User login
Group creates detailed map of proteins in human body
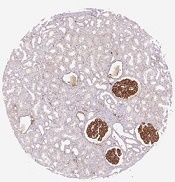
in the renal glomeruli,
the network responsible
for filtering the blood
Credit: Human Protein Atlas
Scientists say they’ve completed the first major analysis based on the Human Protein Atlas, providing a detailed picture of proteins linked to cancer, the number of proteins present in the bloodstream, and all proteins targeted by drugs.
The group described their work in Science.
The Human Protein Atlas, a multinational research project, recently launched an open-source, tissue-based, interactive map of the human proteome.
In the Science article, researchers described how they studied the human proteome. The group analyzed samples representing the 44 major tissues and organs in the human body.
They used 24,028 antibodies, corresponding to 16,975 protein-encoding genes, to produce more than 13 million tissue-based immunohistochemistry images. They complemented this analysis with RNA-sequencing data for 32 of the 44 tissue types.
In this way, the scientists mapped the distribution of proteins in all major tissues and organs in the human body. They identified proteins restricted to certain tissues—such as the brain, heart, or liver—and those present throughout the body.
Almost half of the nearly 17,000 protein-encoding genes are expressed in all the tissues the researchers analyzed. The group also found that 3171 proteins are secreted from cells, and 5570 are located in the membrane systems of cells.
“This is important information for the pharmaceutical industry,” said study author Mathias Uhlén, PhD, a professor at the KTH Royal Institute of Technology in Stockholm, Sweden, and the director of the Human Protein Atlas program.
“We show that 70% of the current targets for approved pharmaceutical drugs are either secreted or membrane-bound proteins. Interestingly, 30% of these protein targets are found in all analyzed tissues and organs. This could help explain some side effects of drugs and, thus, might have consequences for future drug development.” ![]()

in the renal glomeruli,
the network responsible
for filtering the blood
Credit: Human Protein Atlas
Scientists say they’ve completed the first major analysis based on the Human Protein Atlas, providing a detailed picture of proteins linked to cancer, the number of proteins present in the bloodstream, and all proteins targeted by drugs.
The group described their work in Science.
The Human Protein Atlas, a multinational research project, recently launched an open-source, tissue-based, interactive map of the human proteome.
In the Science article, researchers described how they studied the human proteome. The group analyzed samples representing the 44 major tissues and organs in the human body.
They used 24,028 antibodies, corresponding to 16,975 protein-encoding genes, to produce more than 13 million tissue-based immunohistochemistry images. They complemented this analysis with RNA-sequencing data for 32 of the 44 tissue types.
In this way, the scientists mapped the distribution of proteins in all major tissues and organs in the human body. They identified proteins restricted to certain tissues—such as the brain, heart, or liver—and those present throughout the body.
Almost half of the nearly 17,000 protein-encoding genes are expressed in all the tissues the researchers analyzed. The group also found that 3171 proteins are secreted from cells, and 5570 are located in the membrane systems of cells.
“This is important information for the pharmaceutical industry,” said study author Mathias Uhlén, PhD, a professor at the KTH Royal Institute of Technology in Stockholm, Sweden, and the director of the Human Protein Atlas program.
“We show that 70% of the current targets for approved pharmaceutical drugs are either secreted or membrane-bound proteins. Interestingly, 30% of these protein targets are found in all analyzed tissues and organs. This could help explain some side effects of drugs and, thus, might have consequences for future drug development.” ![]()

in the renal glomeruli,
the network responsible
for filtering the blood
Credit: Human Protein Atlas
Scientists say they’ve completed the first major analysis based on the Human Protein Atlas, providing a detailed picture of proteins linked to cancer, the number of proteins present in the bloodstream, and all proteins targeted by drugs.
The group described their work in Science.
The Human Protein Atlas, a multinational research project, recently launched an open-source, tissue-based, interactive map of the human proteome.
In the Science article, researchers described how they studied the human proteome. The group analyzed samples representing the 44 major tissues and organs in the human body.
They used 24,028 antibodies, corresponding to 16,975 protein-encoding genes, to produce more than 13 million tissue-based immunohistochemistry images. They complemented this analysis with RNA-sequencing data for 32 of the 44 tissue types.
In this way, the scientists mapped the distribution of proteins in all major tissues and organs in the human body. They identified proteins restricted to certain tissues—such as the brain, heart, or liver—and those present throughout the body.
Almost half of the nearly 17,000 protein-encoding genes are expressed in all the tissues the researchers analyzed. The group also found that 3171 proteins are secreted from cells, and 5570 are located in the membrane systems of cells.
“This is important information for the pharmaceutical industry,” said study author Mathias Uhlén, PhD, a professor at the KTH Royal Institute of Technology in Stockholm, Sweden, and the director of the Human Protein Atlas program.
“We show that 70% of the current targets for approved pharmaceutical drugs are either secreted or membrane-bound proteins. Interestingly, 30% of these protein targets are found in all analyzed tissues and organs. This could help explain some side effects of drugs and, thus, might have consequences for future drug development.” ![]()
CO2 tells malaria-carrying mosquitoes when to land

working on an experiment
involving a wind tunnel
Credit: Carrie Rosema
House-dwelling, malaria-carrying mosquitoes can detect minute changes in concentrations of exhaled carbon dioxide to determine when humans are present, according to research published in the Journal of Chemical Ecology.
Anopheles gambiae mosquitoes spend much of their adult lives indoors, where they are constantly exposed to human odor, even when people are absent.
But researchers found these mosquitoes respond very weakly to human skin odor alone.
Experiments showed that mosquitoes were more likely to a land on a source of skin odor if carbon dioxide was also present, even at very low levels.
“Responding strongly to human skin odor alone once inside a dwelling where human odor is ubiquitous is a highly inefficient means for the mosquito of locating a feeding site,” said study author Ring Cardé, PhD, of the University of California, Riverside.
“We already know that mosquitoes will readily fly upwind towards human skin odor, but landing, the final stage of host location, which typically takes place indoors, does not occur unless a fluctuating concentration of carbon dioxide indicates that a human host is present.”
Dr Cardé and his colleagues discovered the importance of carbon dioxide in mosquitoes’ landing patterns by studying Anopheles gambiae mosquitoes collected in Cameroon.
The researchers collected skin odor by using pieces of white polyester gauze worn by one of the study authors in a cotton sock for 4 to 6 hours before the experiments began. The team then recorded the mosquitoes’ landing behavior with a video camera equipped with night vision.
The landing behavior “dramatically increased” with the addition of carbon dioxide at a range of concentrations above ambient. This was true even when the carbon dioxide level was just 0.015% above ambient within the assay cage.
These results suggest the mosquitoes use a “sit-and-wait” ambush strategy during which they ignore persistent human odor until a living human is present.
One take-home message from this work is that researchers investigating which human odors mediate host-finding and which compounds are good mosquito repellents need to precisely control exposure to carbon dioxide. A researcher entering an assay room quickly elevates the level of carbon dioxide, thereby altering the mosquitoes’ behavior.
“It also would be useful next to see if mosquitoes’ response to skin odor is similarly affected by carbon dioxide in outdoor situations and how these interactions play out in human dwellings,” Dr Cardé noted. ![]()

working on an experiment
involving a wind tunnel
Credit: Carrie Rosema
House-dwelling, malaria-carrying mosquitoes can detect minute changes in concentrations of exhaled carbon dioxide to determine when humans are present, according to research published in the Journal of Chemical Ecology.
Anopheles gambiae mosquitoes spend much of their adult lives indoors, where they are constantly exposed to human odor, even when people are absent.
But researchers found these mosquitoes respond very weakly to human skin odor alone.
Experiments showed that mosquitoes were more likely to a land on a source of skin odor if carbon dioxide was also present, even at very low levels.
“Responding strongly to human skin odor alone once inside a dwelling where human odor is ubiquitous is a highly inefficient means for the mosquito of locating a feeding site,” said study author Ring Cardé, PhD, of the University of California, Riverside.
“We already know that mosquitoes will readily fly upwind towards human skin odor, but landing, the final stage of host location, which typically takes place indoors, does not occur unless a fluctuating concentration of carbon dioxide indicates that a human host is present.”
Dr Cardé and his colleagues discovered the importance of carbon dioxide in mosquitoes’ landing patterns by studying Anopheles gambiae mosquitoes collected in Cameroon.
The researchers collected skin odor by using pieces of white polyester gauze worn by one of the study authors in a cotton sock for 4 to 6 hours before the experiments began. The team then recorded the mosquitoes’ landing behavior with a video camera equipped with night vision.
The landing behavior “dramatically increased” with the addition of carbon dioxide at a range of concentrations above ambient. This was true even when the carbon dioxide level was just 0.015% above ambient within the assay cage.
These results suggest the mosquitoes use a “sit-and-wait” ambush strategy during which they ignore persistent human odor until a living human is present.
One take-home message from this work is that researchers investigating which human odors mediate host-finding and which compounds are good mosquito repellents need to precisely control exposure to carbon dioxide. A researcher entering an assay room quickly elevates the level of carbon dioxide, thereby altering the mosquitoes’ behavior.
“It also would be useful next to see if mosquitoes’ response to skin odor is similarly affected by carbon dioxide in outdoor situations and how these interactions play out in human dwellings,” Dr Cardé noted. ![]()

working on an experiment
involving a wind tunnel
Credit: Carrie Rosema
House-dwelling, malaria-carrying mosquitoes can detect minute changes in concentrations of exhaled carbon dioxide to determine when humans are present, according to research published in the Journal of Chemical Ecology.
Anopheles gambiae mosquitoes spend much of their adult lives indoors, where they are constantly exposed to human odor, even when people are absent.
But researchers found these mosquitoes respond very weakly to human skin odor alone.
Experiments showed that mosquitoes were more likely to a land on a source of skin odor if carbon dioxide was also present, even at very low levels.
“Responding strongly to human skin odor alone once inside a dwelling where human odor is ubiquitous is a highly inefficient means for the mosquito of locating a feeding site,” said study author Ring Cardé, PhD, of the University of California, Riverside.
“We already know that mosquitoes will readily fly upwind towards human skin odor, but landing, the final stage of host location, which typically takes place indoors, does not occur unless a fluctuating concentration of carbon dioxide indicates that a human host is present.”
Dr Cardé and his colleagues discovered the importance of carbon dioxide in mosquitoes’ landing patterns by studying Anopheles gambiae mosquitoes collected in Cameroon.
The researchers collected skin odor by using pieces of white polyester gauze worn by one of the study authors in a cotton sock for 4 to 6 hours before the experiments began. The team then recorded the mosquitoes’ landing behavior with a video camera equipped with night vision.
The landing behavior “dramatically increased” with the addition of carbon dioxide at a range of concentrations above ambient. This was true even when the carbon dioxide level was just 0.015% above ambient within the assay cage.
These results suggest the mosquitoes use a “sit-and-wait” ambush strategy during which they ignore persistent human odor until a living human is present.
One take-home message from this work is that researchers investigating which human odors mediate host-finding and which compounds are good mosquito repellents need to precisely control exposure to carbon dioxide. A researcher entering an assay room quickly elevates the level of carbon dioxide, thereby altering the mosquitoes’ behavior.
“It also would be useful next to see if mosquitoes’ response to skin odor is similarly affected by carbon dioxide in outdoor situations and how these interactions play out in human dwellings,” Dr Cardé noted. ![]()
Theorem helps pinpoint start of patient recovery

