration (FDA) has issued 5 draft documents related to drug compounding and repackaging that aim to help entities comply with public health provisions.
The agency said these draft documents are applicable to pharmacies, federal facilities, outsourcing facilities, and physicians.
The new category of outsourcing facilities was created under the Drug Quality and Security Act (DQSA), which was enacted by Congress in November 2013.
It was enacted in response to a deadly fungal meningitis outbreak that was linked to contaminated sterile compounded drug products.
Drugs compounded in an outsourcing facility that meet certain conditions may be entitled to exemptions from certain provisions of the Federal Food, Drug, and Cosmetic Act (FD&C Act), including the new drug approval requirements and the requirement to label drug products with adequate directions for use.
Outsourcing facilities are subject to current good manufacturing practice requirements and inspections by the FDA according to a risk-based schedule.
Drugs produced by compounders that are not registered as outsourcing facilities must meet certain other conditions described in the FD&C Act, or they will be subject to all of the requirements applicable to drugs produced by conventional drug manufacturers.
“The draft guidance documents provide information to pharmacies, outsourcing facilities, healthcare entities, and others about these FDA-proposed policies, which are critical to protecting the public health,” said Janet Woodcock, MD, director of the FDA’s Center for Drug Evaluation and Research.
Descriptions of these documents follow.
This draft guidance provides an entity considering whether to register with the FDA as an outsourcing facility with information about the regulatory impact of registering.
For example, it explains that a facility engaged in only certain activities, including repackaging human drugs and compounding non-sterile drugs, should not register as an outsourcing facility because its drug products will not qualify for the exemptions provided in section 503B, including the exemption from the new drug approval requirements.
This draft guidance describes the conditions under which the FDA does not intend to take action for certain violations of the law when state-licensed pharmacies, federal facilities, or outsourcing facilities repackage certain drug products.
Repackaged drug products are generally not exempt from any of the provisions of the FD&C Act related to the production of drugs, and the compounding provisions of the FD&C Act do not address repackaging. Therefore, the FDA is issuing guidance to describe how it intends to address repackaging when done in a state-licensed pharmacy, federal facility, or outsourcing facility.
This draft guidance describes the conditions under which the FDA does not intend to take action for violations of certain sections of the Public Health Service Act (PHS Act) and the FD&C Act when state-licensed pharmacies, federal facilities, or outsourcing facilities mix, dilute, or repackage specific biological products without an approved BLA, or when such facilities or physicians prepare prescription sets of allergenic extracts without an approved BLA.
The draft guidance notes that a biological product that is mixed, diluted, or repackaged outside the scope of an approved BLA is an unlicensed biological product under section 351 of the PHS Act and may not be legally marketed without an approved BLA.
Additionally, the compounding provisions of the FD&C Act do not address biological products subject to licensure under section 351 of the PHS Act. Therefore, the FDA is issuing the guidance to describe how it intends to address these practices.
Entities registered as outsourcing facilities are required to report adverse events to the FDA. This draft guidance explains adverse event reporting for such facilities.
The draft memorandum of understanding (MOU) under section 503A of the FD&C Act describes the responsibilities of a state that chooses to sign the MOU in investigating and responding to complaints related to compounded human drug products distributed outside the state, and in addressing the interstate distribution of “inordinate amounts” of compounded human drug products.
These documents are the latest in a series of policy documents related to FDA oversight of drugs produced by state-licensed pharmacies, federal facilities, and outsourcing facilities.
The draft guidance documents are available for public comment for 90 days. The public has 120 days to comment on the draft MOU between the states and the FDA. ![]()
Neural stem cells may fight chemo brain

Photo by Janet Stevens
Human neural stem cell treatments are showing promise for reversing learning and memory deficits after chemotherapy, according to an article in Cancer Research.
Investigators found that transplanting stem cells in rats a week after they completed a series of chemotherapy sessions restored a range of cognitive functions, as
measured a month later via behavioral testing.
In contrast, animals that did not receive stem cells showed significant learning and memory impairment.
“Our findings provide the first solid evidence that transplantation of human neural stem cells can be used to reverse chemotherapeutic-induced damage of healthy tissue in the brain,” said study author Charles Limoli, PhD, of the University of California, Irvine.
For this study, Dr Limoli and his colleagues transplanted adult neural stem cells into the brains of rats that had received cyclophosphamide.
The cells migrated throughout the hippocampus, where they survived and differentiated into multiple neural cell types. Additionally, these cells triggered the secretion of neurotrophic growth factors that helped rebuild wounded neurons.
The investigators also found that engrafted cells protected the host neurons, thereby preventing the loss or promoting the repair of damaged neurons and their finer structural elements, referred to as dendritic spines.
“This research suggests that stem cell therapies may one day be implemented in the clinic to provide relief to patients suffering from cognitive impairments incurred as a result of their cancer treatments,” Dr Limoli said. “While much work remains, a clinical trial analyzing the safety of such approaches may be possible within a few years.” ![]()

