User login
Team discovers key aspects of HSC development

New research suggests proinflammatory signaling is crucial to the creation of hematopoietic stem cells (HSCs) during embryonic development, a finding that could help scientists reproduce HSCs for therapeutic use.
Researchers discovered that TNFR2, via TNFα, activates the Notch and NF-kB signaling pathways to establish HSC fate, which suggests inflammatory signaling is required for HSC generation.
The group also found that primitive neutrophils are the major source of TNFa. So it seems these cells are crucial to HSC development as well.
The researchers described these findings in Cell.
“The development of some mature cell lineages from iPSCs [induced pluripotent stem cells], such as cardiac and neural, has been reasonably straightforward, but not with HSCs,” said principal investigator David Traver, PhD, of the University of California, San Diego School of Medicine.
“This is likely due, at least in part, to not fully understanding all of the factors used by the embryo to generate HSCs. We believe the discovery that proinflammatory cues are important in vivo will help us recapitulate instruction of HSC fate in vitro from iPSCs.”
For this study, Dr Traver and his colleagues decided to examine the role of TNFα in HSC development, extending previous research by Victoriano Mulero, PhD, of the University of Murcia in Spain.
Dr Mulero reported that TNFα is important in the function of the embryonic vascular system. And, in animal models where TNF function was absent, blood defects resulted.
Raquel Espin-Palazon, PhD, a researcher in Dr Traver’s lab and a former colleague of Dr Mulero’s, determined that TNFα is required for the emergence of HSCs during embryogenesis in zebrafish.
Dr Traver said the finding was completely unexpected because HSCs emerge relatively early in embryonic formation, when the developing organism is considered to be largely sterile and devoid of infection.
“Thus, there was no expectation that proinflammatory signaling would be active at this time or in the blood-forming regions,” Dr Traver said. “Equally surprising, we found that a population of embryonic myeloid cells, which are transient cells produced before HSCs arise, are the producers of the TNFα needed to establish HSC fate.”
“So it turns out that a small subset of myeloid cells that persist for only a few days in development are necessary to help generate the lineal precursors of the entire adult blood-forming system.” ![]()

New research suggests proinflammatory signaling is crucial to the creation of hematopoietic stem cells (HSCs) during embryonic development, a finding that could help scientists reproduce HSCs for therapeutic use.
Researchers discovered that TNFR2, via TNFα, activates the Notch and NF-kB signaling pathways to establish HSC fate, which suggests inflammatory signaling is required for HSC generation.
The group also found that primitive neutrophils are the major source of TNFa. So it seems these cells are crucial to HSC development as well.
The researchers described these findings in Cell.
“The development of some mature cell lineages from iPSCs [induced pluripotent stem cells], such as cardiac and neural, has been reasonably straightforward, but not with HSCs,” said principal investigator David Traver, PhD, of the University of California, San Diego School of Medicine.
“This is likely due, at least in part, to not fully understanding all of the factors used by the embryo to generate HSCs. We believe the discovery that proinflammatory cues are important in vivo will help us recapitulate instruction of HSC fate in vitro from iPSCs.”
For this study, Dr Traver and his colleagues decided to examine the role of TNFα in HSC development, extending previous research by Victoriano Mulero, PhD, of the University of Murcia in Spain.
Dr Mulero reported that TNFα is important in the function of the embryonic vascular system. And, in animal models where TNF function was absent, blood defects resulted.
Raquel Espin-Palazon, PhD, a researcher in Dr Traver’s lab and a former colleague of Dr Mulero’s, determined that TNFα is required for the emergence of HSCs during embryogenesis in zebrafish.
Dr Traver said the finding was completely unexpected because HSCs emerge relatively early in embryonic formation, when the developing organism is considered to be largely sterile and devoid of infection.
“Thus, there was no expectation that proinflammatory signaling would be active at this time or in the blood-forming regions,” Dr Traver said. “Equally surprising, we found that a population of embryonic myeloid cells, which are transient cells produced before HSCs arise, are the producers of the TNFα needed to establish HSC fate.”
“So it turns out that a small subset of myeloid cells that persist for only a few days in development are necessary to help generate the lineal precursors of the entire adult blood-forming system.” ![]()

New research suggests proinflammatory signaling is crucial to the creation of hematopoietic stem cells (HSCs) during embryonic development, a finding that could help scientists reproduce HSCs for therapeutic use.
Researchers discovered that TNFR2, via TNFα, activates the Notch and NF-kB signaling pathways to establish HSC fate, which suggests inflammatory signaling is required for HSC generation.
The group also found that primitive neutrophils are the major source of TNFa. So it seems these cells are crucial to HSC development as well.
The researchers described these findings in Cell.
“The development of some mature cell lineages from iPSCs [induced pluripotent stem cells], such as cardiac and neural, has been reasonably straightforward, but not with HSCs,” said principal investigator David Traver, PhD, of the University of California, San Diego School of Medicine.
“This is likely due, at least in part, to not fully understanding all of the factors used by the embryo to generate HSCs. We believe the discovery that proinflammatory cues are important in vivo will help us recapitulate instruction of HSC fate in vitro from iPSCs.”
For this study, Dr Traver and his colleagues decided to examine the role of TNFα in HSC development, extending previous research by Victoriano Mulero, PhD, of the University of Murcia in Spain.
Dr Mulero reported that TNFα is important in the function of the embryonic vascular system. And, in animal models where TNF function was absent, blood defects resulted.
Raquel Espin-Palazon, PhD, a researcher in Dr Traver’s lab and a former colleague of Dr Mulero’s, determined that TNFα is required for the emergence of HSCs during embryogenesis in zebrafish.
Dr Traver said the finding was completely unexpected because HSCs emerge relatively early in embryonic formation, when the developing organism is considered to be largely sterile and devoid of infection.
“Thus, there was no expectation that proinflammatory signaling would be active at this time or in the blood-forming regions,” Dr Traver said. “Equally surprising, we found that a population of embryonic myeloid cells, which are transient cells produced before HSCs arise, are the producers of the TNFα needed to establish HSC fate.”
“So it turns out that a small subset of myeloid cells that persist for only a few days in development are necessary to help generate the lineal precursors of the entire adult blood-forming system.” ![]()
Obesity affects toxicity of immunotherapy
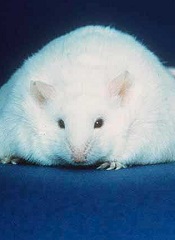
Immunotherapy that can be effective against tumors in young, thin mice can be lethal to obese ones, according to research published in The Journal of Experimental Medicine.
Investigators conducted experiments in mouse models to determine if there is a subset of cancer patients for whom certain immunotherapies might be especially toxic.
The group found a potential link between body fat and the risk of toxicity from some types of immunotherapy.
“Cancer is primarily considered a disease of the aged, and yet preclinical studies generally use young, lean animal models that may not be reflective of the ‘typical’ cancer patient,” said study author Annie Mirsoian, a PhD candidate at the University of California, Davis in Sacramento.
“Aging is a dynamic process that is characterized by increases in inflammatory factors, as well as a shift in body composition where there is a gradual loss of lean muscle mass and an increase in fat accumulation, which effect how the immune system functions.”
Mirsoian and her colleagues sought to determine if, by adjusting the mouse model to more closely reflect the cancer patient phenotype (advanced age and overweight), they could better understand the discrepancies between animal study outcomes and those in patients in the clinic.
So the team examined aged mice on standard diets and compared those to aged mice that were calorie-restricted throughout their lives.
The investigators found that calorie restriction plays a protective role against toxicity. When aged mice ate their standard diet freely throughout life, they became obese and ultimately experienced lethal adverse reactions after receiving a systemic immunotherapy regimen.
“We know that people who are obese in general are at higher risk for complications from surgery, radiation, and chemotherapy,” said study author Arta Monjazeb, MD, PhD, of the University of California, Davis.
“We know that obese people have higher levels of inflammatory markers in their blood, but there is a lack of data examining the effects of obesity on cancer treatment outcomes.”
In follow-up experiments, the investigators found that young mice that are obese also endure similar toxic consequences, demonstrating that fat is a critical factor in toxic responses to stimulatory anticancer immunotherapy regimens.
“It is important to note, however, that the aged mice on standard diets succumbed to lethality at a quicker rate than young obese mice,” Mirsoian said. “Although our data demonstrate that obesity plays a central role in the development of adverse effects, future studies will focus on examining the aged immune system and cellular characteristics that may have enhanced the sensitivity of these mice to inflammation.”
This study follows an earlier paper, which demonstrated that while young, lean mice tolerate immunotherapy regimens without toxicity, the same regimen for an aged cohort resulted in lethal consequences. The new paper takes a deeper look into how fat deposition throughout aging can be critical in determining treatment tolerance and efficacy.
“Obesity has become an epidemic in our society and is now also affecting younger populations,” Mirsoian said. “Therefore, it’s likely that what the ‘typical’ cancer patient looks like will change. Our findings demonstrate the importance of having preclinical animal models that reflect the clinical scenario.”
“Changing the characteristics of our mouse models allowed for a more accurate determination of possible adverse reactions to therapy and more closely modeled what has been reported in the clinic with stimulatory immunotherapies.”
The investigators said factors like age, fat content, and the types of infections experienced throughout life together shape how the immune system reacts, and they will continue to work on improving their modeling system to reflect these changes.
They project that improvements in mouse modeling may help produce data that can better modulate treatment choices for patients, as well as identify early which patients would benefit from the inclusion of drugs to prevent adverse reactions while maintaining anticancer efficacy. ![]()