Credit: CDC
The 2500-year-old Pythagorean theorem could be the most effective way to identify the point at which a patient’s health begins to improve, a new study suggests.
Researchers made the discovery while examining receiver operating characteristic (ROC) curves, which are used to measure changes in a patient’s health status.
“It all comes down to choosing a point on a curve to determine when recovery has occurred,” said study author Rob Froud, PhD, of the University of Warwick in Coventry, UK.
“For many chronic conditions, epidemiologists agree that the correct point to choose is that which is closest to the top-left corner of the plot containing the curve. As we stopped to think about it, it struck us as obvious that the way to choose this point was by using Pythagoras’s theorem.”
The theorem states that, in a right-angled triangle, the sum of the squares of the 2 right-angled sides is equal to the square of the hypotenuse (the longer diagonal that joins the 2 right-angled sides).
With this formula (a2+b2=c2), a person can determine the length of the hypotenuse when given the length of the other 2 sides.
“We set about exploring the implications of this and how it might change conclusions in research,” Dr Froud said. “We conducted several experiments using real trial data, and it seems using Pythagoras’s theorem makes a material difference.”
“It helps to identify the point at which a patient has improved with more consistency and accuracy than other methods commonly used. The moral of the story is that, before you throw out the old stuff in the attic, just go through it one last time, as there may be something in there that is still relevant and useful.”
Dr Froud and his colleague Gary Abel, PhD, of the University of Cambridge in the UK, described this research in PLOS ONE. ![]()

Credit: CDC
The 2500-year-old Pythagorean theorem could be the most effective way to identify the point at which a patient’s health begins to improve, a new study suggests.
Researchers made the discovery while examining receiver operating characteristic (ROC) curves, which are used to measure changes in a patient’s health status.
“It all comes down to choosing a point on a curve to determine when recovery has occurred,” said study author Rob Froud, PhD, of the University of Warwick in Coventry, UK.
“For many chronic conditions, epidemiologists agree that the correct point to choose is that which is closest to the top-left corner of the plot containing the curve. As we stopped to think about it, it struck us as obvious that the way to choose this point was by using Pythagoras’s theorem.”
The theorem states that, in a right-angled triangle, the sum of the squares of the 2 right-angled sides is equal to the square of the hypotenuse (the longer diagonal that joins the 2 right-angled sides).
With this formula (a2+b2=c2), a person can determine the length of the hypotenuse when given the length of the other 2 sides.
“We set about exploring the implications of this and how it might change conclusions in research,” Dr Froud said. “We conducted several experiments using real trial data, and it seems using Pythagoras’s theorem makes a material difference.”
“It helps to identify the point at which a patient has improved with more consistency and accuracy than other methods commonly used. The moral of the story is that, before you throw out the old stuff in the attic, just go through it one last time, as there may be something in there that is still relevant and useful.”
Dr Froud and his colleague Gary Abel, PhD, of the University of Cambridge in the UK, described this research in PLOS ONE. ![]()

Credit: CDC
The 2500-year-old Pythagorean theorem could be the most effective way to identify the point at which a patient’s health begins to improve, a new study suggests.
Researchers made the discovery while examining receiver operating characteristic (ROC) curves, which are used to measure changes in a patient’s health status.
“It all comes down to choosing a point on a curve to determine when recovery has occurred,” said study author Rob Froud, PhD, of the University of Warwick in Coventry, UK.
“For many chronic conditions, epidemiologists agree that the correct point to choose is that which is closest to the top-left corner of the plot containing the curve. As we stopped to think about it, it struck us as obvious that the way to choose this point was by using Pythagoras’s theorem.”
The theorem states that, in a right-angled triangle, the sum of the squares of the 2 right-angled sides is equal to the square of the hypotenuse (the longer diagonal that joins the 2 right-angled sides).
With this formula (a2+b2=c2), a person can determine the length of the hypotenuse when given the length of the other 2 sides.
“We set about exploring the implications of this and how it might change conclusions in research,” Dr Froud said. “We conducted several experiments using real trial data, and it seems using Pythagoras’s theorem makes a material difference.”
“It helps to identify the point at which a patient has improved with more consistency and accuracy than other methods commonly used. The moral of the story is that, before you throw out the old stuff in the attic, just go through it one last time, as there may be something in there that is still relevant and useful.”
Dr Froud and his colleague Gary Abel, PhD, of the University of Cambridge in the UK, described this research in PLOS ONE. ![]()
Nanoparticle could enable ‘hypermodal’ imaging
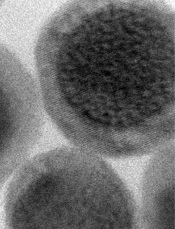
Credit: Jonathan Lovell
A new type of nanoparticle can be used with 6 different imaging techniques, according to research published in Advanced Materials.
Investigators found they could detect these nanoparticles via CT and PET scans, as well as photoacoustic, fluorescence, upconversion, and Cerenkov luminescence imaging.
A machine capable of performing all 6 imaging techniques at once has not yet been invented, to the researchers’ knowledge.
But they hope the creation of their nanoparticles and related work will spur the development of such technology.
That way, patients could receive a single injection of the nanoparticles and have several types of imaging done, which would provide a clearer picture of organs and tissues than a single imaging method alone.
For instance, when the investigators used their nanoparticles to examine the lymph nodes of mice, they found that CT and PET scans provided the
deepest tissue penetration, while the photoacoustic imaging showed blood vessel details the first 2 techniques missed.
“This nanoparticle may open the door for new ‘hypermodal’ imaging systems that allow a lot of new information to be obtained using just one contrast agent,” said study author Jonathan Lovell, PhD, of the University of Buffalo in New York.
“Once such systems are developed, a patient could theoretically go in for one scan with one machine instead of multiple scans with multiple machines.”
Dr Lovell and his colleagues designed their nanoparticles to have 2 components: a core that glows blue when struck by near-infrared light and an outer fabric of porphyrin-phospholipids (PoP) that wraps around the core.
Each part has unique characteristics that make it ideal for certain types of imaging.
The core, initially designed for upconversion imaging, is made from sodium, ytterbium, fluorine, yttrium, and thulium. The ytterbium is dense in electrons—a property that facilitates detection by CT scans.
The PoP wrapper has biophotonic qualities that make it a great match for fluorescence and photoacoustic imagining. The PoP layer is also adept at attracting copper, which is used in PET and Cerenkov luminescence imaging.
“Combining these 2 biocompatible components into a single nanoparticle could give tomorrow’s doctors a powerful new tool for medical imaging,” said Paras Prasad, PhD, also of the University of Buffalo.
“More studies would have to be done to determine whether the nanoparticle is safe to use for such purposes, but it does not contain toxic metals, such as cadmium, that are known to pose potential risks and are found in some other nanoparticles.”
“Another advantage of this core/shell imaging contrast agent is that it could enable biomedical imaging at multiple scales, from single-molecule to cell imaging, as well as from vascular and organ imaging to whole-body bioimaging,” added Guanying Chen, PhD, of the University of Buffalo and Harbin Institute of Technology in China.
Dr Lovell said the next step for this research is to explore additional uses for the technology.
For example, it might be possible to attach a targeting molecule to the PoP surface that would enable cancer cells to take up the particles, something that photoacoustic and fluorescence imaging can detect due to the properties of the smart PoP coating. This would enable doctors to better see where tumors begin and end. ![]()

Credit: Jonathan Lovell
A new type of nanoparticle can be used with 6 different imaging techniques, according to research published in Advanced Materials.
Investigators found they could detect these nanoparticles via CT and PET scans, as well as photoacoustic, fluorescence, upconversion, and Cerenkov luminescence imaging.
A machine capable of performing all 6 imaging techniques at once has not yet been invented, to the researchers’ knowledge.
But they hope the creation of their nanoparticles and related work will spur the development of such technology.
That way, patients could receive a single injection of the nanoparticles and have several types of imaging done, which would provide a clearer picture of organs and tissues than a single imaging method alone.
For instance, when the investigators used their nanoparticles to examine the lymph nodes of mice, they found that CT and PET scans provided the
deepest tissue penetration, while the photoacoustic imaging showed blood vessel details the first 2 techniques missed.
“This nanoparticle may open the door for new ‘hypermodal’ imaging systems that allow a lot of new information to be obtained using just one contrast agent,” said study author Jonathan Lovell, PhD, of the University of Buffalo in New York.
“Once such systems are developed, a patient could theoretically go in for one scan with one machine instead of multiple scans with multiple machines.”
Dr Lovell and his colleagues designed their nanoparticles to have 2 components: a core that glows blue when struck by near-infrared light and an outer fabric of porphyrin-phospholipids (PoP) that wraps around the core.
Each part has unique characteristics that make it ideal for certain types of imaging.
The core, initially designed for upconversion imaging, is made from sodium, ytterbium, fluorine, yttrium, and thulium. The ytterbium is dense in electrons—a property that facilitates detection by CT scans.
The PoP wrapper has biophotonic qualities that make it a great match for fluorescence and photoacoustic imagining. The PoP layer is also adept at attracting copper, which is used in PET and Cerenkov luminescence imaging.
“Combining these 2 biocompatible components into a single nanoparticle could give tomorrow’s doctors a powerful new tool for medical imaging,” said Paras Prasad, PhD, also of the University of Buffalo.
“More studies would have to be done to determine whether the nanoparticle is safe to use for such purposes, but it does not contain toxic metals, such as cadmium, that are known to pose potential risks and are found in some other nanoparticles.”
“Another advantage of this core/shell imaging contrast agent is that it could enable biomedical imaging at multiple scales, from single-molecule to cell imaging, as well as from vascular and organ imaging to whole-body bioimaging,” added Guanying Chen, PhD, of the University of Buffalo and Harbin Institute of Technology in China.
Dr Lovell said the next step for this research is to explore additional uses for the technology.
For example, it might be possible to attach a targeting molecule to the PoP surface that would enable cancer cells to take up the particles, something that photoacoustic and fluorescence imaging can detect due to the properties of the smart PoP coating. This would enable doctors to better see where tumors begin and end. ![]()