Photo by Janet Stevens
Human neural stem cell treatments are showing promise for reversing learning and memory deficits after chemotherapy, according to an article in Cancer Research.
Investigators found that transplanting stem cells in rats a week after they completed a series of chemotherapy sessions restored a range of cognitive functions, as
measured a month later via behavioral testing.
In contrast, animals that did not receive stem cells showed significant learning and memory impairment.
“Our findings provide the first solid evidence that transplantation of human neural stem cells can be used to reverse chemotherapeutic-induced damage of healthy tissue in the brain,” said study author Charles Limoli, PhD, of the University of California, Irvine.
For this study, Dr Limoli and his colleagues transplanted adult neural stem cells into the brains of rats that had received cyclophosphamide.
The cells migrated throughout the hippocampus, where they survived and differentiated into multiple neural cell types. Additionally, these cells triggered the secretion of neurotrophic growth factors that helped rebuild wounded neurons.
The investigators also found that engrafted cells protected the host neurons, thereby preventing the loss or promoting the repair of damaged neurons and their finer structural elements, referred to as dendritic spines.
“This research suggests that stem cell therapies may one day be implemented in the clinic to provide relief to patients suffering from cognitive impairments incurred as a result of their cancer treatments,” Dr Limoli said. “While much work remains, a clinical trial analyzing the safety of such approaches may be possible within a few years.” ![]()

Photo by Janet Stevens
Human neural stem cell treatments are showing promise for reversing learning and memory deficits after chemotherapy, according to an article in Cancer Research.
Investigators found that transplanting stem cells in rats a week after they completed a series of chemotherapy sessions restored a range of cognitive functions, as
measured a month later via behavioral testing.
In contrast, animals that did not receive stem cells showed significant learning and memory impairment.
“Our findings provide the first solid evidence that transplantation of human neural stem cells can be used to reverse chemotherapeutic-induced damage of healthy tissue in the brain,” said study author Charles Limoli, PhD, of the University of California, Irvine.
For this study, Dr Limoli and his colleagues transplanted adult neural stem cells into the brains of rats that had received cyclophosphamide.
The cells migrated throughout the hippocampus, where they survived and differentiated into multiple neural cell types. Additionally, these cells triggered the secretion of neurotrophic growth factors that helped rebuild wounded neurons.
The investigators also found that engrafted cells protected the host neurons, thereby preventing the loss or promoting the repair of damaged neurons and their finer structural elements, referred to as dendritic spines.
“This research suggests that stem cell therapies may one day be implemented in the clinic to provide relief to patients suffering from cognitive impairments incurred as a result of their cancer treatments,” Dr Limoli said. “While much work remains, a clinical trial analyzing the safety of such approaches may be possible within a few years.” ![]()
Team tracks blood formation in real time

in the bone marrow
Scientists have reported a method for equipping mouse hematopoietic stem cells (HSCs) with a fluorescent marker that can be switched on from the outside.
Using this tool, they were able to observe how HSCs mature into blood cells under normal conditions, and they developed a mathematical model of the dynamics of hematopoiesis.
The research suggests the normal process of hematopoiesis differs from what scientists previously assumed when using data from stem cell transplants.
“[A] problem with almost all research on hematopoiesis in past decades is that it has been restricted to experiments in culture or using transplantation into mice,” said study author Hans-Reimer Rodewald, PhD, of the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) in Heidelberg.
“We have now developed the first model where we can observe the development of a stem cell into a mature blood cell in a living organism.”
The researchers described this model in Nature.
The team genetically modified mice by introducing a protein into their HSCs that sends out a yellow fluorescent signal. This marker can be turned on by administering a reagent. All daughter cells that arise from a cell containing the marker also send out a light signal.
When they turned on the marker in adult mice, the researchers observed that at least a third of a mouse’s HSCs (approximately 5000 cells) produce differentiated progenitor cells.
“This was the first surprise,” said study author Katrin Busch, also of DKFZ. “Until now, scientists had believed that, in the normal state, very few stem cells—only about 10—are actively involved in blood formation.”
The researchers performed a mathematical analysis of these experimental data to provide additional insight into blood stem cell dynamics. They were surprised to find that, under normal conditions, HSCs do not replenish blood cells.
Instead, blood cells are supplied by the first progenitor cells that develop during the differentiation step. These cells are able to regenerate themselves for a long time, though not quite as long as HSCs.
To ensure that the population of this cell type never runs out, HSCs must occasionally produce a couple of new first progenitors.
During murine embryonic development, however, the situation is different. To build up the system, all mature blood and immune cells develop much more rapidly and almost completely from HSCs.
The researchers were also able to accelerate this process in adult mice by artificially depleting their white blood cells. Under these conditions, HSCs increase the formation of first progenitor cells, which then immediately start supplying new, mature blood cells.
During this process, several hundred times more myeloid cells (thrombocytes, erythrocytes, granulocytes, monocytes) form than long-lived lymphocytes (T cells, B cells, natural killer cells).
“When we transplanted our labeled blood stem cells from the bone marrow into other mice, only a few stem cells were active in the recipients, and many stem cells were lost,” Dr Rodewald noted.
“Our new data therefore show that the findings obtained up until now using transplanted stem cells can surely not be reflective of normal hematopoiesis. On the contrary, transplantation is an exception. This shows how important it is that we actually follow hematopoiesis under normal conditions in a living organism.”
The researchers now plan to use their model to investigate the impact of pathogenic challenges to blood formation; for example, in cancer, cachexia, or infection. This method would also allow them to follow potential aging processes in HSCs as they occur naturally in a living organism. ![]()