Immunotherapy that can be effective against tumors in young, thin mice can be lethal to obese ones, according to research published in The Journal of Experimental Medicine.
Investigators conducted experiments in mouse models to determine if there is a subset of cancer patients for whom certain immunotherapies might be especially toxic.
The group found a potential link between body fat and the risk of toxicity from some types of immunotherapy.
“Cancer is primarily considered a disease of the aged, and yet preclinical studies generally use young, lean animal models that may not be reflective of the ‘typical’ cancer patient,” said study author Annie Mirsoian, a PhD candidate at the University of California, Davis in Sacramento.
“Aging is a dynamic process that is characterized by increases in inflammatory factors, as well as a shift in body composition where there is a gradual loss of lean muscle mass and an increase in fat accumulation, which effect how the immune system functions.”
Mirsoian and her colleagues sought to determine if, by adjusting the mouse model to more closely reflect the cancer patient phenotype (advanced age and overweight), they could better understand the discrepancies between animal study outcomes and those in patients in the clinic.
So the team examined aged mice on standard diets and compared those to aged mice that were calorie-restricted throughout their lives.
The investigators found that calorie restriction plays a protective role against toxicity. When aged mice ate their standard diet freely throughout life, they became obese and ultimately experienced lethal adverse reactions after receiving a systemic immunotherapy regimen.
“We know that people who are obese in general are at higher risk for complications from surgery, radiation, and chemotherapy,” said study author Arta Monjazeb, MD, PhD, of the University of California, Davis.
“We know that obese people have higher levels of inflammatory markers in their blood, but there is a lack of data examining the effects of obesity on cancer treatment outcomes.”
In follow-up experiments, the investigators found that young mice that are obese also endure similar toxic consequences, demonstrating that fat is a critical factor in toxic responses to stimulatory anticancer immunotherapy regimens.
“It is important to note, however, that the aged mice on standard diets succumbed to lethality at a quicker rate than young obese mice,” Mirsoian said. “Although our data demonstrate that obesity plays a central role in the development of adverse effects, future studies will focus on examining the aged immune system and cellular characteristics that may have enhanced the sensitivity of these mice to inflammation.”
This study follows an earlier paper, which demonstrated that while young, lean mice tolerate immunotherapy regimens without toxicity, the same regimen for an aged cohort resulted in lethal consequences. The new paper takes a deeper look into how fat deposition throughout aging can be critical in determining treatment tolerance and efficacy.
“Obesity has become an epidemic in our society and is now also affecting younger populations,” Mirsoian said. “Therefore, it’s likely that what the ‘typical’ cancer patient looks like will change. Our findings demonstrate the importance of having preclinical animal models that reflect the clinical scenario.”
“Changing the characteristics of our mouse models allowed for a more accurate determination of possible adverse reactions to therapy and more closely modeled what has been reported in the clinic with stimulatory immunotherapies.”
The investigators said factors like age, fat content, and the types of infections experienced throughout life together shape how the immune system reacts, and they will continue to work on improving their modeling system to reflect these changes.
They project that improvements in mouse modeling may help produce data that can better modulate treatment choices for patients, as well as identify early which patients would benefit from the inclusion of drugs to prevent adverse reactions while maintaining anticancer efficacy. ![]()

Immunotherapy that can be effective against tumors in young, thin mice can be lethal to obese ones, according to research published in The Journal of Experimental Medicine.
Investigators conducted experiments in mouse models to determine if there is a subset of cancer patients for whom certain immunotherapies might be especially toxic.
The group found a potential link between body fat and the risk of toxicity from some types of immunotherapy.
“Cancer is primarily considered a disease of the aged, and yet preclinical studies generally use young, lean animal models that may not be reflective of the ‘typical’ cancer patient,” said study author Annie Mirsoian, a PhD candidate at the University of California, Davis in Sacramento.
“Aging is a dynamic process that is characterized by increases in inflammatory factors, as well as a shift in body composition where there is a gradual loss of lean muscle mass and an increase in fat accumulation, which effect how the immune system functions.”
Mirsoian and her colleagues sought to determine if, by adjusting the mouse model to more closely reflect the cancer patient phenotype (advanced age and overweight), they could better understand the discrepancies between animal study outcomes and those in patients in the clinic.
So the team examined aged mice on standard diets and compared those to aged mice that were calorie-restricted throughout their lives.
The investigators found that calorie restriction plays a protective role against toxicity. When aged mice ate their standard diet freely throughout life, they became obese and ultimately experienced lethal adverse reactions after receiving a systemic immunotherapy regimen.
“We know that people who are obese in general are at higher risk for complications from surgery, radiation, and chemotherapy,” said study author Arta Monjazeb, MD, PhD, of the University of California, Davis.
“We know that obese people have higher levels of inflammatory markers in their blood, but there is a lack of data examining the effects of obesity on cancer treatment outcomes.”
In follow-up experiments, the investigators found that young mice that are obese also endure similar toxic consequences, demonstrating that fat is a critical factor in toxic responses to stimulatory anticancer immunotherapy regimens.
“It is important to note, however, that the aged mice on standard diets succumbed to lethality at a quicker rate than young obese mice,” Mirsoian said. “Although our data demonstrate that obesity plays a central role in the development of adverse effects, future studies will focus on examining the aged immune system and cellular characteristics that may have enhanced the sensitivity of these mice to inflammation.”
This study follows an earlier paper, which demonstrated that while young, lean mice tolerate immunotherapy regimens without toxicity, the same regimen for an aged cohort resulted in lethal consequences. The new paper takes a deeper look into how fat deposition throughout aging can be critical in determining treatment tolerance and efficacy.
“Obesity has become an epidemic in our society and is now also affecting younger populations,” Mirsoian said. “Therefore, it’s likely that what the ‘typical’ cancer patient looks like will change. Our findings demonstrate the importance of having preclinical animal models that reflect the clinical scenario.”
“Changing the characteristics of our mouse models allowed for a more accurate determination of possible adverse reactions to therapy and more closely modeled what has been reported in the clinic with stimulatory immunotherapies.”
The investigators said factors like age, fat content, and the types of infections experienced throughout life together shape how the immune system reacts, and they will continue to work on improving their modeling system to reflect these changes.
They project that improvements in mouse modeling may help produce data that can better modulate treatment choices for patients, as well as identify early which patients would benefit from the inclusion of drugs to prevent adverse reactions while maintaining anticancer efficacy. ![]()
Paperwork consumes docs’ time, erodes morale

