User login
Compounds can target Ras pathway

Credit: NIH
A newly identified class of compounds recognize a key target in the Ras signaling pathway and could therefore prove useful in treating a range of malignancies, according to research published in Chemistry & Biology.
The lead compound, NSC-658497, targeted the catalytic activation of Ras by an enzyme called SOS1.
NSC-658497 blocked SOS1-mediated molecular signaling in the Ras pathway that causes rapid cell proliferation, tumor development, and cancer.
“While Ras pathway activation is a dominant event happening in many diseases, so far, the immediate signaling module of the Ras pathway has been difficult to target,” said study author Yi Zheng, PhD, of Cincinnati Children’s Hospital in Ohio.
“Most strategies for treatment have been geared toward hitting molecular effectors that are farther downstream. In this study, we have identified synthetic compounds that specifically recognize the catalytic pocket of SOS1 and demonstrated that they are effective inhibitors of Ras signaling in cells. This establishes a novel targeting approach for cancers and Rasopathies that is useful in developing therapeutics.”
Rasopathies include a group of 9 developmental syndromes that are caused by mutations in the Ras pathway (Noonan, LEOPARD, hereditary Gingival fibromatosis type 1, Capillary malformation-AV malformation, Neurofibromatosis type 1, Legius, Costello, Cardio-facio-cutaneous, and autoimmune lymphoproliferative syndromes).
Dysregulation of the Ras pathway (including its SOS1 catalytic activator) is also linked to a number of malignancies, such as breast, pancreatic, and cervical cancers, as well as leukemia.
To find compounds that could target the Ras pathway, Dr Zheng and his colleagues tested 30,000 synthetic molecular compounds in a database maintained by the National Cancer Institute.
The researchers looked for the compounds’ ability to dock with the catalytic site of SOS1, which led them to identify NSC-658497 and derivatives as lead candidates for the development of a prospective drug.
The team then tested NSC-658497 in cell lines of mouse fibroblasts and prostate cancer. These experiments showed the compound successfully blocked SOS1-to-Ras signaling and the proliferation of cancer cells.
Dr Zheng said one of the researchers’ next steps is to transform NSC-658497 into a drug that can be administered to a living organism so the team can begin testing the inhibitor in mouse models of different Rasopathies and cancers.
One of the targeted approaches the researchers plan to explore is whether NSC-658497 might be most promising in individuals who have a subset of disease in which SOS1 is significantly overexpressed or mutated. ![]()

Credit: NIH
A newly identified class of compounds recognize a key target in the Ras signaling pathway and could therefore prove useful in treating a range of malignancies, according to research published in Chemistry & Biology.
The lead compound, NSC-658497, targeted the catalytic activation of Ras by an enzyme called SOS1.
NSC-658497 blocked SOS1-mediated molecular signaling in the Ras pathway that causes rapid cell proliferation, tumor development, and cancer.
“While Ras pathway activation is a dominant event happening in many diseases, so far, the immediate signaling module of the Ras pathway has been difficult to target,” said study author Yi Zheng, PhD, of Cincinnati Children’s Hospital in Ohio.
“Most strategies for treatment have been geared toward hitting molecular effectors that are farther downstream. In this study, we have identified synthetic compounds that specifically recognize the catalytic pocket of SOS1 and demonstrated that they are effective inhibitors of Ras signaling in cells. This establishes a novel targeting approach for cancers and Rasopathies that is useful in developing therapeutics.”
Rasopathies include a group of 9 developmental syndromes that are caused by mutations in the Ras pathway (Noonan, LEOPARD, hereditary Gingival fibromatosis type 1, Capillary malformation-AV malformation, Neurofibromatosis type 1, Legius, Costello, Cardio-facio-cutaneous, and autoimmune lymphoproliferative syndromes).
Dysregulation of the Ras pathway (including its SOS1 catalytic activator) is also linked to a number of malignancies, such as breast, pancreatic, and cervical cancers, as well as leukemia.
To find compounds that could target the Ras pathway, Dr Zheng and his colleagues tested 30,000 synthetic molecular compounds in a database maintained by the National Cancer Institute.
The researchers looked for the compounds’ ability to dock with the catalytic site of SOS1, which led them to identify NSC-658497 and derivatives as lead candidates for the development of a prospective drug.
The team then tested NSC-658497 in cell lines of mouse fibroblasts and prostate cancer. These experiments showed the compound successfully blocked SOS1-to-Ras signaling and the proliferation of cancer cells.
Dr Zheng said one of the researchers’ next steps is to transform NSC-658497 into a drug that can be administered to a living organism so the team can begin testing the inhibitor in mouse models of different Rasopathies and cancers.
One of the targeted approaches the researchers plan to explore is whether NSC-658497 might be most promising in individuals who have a subset of disease in which SOS1 is significantly overexpressed or mutated. ![]()

Credit: NIH
A newly identified class of compounds recognize a key target in the Ras signaling pathway and could therefore prove useful in treating a range of malignancies, according to research published in Chemistry & Biology.
The lead compound, NSC-658497, targeted the catalytic activation of Ras by an enzyme called SOS1.
NSC-658497 blocked SOS1-mediated molecular signaling in the Ras pathway that causes rapid cell proliferation, tumor development, and cancer.
“While Ras pathway activation is a dominant event happening in many diseases, so far, the immediate signaling module of the Ras pathway has been difficult to target,” said study author Yi Zheng, PhD, of Cincinnati Children’s Hospital in Ohio.
“Most strategies for treatment have been geared toward hitting molecular effectors that are farther downstream. In this study, we have identified synthetic compounds that specifically recognize the catalytic pocket of SOS1 and demonstrated that they are effective inhibitors of Ras signaling in cells. This establishes a novel targeting approach for cancers and Rasopathies that is useful in developing therapeutics.”
Rasopathies include a group of 9 developmental syndromes that are caused by mutations in the Ras pathway (Noonan, LEOPARD, hereditary Gingival fibromatosis type 1, Capillary malformation-AV malformation, Neurofibromatosis type 1, Legius, Costello, Cardio-facio-cutaneous, and autoimmune lymphoproliferative syndromes).
Dysregulation of the Ras pathway (including its SOS1 catalytic activator) is also linked to a number of malignancies, such as breast, pancreatic, and cervical cancers, as well as leukemia.
To find compounds that could target the Ras pathway, Dr Zheng and his colleagues tested 30,000 synthetic molecular compounds in a database maintained by the National Cancer Institute.
The researchers looked for the compounds’ ability to dock with the catalytic site of SOS1, which led them to identify NSC-658497 and derivatives as lead candidates for the development of a prospective drug.
The team then tested NSC-658497 in cell lines of mouse fibroblasts and prostate cancer. These experiments showed the compound successfully blocked SOS1-to-Ras signaling and the proliferation of cancer cells.
Dr Zheng said one of the researchers’ next steps is to transform NSC-658497 into a drug that can be administered to a living organism so the team can begin testing the inhibitor in mouse models of different Rasopathies and cancers.
One of the targeted approaches the researchers plan to explore is whether NSC-658497 might be most promising in individuals who have a subset of disease in which SOS1 is significantly overexpressed or mutated. ![]()
Comparison of mice and men may lead to better use of mouse models

Credit: Aaron Logan
Scientists have long known that mice are not perfect models for studying conditions in humans, but new research reveals why certain processes and systems in
mice are so different from those in humans.
As part of the mouse ENCODE project, researchers discovered that a significant number of mouse genes do not behave like their human counterparts.
This suggests scientists will need to rethink at least some roles of the lab mouse as a model organism.
“There are a substantial number of mouse genes that are regulated in ways different from similar genes in humans,” said Bing Ren, PhD, of the University of California, San Diego.
“The differences are not random. They are clustered along certain pathways, such as in genes regulating the immune system.”
The findings, part of a series of related papers being published in Nature, Science, and other journals (see below), are derived from the ongoing mouse ENCODE (Encyclopedia of DNA Elements) project.
This multi-institution effort was launched in 2007 to build a comprehensive list of functional elements of the mouse genome. It complements the earlier human ENCODE project, which published its functional catalogue in 2012.
“Both the original human and mouse genome projects gave us the sequence of genetic letters that comprise each organism but no idea how they worked or worked together to create and sustain life,” Dr Ren said.
“The human ENCODE project was designed to answer some of those questions. The mouse ENCODE project is its complement. It’s intended to provide scientists with comprehensive annotation of what mouse genes do, information that may ultimately be used for human therapeutic purposes.”
Only half of human genomic DNA aligns to mouse genomic DNA. But protein-coding genes, which provide the actionable instructions to build a living organism, are more strongly conserved across the two species.
Mice and humans share approximately 70% of the same protein-coding gene sequences, though these genes constitute just 1.5% of their respective genomes.
Dr Ren said scientists had assumed that significant conservation would occur at the deeper level of gene regulation as well, that similar genes in humans and mice would be expressed in similar ways.
Using the same high throughput technologies applied in the human ENCODE project, he and his colleagues analyzed 100 different mouse cell types and tissues.
They found that, while much conservation did exist, the expression profiles of some distinct biological pathways in mouse samples diverged considerably from human samples.
Put another way, core genomic programs were largely conserved between the species, but genes and their underlying regulatory programs had changed significantly over time. Each species had evolved to find different ways to do some of the same things.
The findings are not entirely unexpected. Dr Ren said previous studies had documented rapidly evolving transcription factors in a handful of cell types and model organisms, but the ability to more systematically discern how humans and mice differ in genomic function marks an important milestone.
“One benefit is that, while mice have proved to be substantially different than humans in some ways, we now have a better idea of where exactly they are different, where we will need to take into account those differences, perhaps finding or developing a better model, and where the mouse continues to be a very good model indeed,” Dr Ren concluded.
Visit the following links for the mouse ENCODE papers published yesterday in Nature and Science:
A comparative encyclopedia of DNA elements in the mouse genome
Conservation of trans-acting circuitry during mammalian regulatory evolution
Principles of regulatory information conservation between mouse and human
Topologically associating domains are stable units of replication-timing regulation
Mouse regulatory DNA landscapes reveal global principles of cis-regulatory evolution
Related studies are set to appear in PNAS, Genome Research, Genome Biology, Nature Communications, and Blood. ![]()