in the bone marrow
Scientists have reported a method for equipping mouse hematopoietic stem cells (HSCs) with a fluorescent marker that can be switched on from the outside.
Using this tool, they were able to observe how HSCs mature into blood cells under normal conditions, and they developed a mathematical model of the dynamics of hematopoiesis.
The research suggests the normal process of hematopoiesis differs from what scientists previously assumed when using data from stem cell transplants.
“[A] problem with almost all research on hematopoiesis in past decades is that it has been restricted to experiments in culture or using transplantation into mice,” said study author Hans-Reimer Rodewald, PhD, of the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) in Heidelberg.
“We have now developed the first model where we can observe the development of a stem cell into a mature blood cell in a living organism.”
The researchers described this model in Nature.
The team genetically modified mice by introducing a protein into their HSCs that sends out a yellow fluorescent signal. This marker can be turned on by administering a reagent. All daughter cells that arise from a cell containing the marker also send out a light signal.
When they turned on the marker in adult mice, the researchers observed that at least a third of a mouse’s HSCs (approximately 5000 cells) produce differentiated progenitor cells.
“This was the first surprise,” said study author Katrin Busch, also of DKFZ. “Until now, scientists had believed that, in the normal state, very few stem cells—only about 10—are actively involved in blood formation.”
The researchers performed a mathematical analysis of these experimental data to provide additional insight into blood stem cell dynamics. They were surprised to find that, under normal conditions, HSCs do not replenish blood cells.
Instead, blood cells are supplied by the first progenitor cells that develop during the differentiation step. These cells are able to regenerate themselves for a long time, though not quite as long as HSCs.
To ensure that the population of this cell type never runs out, HSCs must occasionally produce a couple of new first progenitors.
During murine embryonic development, however, the situation is different. To build up the system, all mature blood and immune cells develop much more rapidly and almost completely from HSCs.
The researchers were also able to accelerate this process in adult mice by artificially depleting their white blood cells. Under these conditions, HSCs increase the formation of first progenitor cells, which then immediately start supplying new, mature blood cells.
During this process, several hundred times more myeloid cells (thrombocytes, erythrocytes, granulocytes, monocytes) form than long-lived lymphocytes (T cells, B cells, natural killer cells).
“When we transplanted our labeled blood stem cells from the bone marrow into other mice, only a few stem cells were active in the recipients, and many stem cells were lost,” Dr Rodewald noted.
“Our new data therefore show that the findings obtained up until now using transplanted stem cells can surely not be reflective of normal hematopoiesis. On the contrary, transplantation is an exception. This shows how important it is that we actually follow hematopoiesis under normal conditions in a living organism.”
The researchers now plan to use their model to investigate the impact of pathogenic challenges to blood formation; for example, in cancer, cachexia, or infection. This method would also allow them to follow potential aging processes in HSCs as they occur naturally in a living organism. ![]()

in the bone marrow
Scientists have reported a method for equipping mouse hematopoietic stem cells (HSCs) with a fluorescent marker that can be switched on from the outside.
Using this tool, they were able to observe how HSCs mature into blood cells under normal conditions, and they developed a mathematical model of the dynamics of hematopoiesis.
The research suggests the normal process of hematopoiesis differs from what scientists previously assumed when using data from stem cell transplants.
“[A] problem with almost all research on hematopoiesis in past decades is that it has been restricted to experiments in culture or using transplantation into mice,” said study author Hans-Reimer Rodewald, PhD, of the German Cancer Research Center (Deutsches Krebsforschungszentrum, DKFZ) in Heidelberg.
“We have now developed the first model where we can observe the development of a stem cell into a mature blood cell in a living organism.”
The researchers described this model in Nature.
The team genetically modified mice by introducing a protein into their HSCs that sends out a yellow fluorescent signal. This marker can be turned on by administering a reagent. All daughter cells that arise from a cell containing the marker also send out a light signal.
When they turned on the marker in adult mice, the researchers observed that at least a third of a mouse’s HSCs (approximately 5000 cells) produce differentiated progenitor cells.
“This was the first surprise,” said study author Katrin Busch, also of DKFZ. “Until now, scientists had believed that, in the normal state, very few stem cells—only about 10—are actively involved in blood formation.”
The researchers performed a mathematical analysis of these experimental data to provide additional insight into blood stem cell dynamics. They were surprised to find that, under normal conditions, HSCs do not replenish blood cells.
Instead, blood cells are supplied by the first progenitor cells that develop during the differentiation step. These cells are able to regenerate themselves for a long time, though not quite as long as HSCs.
To ensure that the population of this cell type never runs out, HSCs must occasionally produce a couple of new first progenitors.
During murine embryonic development, however, the situation is different. To build up the system, all mature blood and immune cells develop much more rapidly and almost completely from HSCs.
The researchers were also able to accelerate this process in adult mice by artificially depleting their white blood cells. Under these conditions, HSCs increase the formation of first progenitor cells, which then immediately start supplying new, mature blood cells.
During this process, several hundred times more myeloid cells (thrombocytes, erythrocytes, granulocytes, monocytes) form than long-lived lymphocytes (T cells, B cells, natural killer cells).
“When we transplanted our labeled blood stem cells from the bone marrow into other mice, only a few stem cells were active in the recipients, and many stem cells were lost,” Dr Rodewald noted.
“Our new data therefore show that the findings obtained up until now using transplanted stem cells can surely not be reflective of normal hematopoiesis. On the contrary, transplantation is an exception. This shows how important it is that we actually follow hematopoiesis under normal conditions in a living organism.”
The researchers now plan to use their model to investigate the impact of pathogenic challenges to blood formation; for example, in cancer, cachexia, or infection. This method would also allow them to follow potential aging processes in HSCs as they occur naturally in a living organism. ![]()
Survey results support shared decision-making