A survey of nearly 5000 US physicians showed that the average doctor spent 16.6% of his or her working hours on non-patient-related paperwork.
This includes tasks such as billing, obtaining insurance approvals, financial and personnel management, and negotiating contracts.
The more time doctors spent on such tasks, the less satisfied they were with medicine as a career.
Researchers detailed these findings in the International Journal of Health Services.
“Our crazy health financing system is demoralizing doctors and wasting vast resources,” said study author David Himmelstein, MD, a professor at Hunter College of the City University of New York.
“Turning healthcare into a business means we spend more and more time on billing, insurance paperwork, and the bottom line. We need to move to a simple, nonprofit national health insurance system that lets doctors and hospitals focus on patients, not finances.”
Dr Himmelstein and colleague Steffie Woolhandler, MD, analyzed confidential data from the 2008 Health Tracking Physician Survey (the most recent data available). The survey included information from a nationally representative sample of 4720 physicians who practiced at least 20 hours per week.
The data showed that the average doctor spent 8.7 hours per week, or 16.6% of his or her working time, on non-patient-related administration. This excludes tasks such as writing chart notes, communicating with other doctors, and ordering lab tests.
In total, patient-care physicians spent 168.4 million hours on non-patient-related administrative tasks in 2008. Drs Himmelstein and Woolhandler estimate that the total cost of physician time spent on administration in 2014 will amount to $102 billion.
Career satisfaction was lower for physicians who spent more time on administration. “Very satisfied” doctors spent, on average, 16.1% of their time on administration. “Very dissatisfied” doctors spent 20.6% of their time on such tasks.
Among various specialties, psychiatrists spent the most time on administration (20.3%), followed by internists (17.3%) and family/general practitioners (17.3%). Pediatricians spent the least amount of time (14.1%) on non-patient-related administrative tasks and were the most satisfied group of doctors.
Solo practice was associated with more administrative work, but small group practice was not. Doctors practicing in groups of 100 or more actually spent more time (19.7%) on such tasks than those in small groups (16.3%).
The researchers were surprised to find that physicians who used electronic health records spent more time (17.2% for those using entirely electronic records, 18% for those using a mix of paper and electronic) on administration than those who used only paper records (15.5%).
The pair noted that physicians in Canada spend far less time on administration than US doctors, and they attributed the difference to Canada’s single-payer system, which has greatly simplified billing and reduced bureaucracy.
The researchers pointed out that the only previous nationally representative survey of this kind was carried out in 1995, and that study showed that administration and insurance-related matters accounted for 13.5% of physicians’ total work time. Other, less representative studies also suggest the bureaucratic burden on physicians has grown in the past two decades.
“American doctors are drowning in paperwork,” Dr Woolhandler said. “Our study almost certainly understates physicians’ current administrative burden.”
“Since 2008, when the survey we analyzed was collected, tens of thousands of doctors have moved from small private practices with minimal bureaucracy into giant group practices where bureaucracy is rampant. And under the accountable care organizations favored by insurers, more doctors are facing HMO-type incentives to deny care to their patients, a move that our data shows drives up administrative work.” ![]()

A survey of nearly 5000 US physicians showed that the average doctor spent 16.6% of his or her working hours on non-patient-related paperwork.
This includes tasks such as billing, obtaining insurance approvals, financial and personnel management, and negotiating contracts.
The more time doctors spent on such tasks, the less satisfied they were with medicine as a career.
Researchers detailed these findings in the International Journal of Health Services.
“Our crazy health financing system is demoralizing doctors and wasting vast resources,” said study author David Himmelstein, MD, a professor at Hunter College of the City University of New York.
“Turning healthcare into a business means we spend more and more time on billing, insurance paperwork, and the bottom line. We need to move to a simple, nonprofit national health insurance system that lets doctors and hospitals focus on patients, not finances.”
Dr Himmelstein and colleague Steffie Woolhandler, MD, analyzed confidential data from the 2008 Health Tracking Physician Survey (the most recent data available). The survey included information from a nationally representative sample of 4720 physicians who practiced at least 20 hours per week.
The data showed that the average doctor spent 8.7 hours per week, or 16.6% of his or her working time, on non-patient-related administration. This excludes tasks such as writing chart notes, communicating with other doctors, and ordering lab tests.
In total, patient-care physicians spent 168.4 million hours on non-patient-related administrative tasks in 2008. Drs Himmelstein and Woolhandler estimate that the total cost of physician time spent on administration in 2014 will amount to $102 billion.
Career satisfaction was lower for physicians who spent more time on administration. “Very satisfied” doctors spent, on average, 16.1% of their time on administration. “Very dissatisfied” doctors spent 20.6% of their time on such tasks.
Among various specialties, psychiatrists spent the most time on administration (20.3%), followed by internists (17.3%) and family/general practitioners (17.3%). Pediatricians spent the least amount of time (14.1%) on non-patient-related administrative tasks and were the most satisfied group of doctors.
Solo practice was associated with more administrative work, but small group practice was not. Doctors practicing in groups of 100 or more actually spent more time (19.7%) on such tasks than those in small groups (16.3%).
The researchers were surprised to find that physicians who used electronic health records spent more time (17.2% for those using entirely electronic records, 18% for those using a mix of paper and electronic) on administration than those who used only paper records (15.5%).
The pair noted that physicians in Canada spend far less time on administration than US doctors, and they attributed the difference to Canada’s single-payer system, which has greatly simplified billing and reduced bureaucracy.
The researchers pointed out that the only previous nationally representative survey of this kind was carried out in 1995, and that study showed that administration and insurance-related matters accounted for 13.5% of physicians’ total work time. Other, less representative studies also suggest the bureaucratic burden on physicians has grown in the past two decades.
“American doctors are drowning in paperwork,” Dr Woolhandler said. “Our study almost certainly understates physicians’ current administrative burden.”
“Since 2008, when the survey we analyzed was collected, tens of thousands of doctors have moved from small private practices with minimal bureaucracy into giant group practices where bureaucracy is rampant. And under the accountable care organizations favored by insurers, more doctors are facing HMO-type incentives to deny care to their patients, a move that our data shows drives up administrative work.” ![]()