Credit: Aaron Logan
Scientists have long known that mice are not perfect models for studying conditions in humans, but new research reveals why certain processes and systems in
mice are so different from those in humans.
As part of the mouse ENCODE project, researchers discovered that a significant number of mouse genes do not behave like their human counterparts.
This suggests scientists will need to rethink at least some roles of the lab mouse as a model organism.
“There are a substantial number of mouse genes that are regulated in ways different from similar genes in humans,” said Bing Ren, PhD, of the University of California, San Diego.
“The differences are not random. They are clustered along certain pathways, such as in genes regulating the immune system.”
The findings, part of a series of related papers being published in Nature, Science, and other journals (see below), are derived from the ongoing mouse ENCODE (Encyclopedia of DNA Elements) project.
This multi-institution effort was launched in 2007 to build a comprehensive list of functional elements of the mouse genome. It complements the earlier human ENCODE project, which published its functional catalogue in 2012.
“Both the original human and mouse genome projects gave us the sequence of genetic letters that comprise each organism but no idea how they worked or worked together to create and sustain life,” Dr Ren said.
“The human ENCODE project was designed to answer some of those questions. The mouse ENCODE project is its complement. It’s intended to provide scientists with comprehensive annotation of what mouse genes do, information that may ultimately be used for human therapeutic purposes.”
Only half of human genomic DNA aligns to mouse genomic DNA. But protein-coding genes, which provide the actionable instructions to build a living organism, are more strongly conserved across the two species.
Mice and humans share approximately 70% of the same protein-coding gene sequences, though these genes constitute just 1.5% of their respective genomes.
Dr Ren said scientists had assumed that significant conservation would occur at the deeper level of gene regulation as well, that similar genes in humans and mice would be expressed in similar ways.
Using the same high throughput technologies applied in the human ENCODE project, he and his colleagues analyzed 100 different mouse cell types and tissues.
They found that, while much conservation did exist, the expression profiles of some distinct biological pathways in mouse samples diverged considerably from human samples.
Put another way, core genomic programs were largely conserved between the species, but genes and their underlying regulatory programs had changed significantly over time. Each species had evolved to find different ways to do some of the same things.
The findings are not entirely unexpected. Dr Ren said previous studies had documented rapidly evolving transcription factors in a handful of cell types and model organisms, but the ability to more systematically discern how humans and mice differ in genomic function marks an important milestone.
“One benefit is that, while mice have proved to be substantially different than humans in some ways, we now have a better idea of where exactly they are different, where we will need to take into account those differences, perhaps finding or developing a better model, and where the mouse continues to be a very good model indeed,” Dr Ren concluded.
Visit the following links for the mouse ENCODE papers published yesterday in Nature and Science:
A comparative encyclopedia of DNA elements in the mouse genome
Conservation of trans-acting circuitry during mammalian regulatory evolution
Principles of regulatory information conservation between mouse and human
Topologically associating domains are stable units of replication-timing regulation
Mouse regulatory DNA landscapes reveal global principles of cis-regulatory evolution
Related studies are set to appear in PNAS, Genome Research, Genome Biology, Nature Communications, and Blood. ![]()

Credit: Aaron Logan
Scientists have long known that mice are not perfect models for studying conditions in humans, but new research reveals why certain processes and systems in
mice are so different from those in humans.
As part of the mouse ENCODE project, researchers discovered that a significant number of mouse genes do not behave like their human counterparts.
This suggests scientists will need to rethink at least some roles of the lab mouse as a model organism.
“There are a substantial number of mouse genes that are regulated in ways different from similar genes in humans,” said Bing Ren, PhD, of the University of California, San Diego.
“The differences are not random. They are clustered along certain pathways, such as in genes regulating the immune system.”
The findings, part of a series of related papers being published in Nature, Science, and other journals (see below), are derived from the ongoing mouse ENCODE (Encyclopedia of DNA Elements) project.
This multi-institution effort was launched in 2007 to build a comprehensive list of functional elements of the mouse genome. It complements the earlier human ENCODE project, which published its functional catalogue in 2012.
“Both the original human and mouse genome projects gave us the sequence of genetic letters that comprise each organism but no idea how they worked or worked together to create and sustain life,” Dr Ren said.
“The human ENCODE project was designed to answer some of those questions. The mouse ENCODE project is its complement. It’s intended to provide scientists with comprehensive annotation of what mouse genes do, information that may ultimately be used for human therapeutic purposes.”
Only half of human genomic DNA aligns to mouse genomic DNA. But protein-coding genes, which provide the actionable instructions to build a living organism, are more strongly conserved across the two species.
Mice and humans share approximately 70% of the same protein-coding gene sequences, though these genes constitute just 1.5% of their respective genomes.
Dr Ren said scientists had assumed that significant conservation would occur at the deeper level of gene regulation as well, that similar genes in humans and mice would be expressed in similar ways.
Using the same high throughput technologies applied in the human ENCODE project, he and his colleagues analyzed 100 different mouse cell types and tissues.
They found that, while much conservation did exist, the expression profiles of some distinct biological pathways in mouse samples diverged considerably from human samples.
Put another way, core genomic programs were largely conserved between the species, but genes and their underlying regulatory programs had changed significantly over time. Each species had evolved to find different ways to do some of the same things.
The findings are not entirely unexpected. Dr Ren said previous studies had documented rapidly evolving transcription factors in a handful of cell types and model organisms, but the ability to more systematically discern how humans and mice differ in genomic function marks an important milestone.
“One benefit is that, while mice have proved to be substantially different than humans in some ways, we now have a better idea of where exactly they are different, where we will need to take into account those differences, perhaps finding or developing a better model, and where the mouse continues to be a very good model indeed,” Dr Ren concluded.
Visit the following links for the mouse ENCODE papers published yesterday in Nature and Science:
A comparative encyclopedia of DNA elements in the mouse genome
Conservation of trans-acting circuitry during mammalian regulatory evolution
Principles of regulatory information conservation between mouse and human
Topologically associating domains are stable units of replication-timing regulation
Mouse regulatory DNA landscapes reveal global principles of cis-regulatory evolution
Related studies are set to appear in PNAS, Genome Research, Genome Biology, Nature Communications, and Blood. ![]()
Immunologist Herman Eisen dies at 96