Photo by Rhoda Baer
A survey of cancer patients has shown that when physicians make treatment decisions alone, patients tend to rate the quality of care lower than when physicians include patients in the decision-making process.
Researchers found this to be the case even among patients who said they preferred it when physicians made treatment decisions alone.
Kenneth L. Kehl, MD, of MD Anderson Cancer Center in Houston, Texas, and his colleagues reported these findings in JAMA Oncology.
The researchers surveyed 5315 cancer patients who reported decision roles for 10,817 treatment decisions. The team assessed the association between patients’ roles in decisions with their reports on quality of care and physician communication.
Most of the patients (58%) said they preferred shared roles in decision-making, 36% preferred patient-controlled decisions, and 6% preferred physician-controlled decisions.
The patients reported that their actual decision-making process was patient-controlled in 39% of decisions, shared in 44%, and physician-controlled in 17%. Of the treatment decisions made by patients, 42% were regarding surgery, 36% were regarding chemotherapy, and 22% were regarding radiation.
The researchers found that patients’ preferred role in decision-making was not associated with how they rated the quality of care. But when they reported that treatment decisions were controlled by physicians, the patients were less likely to rate the quality of care as excellent, as compared to shared-decision making situations.
Patients said physician care was excellent in 67.8% of cases. And 55.8% of patients gave their physicians the highest possible rating of communication.
However, patients who preferred physician-controlled decisions to shared decision-making were less likely to give top ratings to their physicians, as were patients who reported actually experiencing physician-controlled vs shared decisions.
The researchers said these results highlight the benefits of promoting shared decision-making among all patients with cancer, even those who seem to prefer less active roles in the process.
In a related commentary, Sarah T. Hawley, PhD, and Reshma Jagsi, MD, DPhil, of the University of Michigan in Ann Arbor, said they were intrigued by the fact that the association between shared decision-making and patient appraisal of care quality remained even when controlling for a patient’s preferred role in the decision-making process.
“Kehl and colleagues conclude from this finding that it is important to promote [shared decision-making], even among patients who may seek less active roles,” Drs Hawley and Jagsi wrote.
“Yet . . . prior work . . . has suggested that it is the match between patients’ preferred and actual involvement that contributes to greater satisfaction with care. These conflicting results underscore the need for further work to better quantify and link measures of [shared decision-making] to patient appraisal of care.” ![]()

Photo by Rhoda Baer
A survey of cancer patients has shown that when physicians make treatment decisions alone, patients tend to rate the quality of care lower than when physicians include patients in the decision-making process.
Researchers found this to be the case even among patients who said they preferred it when physicians made treatment decisions alone.
Kenneth L. Kehl, MD, of MD Anderson Cancer Center in Houston, Texas, and his colleagues reported these findings in JAMA Oncology.
The researchers surveyed 5315 cancer patients who reported decision roles for 10,817 treatment decisions. The team assessed the association between patients’ roles in decisions with their reports on quality of care and physician communication.
Most of the patients (58%) said they preferred shared roles in decision-making, 36% preferred patient-controlled decisions, and 6% preferred physician-controlled decisions.
The patients reported that their actual decision-making process was patient-controlled in 39% of decisions, shared in 44%, and physician-controlled in 17%. Of the treatment decisions made by patients, 42% were regarding surgery, 36% were regarding chemotherapy, and 22% were regarding radiation.
The researchers found that patients’ preferred role in decision-making was not associated with how they rated the quality of care. But when they reported that treatment decisions were controlled by physicians, the patients were less likely to rate the quality of care as excellent, as compared to shared-decision making situations.
Patients said physician care was excellent in 67.8% of cases. And 55.8% of patients gave their physicians the highest possible rating of communication.
However, patients who preferred physician-controlled decisions to shared decision-making were less likely to give top ratings to their physicians, as were patients who reported actually experiencing physician-controlled vs shared decisions.
The researchers said these results highlight the benefits of promoting shared decision-making among all patients with cancer, even those who seem to prefer less active roles in the process.
In a related commentary, Sarah T. Hawley, PhD, and Reshma Jagsi, MD, DPhil, of the University of Michigan in Ann Arbor, said they were intrigued by the fact that the association between shared decision-making and patient appraisal of care quality remained even when controlling for a patient’s preferred role in the decision-making process.
“Kehl and colleagues conclude from this finding that it is important to promote [shared decision-making], even among patients who may seek less active roles,” Drs Hawley and Jagsi wrote.
“Yet . . . prior work . . . has suggested that it is the match between patients’ preferred and actual involvement that contributes to greater satisfaction with care. These conflicting results underscore the need for further work to better quantify and link measures of [shared decision-making] to patient appraisal of care.” ![]()