Credit: Jonathan Lovell
A new type of nanoparticle can be used with 6 different imaging techniques, according to research published in Advanced Materials.
Investigators found they could detect these nanoparticles via CT and PET scans, as well as photoacoustic, fluorescence, upconversion, and Cerenkov luminescence imaging.
A machine capable of performing all 6 imaging techniques at once has not yet been invented, to the researchers’ knowledge.
But they hope the creation of their nanoparticles and related work will spur the development of such technology.
That way, patients could receive a single injection of the nanoparticles and have several types of imaging done, which would provide a clearer picture of organs and tissues than a single imaging method alone.
For instance, when the investigators used their nanoparticles to examine the lymph nodes of mice, they found that CT and PET scans provided the
deepest tissue penetration, while the photoacoustic imaging showed blood vessel details the first 2 techniques missed.
“This nanoparticle may open the door for new ‘hypermodal’ imaging systems that allow a lot of new information to be obtained using just one contrast agent,” said study author Jonathan Lovell, PhD, of the University of Buffalo in New York.
“Once such systems are developed, a patient could theoretically go in for one scan with one machine instead of multiple scans with multiple machines.”
Dr Lovell and his colleagues designed their nanoparticles to have 2 components: a core that glows blue when struck by near-infrared light and an outer fabric of porphyrin-phospholipids (PoP) that wraps around the core.
Each part has unique characteristics that make it ideal for certain types of imaging.
The core, initially designed for upconversion imaging, is made from sodium, ytterbium, fluorine, yttrium, and thulium. The ytterbium is dense in electrons—a property that facilitates detection by CT scans.
The PoP wrapper has biophotonic qualities that make it a great match for fluorescence and photoacoustic imagining. The PoP layer is also adept at attracting copper, which is used in PET and Cerenkov luminescence imaging.
“Combining these 2 biocompatible components into a single nanoparticle could give tomorrow’s doctors a powerful new tool for medical imaging,” said Paras Prasad, PhD, also of the University of Buffalo.
“More studies would have to be done to determine whether the nanoparticle is safe to use for such purposes, but it does not contain toxic metals, such as cadmium, that are known to pose potential risks and are found in some other nanoparticles.”
“Another advantage of this core/shell imaging contrast agent is that it could enable biomedical imaging at multiple scales, from single-molecule to cell imaging, as well as from vascular and organ imaging to whole-body bioimaging,” added Guanying Chen, PhD, of the University of Buffalo and Harbin Institute of Technology in China.
Dr Lovell said the next step for this research is to explore additional uses for the technology.
For example, it might be possible to attach a targeting molecule to the PoP surface that would enable cancer cells to take up the particles, something that photoacoustic and fluorescence imaging can detect due to the properties of the smart PoP coating. This would enable doctors to better see where tumors begin and end. ![]()
Study reveals genetic changes driving artemisinin resistance

Plasmodium falciparum
Credit: CDC/Mae Melvin
Researchers say they’ve uncovered the complex genetic architecture that enables the malaria parasite Plasmodium falciparum to develop resistance to the antimalarial drug artemisinin.
The team found evidence to suggest that 20 mutations in a single gene work with background mutations in 4 other genes to promote resistance.
The group believes their findings, published in Nature Genetics, could help improve early detection of emerging artemisinin resistance.
To make their discovery, the researchers analyzed 1612 samples from subjects at 15 locations in Southeast Asia and Africa. The team performed P falciparum genome sequencing and genotype calling at more than 600,000 single-nucleotide polymorphism positions on all samples.
The work revealed 20 mutations in the kelch13 gene, a known artemisinin resistance marker, that appear to work in concert with a set of background mutations in 4 other genes—fd, arps10, mdr2, and crt—to support artemisinin resistance.
“Our findings suggest that these background mutations emerged with limited impact on artemisinin resistance—until mutations occurred in the kelch13 gene,” said Roberto Amato, PhD, of the Wellcome Trust Sanger Institute in Oxford, UK.
“It’s similar to what we see with precancerous cells, which accumulate genetic changes but only become malignant when they acquire critical driver mutations that kick off growth.”
The variety of kelch13 mutations associated with artemisinin resistance makes it difficult to use this gene alone as a marker for genetic surveillance.
Monitoring parasite populations for a specific genetic background—in this case, a fixed set of 4 well-defined mutations in fd, arps10, mdr2, and crt—could allow researchers to assess the likelihood of new resistance-causing mutations emerging in different locations, helping to target high-risk regions before resistant parasites take hold.
“We are at a pivotal point for malaria control,” said Nick Day, MBBS, of the Mahidol-Oxford Tropical Medicine Research Unit (MORU) in Bangkok, Thailand.
“While malaria deaths have been halved, this progress is at risk if artemisinin ceases to be effective. We need to use every tool at our disposal to protect this drug. Monitoring parasites for background mutations could provide an early warning system to identify areas at risk for artemisinin resistance.”
The researchers also uncovered new clues about how artemisinin resistance has evolved in Southeast Asia. By comparing parasites from Cambodia, Vietnam, Laos, Thailand, Myanmar, and Bangladesh, the team found that the distribution of different kelch13 mutations is localized within relatively well-defined geographical areas.
Although artemisinin-resistant parasites appear to have migrated across national borders, this only happened on a limited scale. In fact, the most widespread kelch13 mutation, C580Y, seems to have emerged independently on several occasions.
Parasites along the Thailand-Myanmar border appear to have acquired C580Y separately from those in Cambodia and Vietnam. But parasite populations in both regions possess the genetic background mutations, even though they are clearly genetically distinct.
“We don’t yet know the role of these background mutations,” said Olivo Miotto, PhD, also of MORU. “Some may not affect drug resistance directly but, rather, provide an environment where drug-resistance mutations are tolerated.”
“Since kelch13 has hardly changed in 50 million years of Plasmodium evolution, we can assume that this gene is essential to parasite survival. Therefore, kelch13 mutations may severely handicap mutant parasites, compromising their survival unless some other change can counteract this negative effect.”
Mutations in the kelch13 gene were present, yet rare, in Africa. But they weren’t associated with artemisinin resistance and lacked the genetic background present in artemisinin-resistant parasites in Southeast Asia. This provides some reassurance for public health authorities working to prevent the spread of artemisinin resistance to Africa, where most malaria deaths occur.
“These data serve as a reminder of how crucial surveillance and elimination programs are,” said Dominic Kwiatkowski, MBBS, of the Wellcome Trust Sanger Institute.
“At present, artemisinin resistance appears to be largely confined to Southeast Asia, but the situation might change as the parasite population continues to evolve. By linking genomic data with clinical data, we’re developing a better understanding of the multiple genetic factors involved in the emergence of resistance, and that is starting to provide vital clues about how to prevent its spread.” ![]()

Plasmodium falciparum
Credit: CDC/Mae Melvin
Researchers say they’ve uncovered the complex genetic architecture that enables the malaria parasite Plasmodium falciparum to develop resistance to the antimalarial drug artemisinin.
The team found evidence to suggest that 20 mutations in a single gene work with background mutations in 4 other genes to promote resistance.
The group believes their findings, published in Nature Genetics, could help improve early detection of emerging artemisinin resistance.
To make their discovery, the researchers analyzed 1612 samples from subjects at 15 locations in Southeast Asia and Africa. The team performed P falciparum genome sequencing and genotype calling at more than 600,000 single-nucleotide polymorphism positions on all samples.
The work revealed 20 mutations in the kelch13 gene, a known artemisinin resistance marker, that appear to work in concert with a set of background mutations in 4 other genes—fd, arps10, mdr2, and crt—to support artemisinin resistance.
“Our findings suggest that these background mutations emerged with limited impact on artemisinin resistance—until mutations occurred in the kelch13 gene,” said Roberto Amato, PhD, of the Wellcome Trust Sanger Institute in Oxford, UK.
“It’s similar to what we see with precancerous cells, which accumulate genetic changes but only become malignant when they acquire critical driver mutations that kick off growth.”
The variety of kelch13 mutations associated with artemisinin resistance makes it difficult to use this gene alone as a marker for genetic surveillance.
Monitoring parasite populations for a specific genetic background—in this case, a fixed set of 4 well-defined mutations in fd, arps10, mdr2, and crt—could allow researchers to assess the likelihood of new resistance-causing mutations emerging in different locations, helping to target high-risk regions before resistant parasites take hold.
“We are at a pivotal point for malaria control,” said Nick Day, MBBS, of the Mahidol-Oxford Tropical Medicine Research Unit (MORU) in Bangkok, Thailand.
“While malaria deaths have been halved, this progress is at risk if artemisinin ceases to be effective. We need to use every tool at our disposal to protect this drug. Monitoring parasites for background mutations could provide an early warning system to identify areas at risk for artemisinin resistance.”
The researchers also uncovered new clues about how artemisinin resistance has evolved in Southeast Asia. By comparing parasites from Cambodia, Vietnam, Laos, Thailand, Myanmar, and Bangladesh, the team found that the distribution of different kelch13 mutations is localized within relatively well-defined geographical areas.
Although artemisinin-resistant parasites appear to have migrated across national borders, this only happened on a limited scale. In fact, the most widespread kelch13 mutation, C580Y, seems to have emerged independently on several occasions.
Parasites along the Thailand-Myanmar border appear to have acquired C580Y separately from those in Cambodia and Vietnam. But parasite populations in both regions possess the genetic background mutations, even though they are clearly genetically distinct.
“We don’t yet know the role of these background mutations,” said Olivo Miotto, PhD, also of MORU. “Some may not affect drug resistance directly but, rather, provide an environment where drug-resistance mutations are tolerated.”
“Since kelch13 has hardly changed in 50 million years of Plasmodium evolution, we can assume that this gene is essential to parasite survival. Therefore, kelch13 mutations may severely handicap mutant parasites, compromising their survival unless some other change can counteract this negative effect.”
Mutations in the kelch13 gene were present, yet rare, in Africa. But they weren’t associated with artemisinin resistance and lacked the genetic background present in artemisinin-resistant parasites in Southeast Asia. This provides some reassurance for public health authorities working to prevent the spread of artemisinin resistance to Africa, where most malaria deaths occur.
“These data serve as a reminder of how crucial surveillance and elimination programs are,” said Dominic Kwiatkowski, MBBS, of the Wellcome Trust Sanger Institute.
“At present, artemisinin resistance appears to be largely confined to Southeast Asia, but the situation might change as the parasite population continues to evolve. By linking genomic data with clinical data, we’re developing a better understanding of the multiple genetic factors involved in the emergence of resistance, and that is starting to provide vital clues about how to prevent its spread.” ![]()