Photo courtesy of MIT
Herman Eisen, MD, a respected immunologist, has died at the age of 96.
Over a 70-year career, Dr Eisen contributed a great deal to his own field and other fields of research.
He published work describing affinity maturation, clarified the basis for certain allergic reactions, and provided new insight into multiple myeloma and other cancers.
Dr Eisen was a professor emeritus of biology at the Massachusetts Institute of Technology (MIT) and a founding member of the MIT Center for Cancer Research (now the Koch Institute for Integrative Cancer Research).
He joined MIT in 1973 and retired in 1989, but only in the official sense. As a professor emeritus, he maintained an active lab and continued to research, publish, and advise students and postdocs at MIT until his passing.
Early years
Born in 1918 in Brooklyn, New York, Dr Eisen developed a keen interest in science at an early age, when a high school chemistry class helped frame his perception of the world as a collection of atoms and molecules.
Dr Eisen began premedical studies at New York University (NYU) in 1934, but halfway through his undergraduate career, he developed tuberculosis and left school. Though this kept him out of school for one year, the illness sparked a curiosity about the immune system that would endure for the rest of his life.
Dr Eisen returned to NYU to complete his bachelor’s degree, then enrolled at the university’s medical school. He graduated with an MD in 1943 and then worked as an assistant in the pathology department at the Columbia University College of Physicians and Surgeons before going back to NYU for his residency.
Research interests
Dr Eisen had a strong interest in basic science research, particularly in trying to better understand the body’s immune system. Though career options for physician-scientists had historically been limited, the federal government began to increase its funding of biomedical research through the National Institutes of Health (NIH) following World War II.
Seizing these new opportunities, Dr Eisen became one of the first recipients of an NIH fellowship, which supported his research on sulfonamide-induced antibodies at NYU. These investigations helped him and colleague Fred Karush, PhD, determine the number of antigen-binding sites on antibodies.
After his 2-year NIH fellowship, Dr Eisen worked briefly at the Sloan Kettering Institute before returning once again to NYU as a faculty member.
Inspired by the work of his recently deceased role model, Karl Landsteiner, MD, Dr Eisen studied immune reactions of the skin. In doing so, he clarified the basis for certain allergic responses and showed that only those chemicals capable of forming covalent bonds to skin proteins could cause a characteristic itchy rash.
In 1955, Washington University in St Louis recruited Dr Eisen to join the faculty of its School of Medicine. There, he served as dermatologist-in-chief for 5 years before moving to the Department of Microbiology to serve as chair.
While at Washington University, Dr Eisen published groundbreaking research in which he described affinity maturation: the process by which activated B cells produce antibodies with an increasingly higher affinity for invading pathogens after infection. This process is fundamental to the development of potent immune responses.
“Our understanding of affinity maturation begins with Herman’s papers,” said Arup K. Chakraborty, PhD, director of MIT’s Institute for Medical Engineering and Science.
“Understanding this evolutionary process is critical for vaccine design, and affinity maturation is also mimicked in countless academic laboratories and companies to design antibody-based therapies.”
Cancer research
In response to the National Cancer Act of 1971, MIT tasked Nobel Prize-winning biology professor Salvador Luria, MD, with establishing and leading a new MIT Center for Cancer Research. Wanting to include cancer immunology as a focus of this new center, Dr Luria approached Dr Eisen about joining as a founding faculty member.
Dr Eisen accepted the role and arrived at MIT in 1973 as a professor in the Department of Biology. He brought his immunology expertise to MIT’s new cancer center to study how cancer cells evade the body’s natural immune response.
Much of his work focused on studying myeloma tumors in mice and screening their associated proteins. He found that if he used myeloma proteins from one mouse to immunize other mice from the same strain, they were resistant when challenged with cancer cells.
Dr Eisen and his lab went on to study how CD8 T cells develop into cytotoxic T cells and long-lived memory T cells. Therapeutic vaccines that exploit CD8 responses have not yet been developed for humans.
Dr Eisen was working to understand and overcome the barriers to creating effective CD8 vaccines, and his research on the subject was of particular importance to the advancement of cancer immunology.
“Herman’s lifelong pursuit of science, even to the very last day of his life, has been an inspiration to many of us,” said Jianzhu Chen, PhD, of the Koch Institute. “He was a great human being with a great attitude and a clear mind. He will be missed greatly.”
Other colleagues remember Dr Eisen not only as a respected immunologist, but as a hardworking collaborator and a man of integrity. He continued to be an active scientist and had been working with Dr Chakraborty on a paper until his passing.
“Herman was a giant in the field of immunology, with many seminal discoveries,” Dr Chakraborty said. “He was also the kindest and most generous and moral person I have known. Until the end, he was working on scientific problems with junior colleagues and students who benefited from his wisdom. I am lucky to have worked with this great scientist and wonderful human being.”
Dr Eisen was elected to the American Academy of Arts and Sciences in 1965, the National Academy of Sciences in 1969, and the Institute of Medicine of the National Academies in 1974.
He received numerous other awards and honors throughout his career, including the Behring-Heidelberger Award from the American Association of Immunologists, an Outstanding Investigator Award from the National Cancer Institute, and the Lifetime Service Award from the American Association of Immunologists, of which he served as president from 1968 to 1969.
Dr Eisen passed away on November 2. He is survived by his wife Natalie and their children, Ellen, Jane, Jim, Tom, and Matthew, as well as 12 grandchildren. ![]()

Photo courtesy of MIT
Herman Eisen, MD, a respected immunologist, has died at the age of 96.
Over a 70-year career, Dr Eisen contributed a great deal to his own field and other fields of research.
He published work describing affinity maturation, clarified the basis for certain allergic reactions, and provided new insight into multiple myeloma and other cancers.
Dr Eisen was a professor emeritus of biology at the Massachusetts Institute of Technology (MIT) and a founding member of the MIT Center for Cancer Research (now the Koch Institute for Integrative Cancer Research).
He joined MIT in 1973 and retired in 1989, but only in the official sense. As a professor emeritus, he maintained an active lab and continued to research, publish, and advise students and postdocs at MIT until his passing.
Early years
Born in 1918 in Brooklyn, New York, Dr Eisen developed a keen interest in science at an early age, when a high school chemistry class helped frame his perception of the world as a collection of atoms and molecules.
Dr Eisen began premedical studies at New York University (NYU) in 1934, but halfway through his undergraduate career, he developed tuberculosis and left school. Though this kept him out of school for one year, the illness sparked a curiosity about the immune system that would endure for the rest of his life.
Dr Eisen returned to NYU to complete his bachelor’s degree, then enrolled at the university’s medical school. He graduated with an MD in 1943 and then worked as an assistant in the pathology department at the Columbia University College of Physicians and Surgeons before going back to NYU for his residency.
Research interests
Dr Eisen had a strong interest in basic science research, particularly in trying to better understand the body’s immune system. Though career options for physician-scientists had historically been limited, the federal government began to increase its funding of biomedical research through the National Institutes of Health (NIH) following World War II.
Seizing these new opportunities, Dr Eisen became one of the first recipients of an NIH fellowship, which supported his research on sulfonamide-induced antibodies at NYU. These investigations helped him and colleague Fred Karush, PhD, determine the number of antigen-binding sites on antibodies.
After his 2-year NIH fellowship, Dr Eisen worked briefly at the Sloan Kettering Institute before returning once again to NYU as a faculty member.
Inspired by the work of his recently deceased role model, Karl Landsteiner, MD, Dr Eisen studied immune reactions of the skin. In doing so, he clarified the basis for certain allergic responses and showed that only those chemicals capable of forming covalent bonds to skin proteins could cause a characteristic itchy rash.
In 1955, Washington University in St Louis recruited Dr Eisen to join the faculty of its School of Medicine. There, he served as dermatologist-in-chief for 5 years before moving to the Department of Microbiology to serve as chair.
While at Washington University, Dr Eisen published groundbreaking research in which he described affinity maturation: the process by which activated B cells produce antibodies with an increasingly higher affinity for invading pathogens after infection. This process is fundamental to the development of potent immune responses.
“Our understanding of affinity maturation begins with Herman’s papers,” said Arup K. Chakraborty, PhD, director of MIT’s Institute for Medical Engineering and Science.
“Understanding this evolutionary process is critical for vaccine design, and affinity maturation is also mimicked in countless academic laboratories and companies to design antibody-based therapies.”
Cancer research
In response to the National Cancer Act of 1971, MIT tasked Nobel Prize-winning biology professor Salvador Luria, MD, with establishing and leading a new MIT Center for Cancer Research. Wanting to include cancer immunology as a focus of this new center, Dr Luria approached Dr Eisen about joining as a founding faculty member.
Dr Eisen accepted the role and arrived at MIT in 1973 as a professor in the Department of Biology. He brought his immunology expertise to MIT’s new cancer center to study how cancer cells evade the body’s natural immune response.
Much of his work focused on studying myeloma tumors in mice and screening their associated proteins. He found that if he used myeloma proteins from one mouse to immunize other mice from the same strain, they were resistant when challenged with cancer cells.
Dr Eisen and his lab went on to study how CD8 T cells develop into cytotoxic T cells and long-lived memory T cells. Therapeutic vaccines that exploit CD8 responses have not yet been developed for humans.
Dr Eisen was working to understand and overcome the barriers to creating effective CD8 vaccines, and his research on the subject was of particular importance to the advancement of cancer immunology.
“Herman’s lifelong pursuit of science, even to the very last day of his life, has been an inspiration to many of us,” said Jianzhu Chen, PhD, of the Koch Institute. “He was a great human being with a great attitude and a clear mind. He will be missed greatly.”
Other colleagues remember Dr Eisen not only as a respected immunologist, but as a hardworking collaborator and a man of integrity. He continued to be an active scientist and had been working with Dr Chakraborty on a paper until his passing.
“Herman was a giant in the field of immunology, with many seminal discoveries,” Dr Chakraborty said. “He was also the kindest and most generous and moral person I have known. Until the end, he was working on scientific problems with junior colleagues and students who benefited from his wisdom. I am lucky to have worked with this great scientist and wonderful human being.”
Dr Eisen was elected to the American Academy of Arts and Sciences in 1965, the National Academy of Sciences in 1969, and the Institute of Medicine of the National Academies in 1974.
He received numerous other awards and honors throughout his career, including the Behring-Heidelberger Award from the American Association of Immunologists, an Outstanding Investigator Award from the National Cancer Institute, and the Lifetime Service Award from the American Association of Immunologists, of which he served as president from 1968 to 1969.
Dr Eisen passed away on November 2. He is survived by his wife Natalie and their children, Ellen, Jane, Jim, Tom, and Matthew, as well as 12 grandchildren. ![]()