Photo by Rhoda Baer
A survey of cancer patients has shown that when physicians make treatment decisions alone, patients tend to rate the quality of care lower than when physicians include patients in the decision-making process.
Researchers found this to be the case even among patients who said they preferred it when physicians made treatment decisions alone.
Kenneth L. Kehl, MD, of MD Anderson Cancer Center in Houston, Texas, and his colleagues reported these findings in JAMA Oncology.
The researchers surveyed 5315 cancer patients who reported decision roles for 10,817 treatment decisions. The team assessed the association between patients’ roles in decisions with their reports on quality of care and physician communication.
Most of the patients (58%) said they preferred shared roles in decision-making, 36% preferred patient-controlled decisions, and 6% preferred physician-controlled decisions.
The patients reported that their actual decision-making process was patient-controlled in 39% of decisions, shared in 44%, and physician-controlled in 17%. Of the treatment decisions made by patients, 42% were regarding surgery, 36% were regarding chemotherapy, and 22% were regarding radiation.
The researchers found that patients’ preferred role in decision-making was not associated with how they rated the quality of care. But when they reported that treatment decisions were controlled by physicians, the patients were less likely to rate the quality of care as excellent, as compared to shared-decision making situations.
Patients said physician care was excellent in 67.8% of cases. And 55.8% of patients gave their physicians the highest possible rating of communication.
However, patients who preferred physician-controlled decisions to shared decision-making were less likely to give top ratings to their physicians, as were patients who reported actually experiencing physician-controlled vs shared decisions.
The researchers said these results highlight the benefits of promoting shared decision-making among all patients with cancer, even those who seem to prefer less active roles in the process.
In a related commentary, Sarah T. Hawley, PhD, and Reshma Jagsi, MD, DPhil, of the University of Michigan in Ann Arbor, said they were intrigued by the fact that the association between shared decision-making and patient appraisal of care quality remained even when controlling for a patient’s preferred role in the decision-making process.
“Kehl and colleagues conclude from this finding that it is important to promote [shared decision-making], even among patients who may seek less active roles,” Drs Hawley and Jagsi wrote.
“Yet . . . prior work . . . has suggested that it is the match between patients’ preferred and actual involvement that contributes to greater satisfaction with care. These conflicting results underscore the need for further work to better quantify and link measures of [shared decision-making] to patient appraisal of care.”
Cancer patients rarely make inappropriate requests, study shows

Photo courtesy of NIH
Although it makes sense that patient requests might drive physicians to practice defensive medicine, new research suggests that may not be the case with cancer patients.
The study, conducted at outpatient oncology centers, showed that patients rarely made clinically inappropriate requests.
Only 1% of more than 5000 patient-clinician encounters resulted in a clinically inappropriate request. And physicians rarely complied with these requests.
Keerthi Gogineni, MD, of the Hospital of the University of Pennsylvania in Philadelphia, and colleagues reported these findings in JAMA Oncology.
The researchers analyzed interviews with clinicians immediately after they visited with patients to assess whether a patient had made a request, the type of request made, and the clinical appropriateness of it.
The interviews were conducted at outpatient oncology facilities at 3 Philadelphia-area hospitals between October 2013 and June 2014.
The authors evaluated 5050 patient-clinician encounters involving 3624 patients and 60 clinicians. Most of the patients were women, and the most common cancer was hematologic.
Overall, 440 (8.7%) of the encounters included a patient demand or request, such as for imaging studies, treatments, or tests. And physicians complied with 365 (83%) of them.
Of all the patient-clinician encounters, 50 (1%) included a clinically inappropriate request. Clinicians complied with 7 of them. So, in 0.14% of encounters, clinicians ordered a test or treatment based on a clinically inappropriate request.
“At least in oncology, ‘demanding patients’ seem infrequent and may not account for a significant proportion of costs,” the researchers concluded.
In a related editorial, Anthony L. Back, MD, of the Seattle Cancer Care Alliance in Washington, wrote that inappropriate patient demands appear to be “more mythical than real.”
“[W]e have to stop blaming patients for being demanding,” he wrote. “In reality, it is hardly happening. The myth of the demanding patient is more about our own responses and how lackluster communication skills can contribute to difficult situations that stick in our throats and in our memories. And when we have calmed down enough to look up, we see that what is really happening between patients and physicians these days is something quite different.”
“It is possible that what the study by Gogineni et al documents is a point in the evolution of the patient-physician relationship when both sides recognize the complexity of cancer care belies a simple fix. Perhaps this ‘negative’ study is pointing to an important truth: that we need to redirect our attention from the myths that are distracting us.”

Photo courtesy of NIH
Although it makes sense that patient requests might drive physicians to practice defensive medicine, new research suggests that may not be the case with cancer patients.
The study, conducted at outpatient oncology centers, showed that patients rarely made clinically inappropriate requests.
Only 1% of more than 5000 patient-clinician encounters resulted in a clinically inappropriate request. And physicians rarely complied with these requests.
Keerthi Gogineni, MD, of the Hospital of the University of Pennsylvania in Philadelphia, and colleagues reported these findings in JAMA Oncology.
The researchers analyzed interviews with clinicians immediately after they visited with patients to assess whether a patient had made a request, the type of request made, and the clinical appropriateness of it.
The interviews were conducted at outpatient oncology facilities at 3 Philadelphia-area hospitals between October 2013 and June 2014.
The authors evaluated 5050 patient-clinician encounters involving 3624 patients and 60 clinicians. Most of the patients were women, and the most common cancer was hematologic.
Overall, 440 (8.7%) of the encounters included a patient demand or request, such as for imaging studies, treatments, or tests. And physicians complied with 365 (83%) of them.
Of all the patient-clinician encounters, 50 (1%) included a clinically inappropriate request. Clinicians complied with 7 of them. So, in 0.14% of encounters, clinicians ordered a test or treatment based on a clinically inappropriate request.
“At least in oncology, ‘demanding patients’ seem infrequent and may not account for a significant proportion of costs,” the researchers concluded.
In a related editorial, Anthony L. Back, MD, of the Seattle Cancer Care Alliance in Washington, wrote that inappropriate patient demands appear to be “more mythical than real.”
“[W]e have to stop blaming patients for being demanding,” he wrote. “In reality, it is hardly happening. The myth of the demanding patient is more about our own responses and how lackluster communication skills can contribute to difficult situations that stick in our throats and in our memories. And when we have calmed down enough to look up, we see that what is really happening between patients and physicians these days is something quite different.”
“It is possible that what the study by Gogineni et al documents is a point in the evolution of the patient-physician relationship when both sides recognize the complexity of cancer care belies a simple fix. Perhaps this ‘negative’ study is pointing to an important truth: that we need to redirect our attention from the myths that are distracting us.”