A survey of nearly 5000 US physicians showed that the average doctor spent 16.6% of his or her working hours on non-patient-related paperwork.
This includes tasks such as billing, obtaining insurance approvals, financial and personnel management, and negotiating contracts.
The more time doctors spent on such tasks, the less satisfied they were with medicine as a career.
Researchers detailed these findings in the International Journal of Health Services.
“Our crazy health financing system is demoralizing doctors and wasting vast resources,” said study author David Himmelstein, MD, a professor at Hunter College of the City University of New York.
“Turning healthcare into a business means we spend more and more time on billing, insurance paperwork, and the bottom line. We need to move to a simple, nonprofit national health insurance system that lets doctors and hospitals focus on patients, not finances.”
Dr Himmelstein and colleague Steffie Woolhandler, MD, analyzed confidential data from the 2008 Health Tracking Physician Survey (the most recent data available). The survey included information from a nationally representative sample of 4720 physicians who practiced at least 20 hours per week.
The data showed that the average doctor spent 8.7 hours per week, or 16.6% of his or her working time, on non-patient-related administration. This excludes tasks such as writing chart notes, communicating with other doctors, and ordering lab tests.
In total, patient-care physicians spent 168.4 million hours on non-patient-related administrative tasks in 2008. Drs Himmelstein and Woolhandler estimate that the total cost of physician time spent on administration in 2014 will amount to $102 billion.
Career satisfaction was lower for physicians who spent more time on administration. “Very satisfied” doctors spent, on average, 16.1% of their time on administration. “Very dissatisfied” doctors spent 20.6% of their time on such tasks.
Among various specialties, psychiatrists spent the most time on administration (20.3%), followed by internists (17.3%) and family/general practitioners (17.3%). Pediatricians spent the least amount of time (14.1%) on non-patient-related administrative tasks and were the most satisfied group of doctors.
Solo practice was associated with more administrative work, but small group practice was not. Doctors practicing in groups of 100 or more actually spent more time (19.7%) on such tasks than those in small groups (16.3%).
The researchers were surprised to find that physicians who used electronic health records spent more time (17.2% for those using entirely electronic records, 18% for those using a mix of paper and electronic) on administration than those who used only paper records (15.5%).
The pair noted that physicians in Canada spend far less time on administration than US doctors, and they attributed the difference to Canada’s single-payer system, which has greatly simplified billing and reduced bureaucracy.
The researchers pointed out that the only previous nationally representative survey of this kind was carried out in 1995, and that study showed that administration and insurance-related matters accounted for 13.5% of physicians’ total work time. Other, less representative studies also suggest the bureaucratic burden on physicians has grown in the past two decades.
“American doctors are drowning in paperwork,” Dr Woolhandler said. “Our study almost certainly understates physicians’ current administrative burden.”
“Since 2008, when the survey we analyzed was collected, tens of thousands of doctors have moved from small private practices with minimal bureaucracy into giant group practices where bureaucracy is rampant. And under the accountable care organizations favored by insurers, more doctors are facing HMO-type incentives to deny care to their patients, a move that our data shows drives up administrative work.” ![]()
Device monitors methotrexate levels faster

Credit: Juan D. Alfonso
A new device can measure methotrexate levels in a patient’s blood in less than a minute, according to research published in Biosensors and Bioelectronics.
Researchers say this nanoscale device is just as accurate and 10 times less expensive than equipment currently used in hospitals.
It has an optical system that can rapidly gauge the optimal dose of methotrexate a patient needs, thereby reducing the risk of adverse effects.
“While effective, methotrexate is also highly toxic and can damage the healthy cells of patients, hence the importance of closely monitoring the drug’s concentration in the serum of treated individuals to adjust the dosage,” said study author Jean François Masson, PhD, of the University of Montreal in Quebec, Canada.
“The operation of the current [methotrexate monitoring] device is based on a cumbersome, expensive platform that requires experienced personnel because of the many samples that need to be manipulated.”
With this in mind, Dr Masson and his colleagues set out to simplify methotrexate monitoring.
In the course of their research, the team developed and manufactured a miniaturized device that works by surface plasmon resonance. It measures the concentration of serum methotrexate through gold nanoparticles on the surface of a receptacle.
In “competing” with methotrexate to block the enzyme dihydrofolate reductase, the gold nanoparticles change the color of the light detected by the instrument. And the color of the light detected reflects the exact concentration of the drug in the blood sample.
The researchers compared the accuracy of measurements taken with the new device to those taken with equipment used at the Maisonneuve-Rosemont Hospital in Montreal.
“Testing was conclusive,” Dr Masson said. “Not only were the measurements as accurate, but our device took less than 60 seconds to produce results, compared to 30 minutes for current devices.”
Moreover, the comparative tests were performed by lab technicians who were not experienced with surface plasmon resonance and did not encounter major difficulties in operating the new equipment or obtaining the same conclusive results as Dr Masson and his research team.
“In the near future, we can foresee the device in doctors’ offices or even at the bedside, where patients would receive individualized and optimal doses while minimizing the risk of complications,” Dr Masson said.
“While traditional equipment requires an investment of around $100,000, the new mobile device would likely cost 10 times less, around $10,000.” ![]()

Credit: Juan D. Alfonso
A new device can measure methotrexate levels in a patient’s blood in less than a minute, according to research published in Biosensors and Bioelectronics.
Researchers say this nanoscale device is just as accurate and 10 times less expensive than equipment currently used in hospitals.
It has an optical system that can rapidly gauge the optimal dose of methotrexate a patient needs, thereby reducing the risk of adverse effects.
“While effective, methotrexate is also highly toxic and can damage the healthy cells of patients, hence the importance of closely monitoring the drug’s concentration in the serum of treated individuals to adjust the dosage,” said study author Jean François Masson, PhD, of the University of Montreal in Quebec, Canada.
“The operation of the current [methotrexate monitoring] device is based on a cumbersome, expensive platform that requires experienced personnel because of the many samples that need to be manipulated.”
With this in mind, Dr Masson and his colleagues set out to simplify methotrexate monitoring.
In the course of their research, the team developed and manufactured a miniaturized device that works by surface plasmon resonance. It measures the concentration of serum methotrexate through gold nanoparticles on the surface of a receptacle.
In “competing” with methotrexate to block the enzyme dihydrofolate reductase, the gold nanoparticles change the color of the light detected by the instrument. And the color of the light detected reflects the exact concentration of the drug in the blood sample.
The researchers compared the accuracy of measurements taken with the new device to those taken with equipment used at the Maisonneuve-Rosemont Hospital in Montreal.
“Testing was conclusive,” Dr Masson said. “Not only were the measurements as accurate, but our device took less than 60 seconds to produce results, compared to 30 minutes for current devices.”
Moreover, the comparative tests were performed by lab technicians who were not experienced with surface plasmon resonance and did not encounter major difficulties in operating the new equipment or obtaining the same conclusive results as Dr Masson and his research team.
“In the near future, we can foresee the device in doctors’ offices or even at the bedside, where patients would receive individualized and optimal doses while minimizing the risk of complications,” Dr Masson said.
“While traditional equipment requires an investment of around $100,000, the new mobile device would likely cost 10 times less, around $10,000.” ![]()

Credit: Juan D. Alfonso
A new device can measure methotrexate levels in a patient’s blood in less than a minute, according to research published in Biosensors and Bioelectronics.
Researchers say this nanoscale device is just as accurate and 10 times less expensive than equipment currently used in hospitals.
It has an optical system that can rapidly gauge the optimal dose of methotrexate a patient needs, thereby reducing the risk of adverse effects.
“While effective, methotrexate is also highly toxic and can damage the healthy cells of patients, hence the importance of closely monitoring the drug’s concentration in the serum of treated individuals to adjust the dosage,” said study author Jean François Masson, PhD, of the University of Montreal in Quebec, Canada.
“The operation of the current [methotrexate monitoring] device is based on a cumbersome, expensive platform that requires experienced personnel because of the many samples that need to be manipulated.”
With this in mind, Dr Masson and his colleagues set out to simplify methotrexate monitoring.
In the course of their research, the team developed and manufactured a miniaturized device that works by surface plasmon resonance. It measures the concentration of serum methotrexate through gold nanoparticles on the surface of a receptacle.
In “competing” with methotrexate to block the enzyme dihydrofolate reductase, the gold nanoparticles change the color of the light detected by the instrument. And the color of the light detected reflects the exact concentration of the drug in the blood sample.
The researchers compared the accuracy of measurements taken with the new device to those taken with equipment used at the Maisonneuve-Rosemont Hospital in Montreal.
“Testing was conclusive,” Dr Masson said. “Not only were the measurements as accurate, but our device took less than 60 seconds to produce results, compared to 30 minutes for current devices.”
Moreover, the comparative tests were performed by lab technicians who were not experienced with surface plasmon resonance and did not encounter major difficulties in operating the new equipment or obtaining the same conclusive results as Dr Masson and his research team.
“In the near future, we can foresee the device in doctors’ offices or even at the bedside, where patients would receive individualized and optimal doses while minimizing the risk of complications,” Dr Masson said.
“While traditional equipment requires an investment of around $100,000, the new mobile device would likely cost 10 times less, around $10,000.” ![]()
Texts improve malaria treatment adherence