Photo courtesy of MIT
Herman Eisen, MD, a respected immunologist, has died at the age of 96.
Over a 70-year career, Dr Eisen contributed a great deal to his own field and other fields of research.
He published work describing affinity maturation, clarified the basis for certain allergic reactions, and provided new insight into multiple myeloma and other cancers.
Dr Eisen was a professor emeritus of biology at the Massachusetts Institute of Technology (MIT) and a founding member of the MIT Center for Cancer Research (now the Koch Institute for Integrative Cancer Research).
He joined MIT in 1973 and retired in 1989, but only in the official sense. As a professor emeritus, he maintained an active lab and continued to research, publish, and advise students and postdocs at MIT until his passing.
Early years
Born in 1918 in Brooklyn, New York, Dr Eisen developed a keen interest in science at an early age, when a high school chemistry class helped frame his perception of the world as a collection of atoms and molecules.
Dr Eisen began premedical studies at New York University (NYU) in 1934, but halfway through his undergraduate career, he developed tuberculosis and left school. Though this kept him out of school for one year, the illness sparked a curiosity about the immune system that would endure for the rest of his life.
Dr Eisen returned to NYU to complete his bachelor’s degree, then enrolled at the university’s medical school. He graduated with an MD in 1943 and then worked as an assistant in the pathology department at the Columbia University College of Physicians and Surgeons before going back to NYU for his residency.
Research interests
Dr Eisen had a strong interest in basic science research, particularly in trying to better understand the body’s immune system. Though career options for physician-scientists had historically been limited, the federal government began to increase its funding of biomedical research through the National Institutes of Health (NIH) following World War II.
Seizing these new opportunities, Dr Eisen became one of the first recipients of an NIH fellowship, which supported his research on sulfonamide-induced antibodies at NYU. These investigations helped him and colleague Fred Karush, PhD, determine the number of antigen-binding sites on antibodies.
After his 2-year NIH fellowship, Dr Eisen worked briefly at the Sloan Kettering Institute before returning once again to NYU as a faculty member.
Inspired by the work of his recently deceased role model, Karl Landsteiner, MD, Dr Eisen studied immune reactions of the skin. In doing so, he clarified the basis for certain allergic responses and showed that only those chemicals capable of forming covalent bonds to skin proteins could cause a characteristic itchy rash.
In 1955, Washington University in St Louis recruited Dr Eisen to join the faculty of its School of Medicine. There, he served as dermatologist-in-chief for 5 years before moving to the Department of Microbiology to serve as chair.
While at Washington University, Dr Eisen published groundbreaking research in which he described affinity maturation: the process by which activated B cells produce antibodies with an increasingly higher affinity for invading pathogens after infection. This process is fundamental to the development of potent immune responses.
“Our understanding of affinity maturation begins with Herman’s papers,” said Arup K. Chakraborty, PhD, director of MIT’s Institute for Medical Engineering and Science.
“Understanding this evolutionary process is critical for vaccine design, and affinity maturation is also mimicked in countless academic laboratories and companies to design antibody-based therapies.”
Cancer research
In response to the National Cancer Act of 1971, MIT tasked Nobel Prize-winning biology professor Salvador Luria, MD, with establishing and leading a new MIT Center for Cancer Research. Wanting to include cancer immunology as a focus of this new center, Dr Luria approached Dr Eisen about joining as a founding faculty member.
Dr Eisen accepted the role and arrived at MIT in 1973 as a professor in the Department of Biology. He brought his immunology expertise to MIT’s new cancer center to study how cancer cells evade the body’s natural immune response.
Much of his work focused on studying myeloma tumors in mice and screening their associated proteins. He found that if he used myeloma proteins from one mouse to immunize other mice from the same strain, they were resistant when challenged with cancer cells.
Dr Eisen and his lab went on to study how CD8 T cells develop into cytotoxic T cells and long-lived memory T cells. Therapeutic vaccines that exploit CD8 responses have not yet been developed for humans.
Dr Eisen was working to understand and overcome the barriers to creating effective CD8 vaccines, and his research on the subject was of particular importance to the advancement of cancer immunology.
“Herman’s lifelong pursuit of science, even to the very last day of his life, has been an inspiration to many of us,” said Jianzhu Chen, PhD, of the Koch Institute. “He was a great human being with a great attitude and a clear mind. He will be missed greatly.”
Other colleagues remember Dr Eisen not only as a respected immunologist, but as a hardworking collaborator and a man of integrity. He continued to be an active scientist and had been working with Dr Chakraborty on a paper until his passing.
“Herman was a giant in the field of immunology, with many seminal discoveries,” Dr Chakraborty said. “He was also the kindest and most generous and moral person I have known. Until the end, he was working on scientific problems with junior colleagues and students who benefited from his wisdom. I am lucky to have worked with this great scientist and wonderful human being.”
Dr Eisen was elected to the American Academy of Arts and Sciences in 1965, the National Academy of Sciences in 1969, and the Institute of Medicine of the National Academies in 1974.
He received numerous other awards and honors throughout his career, including the Behring-Heidelberger Award from the American Association of Immunologists, an Outstanding Investigator Award from the National Cancer Institute, and the Lifetime Service Award from the American Association of Immunologists, of which he served as president from 1968 to 1969.
Dr Eisen passed away on November 2. He is survived by his wife Natalie and their children, Ellen, Jane, Jim, Tom, and Matthew, as well as 12 grandchildren. ![]()
Test detects bloodstream infections faster

Credit: Graham Colm
A new test can detect bloodstream infections with “unprecedented” speed and accuracy, according to researchers.
The group developed a test called Integrated Comprehensive Droplet Digital Detection (IC 3D).
And experiments showed that IC 3D can detect bacteria in milliliters of blood with single-cell sensitivity in 1.5 to 4 hours, with no cell culture necessary.
The researchers described this test in Nature Communications.
“We are extremely excited about this technology because it addresses a long-standing unmet medical need in the field,” said study author Weian Zhao, PhD, of the University of California Irvine (UCI).
“As a platform technology, it may have many applications in detecting extremely low-abundance biomarkers in other areas, such as cancers, HIV, and, most notably, Ebola.”
Worldwide, more than 2 million people a year get antibiotic-resistant blood infections, and 23,000 of them die, according to the US Centers for Disease Control & Prevention. This high mortality rate is due, in part, to the inability to diagnose and treat patients in the early stages.
Recent molecular diagnostic methods can reduce the assay time to hours but may not be sensitive enough to detect bacteria that occur at low concentrations in blood.
The IC 3D technology differs from other diagnostic techniques in that it converts blood samples directly into billions of very small droplets. Fluorescent DNA sensor solution infused into the droplets detects those with bacterial markers, lighting them up with an intense fluorescent signal.
Dr Zhao said that separating the samples into so many small droplets minimizes the interference of other components in blood, making it possible to directly detect target bacteria without the purification typically required in conventional assays.
To identify bacteria-containing droplets among billions of others in a timely fashion, Dr Zhao and his colleagues incorporated a 3-dimensional particle counter developed by UCI biomedical engineer Enrico Gratton, PhD, and his colleagues that tags fluorescent particles within several minutes.
“The IC 3D instrument is designed to read a large volume in each measurement, to speed up diagnosis,” Dr Gratton said. “Importantly, using this technique, we can detect a positive hit with very high confidence.”
The researchers reported that IC 3D provided absolute quantification of stock and clinical isolates of Escherichia coli at a wide range of concentrations, from 1 to 10,000 bacteria per mL, in 1.5 to 4 hours.
A UCI spinoff, Velox Biosystems, is now developing the IC 3D technology. ![]()

Credit: Graham Colm
A new test can detect bloodstream infections with “unprecedented” speed and accuracy, according to researchers.
The group developed a test called Integrated Comprehensive Droplet Digital Detection (IC 3D).
And experiments showed that IC 3D can detect bacteria in milliliters of blood with single-cell sensitivity in 1.5 to 4 hours, with no cell culture necessary.
The researchers described this test in Nature Communications.
“We are extremely excited about this technology because it addresses a long-standing unmet medical need in the field,” said study author Weian Zhao, PhD, of the University of California Irvine (UCI).
“As a platform technology, it may have many applications in detecting extremely low-abundance biomarkers in other areas, such as cancers, HIV, and, most notably, Ebola.”
Worldwide, more than 2 million people a year get antibiotic-resistant blood infections, and 23,000 of them die, according to the US Centers for Disease Control & Prevention. This high mortality rate is due, in part, to the inability to diagnose and treat patients in the early stages.
Recent molecular diagnostic methods can reduce the assay time to hours but may not be sensitive enough to detect bacteria that occur at low concentrations in blood.
The IC 3D technology differs from other diagnostic techniques in that it converts blood samples directly into billions of very small droplets. Fluorescent DNA sensor solution infused into the droplets detects those with bacterial markers, lighting them up with an intense fluorescent signal.
Dr Zhao said that separating the samples into so many small droplets minimizes the interference of other components in blood, making it possible to directly detect target bacteria without the purification typically required in conventional assays.
To identify bacteria-containing droplets among billions of others in a timely fashion, Dr Zhao and his colleagues incorporated a 3-dimensional particle counter developed by UCI biomedical engineer Enrico Gratton, PhD, and his colleagues that tags fluorescent particles within several minutes.
“The IC 3D instrument is designed to read a large volume in each measurement, to speed up diagnosis,” Dr Gratton said. “Importantly, using this technique, we can detect a positive hit with very high confidence.”
The researchers reported that IC 3D provided absolute quantification of stock and clinical isolates of Escherichia coli at a wide range of concentrations, from 1 to 10,000 bacteria per mL, in 1.5 to 4 hours.
A UCI spinoff, Velox Biosystems, is now developing the IC 3D technology. ![]()