Plasmodium falciparum
Credit: CDC/Mae Melvin
Researchers say they’ve uncovered the complex genetic architecture that enables the malaria parasite Plasmodium falciparum to develop resistance to the antimalarial drug artemisinin.
The team found evidence to suggest that 20 mutations in a single gene work with background mutations in 4 other genes to promote resistance.
The group believes their findings, published in Nature Genetics, could help improve early detection of emerging artemisinin resistance.
To make their discovery, the researchers analyzed 1612 samples from subjects at 15 locations in Southeast Asia and Africa. The team performed P falciparum genome sequencing and genotype calling at more than 600,000 single-nucleotide polymorphism positions on all samples.
The work revealed 20 mutations in the kelch13 gene, a known artemisinin resistance marker, that appear to work in concert with a set of background mutations in 4 other genes—fd, arps10, mdr2, and crt—to support artemisinin resistance.
“Our findings suggest that these background mutations emerged with limited impact on artemisinin resistance—until mutations occurred in the kelch13 gene,” said Roberto Amato, PhD, of the Wellcome Trust Sanger Institute in Oxford, UK.
“It’s similar to what we see with precancerous cells, which accumulate genetic changes but only become malignant when they acquire critical driver mutations that kick off growth.”
The variety of kelch13 mutations associated with artemisinin resistance makes it difficult to use this gene alone as a marker for genetic surveillance.
Monitoring parasite populations for a specific genetic background—in this case, a fixed set of 4 well-defined mutations in fd, arps10, mdr2, and crt—could allow researchers to assess the likelihood of new resistance-causing mutations emerging in different locations, helping to target high-risk regions before resistant parasites take hold.
“We are at a pivotal point for malaria control,” said Nick Day, MBBS, of the Mahidol-Oxford Tropical Medicine Research Unit (MORU) in Bangkok, Thailand.
“While malaria deaths have been halved, this progress is at risk if artemisinin ceases to be effective. We need to use every tool at our disposal to protect this drug. Monitoring parasites for background mutations could provide an early warning system to identify areas at risk for artemisinin resistance.”
The researchers also uncovered new clues about how artemisinin resistance has evolved in Southeast Asia. By comparing parasites from Cambodia, Vietnam, Laos, Thailand, Myanmar, and Bangladesh, the team found that the distribution of different kelch13 mutations is localized within relatively well-defined geographical areas.
Although artemisinin-resistant parasites appear to have migrated across national borders, this only happened on a limited scale. In fact, the most widespread kelch13 mutation, C580Y, seems to have emerged independently on several occasions.
Parasites along the Thailand-Myanmar border appear to have acquired C580Y separately from those in Cambodia and Vietnam. But parasite populations in both regions possess the genetic background mutations, even though they are clearly genetically distinct.
“We don’t yet know the role of these background mutations,” said Olivo Miotto, PhD, also of MORU. “Some may not affect drug resistance directly but, rather, provide an environment where drug-resistance mutations are tolerated.”
“Since kelch13 has hardly changed in 50 million years of Plasmodium evolution, we can assume that this gene is essential to parasite survival. Therefore, kelch13 mutations may severely handicap mutant parasites, compromising their survival unless some other change can counteract this negative effect.”
Mutations in the kelch13 gene were present, yet rare, in Africa. But they weren’t associated with artemisinin resistance and lacked the genetic background present in artemisinin-resistant parasites in Southeast Asia. This provides some reassurance for public health authorities working to prevent the spread of artemisinin resistance to Africa, where most malaria deaths occur.
“These data serve as a reminder of how crucial surveillance and elimination programs are,” said Dominic Kwiatkowski, MBBS, of the Wellcome Trust Sanger Institute.
“At present, artemisinin resistance appears to be largely confined to Southeast Asia, but the situation might change as the parasite population continues to evolve. By linking genomic data with clinical data, we’re developing a better understanding of the multiple genetic factors involved in the emergence of resistance, and that is starting to provide vital clues about how to prevent its spread.” ![]()
Combining bed nets and vaccines may worsen malaria risk

Credit: Caitlin Kleiboer
New research suggests that combining the use of malaria vaccines and insecticide-treated bed nets may actually increase the incidence of malaria.
The researchers used a mathematical model of malaria transmission to examine potential interactions between vaccines and bed nets.
They found that using insecticide-treated bed nets along with pre-erythrocytic vaccines (PEVs) or blood-stage vaccines (BSVs) increased the number of malaria cases.
However, using bed nets in conjunction with transmission-blocking vaccines (TBVs) resulted in fewer cases of malaria and increased the probability of eliminating the disease.
“The joint use of bed nets and vaccines will not always lead to consistent increases in the efficacy of malaria control,” said study author Mercedes Pascual, PhD, of the University of Michigan in Ann Arbor.
“Specifically, our study suggests that the combined use of some malaria vaccines with bed nets can lead to increased morbidity and mortality in older age classes.”
Dr Pascual and her colleagues described this research in Proceedings of the National Academy of Sciences.
The team noted that the malaria vaccine candidates currently under development fall into 3 categories, each focusing on a different stage of the malaria life cycle.
PEVs aim to reduce the chances that a person will be infected when bitten by a disease-carrying mosquito. BSVs don’t block infection but try to reduce the level of disease severity and the number of fatalities.
And TBVs don’t protect vaccinated individuals against infection or illness, but they prevent mosquitoes from spreading the disease to others after biting a vaccinated person.
Dr Pascual and her colleagues found that using bed nets in communities treated with BSVs can increase levels of morbidity—to levels even higher than those expected in the absence of nets. Furthermore, BSVs can’t promote malaria elimination on their own.
PEVs can promote malaria elimination, but the researchers found regions of decreased morbidity when PEV vaccination levels were low and increased morbidity when PEV vaccination levels were high.
This suggests that higher levels of PEV coverage and bed net use could result in malaria elimination, but it would involve crossing a peak of enhanced morbidity.
Finally, the researchers found that using bed nets in communities treated with TBVs always leads to significant decreases in morbidity and increases the probability of malaria elimination.
“Ironically, the vaccines that work best with bed nets are the ones that do not protect the vaccinated host—the bed net does that—but instead block transmission of malaria in mosquitoes that have found an opportunity to bite vaccinated hosts,” said study author Yael Artzy-Randrup, PhD, of the University of Amsterdam in The Netherlands.
Unraveling the interactions between bed nets and vaccines is especially challenging due to the complex and transient nature of malaria immunity, the researchers noted.
A child’s first malaria infection can result in severe, sometimes fatal, illness. If the child survives, he or she will gain partial immunity that reduces the risk of severe illness in the future.
Additional bites from infected mosquitoes can help the child retain that immunity, which would otherwise wane after 1 to 2 years. But the combination of bed nets and certain vaccines can undermine that natural immunity.
“This complexity is at the heart of why it has been so hard to develop any sort of malaria vaccine,” said study author Andrew Dobson, DPhil, of Princeton University in New Jersey. ![]()