Photo courtesy of NIH
Although it makes sense that patient requests might drive physicians to practice defensive medicine, new research suggests that may not be the case with cancer patients.
The study, conducted at outpatient oncology centers, showed that patients rarely made clinically inappropriate requests.
Only 1% of more than 5000 patient-clinician encounters resulted in a clinically inappropriate request. And physicians rarely complied with these requests.
Keerthi Gogineni, MD, of the Hospital of the University of Pennsylvania in Philadelphia, and colleagues reported these findings in JAMA Oncology.
The researchers analyzed interviews with clinicians immediately after they visited with patients to assess whether a patient had made a request, the type of request made, and the clinical appropriateness of it.
The interviews were conducted at outpatient oncology facilities at 3 Philadelphia-area hospitals between October 2013 and June 2014.
The authors evaluated 5050 patient-clinician encounters involving 3624 patients and 60 clinicians. Most of the patients were women, and the most common cancer was hematologic.
Overall, 440 (8.7%) of the encounters included a patient demand or request, such as for imaging studies, treatments, or tests. And physicians complied with 365 (83%) of them.
Of all the patient-clinician encounters, 50 (1%) included a clinically inappropriate request. Clinicians complied with 7 of them. So, in 0.14% of encounters, clinicians ordered a test or treatment based on a clinically inappropriate request.
“At least in oncology, ‘demanding patients’ seem infrequent and may not account for a significant proportion of costs,” the researchers concluded.
In a related editorial, Anthony L. Back, MD, of the Seattle Cancer Care Alliance in Washington, wrote that inappropriate patient demands appear to be “more mythical than real.”
“[W]e have to stop blaming patients for being demanding,” he wrote. “In reality, it is hardly happening. The myth of the demanding patient is more about our own responses and how lackluster communication skills can contribute to difficult situations that stick in our throats and in our memories. And when we have calmed down enough to look up, we see that what is really happening between patients and physicians these days is something quite different.”
“It is possible that what the study by Gogineni et al documents is a point in the evolution of the patient-physician relationship when both sides recognize the complexity of cancer care belies a simple fix. Perhaps this ‘negative’ study is pointing to an important truth: that we need to redirect our attention from the myths that are distracting us.”
Signs may predict death in cancer patients

Researchers have identified 8 highly specific physical and cognitive signs that seem to be associated with imminent death in cancer patients.
The findings, published in Cancer, could offer clinicians the ability to better communicate with patients and their families.
The research might also help guide the medical team and caregivers when it comes to complex decision making, such as discontinuing tests and therapy, plans for hospital discharge, and hospice referral.
Previous studies in end-of-life care have focused on physicians prognosticating better. However, research on how to tell if a patient has entered the final days of life has been minimal, according to David Hui, MD, of the University of Texas MD Anderson Cancer Center in Houston.
“In the past, studies trying to understand the signs associated with impending death were conducted in people who were recognized as dying, so there’s a potential bias built into this model,” Dr Hui said.
“With our study, we observed a list of signs in patients from the time they were admitted to the palliative care unit. They were observed systematically, twice a day, without knowing if the patient would die or be discharged.”
Dr Hui and his colleagues observed 357 cancer patients, 57% of whom ultimately died. The researchers observed 52 physical and cognitive signs—identified by Dr Hui and his colleagues in previous research—twice a day from the patient’s admission to discharge or death.
Of those 52 signs, the 8 most highly associated with impending death within 3 days were:
- Nonreactive pupils
- Decreased response to verbal stimuli
- Decreased response to visual stimuli
- Inability to close eyelids
- Drooping of the nasolabial fold
- Neck hyperextension
- Grunting of vocal cords
- Upper gastrointestinal bleeding.
“When cancer patients reach the last days of life, this is an extremely emotional time for families; their stress levels cannot be understated,” Dr Hui said.
“Knowing when death is imminent would provide more information so caregivers can plan appropriately. For clinicians, having this information could help reassure families that we are providing the best care possible.”
Dr Hui stressed that this research is not yet practice-changing, but is an important step in understanding these 8 signs and their relation to impending death. In addition, the findings are only representative of imminent cancer death and should not be generalized to other causes of death.
Follow-up studies in different settings are planned. Dr Hui and his colleagues plan to look at the reliability of the identified signs, as well as evaluate this research in other countries and in the hospice setting.