Credit: Graham Colm
A new test can detect bloodstream infections with “unprecedented” speed and accuracy, according to researchers.
The group developed a test called Integrated Comprehensive Droplet Digital Detection (IC 3D).
And experiments showed that IC 3D can detect bacteria in milliliters of blood with single-cell sensitivity in 1.5 to 4 hours, with no cell culture necessary.
The researchers described this test in Nature Communications.
“We are extremely excited about this technology because it addresses a long-standing unmet medical need in the field,” said study author Weian Zhao, PhD, of the University of California Irvine (UCI).
“As a platform technology, it may have many applications in detecting extremely low-abundance biomarkers in other areas, such as cancers, HIV, and, most notably, Ebola.”
Worldwide, more than 2 million people a year get antibiotic-resistant blood infections, and 23,000 of them die, according to the US Centers for Disease Control & Prevention. This high mortality rate is due, in part, to the inability to diagnose and treat patients in the early stages.
Recent molecular diagnostic methods can reduce the assay time to hours but may not be sensitive enough to detect bacteria that occur at low concentrations in blood.
The IC 3D technology differs from other diagnostic techniques in that it converts blood samples directly into billions of very small droplets. Fluorescent DNA sensor solution infused into the droplets detects those with bacterial markers, lighting them up with an intense fluorescent signal.
Dr Zhao said that separating the samples into so many small droplets minimizes the interference of other components in blood, making it possible to directly detect target bacteria without the purification typically required in conventional assays.
To identify bacteria-containing droplets among billions of others in a timely fashion, Dr Zhao and his colleagues incorporated a 3-dimensional particle counter developed by UCI biomedical engineer Enrico Gratton, PhD, and his colleagues that tags fluorescent particles within several minutes.
“The IC 3D instrument is designed to read a large volume in each measurement, to speed up diagnosis,” Dr Gratton said. “Importantly, using this technique, we can detect a positive hit with very high confidence.”
The researchers reported that IC 3D provided absolute quantification of stock and clinical isolates of Escherichia coli at a wide range of concentrations, from 1 to 10,000 bacteria per mL, in 1.5 to 4 hours.
A UCI spinoff, Velox Biosystems, is now developing the IC 3D technology. ![]()
How ‘urban’ mosquitoes transmit malaria
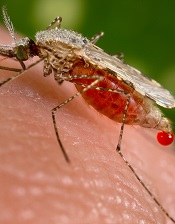
Credit: CDC
Researchers believe that by analyzing the genome of a mosquito species, they have discovered how that mosquito evolves to withstand a variety of environmental conditions.
The results, published in Genome Biology, provide a better understanding of Anopheles stephensi, a common carrier of malaria in urban environments.
“Anopheles stephensi is emerging as a model mosquito species for genetic and molecular studies,” said Zhijian Jake Tu, PhD, of Virginia Tech in Blacksburg.
He and his colleagues believe their genome map of An stephensi will be an important tool for scientists to identify potential targets for mosquito control. In addition, studies of immunity genes can provide insight into mosquito biology and mosquito-parasite interactions.
“Genome mapping of Anopheles stephensi revealed genetic differences between it and a species especially dangerous for transmitting malaria in Africa, Anopheles gambiae,” said Igor Sharakhov, PhD, also of Virginia Tech.
“This tells us that the sex chromosome is especially prone to mutations that flip chromosomal segments, which, in turn, may promote new, evolved species.”
The researchers assembled more than 92% of the An stephensi genome, and physical mapping assigned 62% of the genome onto chromosomes.
When the team compared An stephensi and An gambiae, they discovered the rate of gene order reshuffling on the Anopheles X chromosome was 3 times higher than that on the autosomes.
An stephensi had more repeat-rich heterochromatin in pericentric regions than An gambiae but fewer repetitive sequences in chromosome arms.
The researchers also identified Y-chromosome contigs and BACs, which represent the most abundant set of Y sequences in any Anopheles species.
Lastly, the team noted that RNA-sequencing and studies of immunity genes provided new insights into mosquito biology and mosquito-parasite interactions.
For instance, FKBP12, a protein that interacts with TOR and TGF-β signaling pathways, showed abundant mRNA expression in a wide range of tissues. This information could help improve our understanding of TOR and TGF-β signaling in mosquitoes. ![]()

Credit: CDC
Researchers believe that by analyzing the genome of a mosquito species, they have discovered how that mosquito evolves to withstand a variety of environmental conditions.
The results, published in Genome Biology, provide a better understanding of Anopheles stephensi, a common carrier of malaria in urban environments.
“Anopheles stephensi is emerging as a model mosquito species for genetic and molecular studies,” said Zhijian Jake Tu, PhD, of Virginia Tech in Blacksburg.
He and his colleagues believe their genome map of An stephensi will be an important tool for scientists to identify potential targets for mosquito control. In addition, studies of immunity genes can provide insight into mosquito biology and mosquito-parasite interactions.
“Genome mapping of Anopheles stephensi revealed genetic differences between it and a species especially dangerous for transmitting malaria in Africa, Anopheles gambiae,” said Igor Sharakhov, PhD, also of Virginia Tech.
“This tells us that the sex chromosome is especially prone to mutations that flip chromosomal segments, which, in turn, may promote new, evolved species.”
The researchers assembled more than 92% of the An stephensi genome, and physical mapping assigned 62% of the genome onto chromosomes.
When the team compared An stephensi and An gambiae, they discovered the rate of gene order reshuffling on the Anopheles X chromosome was 3 times higher than that on the autosomes.
An stephensi had more repeat-rich heterochromatin in pericentric regions than An gambiae but fewer repetitive sequences in chromosome arms.
The researchers also identified Y-chromosome contigs and BACs, which represent the most abundant set of Y sequences in any Anopheles species.
Lastly, the team noted that RNA-sequencing and studies of immunity genes provided new insights into mosquito biology and mosquito-parasite interactions.
For instance, FKBP12, a protein that interacts with TOR and TGF-β signaling pathways, showed abundant mRNA expression in a wide range of tissues. This information could help improve our understanding of TOR and TGF-β signaling in mosquitoes. ![]()

Credit: CDC
Researchers believe that by analyzing the genome of a mosquito species, they have discovered how that mosquito evolves to withstand a variety of environmental conditions.
The results, published in Genome Biology, provide a better understanding of Anopheles stephensi, a common carrier of malaria in urban environments.
“Anopheles stephensi is emerging as a model mosquito species for genetic and molecular studies,” said Zhijian Jake Tu, PhD, of Virginia Tech in Blacksburg.
He and his colleagues believe their genome map of An stephensi will be an important tool for scientists to identify potential targets for mosquito control. In addition, studies of immunity genes can provide insight into mosquito biology and mosquito-parasite interactions.
“Genome mapping of Anopheles stephensi revealed genetic differences between it and a species especially dangerous for transmitting malaria in Africa, Anopheles gambiae,” said Igor Sharakhov, PhD, also of Virginia Tech.
“This tells us that the sex chromosome is especially prone to mutations that flip chromosomal segments, which, in turn, may promote new, evolved species.”
The researchers assembled more than 92% of the An stephensi genome, and physical mapping assigned 62% of the genome onto chromosomes.
When the team compared An stephensi and An gambiae, they discovered the rate of gene order reshuffling on the Anopheles X chromosome was 3 times higher than that on the autosomes.
An stephensi had more repeat-rich heterochromatin in pericentric regions than An gambiae but fewer repetitive sequences in chromosome arms.
The researchers also identified Y-chromosome contigs and BACs, which represent the most abundant set of Y sequences in any Anopheles species.
Lastly, the team noted that RNA-sequencing and studies of immunity genes provided new insights into mosquito biology and mosquito-parasite interactions.
For instance, FKBP12, a protein that interacts with TOR and TGF-β signaling pathways, showed abundant mRNA expression in a wide range of tissues. This information could help improve our understanding of TOR and TGF-β signaling in mosquitoes. ![]()
Sharing research with public prompts more citations

Credit: Rhoda Baer
Academic researchers who talk to the press and use social media are more likely than their less communicative peers to have their work cited, a new study suggests.
The research revealed a connection between h-index—a measure of the quality of a researcher’s work and influence—and whether the scientists interact with reporters and get mentioned on Twitter.
The results appear in Journalism & Mass Communications Quarterly.
“I’ve been in science communication for a while now, and I am really seeing a change—especially among the younger scientists—in their willingness to share their work,” said study author Dominique Brossard, PhD, of the University of Wisconsin-Madison.
Attention from reporters is good news for h-index, Dr Brossard noted. But couple that with attention on Twitter, and you see a more pronounced spike in reputation.
“If you talk to reporters and you tweet about your research, your work is more likely to be cited than people who do one or the other,” she said.
That sort of activity hasn’t always been encouraged, Dr Brossard pointed out. Any distraction from a researcher’s work can draw criticism as a waste of a precious resource. But Dr Brossard hopes a new understanding of the relationship between research and communicating with the public can change that.
“What this shows us is that sharing your science with the public is not hurting the science by stealing time,” she said. “If the goal is to encourage people, ultimately, to be productive scientists, and if directors of labs are discouraging people from engaging in this activity, they’re actually hurting the science itself. Because people who do this are cited more often in scientific journals, [and] they’re making science accessible to broader audiences at the same time.”
Social media use is rising in other professional circles as well, according to Michael Xenos, PhD, also of the University of Wisconsin-Madison.
“As in other areas, such as politics for example, social media was once met with skepticism but is increasingly part of the culture,” he said. “Just like it became the norm there, our research shows it may one day become the norm in science.”
Even if you flip the connection between social media attention and h-index on its head, it’s still worth taking to heart, according to the researchers.
“The counter argument is that it may be just the other way around—that it may just be the big names that get mentions,” said study author Dietram A. Scheufele, PhD, also of the University of Wisconsin-Madison.
“But then, the lesson should be that the most successful people in your field are also the ones that are good at getting outside the ivory tower. That should be something to emulate.” ![]()