Credit: Ed Yourdon
Text messages reminding patients to take malaria medication can improve treatment adherence, according to a study published in PLOS ONE.
“When patients don’t complete their full medication regimen, diseases can develop resistance to treatment,” said study author Julia Raifman, a PhD candidate at the Harvard School of Public Health in Boston.
“And with infectious diseases like malaria, drug-resistant diseases can spread to others. We’ve already begun to see resistance to artemisinin in Southeast Asia. It would be catastrophic if that became widespread and there was no effective treatment for the most deadly form of malaria.”
Working with researchers at the non-profit Innovations for Poverty Action in Ghana, Raifman and her colleagues drew on previous research using SMS reminders in situations where people fail to follow through on intentions, such as saving money, paying back loans, or completing college financial aid forms.
The researchers recruited 1140 people in Ghana who were taking artemisinin-based combination therapy to treat malaria.
Participants used their mobile phones to enroll in an automated system, and the system randomly assigned half of them to receive the text message reminders to take their medication.
Local researchers followed up with the participants several days later at their homes to see how many pills they had taken. Subjects who received the texts were significantly more likely to finish the full regimen.
The researchers also tested whether a short or longer, more informative message would be more effective. They were surprised to find the shorter messages had a significant impact, but the longer ones did not.
“SMS reminders are a ‘nudge,’ not a ‘shove,’” said Aaron Dibner-Dunlap, of Innovations for Poverty Action. “They can help people follow through on something they originally intended to do, but human nature is tricky, and the science is still young.”
“We’re optimistic because the technology has become so widespread and inexpensive to administer, that for programs like this one that work, there’s huge potential for helping people at very low cost.” ![]()

Credit: Ed Yourdon
Text messages reminding patients to take malaria medication can improve treatment adherence, according to a study published in PLOS ONE.
“When patients don’t complete their full medication regimen, diseases can develop resistance to treatment,” said study author Julia Raifman, a PhD candidate at the Harvard School of Public Health in Boston.
“And with infectious diseases like malaria, drug-resistant diseases can spread to others. We’ve already begun to see resistance to artemisinin in Southeast Asia. It would be catastrophic if that became widespread and there was no effective treatment for the most deadly form of malaria.”
Working with researchers at the non-profit Innovations for Poverty Action in Ghana, Raifman and her colleagues drew on previous research using SMS reminders in situations where people fail to follow through on intentions, such as saving money, paying back loans, or completing college financial aid forms.
The researchers recruited 1140 people in Ghana who were taking artemisinin-based combination therapy to treat malaria.
Participants used their mobile phones to enroll in an automated system, and the system randomly assigned half of them to receive the text message reminders to take their medication.
Local researchers followed up with the participants several days later at their homes to see how many pills they had taken. Subjects who received the texts were significantly more likely to finish the full regimen.
The researchers also tested whether a short or longer, more informative message would be more effective. They were surprised to find the shorter messages had a significant impact, but the longer ones did not.
“SMS reminders are a ‘nudge,’ not a ‘shove,’” said Aaron Dibner-Dunlap, of Innovations for Poverty Action. “They can help people follow through on something they originally intended to do, but human nature is tricky, and the science is still young.”
“We’re optimistic because the technology has become so widespread and inexpensive to administer, that for programs like this one that work, there’s huge potential for helping people at very low cost.” ![]()

Credit: Ed Yourdon
Text messages reminding patients to take malaria medication can improve treatment adherence, according to a study published in PLOS ONE.
“When patients don’t complete their full medication regimen, diseases can develop resistance to treatment,” said study author Julia Raifman, a PhD candidate at the Harvard School of Public Health in Boston.
“And with infectious diseases like malaria, drug-resistant diseases can spread to others. We’ve already begun to see resistance to artemisinin in Southeast Asia. It would be catastrophic if that became widespread and there was no effective treatment for the most deadly form of malaria.”
Working with researchers at the non-profit Innovations for Poverty Action in Ghana, Raifman and her colleagues drew on previous research using SMS reminders in situations where people fail to follow through on intentions, such as saving money, paying back loans, or completing college financial aid forms.
The researchers recruited 1140 people in Ghana who were taking artemisinin-based combination therapy to treat malaria.
Participants used their mobile phones to enroll in an automated system, and the system randomly assigned half of them to receive the text message reminders to take their medication.
Local researchers followed up with the participants several days later at their homes to see how many pills they had taken. Subjects who received the texts were significantly more likely to finish the full regimen.
The researchers also tested whether a short or longer, more informative message would be more effective. They were surprised to find the shorter messages had a significant impact, but the longer ones did not.
“SMS reminders are a ‘nudge,’ not a ‘shove,’” said Aaron Dibner-Dunlap, of Innovations for Poverty Action. “They can help people follow through on something they originally intended to do, but human nature is tricky, and the science is still young.”
“We’re optimistic because the technology has become so widespread and inexpensive to administer, that for programs like this one that work, there’s huge potential for helping people at very low cost.” ![]()
Bacterium could help control malaria, dengue

Credit: CDC
A bacterium isolated from a mosquito’s gut could aid the fight against malaria and dengue, according to a study published in PLOS Pathogens.
With previous research, scientists isolated Csp_P, a member of the family of chromobacteria, from the gut of Aedes aegypti mosquitoes.
Now, the team has found that Csp_P can directly inhibit malaria and dengue pathogens in vitro and shorten the life span of the mosquitoes that transmit both diseases.
George Dimopoulos, PhD, of Johns Hopkins University in Baltimore, Maryland, and his colleagues examined Csp_P’s actions on both mosquitoes and pathogens, and the results suggest that Csp_P might help to fight malaria and dengue at different levels.
The researchers added Csp_P to sugar water fed to mosquitoes and found that the bacteria are able to quickly colonize the gut of the two most important mosquito disease vectors—Aedes aegypti and Anopheles gambiae.
Moreover, the presence of Csp_P in the gut reduced the susceptibility of the respective mosquitoes to infection with the malaria parasite Plasmodium falciparum or with dengue virus.
Even without gut colonization, exposure to Csp_P through food or breeding water shortened the lifespan of adult mosquitoes and mosquito larvae of both species.
When the researchers tested whether Csp_P could act against the malaria or dengue pathogens directly, they found that the bacterium, likely through the production of toxic metabolites, can inhibit the growth of Plasmodium at various stages during the parasite’s life cycle and also abolish dengue virus infectivity.
The team said these toxic metabolites could potentially be developed into drugs to treat malaria and dengue.
Overall, the researchers concluded that Csp_P’s broad-spectrum antipathogen properties and ability to kill mosquitoes make it a good candidate for the development of novel control strategies for malaria and dengue, so it warrants further study. ![]()