Credit: Caitlin Kleiboer
New research suggests that combining the use of malaria vaccines and insecticide-treated bed nets may actually increase the incidence of malaria.
The researchers used a mathematical model of malaria transmission to examine potential interactions between vaccines and bed nets.
They found that using insecticide-treated bed nets along with pre-erythrocytic vaccines (PEVs) or blood-stage vaccines (BSVs) increased the number of malaria cases.
However, using bed nets in conjunction with transmission-blocking vaccines (TBVs) resulted in fewer cases of malaria and increased the probability of eliminating the disease.
“The joint use of bed nets and vaccines will not always lead to consistent increases in the efficacy of malaria control,” said study author Mercedes Pascual, PhD, of the University of Michigan in Ann Arbor.
“Specifically, our study suggests that the combined use of some malaria vaccines with bed nets can lead to increased morbidity and mortality in older age classes.”
Dr Pascual and her colleagues described this research in Proceedings of the National Academy of Sciences.
The team noted that the malaria vaccine candidates currently under development fall into 3 categories, each focusing on a different stage of the malaria life cycle.
PEVs aim to reduce the chances that a person will be infected when bitten by a disease-carrying mosquito. BSVs don’t block infection but try to reduce the level of disease severity and the number of fatalities.
And TBVs don’t protect vaccinated individuals against infection or illness, but they prevent mosquitoes from spreading the disease to others after biting a vaccinated person.
Dr Pascual and her colleagues found that using bed nets in communities treated with BSVs can increase levels of morbidity—to levels even higher than those expected in the absence of nets. Furthermore, BSVs can’t promote malaria elimination on their own.
PEVs can promote malaria elimination, but the researchers found regions of decreased morbidity when PEV vaccination levels were low and increased morbidity when PEV vaccination levels were high.
This suggests that higher levels of PEV coverage and bed net use could result in malaria elimination, but it would involve crossing a peak of enhanced morbidity.
Finally, the researchers found that using bed nets in communities treated with TBVs always leads to significant decreases in morbidity and increases the probability of malaria elimination.
“Ironically, the vaccines that work best with bed nets are the ones that do not protect the vaccinated host—the bed net does that—but instead block transmission of malaria in mosquitoes that have found an opportunity to bite vaccinated hosts,” said study author Yael Artzy-Randrup, PhD, of the University of Amsterdam in The Netherlands.
Unraveling the interactions between bed nets and vaccines is especially challenging due to the complex and transient nature of malaria immunity, the researchers noted.
A child’s first malaria infection can result in severe, sometimes fatal, illness. If the child survives, he or she will gain partial immunity that reduces the risk of severe illness in the future.
Additional bites from infected mosquitoes can help the child retain that immunity, which would otherwise wane after 1 to 2 years. But the combination of bed nets and certain vaccines can undermine that natural immunity.
“This complexity is at the heart of why it has been so hard to develop any sort of malaria vaccine,” said study author Andrew Dobson, DPhil, of Princeton University in New Jersey. ![]()

Credit: Caitlin Kleiboer
New research suggests that combining the use of malaria vaccines and insecticide-treated bed nets may actually increase the incidence of malaria.
The researchers used a mathematical model of malaria transmission to examine potential interactions between vaccines and bed nets.
They found that using insecticide-treated bed nets along with pre-erythrocytic vaccines (PEVs) or blood-stage vaccines (BSVs) increased the number of malaria cases.
However, using bed nets in conjunction with transmission-blocking vaccines (TBVs) resulted in fewer cases of malaria and increased the probability of eliminating the disease.
“The joint use of bed nets and vaccines will not always lead to consistent increases in the efficacy of malaria control,” said study author Mercedes Pascual, PhD, of the University of Michigan in Ann Arbor.
“Specifically, our study suggests that the combined use of some malaria vaccines with bed nets can lead to increased morbidity and mortality in older age classes.”
Dr Pascual and her colleagues described this research in Proceedings of the National Academy of Sciences.
The team noted that the malaria vaccine candidates currently under development fall into 3 categories, each focusing on a different stage of the malaria life cycle.
PEVs aim to reduce the chances that a person will be infected when bitten by a disease-carrying mosquito. BSVs don’t block infection but try to reduce the level of disease severity and the number of fatalities.
And TBVs don’t protect vaccinated individuals against infection or illness, but they prevent mosquitoes from spreading the disease to others after biting a vaccinated person.
Dr Pascual and her colleagues found that using bed nets in communities treated with BSVs can increase levels of morbidity—to levels even higher than those expected in the absence of nets. Furthermore, BSVs can’t promote malaria elimination on their own.
PEVs can promote malaria elimination, but the researchers found regions of decreased morbidity when PEV vaccination levels were low and increased morbidity when PEV vaccination levels were high.
This suggests that higher levels of PEV coverage and bed net use could result in malaria elimination, but it would involve crossing a peak of enhanced morbidity.
Finally, the researchers found that using bed nets in communities treated with TBVs always leads to significant decreases in morbidity and increases the probability of malaria elimination.
“Ironically, the vaccines that work best with bed nets are the ones that do not protect the vaccinated host—the bed net does that—but instead block transmission of malaria in mosquitoes that have found an opportunity to bite vaccinated hosts,” said study author Yael Artzy-Randrup, PhD, of the University of Amsterdam in The Netherlands.
Unraveling the interactions between bed nets and vaccines is especially challenging due to the complex and transient nature of malaria immunity, the researchers noted.
A child’s first malaria infection can result in severe, sometimes fatal, illness. If the child survives, he or she will gain partial immunity that reduces the risk of severe illness in the future.
Additional bites from infected mosquitoes can help the child retain that immunity, which would otherwise wane after 1 to 2 years. But the combination of bed nets and certain vaccines can undermine that natural immunity.
“This complexity is at the heart of why it has been so hard to develop any sort of malaria vaccine,” said study author Andrew Dobson, DPhil, of Princeton University in New Jersey. ![]()
System can detect Candida better, faster than blood culture
Credit: Jeremy L. Grisham
A diagnostic system can detect sepsis pathogens with high sensitivity and specificity in 3 to 5 hours, eliminating the need for blood culture, according to a study published in Clinical Infectious Diseases.
The system consists of the T2Candida Panel and the T2Dx Instrument, and it provides direct detection of 5 yeast pathogens—Candida albicans, Candida tropicalis, Candida parapsilosis, Candida glabrata, and Candida krusei—in whole blood samples.
T2Candida and T2Dx were cleared for use by the US Food and Drug Administration in September. They are the first diagnostic products powered by T2MR, a magnetic resonance-based diagnostic technology platform that does not require blood culture and sample purification or preparation.
“The ability to determine the presence or absence of Candida within hours—compared to days [with blood culture]—is paradigm-changing for patients at risk for these infections,” said study author Eleftherios Mylonakis, MD, PhD, of Rhode Island Hospital and The Miriam Hospital in Providence.
“It will allow us to move from a ‘best-guess’ approach in treating high-risk patients, such as cancer and transplant patients and patients in the intensive care unit, to a more informed approach where we can quickly direct the best course of therapy, potentially improving patient outcomes and saving lives.”
Study findings
For this multicenter study, Dr Mylonakis and his colleagues collected blood specimens from 1801 hospitalized patients between the ages of 18 and 95 who had a blood culture ordered as part of routine care.
T2Candida and T2Dx demonstrated an overall specificity of 99.4% per assay and 98.1% per patient. The system yielded a specificity of 98.9% for C albicans/C tropicalis, 99.3% for C parapsilosis, and 99.9% for C krusei/C glabrata.
The system had an overall sensitivity of 91.1% per assay and 91.0% per patient. It yielded a sensitivity of 92.3% for C albicans/C tropicalis, 94.2% for C parapsilosis, and 88.1% for C krusei/C glabrata.
The mean time to a positive result for T2Candida and T2Dx was 4.4 hours, compared to 129 hours for blood culture and species identification. The mean time to negative result for T2Candida and T2Dx was 4.2 hours, compared to at least 120 hours for blood culture.
In one case described in the paper, T2Candida and T2Dx detected a Candida infection that blood culture missed in 12 successive tests.
Seven days after the T2Candida result was obtained, physicians performed an invasive procedure to obtain a tissue culture, which proved that the T2Candida result accurately identified a case of intra-abdominal candidiasis.
“Blood culture, the current standard of care for the diagnosis of Candida infections, is known to have poor sensitivity overall and has 38% sensitivity in proven and probable cases of invasive candidiasis,” said study author Cornelius J. Clancy, MD, of the University of Pittsburgh in Pennsylvania.
“In our case, the T2Candida Panel has shown that it can rapidly identify intra-abdominal candidiasis where 12 serial blood culture results were negative. In many patients at risk for candidiasis, the collection of tissue samples for diagnosis is not possible due to their underlying medical conditions. Achieving the level of sensitivity demonstrated in this case, without requiring an intra-abdominal sample, has the potential to positively impact the practice of medicine for these patients.” ![]()

Credit: Jeremy L. Grisham
A diagnostic system can detect sepsis pathogens with high sensitivity and specificity in 3 to 5 hours, eliminating the need for blood culture, according to a study published in Clinical Infectious Diseases.
The system consists of the T2Candida Panel and the T2Dx Instrument, and it provides direct detection of 5 yeast pathogens—Candida albicans, Candida tropicalis, Candida parapsilosis, Candida glabrata, and Candida krusei—in whole blood samples.
T2Candida and T2Dx were cleared for use by the US Food and Drug Administration in September. They are the first diagnostic products powered by T2MR, a magnetic resonance-based diagnostic technology platform that does not require blood culture and sample purification or preparation.
“The ability to determine the presence or absence of Candida within hours—compared to days [with blood culture]—is paradigm-changing for patients at risk for these infections,” said study author Eleftherios Mylonakis, MD, PhD, of Rhode Island Hospital and The Miriam Hospital in Providence.
“It will allow us to move from a ‘best-guess’ approach in treating high-risk patients, such as cancer and transplant patients and patients in the intensive care unit, to a more informed approach where we can quickly direct the best course of therapy, potentially improving patient outcomes and saving lives.”
Study findings
For this multicenter study, Dr Mylonakis and his colleagues collected blood specimens from 1801 hospitalized patients between the ages of 18 and 95 who had a blood culture ordered as part of routine care.
T2Candida and T2Dx demonstrated an overall specificity of 99.4% per assay and 98.1% per patient. The system yielded a specificity of 98.9% for C albicans/C tropicalis, 99.3% for C parapsilosis, and 99.9% for C krusei/C glabrata.
The system had an overall sensitivity of 91.1% per assay and 91.0% per patient. It yielded a sensitivity of 92.3% for C albicans/C tropicalis, 94.2% for C parapsilosis, and 88.1% for C krusei/C glabrata.
The mean time to a positive result for T2Candida and T2Dx was 4.4 hours, compared to 129 hours for blood culture and species identification. The mean time to negative result for T2Candida and T2Dx was 4.2 hours, compared to at least 120 hours for blood culture.
In one case described in the paper, T2Candida and T2Dx detected a Candida infection that blood culture missed in 12 successive tests.
Seven days after the T2Candida result was obtained, physicians performed an invasive procedure to obtain a tissue culture, which proved that the T2Candida result accurately identified a case of intra-abdominal candidiasis.
“Blood culture, the current standard of care for the diagnosis of Candida infections, is known to have poor sensitivity overall and has 38% sensitivity in proven and probable cases of invasive candidiasis,” said study author Cornelius J. Clancy, MD, of the University of Pittsburgh in Pennsylvania.
“In our case, the T2Candida Panel has shown that it can rapidly identify intra-abdominal candidiasis where 12 serial blood culture results were negative. In many patients at risk for candidiasis, the collection of tissue samples for diagnosis is not possible due to their underlying medical conditions. Achieving the level of sensitivity demonstrated in this case, without requiring an intra-abdominal sample, has the potential to positively impact the practice of medicine for these patients.” ![]()