Credit: Rhoda Baer
Academic researchers who talk to the press and use social media are more likely than their less communicative peers to have their work cited, a new study suggests.
The research revealed a connection between h-index—a measure of the quality of a researcher’s work and influence—and whether the scientists interact with reporters and get mentioned on Twitter.
The results appear in Journalism & Mass Communications Quarterly.
“I’ve been in science communication for a while now, and I am really seeing a change—especially among the younger scientists—in their willingness to share their work,” said study author Dominique Brossard, PhD, of the University of Wisconsin-Madison.
Attention from reporters is good news for h-index, Dr Brossard noted. But couple that with attention on Twitter, and you see a more pronounced spike in reputation.
“If you talk to reporters and you tweet about your research, your work is more likely to be cited than people who do one or the other,” she said.
That sort of activity hasn’t always been encouraged, Dr Brossard pointed out. Any distraction from a researcher’s work can draw criticism as a waste of a precious resource. But Dr Brossard hopes a new understanding of the relationship between research and communicating with the public can change that.
“What this shows us is that sharing your science with the public is not hurting the science by stealing time,” she said. “If the goal is to encourage people, ultimately, to be productive scientists, and if directors of labs are discouraging people from engaging in this activity, they’re actually hurting the science itself. Because people who do this are cited more often in scientific journals, [and] they’re making science accessible to broader audiences at the same time.”
Social media use is rising in other professional circles as well, according to Michael Xenos, PhD, also of the University of Wisconsin-Madison.
“As in other areas, such as politics for example, social media was once met with skepticism but is increasingly part of the culture,” he said. “Just like it became the norm there, our research shows it may one day become the norm in science.”
Even if you flip the connection between social media attention and h-index on its head, it’s still worth taking to heart, according to the researchers.
“The counter argument is that it may be just the other way around—that it may just be the big names that get mentions,” said study author Dietram A. Scheufele, PhD, also of the University of Wisconsin-Madison.
“But then, the lesson should be that the most successful people in your field are also the ones that are good at getting outside the ivory tower. That should be something to emulate.” ![]()

Credit: Rhoda Baer
Academic researchers who talk to the press and use social media are more likely than their less communicative peers to have their work cited, a new study suggests.
The research revealed a connection between h-index—a measure of the quality of a researcher’s work and influence—and whether the scientists interact with reporters and get mentioned on Twitter.
The results appear in Journalism & Mass Communications Quarterly.
“I’ve been in science communication for a while now, and I am really seeing a change—especially among the younger scientists—in their willingness to share their work,” said study author Dominique Brossard, PhD, of the University of Wisconsin-Madison.
Attention from reporters is good news for h-index, Dr Brossard noted. But couple that with attention on Twitter, and you see a more pronounced spike in reputation.
“If you talk to reporters and you tweet about your research, your work is more likely to be cited than people who do one or the other,” she said.
That sort of activity hasn’t always been encouraged, Dr Brossard pointed out. Any distraction from a researcher’s work can draw criticism as a waste of a precious resource. But Dr Brossard hopes a new understanding of the relationship between research and communicating with the public can change that.
“What this shows us is that sharing your science with the public is not hurting the science by stealing time,” she said. “If the goal is to encourage people, ultimately, to be productive scientists, and if directors of labs are discouraging people from engaging in this activity, they’re actually hurting the science itself. Because people who do this are cited more often in scientific journals, [and] they’re making science accessible to broader audiences at the same time.”
Social media use is rising in other professional circles as well, according to Michael Xenos, PhD, also of the University of Wisconsin-Madison.
“As in other areas, such as politics for example, social media was once met with skepticism but is increasingly part of the culture,” he said. “Just like it became the norm there, our research shows it may one day become the norm in science.”
Even if you flip the connection between social media attention and h-index on its head, it’s still worth taking to heart, according to the researchers.
“The counter argument is that it may be just the other way around—that it may just be the big names that get mentions,” said study author Dietram A. Scheufele, PhD, also of the University of Wisconsin-Madison.
“But then, the lesson should be that the most successful people in your field are also the ones that are good at getting outside the ivory tower. That should be something to emulate.” ![]()
Hospice cuts cost and use of care for cancer patients

Credit: CDC
Patients with advanced cancer receive less aggressive care and have lower healthcare costs during their last year of life if they use hospice care, according to research published in JAMA.
Patients who entered hospice had significantly lower rates of hospitalization, intensive care unit admissions, and invasive procedures, compared to patients who did not enter hospice.
Furthermore, patients who chose hospice were about 5 times less likely to die in hospitals and nursing homes.
“Our study shows very clearly that hospice matters,” said Ziad Obermeyer, MD, of Brigham and Women’s Hospital in Boston.
“Hospice and non-hospice patients had very similar patterns of healthcare utilization right up until the week of hospice enrollment. Then, the care started to look very different. Patients who didn’t enroll in hospice ended up with far more aggressive care in their last year of life, most of it related to acute complications like infections and organ failure, and not directly related to their cancer diagnosis.”
To conduct this study, Dr Obermeyer and his colleagues used data from Medicare beneficiaries with poor-prognosis cancers, including hematologic malignancies. The study included a nationally representative 20% sample of Medicare fee-for-service beneficiaries who died in 2011.
Among 86,851 patients, 51,924 (60%) entered hospice before death. Matching patients based on various criteria produced hospice and non-hospice groups, each with 18,165 patients. The median hospice duration was 11 days.
The researchers found that non-hospice patients had significantly greater healthcare utilization, largely for acute conditions not directly related to cancer.
This included rates of hospitalization (65% vs 42%), intensive care unit admissions (36% vs 15%), invasive procedures (51% vs 27%), and death in a hospital or nursing facility (74% vs 14%).
The costs of care for hospice and non-hospice patients were not significantly different before hospice care began. But they diverged sharply thereafter, contributing to a significant difference in total costs of $8697 over the last year of life—$71,517 for non-hospice patients and $62,819 for hospice patients.
“These findings highlight the importance of honest discussions between doctors and patients about our patients’ goals of their care at the end of life, relating to treatment decisions and quality of life,” Dr Obermeyer said. “This is of particular importance now, in light of the ongoing policy discussions around reimbursing providers for advance-care planning.” ![]()

Credit: CDC
Patients with advanced cancer receive less aggressive care and have lower healthcare costs during their last year of life if they use hospice care, according to research published in JAMA.
Patients who entered hospice had significantly lower rates of hospitalization, intensive care unit admissions, and invasive procedures, compared to patients who did not enter hospice.
Furthermore, patients who chose hospice were about 5 times less likely to die in hospitals and nursing homes.
“Our study shows very clearly that hospice matters,” said Ziad Obermeyer, MD, of Brigham and Women’s Hospital in Boston.
“Hospice and non-hospice patients had very similar patterns of healthcare utilization right up until the week of hospice enrollment. Then, the care started to look very different. Patients who didn’t enroll in hospice ended up with far more aggressive care in their last year of life, most of it related to acute complications like infections and organ failure, and not directly related to their cancer diagnosis.”
To conduct this study, Dr Obermeyer and his colleagues used data from Medicare beneficiaries with poor-prognosis cancers, including hematologic malignancies. The study included a nationally representative 20% sample of Medicare fee-for-service beneficiaries who died in 2011.
Among 86,851 patients, 51,924 (60%) entered hospice before death. Matching patients based on various criteria produced hospice and non-hospice groups, each with 18,165 patients. The median hospice duration was 11 days.
The researchers found that non-hospice patients had significantly greater healthcare utilization, largely for acute conditions not directly related to cancer.
This included rates of hospitalization (65% vs 42%), intensive care unit admissions (36% vs 15%), invasive procedures (51% vs 27%), and death in a hospital or nursing facility (74% vs 14%).
The costs of care for hospice and non-hospice patients were not significantly different before hospice care began. But they diverged sharply thereafter, contributing to a significant difference in total costs of $8697 over the last year of life—$71,517 for non-hospice patients and $62,819 for hospice patients.
“These findings highlight the importance of honest discussions between doctors and patients about our patients’ goals of their care at the end of life, relating to treatment decisions and quality of life,” Dr Obermeyer said. “This is of particular importance now, in light of the ongoing policy discussions around reimbursing providers for advance-care planning.” ![]()