Researchers have identified 8 highly specific physical and cognitive signs that seem to be associated with imminent death in cancer patients.
The findings, published in Cancer, could offer clinicians the ability to better communicate with patients and their families.
The research might also help guide the medical team and caregivers when it comes to complex decision making, such as discontinuing tests and therapy, plans for hospital discharge, and hospice referral.
Previous studies in end-of-life care have focused on physicians prognosticating better. However, research on how to tell if a patient has entered the final days of life has been minimal, according to David Hui, MD, of the University of Texas MD Anderson Cancer Center in Houston.
“In the past, studies trying to understand the signs associated with impending death were conducted in people who were recognized as dying, so there’s a potential bias built into this model,” Dr Hui said.
“With our study, we observed a list of signs in patients from the time they were admitted to the palliative care unit. They were observed systematically, twice a day, without knowing if the patient would die or be discharged.”
Dr Hui and his colleagues observed 357 cancer patients, 57% of whom ultimately died. The researchers observed 52 physical and cognitive signs—identified by Dr Hui and his colleagues in previous research—twice a day from the patient’s admission to discharge or death.
Of those 52 signs, the 8 most highly associated with impending death within 3 days were:
- Nonreactive pupils
- Decreased response to verbal stimuli
- Decreased response to visual stimuli
- Inability to close eyelids
- Drooping of the nasolabial fold
- Neck hyperextension
- Grunting of vocal cords
- Upper gastrointestinal bleeding.
“When cancer patients reach the last days of life, this is an extremely emotional time for families; their stress levels cannot be understated,” Dr Hui said.
“Knowing when death is imminent would provide more information so caregivers can plan appropriately. For clinicians, having this information could help reassure families that we are providing the best care possible.”
Dr Hui stressed that this research is not yet practice-changing, but is an important step in understanding these 8 signs and their relation to impending death. In addition, the findings are only representative of imminent cancer death and should not be generalized to other causes of death.
Follow-up studies in different settings are planned. Dr Hui and his colleagues plan to look at the reliability of the identified signs, as well as evaluate this research in other countries and in the hospice setting.

Researchers have identified 8 highly specific physical and cognitive signs that seem to be associated with imminent death in cancer patients.
The findings, published in Cancer, could offer clinicians the ability to better communicate with patients and their families.
The research might also help guide the medical team and caregivers when it comes to complex decision making, such as discontinuing tests and therapy, plans for hospital discharge, and hospice referral.
Previous studies in end-of-life care have focused on physicians prognosticating better. However, research on how to tell if a patient has entered the final days of life has been minimal, according to David Hui, MD, of the University of Texas MD Anderson Cancer Center in Houston.
“In the past, studies trying to understand the signs associated with impending death were conducted in people who were recognized as dying, so there’s a potential bias built into this model,” Dr Hui said.
“With our study, we observed a list of signs in patients from the time they were admitted to the palliative care unit. They were observed systematically, twice a day, without knowing if the patient would die or be discharged.”
Dr Hui and his colleagues observed 357 cancer patients, 57% of whom ultimately died. The researchers observed 52 physical and cognitive signs—identified by Dr Hui and his colleagues in previous research—twice a day from the patient’s admission to discharge or death.
Of those 52 signs, the 8 most highly associated with impending death within 3 days were:
- Nonreactive pupils
- Decreased response to verbal stimuli
- Decreased response to visual stimuli
- Inability to close eyelids
- Drooping of the nasolabial fold
- Neck hyperextension
- Grunting of vocal cords
- Upper gastrointestinal bleeding.
“When cancer patients reach the last days of life, this is an extremely emotional time for families; their stress levels cannot be understated,” Dr Hui said.
“Knowing when death is imminent would provide more information so caregivers can plan appropriately. For clinicians, having this information could help reassure families that we are providing the best care possible.”
Dr Hui stressed that this research is not yet practice-changing, but is an important step in understanding these 8 signs and their relation to impending death. In addition, the findings are only representative of imminent cancer death and should not be generalized to other causes of death.
Follow-up studies in different settings are planned. Dr Hui and his colleagues plan to look at the reliability of the identified signs, as well as evaluate this research in other countries and in the hospice setting.
FDA inspection findings rarely reported in literature

Photo by Esther Dyson
A new study suggests that, when the US Food and Drug Administration (FDA) identifies problems at clinical trial sites, those findings are seldom reported in peer-reviewed articles later written about the research.
Only 4% of the articles analyzed in this study disclosed that an FDA inspection revealed significant problems at a trial site.
Charles Seife, of the Carter Institute of Journalism at New York University in New York, New York, reported this finding in JAMA Internal Medicine.
Seife noted that the FDA classifies its inspections based on the severity of the violations, and the most severe is “official action indicated (OAI),” which means objectionable conditions or practices that warrant regulatory action.
During the 2013 fiscal year, about 2% of the 644 inspections the FDA conducted at trial sites were classified as OAI.
With this in mind, Seife and his students set out to identify published trials in which an FDA inspection revealed significant problems and determine whether there was mention of it in the medical literature.
The group identified 57 trials in which an FDA inspection uncovered the following problems:
- Falsification or submission of false information (22 trials, 39%)
- Problems with adverse events reporting (14 trials, 25%)
- Protocol violations (42 trials, 74%)
- Inadequate or inaccurate recordkeeping (35 trials, 61%)
- Failure to protect the safety of patients and/or issues with oversight or informed consent (30 trials, 53%)
- Violations that were not otherwise characterized (20 trials, 35%).
Only 3 of the 78 publications (4%) that resulted from these trials mentioned the objectionable conditions or practices.
“The FDA does not typically notify journals when a site participating in a published clinical trial receives an OAI inspection, nor does it generally make any announcement intended to alert the public about the research misconduct that it finds,” Seife wrote.
“The documents the agency discloses tend to be heavily redacted. As a result, it is usually very difficult, or even impossible, to determine which published clinical trials are implicated by the FDA’s allegations of research misconduct.”
In a related editorial, Robert Steinbrook, MD, of the Yale School of Medicine in New Haven, Connecticut, and Rita F. Redberg, MD, of the University of California, San Francisco, wrote that Seife’s study highlights an important area for improved reporting of clinical trials and enhanced transparency at the FDA.
“A central responsibility of medical journals is maintaining and improving trust in the medical literature,” they wrote. “Journals should expect that investigators and sponsors of clinical trials would promptly notify them of substantial findings from FDA and other regulatory agency inspections and modify their reports of clinical trials as needed, either before or after publication.”