Credit: Jeremy L. Grisham
A diagnostic system can detect sepsis pathogens with high sensitivity and specificity in 3 to 5 hours, eliminating the need for blood culture, according to a study published in Clinical Infectious Diseases.
The system consists of the T2Candida Panel and the T2Dx Instrument, and it provides direct detection of 5 yeast pathogens—Candida albicans, Candida tropicalis, Candida parapsilosis, Candida glabrata, and Candida krusei—in whole blood samples.
T2Candida and T2Dx were cleared for use by the US Food and Drug Administration in September. They are the first diagnostic products powered by T2MR, a magnetic resonance-based diagnostic technology platform that does not require blood culture and sample purification or preparation.
“The ability to determine the presence or absence of Candida within hours—compared to days [with blood culture]—is paradigm-changing for patients at risk for these infections,” said study author Eleftherios Mylonakis, MD, PhD, of Rhode Island Hospital and The Miriam Hospital in Providence.
“It will allow us to move from a ‘best-guess’ approach in treating high-risk patients, such as cancer and transplant patients and patients in the intensive care unit, to a more informed approach where we can quickly direct the best course of therapy, potentially improving patient outcomes and saving lives.”
Study findings
For this multicenter study, Dr Mylonakis and his colleagues collected blood specimens from 1801 hospitalized patients between the ages of 18 and 95 who had a blood culture ordered as part of routine care.
T2Candida and T2Dx demonstrated an overall specificity of 99.4% per assay and 98.1% per patient. The system yielded a specificity of 98.9% for C albicans/C tropicalis, 99.3% for C parapsilosis, and 99.9% for C krusei/C glabrata.
The system had an overall sensitivity of 91.1% per assay and 91.0% per patient. It yielded a sensitivity of 92.3% for C albicans/C tropicalis, 94.2% for C parapsilosis, and 88.1% for C krusei/C glabrata.
The mean time to a positive result for T2Candida and T2Dx was 4.4 hours, compared to 129 hours for blood culture and species identification. The mean time to negative result for T2Candida and T2Dx was 4.2 hours, compared to at least 120 hours for blood culture.
In one case described in the paper, T2Candida and T2Dx detected a Candida infection that blood culture missed in 12 successive tests.
Seven days after the T2Candida result was obtained, physicians performed an invasive procedure to obtain a tissue culture, which proved that the T2Candida result accurately identified a case of intra-abdominal candidiasis.
“Blood culture, the current standard of care for the diagnosis of Candida infections, is known to have poor sensitivity overall and has 38% sensitivity in proven and probable cases of invasive candidiasis,” said study author Cornelius J. Clancy, MD, of the University of Pittsburgh in Pennsylvania.
“In our case, the T2Candida Panel has shown that it can rapidly identify intra-abdominal candidiasis where 12 serial blood culture results were negative. In many patients at risk for candidiasis, the collection of tissue samples for diagnosis is not possible due to their underlying medical conditions. Achieving the level of sensitivity demonstrated in this case, without requiring an intra-abdominal sample, has the potential to positively impact the practice of medicine for these patients.”
Study offers explanation for gender gaps in academia

Credit: Rhoda Baer
New research offers an explanation for the lack of women in certain academic fields.
It isn’t that women don’t want to work long hours or can’t compete in highly selective fields, and it isn’t that they are less analytical than men, the researchers reported.
Instead, it appears that women are underrepresented in academic fields whose practitioners put a lot of emphasis on the importance of being brilliant—a quality some people assume women lack.
Sarah-Jane Leslie, PhD, of Princeton University in New Jersey, and her colleagues reported these findings in Science.
The researchers focused on a broad swath of academic disciplines, including those in the sciences, the humanities, social sciences, and math.
They focused on the culture of different fields, reasoning that stereotypes of women’s inferior intellectual abilities might help explain why women are underrepresented in fields—such as physics or philosophy—that idolize geniuses.
The team surveyed more than 1800 graduate students, post-doctoral researchers, and faculty members in 30 academic disciplines and, among other things, asked them what qualities were required for success in their fields.
Across the board, in the sciences, technology, engineering, and math (STEM) fields, as well as in the humanities and social sciences, women were found to be underrepresented in those disciplines whose practitioners put a premium on brilliance.
“We’re not saying brilliance—or valuing brilliance—is a bad thing,” said study author Andrei Cimpian, PhD, of the University of Illinois at Urbana-Champaign.
“And we’re not saying women are not brilliant or that being brilliant isn’t helpful to one’s academic career. Our data don’t address that. What they suggest is that conveying to your students a belief that brilliance is required for success may have a differential effect on males and females that are looking to pursue careers in your field.”
The team also tested 3 other hypotheses that might help explain women’s underrepresentation in some fields: that women avoid careers that require them to work long hours, that women are less able than men to get into highly selective fields, and that women are outnumbered by men in fields that require analytical, systematical reasoning.
“We found that none of these 3 alternative hypotheses was able to predict women’s representation across the academic spectrum,” Dr Leslie said. “A strong emphasis on brilliance among practitioners of particular fields was the best predictor of women’s underrepresentation in those fields.”
The researchers are still investigating whether women are actively avoiding fields that focus on cultivating brilliant individuals, or if practitioners in those fields are discriminating against women based on their beliefs about women’s aptitudes. A combination of the two is certainly plausible, according to Dr Cimpian.
“There is no convincing evidence in the literature that men and women differ intellectually in ways that would be relevant to their success across the entire range of fields we surveyed,” Dr Cimpian said. “So it is most likely that female underrepresentation is not the result of actual differences in intellectual ability but rather the result of perceived or presumed differences between women and men.”

Credit: Rhoda Baer
New research offers an explanation for the lack of women in certain academic fields.
It isn’t that women don’t want to work long hours or can’t compete in highly selective fields, and it isn’t that they are less analytical than men, the researchers reported.
Instead, it appears that women are underrepresented in academic fields whose practitioners put a lot of emphasis on the importance of being brilliant—a quality some people assume women lack.
Sarah-Jane Leslie, PhD, of Princeton University in New Jersey, and her colleagues reported these findings in Science.
The researchers focused on a broad swath of academic disciplines, including those in the sciences, the humanities, social sciences, and math.
They focused on the culture of different fields, reasoning that stereotypes of women’s inferior intellectual abilities might help explain why women are underrepresented in fields—such as physics or philosophy—that idolize geniuses.
The team surveyed more than 1800 graduate students, post-doctoral researchers, and faculty members in 30 academic disciplines and, among other things, asked them what qualities were required for success in their fields.
Across the board, in the sciences, technology, engineering, and math (STEM) fields, as well as in the humanities and social sciences, women were found to be underrepresented in those disciplines whose practitioners put a premium on brilliance.
“We’re not saying brilliance—or valuing brilliance—is a bad thing,” said study author Andrei Cimpian, PhD, of the University of Illinois at Urbana-Champaign.
“And we’re not saying women are not brilliant or that being brilliant isn’t helpful to one’s academic career. Our data don’t address that. What they suggest is that conveying to your students a belief that brilliance is required for success may have a differential effect on males and females that are looking to pursue careers in your field.”
The team also tested 3 other hypotheses that might help explain women’s underrepresentation in some fields: that women avoid careers that require them to work long hours, that women are less able than men to get into highly selective fields, and that women are outnumbered by men in fields that require analytical, systematical reasoning.
“We found that none of these 3 alternative hypotheses was able to predict women’s representation across the academic spectrum,” Dr Leslie said. “A strong emphasis on brilliance among practitioners of particular fields was the best predictor of women’s underrepresentation in those fields.”
The researchers are still investigating whether women are actively avoiding fields that focus on cultivating brilliant individuals, or if practitioners in those fields are discriminating against women based on their beliefs about women’s aptitudes. A combination of the two is certainly plausible, according to Dr Cimpian.
“There is no convincing evidence in the literature that men and women differ intellectually in ways that would be relevant to their success across the entire range of fields we surveyed,” Dr Cimpian said. “So it is most likely that female underrepresentation is not the result of actual differences in intellectual ability but rather the result of perceived or presumed differences between women and men.”

Credit: Rhoda Baer
New research offers an explanation for the lack of women in certain academic fields.
It isn’t that women don’t want to work long hours or can’t compete in highly selective fields, and it isn’t that they are less analytical than men, the researchers reported.
Instead, it appears that women are underrepresented in academic fields whose practitioners put a lot of emphasis on the importance of being brilliant—a quality some people assume women lack.
Sarah-Jane Leslie, PhD, of Princeton University in New Jersey, and her colleagues reported these findings in Science.
The researchers focused on a broad swath of academic disciplines, including those in the sciences, the humanities, social sciences, and math.
They focused on the culture of different fields, reasoning that stereotypes of women’s inferior intellectual abilities might help explain why women are underrepresented in fields—such as physics or philosophy—that idolize geniuses.
The team surveyed more than 1800 graduate students, post-doctoral researchers, and faculty members in 30 academic disciplines and, among other things, asked them what qualities were required for success in their fields.
Across the board, in the sciences, technology, engineering, and math (STEM) fields, as well as in the humanities and social sciences, women were found to be underrepresented in those disciplines whose practitioners put a premium on brilliance.
“We’re not saying brilliance—or valuing brilliance—is a bad thing,” said study author Andrei Cimpian, PhD, of the University of Illinois at Urbana-Champaign.
“And we’re not saying women are not brilliant or that being brilliant isn’t helpful to one’s academic career. Our data don’t address that. What they suggest is that conveying to your students a belief that brilliance is required for success may have a differential effect on males and females that are looking to pursue careers in your field.”
The team also tested 3 other hypotheses that might help explain women’s underrepresentation in some fields: that women avoid careers that require them to work long hours, that women are less able than men to get into highly selective fields, and that women are outnumbered by men in fields that require analytical, systematical reasoning.
“We found that none of these 3 alternative hypotheses was able to predict women’s representation across the academic spectrum,” Dr Leslie said. “A strong emphasis on brilliance among practitioners of particular fields was the best predictor of women’s underrepresentation in those fields.”
The researchers are still investigating whether women are actively avoiding fields that focus on cultivating brilliant individuals, or if practitioners in those fields are discriminating against women based on their beliefs about women’s aptitudes. A combination of the two is certainly plausible, according to Dr Cimpian.
“There is no convincing evidence in the literature that men and women differ intellectually in ways that would be relevant to their success across the entire range of fields we surveyed,” Dr Cimpian said. “So it is most likely that female underrepresentation is not the result of actual differences in intellectual ability but rather the result of perceived or presumed differences between women and men.”
Antibiotics may enhance mosquitoes’ ability to transmit malaria