Credit: CDC
Patients with advanced cancer receive less aggressive care and have lower healthcare costs during their last year of life if they use hospice care, according to research published in JAMA.
Patients who entered hospice had significantly lower rates of hospitalization, intensive care unit admissions, and invasive procedures, compared to patients who did not enter hospice.
Furthermore, patients who chose hospice were about 5 times less likely to die in hospitals and nursing homes.
“Our study shows very clearly that hospice matters,” said Ziad Obermeyer, MD, of Brigham and Women’s Hospital in Boston.
“Hospice and non-hospice patients had very similar patterns of healthcare utilization right up until the week of hospice enrollment. Then, the care started to look very different. Patients who didn’t enroll in hospice ended up with far more aggressive care in their last year of life, most of it related to acute complications like infections and organ failure, and not directly related to their cancer diagnosis.”
To conduct this study, Dr Obermeyer and his colleagues used data from Medicare beneficiaries with poor-prognosis cancers, including hematologic malignancies. The study included a nationally representative 20% sample of Medicare fee-for-service beneficiaries who died in 2011.
Among 86,851 patients, 51,924 (60%) entered hospice before death. Matching patients based on various criteria produced hospice and non-hospice groups, each with 18,165 patients. The median hospice duration was 11 days.
The researchers found that non-hospice patients had significantly greater healthcare utilization, largely for acute conditions not directly related to cancer.
This included rates of hospitalization (65% vs 42%), intensive care unit admissions (36% vs 15%), invasive procedures (51% vs 27%), and death in a hospital or nursing facility (74% vs 14%).
The costs of care for hospice and non-hospice patients were not significantly different before hospice care began. But they diverged sharply thereafter, contributing to a significant difference in total costs of $8697 over the last year of life—$71,517 for non-hospice patients and $62,819 for hospice patients.
“These findings highlight the importance of honest discussions between doctors and patients about our patients’ goals of their care at the end of life, relating to treatment decisions and quality of life,” Dr Obermeyer said. “This is of particular importance now, in light of the ongoing policy discussions around reimbursing providers for advance-care planning.”
NICE supports use of catheter-positioning device

The UK’s National Institute for Health and Care Excellence (NICE) has opened consultation on a draft guidance about a device designed to help healthcare professionals correctly place peripherally inserted central catheters
(PICCs).
The draft guidance supports using the Sherlock 3CG Tip Confirmation System for placing PICCs.
The standard procedure for placing PICCs is blind insertion, followed by a chest X-ray to check the catheter’s position.
In some cases, fluoroscopy is used instead of standard X-ray to assist with positioning the PICC when placing it proves difficult.
The Sherlock system, on the other hand, uses magnetic and electrocardiographic real-time tracking of a PICC to enable the person placing the catheter to detect and correct any error in how the tip is positioned.
The device’s manufacturer, C.R. Bard, says the Sherlock System eliminates the need for the patient to have an X-ray, thus preventing delays in treatment or monitoring.
“Using the technology also increases staff and patient confidence of the accuracy of the procedure during catheter insertion,” said Professor Carole Longson, director of the NICE centre for health technology evaluation.
The cost of the Sherlock 3CG TCS is stated in the manufacturer’s submission as £9990 (excluding value-added tax). The cost of consumables associated with each insertion is £189.91. Maintenance costs associated with the technology are £595 per year.
Across the whole population in which PICCs are placed, the cost of using the Sherlock system is similar to blind insertion followed by X-ray, but it can save up to £106 per patient in specific clinical situations.
In intensive care, where PICCs are more likely to be placed incorrectly using blind insertion, the savings from using the Sherlock system and a confirmatory X-ray are estimated at around £41 per patient, compared with blind insertion and standard X-ray. (In intensive care settings, staff members sometimes initially use Sherlock with confirmatory X-ray while they are becoming accustomed to the system.)
For more information on the system, see the draft guidance consultation. It is open for public comment until December 9. {HT_DN}

The UK’s National Institute for Health and Care Excellence (NICE) has opened consultation on a draft guidance about a device designed to help healthcare professionals correctly place peripherally inserted central catheters
(PICCs).
The draft guidance supports using the Sherlock 3CG Tip Confirmation System for placing PICCs.
The standard procedure for placing PICCs is blind insertion, followed by a chest X-ray to check the catheter’s position.
In some cases, fluoroscopy is used instead of standard X-ray to assist with positioning the PICC when placing it proves difficult.
The Sherlock system, on the other hand, uses magnetic and electrocardiographic real-time tracking of a PICC to enable the person placing the catheter to detect and correct any error in how the tip is positioned.
The device’s manufacturer, C.R. Bard, says the Sherlock System eliminates the need for the patient to have an X-ray, thus preventing delays in treatment or monitoring.
“Using the technology also increases staff and patient confidence of the accuracy of the procedure during catheter insertion,” said Professor Carole Longson, director of the NICE centre for health technology evaluation.
The cost of the Sherlock 3CG TCS is stated in the manufacturer’s submission as £9990 (excluding value-added tax). The cost of consumables associated with each insertion is £189.91. Maintenance costs associated with the technology are £595 per year.
Across the whole population in which PICCs are placed, the cost of using the Sherlock system is similar to blind insertion followed by X-ray, but it can save up to £106 per patient in specific clinical situations.
In intensive care, where PICCs are more likely to be placed incorrectly using blind insertion, the savings from using the Sherlock system and a confirmatory X-ray are estimated at around £41 per patient, compared with blind insertion and standard X-ray. (In intensive care settings, staff members sometimes initially use Sherlock with confirmatory X-ray while they are becoming accustomed to the system.)
For more information on the system, see the draft guidance consultation. It is open for public comment until December 9. {HT_DN}

The UK’s National Institute for Health and Care Excellence (NICE) has opened consultation on a draft guidance about a device designed to help healthcare professionals correctly place peripherally inserted central catheters
(PICCs).
The draft guidance supports using the Sherlock 3CG Tip Confirmation System for placing PICCs.
The standard procedure for placing PICCs is blind insertion, followed by a chest X-ray to check the catheter’s position.
In some cases, fluoroscopy is used instead of standard X-ray to assist with positioning the PICC when placing it proves difficult.
The Sherlock system, on the other hand, uses magnetic and electrocardiographic real-time tracking of a PICC to enable the person placing the catheter to detect and correct any error in how the tip is positioned.
The device’s manufacturer, C.R. Bard, says the Sherlock System eliminates the need for the patient to have an X-ray, thus preventing delays in treatment or monitoring.
“Using the technology also increases staff and patient confidence of the accuracy of the procedure during catheter insertion,” said Professor Carole Longson, director of the NICE centre for health technology evaluation.
The cost of the Sherlock 3CG TCS is stated in the manufacturer’s submission as £9990 (excluding value-added tax). The cost of consumables associated with each insertion is £189.91. Maintenance costs associated with the technology are £595 per year.
Across the whole population in which PICCs are placed, the cost of using the Sherlock system is similar to blind insertion followed by X-ray, but it can save up to £106 per patient in specific clinical situations.
In intensive care, where PICCs are more likely to be placed incorrectly using blind insertion, the savings from using the Sherlock system and a confirmatory X-ray are estimated at around £41 per patient, compared with blind insertion and standard X-ray. (In intensive care settings, staff members sometimes initially use Sherlock with confirmatory X-ray while they are becoming accustomed to the system.)
For more information on the system, see the draft guidance consultation. It is open for public comment until December 9. {HT_DN}
Group develops cancer health literacy tool

patient and her father
Credit: Rhoda Baer
A new tool can identify patients with limited cancer health literacy, according to research published in the Journal of Health Communications.
The study authors noted that cancer patients are expected to play an active role in their care by adhering to medication regimens, distinguishing between scientifically credible medical evidence and misconceptions, and communicating with their providers about treatment decisions, risks, and survival rates.
However, patients with limited cancer health literacy can struggle with these responsibilities and potentially jeopardize their health by making uninformed decisions.
So Levent Dumenci, PhD, of Virginia Commonwealth University in Richmond, and his colleagues developed a tool to assess health literacy among cancer patients.
“Before now, there were only instruments that measured a particular aspect of general health literacy,” Dr Dumenci said. “It is important to have a tool that is specific to cancer because of the complex treatment options that cancer patients face, along with the increased demand for self-care.”
To meet that need, he and his colleagues developed the Cancer Health Literacy Test (CHLT)-30. The test, which is given via a touch-screen device, includes 30
questions about cancer treatment, medication side effects, and other cancer-related issues.
Six of the questions (CHLT-6) were specifically designed to quickly identify individuals with limited cancer health literacy.
The researchers tested the CHLT-30 in 1306 African American and Caucasian patients who were treated at oncology clinics in Virginia.
The team said the test accurately measured literacy and quickly identified patients with limited cancer health literacy. Eighteen percent of cancer patients had limited literacy, with an overrepresentation of African American, undereducated, and low-income patients.
“Using this tool, it takes just 1 to 2 minutes in the doctor’s office waiting room to identify patients with limited [cancer health literacy],” Dr Dumenci said. “Then, this information can be digitally communicated to the doctors prior to seeing the patients, so that they are prepared to talk with the patients in terms they can understand. This simple change could lead to big improvements in health outcomes.”
In future studies, the researchers hope to evaluate the cancer health literacy of Hispanic patients because prior research has pointed to disparities in this population’s health literacy.