Credit: CDC
A bacterium isolated from a mosquito’s gut could aid the fight against malaria and dengue, according to a study published in PLOS Pathogens.
With previous research, scientists isolated Csp_P, a member of the family of chromobacteria, from the gut of Aedes aegypti mosquitoes.
Now, the team has found that Csp_P can directly inhibit malaria and dengue pathogens in vitro and shorten the life span of the mosquitoes that transmit both diseases.
George Dimopoulos, PhD, of Johns Hopkins University in Baltimore, Maryland, and his colleagues examined Csp_P’s actions on both mosquitoes and pathogens, and the results suggest that Csp_P might help to fight malaria and dengue at different levels.
The researchers added Csp_P to sugar water fed to mosquitoes and found that the bacteria are able to quickly colonize the gut of the two most important mosquito disease vectors—Aedes aegypti and Anopheles gambiae.
Moreover, the presence of Csp_P in the gut reduced the susceptibility of the respective mosquitoes to infection with the malaria parasite Plasmodium falciparum or with dengue virus.
Even without gut colonization, exposure to Csp_P through food or breeding water shortened the lifespan of adult mosquitoes and mosquito larvae of both species.
When the researchers tested whether Csp_P could act against the malaria or dengue pathogens directly, they found that the bacterium, likely through the production of toxic metabolites, can inhibit the growth of Plasmodium at various stages during the parasite’s life cycle and also abolish dengue virus infectivity.
The team said these toxic metabolites could potentially be developed into drugs to treat malaria and dengue.
Overall, the researchers concluded that Csp_P’s broad-spectrum antipathogen properties and ability to kill mosquitoes make it a good candidate for the development of novel control strategies for malaria and dengue, so it warrants further study. ![]()

Credit: CDC
A bacterium isolated from a mosquito’s gut could aid the fight against malaria and dengue, according to a study published in PLOS Pathogens.
With previous research, scientists isolated Csp_P, a member of the family of chromobacteria, from the gut of Aedes aegypti mosquitoes.
Now, the team has found that Csp_P can directly inhibit malaria and dengue pathogens in vitro and shorten the life span of the mosquitoes that transmit both diseases.
George Dimopoulos, PhD, of Johns Hopkins University in Baltimore, Maryland, and his colleagues examined Csp_P’s actions on both mosquitoes and pathogens, and the results suggest that Csp_P might help to fight malaria and dengue at different levels.
The researchers added Csp_P to sugar water fed to mosquitoes and found that the bacteria are able to quickly colonize the gut of the two most important mosquito disease vectors—Aedes aegypti and Anopheles gambiae.
Moreover, the presence of Csp_P in the gut reduced the susceptibility of the respective mosquitoes to infection with the malaria parasite Plasmodium falciparum or with dengue virus.
Even without gut colonization, exposure to Csp_P through food or breeding water shortened the lifespan of adult mosquitoes and mosquito larvae of both species.
When the researchers tested whether Csp_P could act against the malaria or dengue pathogens directly, they found that the bacterium, likely through the production of toxic metabolites, can inhibit the growth of Plasmodium at various stages during the parasite’s life cycle and also abolish dengue virus infectivity.
The team said these toxic metabolites could potentially be developed into drugs to treat malaria and dengue.
Overall, the researchers concluded that Csp_P’s broad-spectrum antipathogen properties and ability to kill mosquitoes make it a good candidate for the development of novel control strategies for malaria and dengue, so it warrants further study. ![]()
Team creates functional vascular grafts in a week
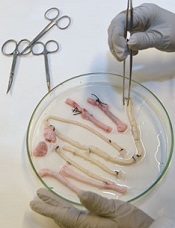
Credit: Robert Emilsson
Researchers have found they can engineer vascular grafts using autologous peripheral blood and successfully transplant them into patients with portal vein thrombosis.
The team said this research provides early evidence for generating personalized blood vessels using stem cells from a blood sample rather than the bone marrow.
Suchitra Sumitran-Holgersson, PhD, of Sahlgrenska University Hospital in Sweden, and her colleagues described the work in EBioMedicine.
The researchers tested their new method on two young children with portal vein thrombosis.
The team used the patients’ own stem cells to grow new blood vessels, a procedure that had been performed at Sahlgrenska University Hospital once before. The novel finding was that they could do this without extracting the cells from the bone marrow.
The researchers took decellularized allogeneic vascular scaffolds and repopulated them with peripheral whole blood in a bioreactor.
The team found they could use 25 mL of blood, the minimum quantity needed to obtain enough stem cells. And the extraction procedure worked the first time.
“Not only that, but the blood itself accelerated growth of the new vein,” Dr Sumitran-Holgersson said. “The entire process took only a week, as opposed to a month in the first case. The blood contains substances that naturally promote growth.”
Dr Sumitran-Holgersson and her colleagues have treated three patients thus far. Two of those patients are still doing well and have veins that are functioning as they should. In the third case, the child is under medical surveillance, and the outcome is more uncertain.
“We believe that this technological progress can lead to dissemination of the method for the benefit of additional groups of patients, such as those with varicose veins or myocardial infarction, who need new blood vessels,” Dr Sumitran-Holgersson said. “Our dream is to be able to grow complete organs as a way of overcoming the current shortage from donors.” ![]()

Credit: Robert Emilsson
Researchers have found they can engineer vascular grafts using autologous peripheral blood and successfully transplant them into patients with portal vein thrombosis.
The team said this research provides early evidence for generating personalized blood vessels using stem cells from a blood sample rather than the bone marrow.
Suchitra Sumitran-Holgersson, PhD, of Sahlgrenska University Hospital in Sweden, and her colleagues described the work in EBioMedicine.
The researchers tested their new method on two young children with portal vein thrombosis.
The team used the patients’ own stem cells to grow new blood vessels, a procedure that had been performed at Sahlgrenska University Hospital once before. The novel finding was that they could do this without extracting the cells from the bone marrow.
The researchers took decellularized allogeneic vascular scaffolds and repopulated them with peripheral whole blood in a bioreactor.
The team found they could use 25 mL of blood, the minimum quantity needed to obtain enough stem cells. And the extraction procedure worked the first time.
“Not only that, but the blood itself accelerated growth of the new vein,” Dr Sumitran-Holgersson said. “The entire process took only a week, as opposed to a month in the first case. The blood contains substances that naturally promote growth.”
Dr Sumitran-Holgersson and her colleagues have treated three patients thus far. Two of those patients are still doing well and have veins that are functioning as they should. In the third case, the child is under medical surveillance, and the outcome is more uncertain.
“We believe that this technological progress can lead to dissemination of the method for the benefit of additional groups of patients, such as those with varicose veins or myocardial infarction, who need new blood vessels,” Dr Sumitran-Holgersson said. “Our dream is to be able to grow complete organs as a way of overcoming the current shortage from donors.” ![]()

Credit: Robert Emilsson
Researchers have found they can engineer vascular grafts using autologous peripheral blood and successfully transplant them into patients with portal vein thrombosis.
The team said this research provides early evidence for generating personalized blood vessels using stem cells from a blood sample rather than the bone marrow.
Suchitra Sumitran-Holgersson, PhD, of Sahlgrenska University Hospital in Sweden, and her colleagues described the work in EBioMedicine.
The researchers tested their new method on two young children with portal vein thrombosis.
The team used the patients’ own stem cells to grow new blood vessels, a procedure that had been performed at Sahlgrenska University Hospital once before. The novel finding was that they could do this without extracting the cells from the bone marrow.
The researchers took decellularized allogeneic vascular scaffolds and repopulated them with peripheral whole blood in a bioreactor.
The team found they could use 25 mL of blood, the minimum quantity needed to obtain enough stem cells. And the extraction procedure worked the first time.
“Not only that, but the blood itself accelerated growth of the new vein,” Dr Sumitran-Holgersson said. “The entire process took only a week, as opposed to a month in the first case. The blood contains substances that naturally promote growth.”
Dr Sumitran-Holgersson and her colleagues have treated three patients thus far. Two of those patients are still doing well and have veins that are functioning as they should. In the third case, the child is under medical surveillance, and the outcome is more uncertain.
“We believe that this technological progress can lead to dissemination of the method for the benefit of additional groups of patients, such as those with varicose veins or myocardial infarction, who need new blood vessels,” Dr Sumitran-Holgersson said. “Our dream is to be able to grow complete organs as a way of overcoming the current shortage from donors.”
Insured cancer patients forgo care, scrimp to get by