Credit: James Gathany
Mosquitoes’ ability to transmit malaria may be affected by antibiotics in the blood of those they bite, according to research published in Nature Communications.
Feeding on blood that contained the antibiotics penicillin and streptomycin (PS) hindered bacterial growth in mosquitoes’ guts.
The mosquitoes also became more susceptible to malaria infection, exhibited improved fertility, and lived longer than mosquitoes whose blood meals did not contain PS.
Study investigators said these findings do not suggest people should avoid taking antibiotics. But the study does indicate that more research is needed to explore how different combinations of antibiotics affect mosquitoes’ ability to spread malaria.
“Antibiotics are a valuable weapon in the fight against malaria and other diseases,” said study author Mathilde Gendrin, PhD, of Imperial College London in the UK.
“Our study suggests that the presence of antibiotics in people’s blood may have hidden effects on the guts of mosquitoes when mosquitoes ingest that blood, and that these effects could alter the mosquitoes’ ability to transmit malaria.”
Dr Gendrin and her colleagues chose to evaluate the effects of PS because these antibiotics are not used to combat malaria and don’t directly affect malaria parasites.
The team began their research by supplementing blood with therapeutic concentrations of PS and feeding the blood to Anopheles gambiae mosquitoes.
The investigators monitored the bacterial load in the mosquito gut over 3 blood feeds offered every 3 days. And they found that the proliferation of bacteria typically seen at 24 hours after a blood meal was reduced by 70% when mosquitoes received blood containing PS.
Next, the researchers conducted 3 experiments to determine whether receiving blood containing PS would influence the mosquitoes’ susceptibility to malaria infection.
In the first experiment, the team fed mosquitoes blood from rodents infected with Plasmodium berghei before or after the animals received PS.
The investigators assessed infection by counting the proportion of mosquitoes carrying oocysts (prevalence) and the number of oocysts per mosquito (intensity). In the presence of PS, infection prevalence increased by 21% (P=5.10-7), and the median intensity doubled (P=0.041).
In the second experiment, the researchers assessed the effect of PS on infection with human parasites. They fed mosquitoes blood containing Plasmodium falciparum gametocytes (cultured in vitro) and supplemented the blood with PS or buffer.
Again, the team observed higher infection prevalence (P=0.0033) and intensity (P=0.00026) in the presence of PS.
In the third experiment, the investigators fed mosquitoes blood freshly drawn from children carrying P falciparum gametocytes. The blood was supplemented with PS or buffer.
Once more, the intensity of infection significantly increased in the presence of PS (P=0.02). The 6.3% increase in infection prevalence was not statistically significant (P=0.4), but the researchers said this was likely due to the reduced statistical power of the experiment.
The team’s final experiments assessed the effects of PS on mosquitoes’ fertility and survival.
Exposure to PS led to a 32% higher proportion of egg-laying females (P=0.0038) and a 53% higher average number of eggs per female (P=0.016), although the proportion of eggs hatching into larvae was not affected.
Mosquito survival increased significantly after the insects ingested PS-treated human blood. The P value was 0.017 for the first blood meal and 0.0016 for all 3 blood meals.
“We only looked at two antibiotics in our study, so this is early stage research, and we don’t know what it means for other antibiotics,” Dr Gendrin noted.
“It’s possible other antibiotics might have no effect, or that they might make it harder for mosquitoes to transmit malaria. We would like to see much more research carried out to further understand our findings and to explore how other antibiotics might affect bacteria in the guts of mosquitoes.”
“Ultimately, we hope that understanding any hidden effects of different antibiotics would mean we can combat the spread of malaria more effectively,” added study author George Christophides, PhD, also of Imperial College London.
“For example, if particular antibiotics make mosquitoes more able to transmit malaria, the use of these could be combined with supply of bed nets in order to reduce mosquito bites. Additionally, if a doctor prescribed such antibiotics to a malaria patient, they could combine this with a drug such as atovaquone that can both treat malaria and block its transmission.”

Credit: James Gathany
Mosquitoes’ ability to transmit malaria may be affected by antibiotics in the blood of those they bite, according to research published in Nature Communications.
Feeding on blood that contained the antibiotics penicillin and streptomycin (PS) hindered bacterial growth in mosquitoes’ guts.
The mosquitoes also became more susceptible to malaria infection, exhibited improved fertility, and lived longer than mosquitoes whose blood meals did not contain PS.
Study investigators said these findings do not suggest people should avoid taking antibiotics. But the study does indicate that more research is needed to explore how different combinations of antibiotics affect mosquitoes’ ability to spread malaria.
“Antibiotics are a valuable weapon in the fight against malaria and other diseases,” said study author Mathilde Gendrin, PhD, of Imperial College London in the UK.
“Our study suggests that the presence of antibiotics in people’s blood may have hidden effects on the guts of mosquitoes when mosquitoes ingest that blood, and that these effects could alter the mosquitoes’ ability to transmit malaria.”
Dr Gendrin and her colleagues chose to evaluate the effects of PS because these antibiotics are not used to combat malaria and don’t directly affect malaria parasites.
The team began their research by supplementing blood with therapeutic concentrations of PS and feeding the blood to Anopheles gambiae mosquitoes.
The investigators monitored the bacterial load in the mosquito gut over 3 blood feeds offered every 3 days. And they found that the proliferation of bacteria typically seen at 24 hours after a blood meal was reduced by 70% when mosquitoes received blood containing PS.
Next, the researchers conducted 3 experiments to determine whether receiving blood containing PS would influence the mosquitoes’ susceptibility to malaria infection.
In the first experiment, the team fed mosquitoes blood from rodents infected with Plasmodium berghei before or after the animals received PS.
The investigators assessed infection by counting the proportion of mosquitoes carrying oocysts (prevalence) and the number of oocysts per mosquito (intensity). In the presence of PS, infection prevalence increased by 21% (P=5.10-7), and the median intensity doubled (P=0.041).
In the second experiment, the researchers assessed the effect of PS on infection with human parasites. They fed mosquitoes blood containing Plasmodium falciparum gametocytes (cultured in vitro) and supplemented the blood with PS or buffer.
Again, the team observed higher infection prevalence (P=0.0033) and intensity (P=0.00026) in the presence of PS.
In the third experiment, the investigators fed mosquitoes blood freshly drawn from children carrying P falciparum gametocytes. The blood was supplemented with PS or buffer.
Once more, the intensity of infection significantly increased in the presence of PS (P=0.02). The 6.3% increase in infection prevalence was not statistically significant (P=0.4), but the researchers said this was likely due to the reduced statistical power of the experiment.
The team’s final experiments assessed the effects of PS on mosquitoes’ fertility and survival.
Exposure to PS led to a 32% higher proportion of egg-laying females (P=0.0038) and a 53% higher average number of eggs per female (P=0.016), although the proportion of eggs hatching into larvae was not affected.
Mosquito survival increased significantly after the insects ingested PS-treated human blood. The P value was 0.017 for the first blood meal and 0.0016 for all 3 blood meals.
“We only looked at two antibiotics in our study, so this is early stage research, and we don’t know what it means for other antibiotics,” Dr Gendrin noted.
“It’s possible other antibiotics might have no effect, or that they might make it harder for mosquitoes to transmit malaria. We would like to see much more research carried out to further understand our findings and to explore how other antibiotics might affect bacteria in the guts of mosquitoes.”
“Ultimately, we hope that understanding any hidden effects of different antibiotics would mean we can combat the spread of malaria more effectively,” added study author George Christophides, PhD, also of Imperial College London.
“For example, if particular antibiotics make mosquitoes more able to transmit malaria, the use of these could be combined with supply of bed nets in order to reduce mosquito bites. Additionally, if a doctor prescribed such antibiotics to a malaria patient, they could combine this with a drug such as atovaquone that can both treat malaria and block its transmission.”