patient and her father
Credit: Rhoda Baer
A new tool can identify patients with limited cancer health literacy, according to research published in the Journal of Health Communications.
The study authors noted that cancer patients are expected to play an active role in their care by adhering to medication regimens, distinguishing between scientifically credible medical evidence and misconceptions, and communicating with their providers about treatment decisions, risks, and survival rates.
However, patients with limited cancer health literacy can struggle with these responsibilities and potentially jeopardize their health by making uninformed decisions.
So Levent Dumenci, PhD, of Virginia Commonwealth University in Richmond, and his colleagues developed a tool to assess health literacy among cancer patients.
“Before now, there were only instruments that measured a particular aspect of general health literacy,” Dr Dumenci said. “It is important to have a tool that is specific to cancer because of the complex treatment options that cancer patients face, along with the increased demand for self-care.”
To meet that need, he and his colleagues developed the Cancer Health Literacy Test (CHLT)-30. The test, which is given via a touch-screen device, includes 30
questions about cancer treatment, medication side effects, and other cancer-related issues.
Six of the questions (CHLT-6) were specifically designed to quickly identify individuals with limited cancer health literacy.
The researchers tested the CHLT-30 in 1306 African American and Caucasian patients who were treated at oncology clinics in Virginia.
The team said the test accurately measured literacy and quickly identified patients with limited cancer health literacy. Eighteen percent of cancer patients had limited literacy, with an overrepresentation of African American, undereducated, and low-income patients.
“Using this tool, it takes just 1 to 2 minutes in the doctor’s office waiting room to identify patients with limited [cancer health literacy],” Dr Dumenci said. “Then, this information can be digitally communicated to the doctors prior to seeing the patients, so that they are prepared to talk with the patients in terms they can understand. This simple change could lead to big improvements in health outcomes.”
In future studies, the researchers hope to evaluate the cancer health literacy of Hispanic patients because prior research has pointed to disparities in this population’s health literacy.

patient and her father
Credit: Rhoda Baer
A new tool can identify patients with limited cancer health literacy, according to research published in the Journal of Health Communications.
The study authors noted that cancer patients are expected to play an active role in their care by adhering to medication regimens, distinguishing between scientifically credible medical evidence and misconceptions, and communicating with their providers about treatment decisions, risks, and survival rates.
However, patients with limited cancer health literacy can struggle with these responsibilities and potentially jeopardize their health by making uninformed decisions.
So Levent Dumenci, PhD, of Virginia Commonwealth University in Richmond, and his colleagues developed a tool to assess health literacy among cancer patients.
“Before now, there were only instruments that measured a particular aspect of general health literacy,” Dr Dumenci said. “It is important to have a tool that is specific to cancer because of the complex treatment options that cancer patients face, along with the increased demand for self-care.”
To meet that need, he and his colleagues developed the Cancer Health Literacy Test (CHLT)-30. The test, which is given via a touch-screen device, includes 30
questions about cancer treatment, medication side effects, and other cancer-related issues.
Six of the questions (CHLT-6) were specifically designed to quickly identify individuals with limited cancer health literacy.
The researchers tested the CHLT-30 in 1306 African American and Caucasian patients who were treated at oncology clinics in Virginia.
The team said the test accurately measured literacy and quickly identified patients with limited cancer health literacy. Eighteen percent of cancer patients had limited literacy, with an overrepresentation of African American, undereducated, and low-income patients.
“Using this tool, it takes just 1 to 2 minutes in the doctor’s office waiting room to identify patients with limited [cancer health literacy],” Dr Dumenci said. “Then, this information can be digitally communicated to the doctors prior to seeing the patients, so that they are prepared to talk with the patients in terms they can understand. This simple change could lead to big improvements in health outcomes.”
In future studies, the researchers hope to evaluate the cancer health literacy of Hispanic patients because prior research has pointed to disparities in this population’s health literacy.
Malaria prevents hospitals from meeting blood demands
PHILADELPHIA—The demand for blood transfusions increases substantially during high malaria transmission season, according to a study of hospitals in Tanzania.
On average, blood demand increased about 24% from low transmission season to high transmission season.
And some hospitals could not meet the increased demand. Unmet demand was highest in government hospitals, followed by faith-based institutions and private facilities.
Bakary Drammeh, DrPH, of the Centers for Disease Control and Prevention in Atlanta, Georgia, and his colleagues presented these results in a poster (SP356) at the AABB Annual Meeting 2014.
The researchers analyzed 14,706 blood prescriptions at 42 Tanzanian hospitals—21 government, 9 private, and 12 faith-based institutions.
The team assessed the number of blood prescriptions according to high and low malaria transmission periods—June-July vs August-September.
On average, there were 130 monthly blood prescriptions written per 100 beds during high malaria transmission season and 107 written during low transmission season.
There were 189 and 153 units of blood or blood components requested per 100 beds during high and low seasons, respectively. And there were 159 and 127 units issued, respectively.
Ultimately, an average of 145 units were transfused per 100 beds during high malaria transmission season, and 122 were transfused during low transmission season.
Across all 42 hospitals, total blood prescriptions increased 29% from low malaria transmission season to high transmission season.
The number of units requested increased 26%, the number of units issued increased 34%, and the number of units transfused increased 28%.
So, on average, blood demand increased 23.5% at these 42 hospitals during high malaria transmission season. And some hospitals did not have enough blood to meet demand.
The unmet blood demand was highest in government hospitals, at 25%, compared to faith-based hospitals, at 11%, and private hospitals, at 5%.
The researchers said these results suggest blood services should monitor malaria transmission surveillance reports and revise or project blood collection targets to meet the anticipated demand.
PHILADELPHIA—The demand for blood transfusions increases substantially during high malaria transmission season, according to a study of hospitals in Tanzania.
On average, blood demand increased about 24% from low transmission season to high transmission season.
And some hospitals could not meet the increased demand. Unmet demand was highest in government hospitals, followed by faith-based institutions and private facilities.
Bakary Drammeh, DrPH, of the Centers for Disease Control and Prevention in Atlanta, Georgia, and his colleagues presented these results in a poster (SP356) at the AABB Annual Meeting 2014.
The researchers analyzed 14,706 blood prescriptions at 42 Tanzanian hospitals—21 government, 9 private, and 12 faith-based institutions.
The team assessed the number of blood prescriptions according to high and low malaria transmission periods—June-July vs August-September.
On average, there were 130 monthly blood prescriptions written per 100 beds during high malaria transmission season and 107 written during low transmission season.
There were 189 and 153 units of blood or blood components requested per 100 beds during high and low seasons, respectively. And there were 159 and 127 units issued, respectively.
Ultimately, an average of 145 units were transfused per 100 beds during high malaria transmission season, and 122 were transfused during low transmission season.
Across all 42 hospitals, total blood prescriptions increased 29% from low malaria transmission season to high transmission season.
The number of units requested increased 26%, the number of units issued increased 34%, and the number of units transfused increased 28%.
So, on average, blood demand increased 23.5% at these 42 hospitals during high malaria transmission season. And some hospitals did not have enough blood to meet demand.
The unmet blood demand was highest in government hospitals, at 25%, compared to faith-based hospitals, at 11%, and private hospitals, at 5%.
The researchers said these results suggest blood services should monitor malaria transmission surveillance reports and revise or project blood collection targets to meet the anticipated demand.
PHILADELPHIA—The demand for blood transfusions increases substantially during high malaria transmission season, according to a study of hospitals in Tanzania.
On average, blood demand increased about 24% from low transmission season to high transmission season.
And some hospitals could not meet the increased demand. Unmet demand was highest in government hospitals, followed by faith-based institutions and private facilities.
Bakary Drammeh, DrPH, of the Centers for Disease Control and Prevention in Atlanta, Georgia, and his colleagues presented these results in a poster (SP356) at the AABB Annual Meeting 2014.
The researchers analyzed 14,706 blood prescriptions at 42 Tanzanian hospitals—21 government, 9 private, and 12 faith-based institutions.
The team assessed the number of blood prescriptions according to high and low malaria transmission periods—June-July vs August-September.
On average, there were 130 monthly blood prescriptions written per 100 beds during high malaria transmission season and 107 written during low transmission season.
There were 189 and 153 units of blood or blood components requested per 100 beds during high and low seasons, respectively. And there were 159 and 127 units issued, respectively.
Ultimately, an average of 145 units were transfused per 100 beds during high malaria transmission season, and 122 were transfused during low transmission season.
Across all 42 hospitals, total blood prescriptions increased 29% from low malaria transmission season to high transmission season.
The number of units requested increased 26%, the number of units issued increased 34%, and the number of units transfused increased 28%.
So, on average, blood demand increased 23.5% at these 42 hospitals during high malaria transmission season. And some hospitals did not have enough blood to meet demand.
The unmet blood demand was highest in government hospitals, at 25%, compared to faith-based hospitals, at 11%, and private hospitals, at 5%.
The researchers said these results suggest blood services should monitor malaria transmission surveillance reports and revise or project blood collection targets to meet the anticipated demand.