cancer patient and her father
Credit: Rhoda Baer
Despite having insurance, many US cancer patients may forgo medical care and change their lifestyles due to treatment-related financial burdens, a new survey suggests.
Nearly 40% of the 174 patients surveyed adopted medical care-altering strategies, such as skipping recommended testing and treatment.
And nearly 9 out of 10 patients made at least one lifestyle change, such as spending less money on food and clothing or selling their possessions.
Prior research has suggested that about 13% of patients suffer from high out-of-pocket financial burden after they are diagnosed with cancer. According to the American Cancer Society, as many as 20% of Americans with cancer spend their life savings to pay for their care.
“We need a better, more open dialogue between patients and providers about the financial burden associated with cancer care costs,” said lead study author Ryan Nipp, MD, of Dana-Farber Cancer Institute in Boston.
“We found that people use a range of different cost-coping strategies, and we need to engage with patients on their choices and develop screening tools to identify patients who are likely to make potentially harmful decisions about their treatment.”
Dr Nipp presented these findings (abstract 161*) in a presscast in advance of the 2014 Palliative Care in Oncology Symposium, which is taking place October 24-25 at the Westin Boston Waterfront in Boston.
The researchers surveyed 174 patients (median age 67, 96% female, 83% white) undergoing treatment for cancer (85% breast, 4% colorectal, 11% other solid tumors). All patients were insured and had requested financial assistance through a national copay assistance program.
Overall, 89% of participants used at least one lifestyle-altering strategy, and 39% used at least one medical care-altering strategy.
The most common medical care-altering strategies were not filling a prescription (28%) and taking less medication than prescribed (22%). Patients also reported skipping tests (10%), forgoing procedures (8%), and missing doctor’s appointments (6%).
Lifestyle-altering strategies included spending less on leisure activities (78%), spending less on basics like food and clothing (57%), borrowing money (54%), spending savings (50%), selling possessions (18%), and having family members work more (15%).
Younger age, higher education, and shorter time on chemotherapy were all associated with a greater likelihood of adopting lifestyle coping strategies compared to older age, lower education, and longer time on chemotherapy.
Younger patients were also more likely to use care-altering strategies compared to older patients. And lower-income patients used more care-altering strategies than higher-income patients.
*Data in the abstract differ from data presented.

cancer patient and her father
Credit: Rhoda Baer
Despite having insurance, many US cancer patients may forgo medical care and change their lifestyles due to treatment-related financial burdens, a new survey suggests.
Nearly 40% of the 174 patients surveyed adopted medical care-altering strategies, such as skipping recommended testing and treatment.
And nearly 9 out of 10 patients made at least one lifestyle change, such as spending less money on food and clothing or selling their possessions.
Prior research has suggested that about 13% of patients suffer from high out-of-pocket financial burden after they are diagnosed with cancer. According to the American Cancer Society, as many as 20% of Americans with cancer spend their life savings to pay for their care.
“We need a better, more open dialogue between patients and providers about the financial burden associated with cancer care costs,” said lead study author Ryan Nipp, MD, of Dana-Farber Cancer Institute in Boston.
“We found that people use a range of different cost-coping strategies, and we need to engage with patients on their choices and develop screening tools to identify patients who are likely to make potentially harmful decisions about their treatment.”
Dr Nipp presented these findings (abstract 161*) in a presscast in advance of the 2014 Palliative Care in Oncology Symposium, which is taking place October 24-25 at the Westin Boston Waterfront in Boston.
The researchers surveyed 174 patients (median age 67, 96% female, 83% white) undergoing treatment for cancer (85% breast, 4% colorectal, 11% other solid tumors). All patients were insured and had requested financial assistance through a national copay assistance program.
Overall, 89% of participants used at least one lifestyle-altering strategy, and 39% used at least one medical care-altering strategy.
The most common medical care-altering strategies were not filling a prescription (28%) and taking less medication than prescribed (22%). Patients also reported skipping tests (10%), forgoing procedures (8%), and missing doctor’s appointments (6%).
Lifestyle-altering strategies included spending less on leisure activities (78%), spending less on basics like food and clothing (57%), borrowing money (54%), spending savings (50%), selling possessions (18%), and having family members work more (15%).
Younger age, higher education, and shorter time on chemotherapy were all associated with a greater likelihood of adopting lifestyle coping strategies compared to older age, lower education, and longer time on chemotherapy.
Younger patients were also more likely to use care-altering strategies compared to older patients. And lower-income patients used more care-altering strategies than higher-income patients.
*Data in the abstract differ from data presented.

cancer patient and her father
Credit: Rhoda Baer
Despite having insurance, many US cancer patients may forgo medical care and change their lifestyles due to treatment-related financial burdens, a new survey suggests.
Nearly 40% of the 174 patients surveyed adopted medical care-altering strategies, such as skipping recommended testing and treatment.
And nearly 9 out of 10 patients made at least one lifestyle change, such as spending less money on food and clothing or selling their possessions.
Prior research has suggested that about 13% of patients suffer from high out-of-pocket financial burden after they are diagnosed with cancer. According to the American Cancer Society, as many as 20% of Americans with cancer spend their life savings to pay for their care.
“We need a better, more open dialogue between patients and providers about the financial burden associated with cancer care costs,” said lead study author Ryan Nipp, MD, of Dana-Farber Cancer Institute in Boston.
“We found that people use a range of different cost-coping strategies, and we need to engage with patients on their choices and develop screening tools to identify patients who are likely to make potentially harmful decisions about their treatment.”
Dr Nipp presented these findings (abstract 161*) in a presscast in advance of the 2014 Palliative Care in Oncology Symposium, which is taking place October 24-25 at the Westin Boston Waterfront in Boston.
The researchers surveyed 174 patients (median age 67, 96% female, 83% white) undergoing treatment for cancer (85% breast, 4% colorectal, 11% other solid tumors). All patients were insured and had requested financial assistance through a national copay assistance program.
Overall, 89% of participants used at least one lifestyle-altering strategy, and 39% used at least one medical care-altering strategy.
The most common medical care-altering strategies were not filling a prescription (28%) and taking less medication than prescribed (22%). Patients also reported skipping tests (10%), forgoing procedures (8%), and missing doctor’s appointments (6%).
Lifestyle-altering strategies included spending less on leisure activities (78%), spending less on basics like food and clothing (57%), borrowing money (54%), spending savings (50%), selling possessions (18%), and having family members work more (15%).
Younger age, higher education, and shorter time on chemotherapy were all associated with a greater likelihood of adopting lifestyle coping strategies compared to older age, lower education, and longer time on chemotherapy.
Younger patients were also more likely to use care-altering strategies compared to older patients. And lower-income patients used more care-altering strategies than higher-income patients.
*Data in the abstract differ from data presented.
Patients in GDR trials were not properly informed