Credit: James Gathany
Mosquitoes’ ability to transmit malaria may be affected by antibiotics in the blood of those they bite, according to research published in Nature Communications.
Feeding on blood that contained the antibiotics penicillin and streptomycin (PS) hindered bacterial growth in mosquitoes’ guts.
The mosquitoes also became more susceptible to malaria infection, exhibited improved fertility, and lived longer than mosquitoes whose blood meals did not contain PS.
Study investigators said these findings do not suggest people should avoid taking antibiotics. But the study does indicate that more research is needed to explore how different combinations of antibiotics affect mosquitoes’ ability to spread malaria.
“Antibiotics are a valuable weapon in the fight against malaria and other diseases,” said study author Mathilde Gendrin, PhD, of Imperial College London in the UK.
“Our study suggests that the presence of antibiotics in people’s blood may have hidden effects on the guts of mosquitoes when mosquitoes ingest that blood, and that these effects could alter the mosquitoes’ ability to transmit malaria.”
Dr Gendrin and her colleagues chose to evaluate the effects of PS because these antibiotics are not used to combat malaria and don’t directly affect malaria parasites.
The team began their research by supplementing blood with therapeutic concentrations of PS and feeding the blood to Anopheles gambiae mosquitoes.
The investigators monitored the bacterial load in the mosquito gut over 3 blood feeds offered every 3 days. And they found that the proliferation of bacteria typically seen at 24 hours after a blood meal was reduced by 70% when mosquitoes received blood containing PS.
Next, the researchers conducted 3 experiments to determine whether receiving blood containing PS would influence the mosquitoes’ susceptibility to malaria infection.
In the first experiment, the team fed mosquitoes blood from rodents infected with Plasmodium berghei before or after the animals received PS.
The investigators assessed infection by counting the proportion of mosquitoes carrying oocysts (prevalence) and the number of oocysts per mosquito (intensity). In the presence of PS, infection prevalence increased by 21% (P=5.10-7), and the median intensity doubled (P=0.041).
In the second experiment, the researchers assessed the effect of PS on infection with human parasites. They fed mosquitoes blood containing Plasmodium falciparum gametocytes (cultured in vitro) and supplemented the blood with PS or buffer.
Again, the team observed higher infection prevalence (P=0.0033) and intensity (P=0.00026) in the presence of PS.
In the third experiment, the investigators fed mosquitoes blood freshly drawn from children carrying P falciparum gametocytes. The blood was supplemented with PS or buffer.
Once more, the intensity of infection significantly increased in the presence of PS (P=0.02). The 6.3% increase in infection prevalence was not statistically significant (P=0.4), but the researchers said this was likely due to the reduced statistical power of the experiment.
The team’s final experiments assessed the effects of PS on mosquitoes’ fertility and survival.
Exposure to PS led to a 32% higher proportion of egg-laying females (P=0.0038) and a 53% higher average number of eggs per female (P=0.016), although the proportion of eggs hatching into larvae was not affected.
Mosquito survival increased significantly after the insects ingested PS-treated human blood. The P value was 0.017 for the first blood meal and 0.0016 for all 3 blood meals.
“We only looked at two antibiotics in our study, so this is early stage research, and we don’t know what it means for other antibiotics,” Dr Gendrin noted.
“It’s possible other antibiotics might have no effect, or that they might make it harder for mosquitoes to transmit malaria. We would like to see much more research carried out to further understand our findings and to explore how other antibiotics might affect bacteria in the guts of mosquitoes.”
“Ultimately, we hope that understanding any hidden effects of different antibiotics would mean we can combat the spread of malaria more effectively,” added study author George Christophides, PhD, also of Imperial College London.
“For example, if particular antibiotics make mosquitoes more able to transmit malaria, the use of these could be combined with supply of bed nets in order to reduce mosquito bites. Additionally, if a doctor prescribed such antibiotics to a malaria patient, they could combine this with a drug such as atovaquone that can both treat malaria and block its transmission.”
IPT doesn’t seem to benefit children with anemia

one of the trials took place
Credit: Gabrielle Tenenbaum
Intermittent preventive antimalarial treatment (IPT) does not provide much benefit for anemic children living in malaria-endemic regions, results of a review indicate.
Researchers reviewed 6 randomized, controlled trials and found that IPT, doses of antimalarial drugs given at regular intervals in case children had contracted malaria, did lead to an improvement in hemoglobin levels.
But this did not translate to a reduction in the incidence of anemia or the rate of death and hospitalization compared to children who received placebo.
“While we did note small benefits in hemoglobin levels when treating anemic children with IPT, there was no detectable effect on the number of deaths or hospital admissions,” said review author Mwaka Athuman, of Ifakara Health Institute in Dodoma, Tanzania, Africa.
“However, 3 of the trials were carried out in areas where malaria transmission was low, so any estimate of the protective effect of IPT would be expected to be modest. The summary of the evidence will assist people forming policy guidance as to whether IPT is worthwhile and provide a basis for researchers to consider whether additional studies are needed.”
The researchers reported these findings in the Cochrane Database of Systematic Reviews.
The team reviewed 6 trials that included a total of 3847 children with anemia. Three trials were conducted in areas of low malaria endemicity and 3 in areas of moderate-to-high endemicity.
In all trials, there was a group of children who received IPT and a control group receiving placebo. In some trials, children also received iron supplements, and this was taken into consideration when the researchers analyzed the data.
Data from 4 of the trials showed that IPT did increase the mean change in hemoglobin levels from baseline to follow-up at 12 weeks—on average, by 0.32 g/dL. The reviewers dubbed this moderate-quality evidence.
Results from the same 4 trials showed that the mean hemoglobin at 12 weeks’ follow-up was, on average, 0.35 g/dL higher in the IPT group than in the placebo group. This was considered low-quality evidence.
Regardless of improvements in hemoglobin, there was no significant difference in the number of children who had anemia at 12 weeks. The median risk of anemia across 4 trials was 579 per 1000 in the placebo group and 561 per 1000 in the IPT group. This was considered moderate-quality evidence.
Similarly, there was no significant difference in the rate of death and hospitalization at 6 months between children who received IPT and those who received placebo.
The median risk of both events combined was 34 per 1000 in the placebo group and 31 per 1000 in the IPT group. This was based on data from 3 trials and was considered moderate-quality evidence.
For all of these outcomes, there was no significant difference between children who received iron and those who did not, and there was no difference between children living in regions of low malaria endemicity and those living in regions of moderate-to-high malaria endemicity.

one of the trials took place
Credit: Gabrielle Tenenbaum
Intermittent preventive antimalarial treatment (IPT) does not provide much benefit for anemic children living in malaria-endemic regions, results of a review indicate.
Researchers reviewed 6 randomized, controlled trials and found that IPT, doses of antimalarial drugs given at regular intervals in case children had contracted malaria, did lead to an improvement in hemoglobin levels.
But this did not translate to a reduction in the incidence of anemia or the rate of death and hospitalization compared to children who received placebo.
“While we did note small benefits in hemoglobin levels when treating anemic children with IPT, there was no detectable effect on the number of deaths or hospital admissions,” said review author Mwaka Athuman, of Ifakara Health Institute in Dodoma, Tanzania, Africa.
“However, 3 of the trials were carried out in areas where malaria transmission was low, so any estimate of the protective effect of IPT would be expected to be modest. The summary of the evidence will assist people forming policy guidance as to whether IPT is worthwhile and provide a basis for researchers to consider whether additional studies are needed.”
The researchers reported these findings in the Cochrane Database of Systematic Reviews.
The team reviewed 6 trials that included a total of 3847 children with anemia. Three trials were conducted in areas of low malaria endemicity and 3 in areas of moderate-to-high endemicity.
In all trials, there was a group of children who received IPT and a control group receiving placebo. In some trials, children also received iron supplements, and this was taken into consideration when the researchers analyzed the data.
Data from 4 of the trials showed that IPT did increase the mean change in hemoglobin levels from baseline to follow-up at 12 weeks—on average, by 0.32 g/dL. The reviewers dubbed this moderate-quality evidence.
Results from the same 4 trials showed that the mean hemoglobin at 12 weeks’ follow-up was, on average, 0.35 g/dL higher in the IPT group than in the placebo group. This was considered low-quality evidence.
Regardless of improvements in hemoglobin, there was no significant difference in the number of children who had anemia at 12 weeks. The median risk of anemia across 4 trials was 579 per 1000 in the placebo group and 561 per 1000 in the IPT group. This was considered moderate-quality evidence.
Similarly, there was no significant difference in the rate of death and hospitalization at 6 months between children who received IPT and those who received placebo.
The median risk of both events combined was 34 per 1000 in the placebo group and 31 per 1000 in the IPT group. This was based on data from 3 trials and was considered moderate-quality evidence.
For all of these outcomes, there was no significant difference between children who received iron and those who did not, and there was no difference between children living in regions of low malaria endemicity and those living in regions of moderate-to-high malaria endemicity.

one of the trials took place
Credit: Gabrielle Tenenbaum
Intermittent preventive antimalarial treatment (IPT) does not provide much benefit for anemic children living in malaria-endemic regions, results of a review indicate.
Researchers reviewed 6 randomized, controlled trials and found that IPT, doses of antimalarial drugs given at regular intervals in case children had contracted malaria, did lead to an improvement in hemoglobin levels.
But this did not translate to a reduction in the incidence of anemia or the rate of death and hospitalization compared to children who received placebo.
“While we did note small benefits in hemoglobin levels when treating anemic children with IPT, there was no detectable effect on the number of deaths or hospital admissions,” said review author Mwaka Athuman, of Ifakara Health Institute in Dodoma, Tanzania, Africa.
“However, 3 of the trials were carried out in areas where malaria transmission was low, so any estimate of the protective effect of IPT would be expected to be modest. The summary of the evidence will assist people forming policy guidance as to whether IPT is worthwhile and provide a basis for researchers to consider whether additional studies are needed.”
The researchers reported these findings in the Cochrane Database of Systematic Reviews.
The team reviewed 6 trials that included a total of 3847 children with anemia. Three trials were conducted in areas of low malaria endemicity and 3 in areas of moderate-to-high endemicity.
In all trials, there was a group of children who received IPT and a control group receiving placebo. In some trials, children also received iron supplements, and this was taken into consideration when the researchers analyzed the data.
Data from 4 of the trials showed that IPT did increase the mean change in hemoglobin levels from baseline to follow-up at 12 weeks—on average, by 0.32 g/dL. The reviewers dubbed this moderate-quality evidence.
Results from the same 4 trials showed that the mean hemoglobin at 12 weeks’ follow-up was, on average, 0.35 g/dL higher in the IPT group than in the placebo group. This was considered low-quality evidence.
Regardless of improvements in hemoglobin, there was no significant difference in the number of children who had anemia at 12 weeks. The median risk of anemia across 4 trials was 579 per 1000 in the placebo group and 561 per 1000 in the IPT group. This was considered moderate-quality evidence.
Similarly, there was no significant difference in the rate of death and hospitalization at 6 months between children who received IPT and those who received placebo.
The median risk of both events combined was 34 per 1000 in the placebo group and 31 per 1000 in the IPT group. This was based on data from 3 trials and was considered moderate-quality evidence.
For all of these outcomes, there was no significant difference between children who received iron and those who did not, and there was no difference between children living in regions of low malaria endemicity and those living in regions of moderate-to-high malaria endemicity.