Photo by Esther Dyson
A new study suggests that, when the US Food and Drug Administration (FDA) identifies problems at clinical trial sites, those findings are seldom reported in peer-reviewed articles later written about the research.
Only 4% of the articles analyzed in this study disclosed that an FDA inspection revealed significant problems at a trial site.
Charles Seife, of the Carter Institute of Journalism at New York University in New York, New York, reported this finding in JAMA Internal Medicine.
Seife noted that the FDA classifies its inspections based on the severity of the violations, and the most severe is “official action indicated (OAI),” which means objectionable conditions or practices that warrant regulatory action.
During the 2013 fiscal year, about 2% of the 644 inspections the FDA conducted at trial sites were classified as OAI.
With this in mind, Seife and his students set out to identify published trials in which an FDA inspection revealed significant problems and determine whether there was mention of it in the medical literature.
The group identified 57 trials in which an FDA inspection uncovered the following problems:
- Falsification or submission of false information (22 trials, 39%)
- Problems with adverse events reporting (14 trials, 25%)
- Protocol violations (42 trials, 74%)
- Inadequate or inaccurate recordkeeping (35 trials, 61%)
- Failure to protect the safety of patients and/or issues with oversight or informed consent (30 trials, 53%)
- Violations that were not otherwise characterized (20 trials, 35%).
Only 3 of the 78 publications (4%) that resulted from these trials mentioned the objectionable conditions or practices.
“The FDA does not typically notify journals when a site participating in a published clinical trial receives an OAI inspection, nor does it generally make any announcement intended to alert the public about the research misconduct that it finds,” Seife wrote.
“The documents the agency discloses tend to be heavily redacted. As a result, it is usually very difficult, or even impossible, to determine which published clinical trials are implicated by the FDA’s allegations of research misconduct.”
In a related editorial, Robert Steinbrook, MD, of the Yale School of Medicine in New Haven, Connecticut, and Rita F. Redberg, MD, of the University of California, San Francisco, wrote that Seife’s study highlights an important area for improved reporting of clinical trials and enhanced transparency at the FDA.
“A central responsibility of medical journals is maintaining and improving trust in the medical literature,” they wrote. “Journals should expect that investigators and sponsors of clinical trials would promptly notify them of substantial findings from FDA and other regulatory agency inspections and modify their reports of clinical trials as needed, either before or after publication.”

Photo by Esther Dyson
A new study suggests that, when the US Food and Drug Administration (FDA) identifies problems at clinical trial sites, those findings are seldom reported in peer-reviewed articles later written about the research.
Only 4% of the articles analyzed in this study disclosed that an FDA inspection revealed significant problems at a trial site.
Charles Seife, of the Carter Institute of Journalism at New York University in New York, New York, reported this finding in JAMA Internal Medicine.
Seife noted that the FDA classifies its inspections based on the severity of the violations, and the most severe is “official action indicated (OAI),” which means objectionable conditions or practices that warrant regulatory action.
During the 2013 fiscal year, about 2% of the 644 inspections the FDA conducted at trial sites were classified as OAI.
With this in mind, Seife and his students set out to identify published trials in which an FDA inspection revealed significant problems and determine whether there was mention of it in the medical literature.
The group identified 57 trials in which an FDA inspection uncovered the following problems:
- Falsification or submission of false information (22 trials, 39%)
- Problems with adverse events reporting (14 trials, 25%)
- Protocol violations (42 trials, 74%)
- Inadequate or inaccurate recordkeeping (35 trials, 61%)
- Failure to protect the safety of patients and/or issues with oversight or informed consent (30 trials, 53%)
- Violations that were not otherwise characterized (20 trials, 35%).
Only 3 of the 78 publications (4%) that resulted from these trials mentioned the objectionable conditions or practices.
“The FDA does not typically notify journals when a site participating in a published clinical trial receives an OAI inspection, nor does it generally make any announcement intended to alert the public about the research misconduct that it finds,” Seife wrote.
“The documents the agency discloses tend to be heavily redacted. As a result, it is usually very difficult, or even impossible, to determine which published clinical trials are implicated by the FDA’s allegations of research misconduct.”
In a related editorial, Robert Steinbrook, MD, of the Yale School of Medicine in New Haven, Connecticut, and Rita F. Redberg, MD, of the University of California, San Francisco, wrote that Seife’s study highlights an important area for improved reporting of clinical trials and enhanced transparency at the FDA.
“A central responsibility of medical journals is maintaining and improving trust in the medical literature,” they wrote. “Journals should expect that investigators and sponsors of clinical trials would promptly notify them of substantial findings from FDA and other regulatory agency inspections and modify their reports of clinical trials as needed, either before or after publication.”