Credit: Esther Dyson
New research has shown that clinical trials carried out in the German Democratic Republic (GDR) in the second half of the 20th century were not always conducted with the full knowledge or understanding of participants.
A review of documents from that time suggests that, although questionable practices took place, the GDR attempted to conduct trials according to international ethical standards.
And there was no evidence to suggest that trial investigators intentionally hurt patients.
Nevertheless, these trials were hidden from the public, there was no record of patient consent, and some documents suggest patients did not receive adequate information.
Dr Rainer Erices, of Friedrich-Alexander-Universität Erlangen-Nuernberg in Germany, and his colleagues detailed these findings in the Journal of Medical Ethics.
The GDR, also known as East Germany, was a state within the Eastern Bloc during the Cold War period and between 1949 and 1990. Since the 1990s, the media has reported that unofficial clinical trials were conducted by Western pharmaceutical companies in East Germany from the 1960s onward.
Reports have suggested the GDR “sold” its patients as “guinea pigs” for experiments in exchange for hard currency; for example, for tests on doping effects in premature babies and on treating seriously ill patients with placebo instead of actual medicine.
However, there is still a lack of reliable data about the extent of studies taking place then, the contracts, the amount of money paid, and more moral issues, such as patient education and informed consent.
Dr Erices and his colleagues set out to uncover more information by evaluating the clinical trials based on archival material from the health system and the secret service.
The team found documents related to 220 trials carried out between 1983 and 1990, which involved more than 14,000 patients and 68 Western pharmaceutical companies.
However, there was no record of patient information forms or systematic documentation regarding the provision of patient consent.
A range of drugs were tested in these studies, including chemotherapeutic agents, heparin, insulin, anti-depressants, anti-allergy drugs, contrast agents, and toothpastes.
Between 1983 and 1990, the GDR’s health system received approximately DM 16.5 million for the trials, which were cost-effective for the drug firms, according to the researchers. The team also noted that the GDR agreed to these trials due to its desperate need for hard currency (impending bankruptcy).
Overall, the files the researchers studied suggested that the GDR attempted to conduct trials according to international ethical standards.
However, the trials were concealed from the public. And state legislation stipulated that patients had to consent to the trials, but no evidence was found to suggest that patients were systematically informed.
Some documents suggested that at least some of the trials were carried out without patients having a comprehensive understanding of what the trial involved. And it was unclear whether the patients themselves knew that they were participating in trials and were aware of all the risks.
The researchers concluded that further investigation of these trials is needed, and specific trials should be studied separately.

Credit: Esther Dyson
New research has shown that clinical trials carried out in the German Democratic Republic (GDR) in the second half of the 20th century were not always conducted with the full knowledge or understanding of participants.
A review of documents from that time suggests that, although questionable practices took place, the GDR attempted to conduct trials according to international ethical standards.
And there was no evidence to suggest that trial investigators intentionally hurt patients.
Nevertheless, these trials were hidden from the public, there was no record of patient consent, and some documents suggest patients did not receive adequate information.
Dr Rainer Erices, of Friedrich-Alexander-Universität Erlangen-Nuernberg in Germany, and his colleagues detailed these findings in the Journal of Medical Ethics.
The GDR, also known as East Germany, was a state within the Eastern Bloc during the Cold War period and between 1949 and 1990. Since the 1990s, the media has reported that unofficial clinical trials were conducted by Western pharmaceutical companies in East Germany from the 1960s onward.
Reports have suggested the GDR “sold” its patients as “guinea pigs” for experiments in exchange for hard currency; for example, for tests on doping effects in premature babies and on treating seriously ill patients with placebo instead of actual medicine.
However, there is still a lack of reliable data about the extent of studies taking place then, the contracts, the amount of money paid, and more moral issues, such as patient education and informed consent.
Dr Erices and his colleagues set out to uncover more information by evaluating the clinical trials based on archival material from the health system and the secret service.
The team found documents related to 220 trials carried out between 1983 and 1990, which involved more than 14,000 patients and 68 Western pharmaceutical companies.
However, there was no record of patient information forms or systematic documentation regarding the provision of patient consent.
A range of drugs were tested in these studies, including chemotherapeutic agents, heparin, insulin, anti-depressants, anti-allergy drugs, contrast agents, and toothpastes.
Between 1983 and 1990, the GDR’s health system received approximately DM 16.5 million for the trials, which were cost-effective for the drug firms, according to the researchers. The team also noted that the GDR agreed to these trials due to its desperate need for hard currency (impending bankruptcy).
Overall, the files the researchers studied suggested that the GDR attempted to conduct trials according to international ethical standards.
However, the trials were concealed from the public. And state legislation stipulated that patients had to consent to the trials, but no evidence was found to suggest that patients were systematically informed.
Some documents suggested that at least some of the trials were carried out without patients having a comprehensive understanding of what the trial involved. And it was unclear whether the patients themselves knew that they were participating in trials and were aware of all the risks.
The researchers concluded that further investigation of these trials is needed, and specific trials should be studied separately.

Credit: Esther Dyson
New research has shown that clinical trials carried out in the German Democratic Republic (GDR) in the second half of the 20th century were not always conducted with the full knowledge or understanding of participants.
A review of documents from that time suggests that, although questionable practices took place, the GDR attempted to conduct trials according to international ethical standards.
And there was no evidence to suggest that trial investigators intentionally hurt patients.
Nevertheless, these trials were hidden from the public, there was no record of patient consent, and some documents suggest patients did not receive adequate information.
Dr Rainer Erices, of Friedrich-Alexander-Universität Erlangen-Nuernberg in Germany, and his colleagues detailed these findings in the Journal of Medical Ethics.
The GDR, also known as East Germany, was a state within the Eastern Bloc during the Cold War period and between 1949 and 1990. Since the 1990s, the media has reported that unofficial clinical trials were conducted by Western pharmaceutical companies in East Germany from the 1960s onward.
Reports have suggested the GDR “sold” its patients as “guinea pigs” for experiments in exchange for hard currency; for example, for tests on doping effects in premature babies and on treating seriously ill patients with placebo instead of actual medicine.
However, there is still a lack of reliable data about the extent of studies taking place then, the contracts, the amount of money paid, and more moral issues, such as patient education and informed consent.
Dr Erices and his colleagues set out to uncover more information by evaluating the clinical trials based on archival material from the health system and the secret service.
The team found documents related to 220 trials carried out between 1983 and 1990, which involved more than 14,000 patients and 68 Western pharmaceutical companies.
However, there was no record of patient information forms or systematic documentation regarding the provision of patient consent.
A range of drugs were tested in these studies, including chemotherapeutic agents, heparin, insulin, anti-depressants, anti-allergy drugs, contrast agents, and toothpastes.
Between 1983 and 1990, the GDR’s health system received approximately DM 16.5 million for the trials, which were cost-effective for the drug firms, according to the researchers. The team also noted that the GDR agreed to these trials due to its desperate need for hard currency (impending bankruptcy).
Overall, the files the researchers studied suggested that the GDR attempted to conduct trials according to international ethical standards.
However, the trials were concealed from the public. And state legislation stipulated that patients had to consent to the trials, but no evidence was found to suggest that patients were systematically informed.
Some documents suggested that at least some of the trials were carried out without patients having a comprehensive understanding of what the trial involved. And it was unclear whether the patients themselves knew that they were participating in trials and were aware of all the risks.
The researchers concluded that further investigation of these trials is needed, and specific trials should be studied separately.
Cancer survivors face financial, work-related issues

chemotherapy
Credit: Rhoda Baer
Many US cancer survivors may be experiencing financial or work-related hardship, a new survey suggests.
Twenty-seven percent of the nearly 1600 survivors surveyed reported at least one financial problem, such as debt or bankruptcy.
And 37% reported having to modify work plans, such as taking extended time off or delaying retirement.
Women, younger survivors, racial/ethnic minorities, and uninsured survivors were all disproportionally burdened by these challenges.
This research (abstract 238*) was presented in a presscast prior to the 2014 Palliative Care in Oncology Symposium, which is scheduled to take place October 24-25 at the Westin Boston Waterfront in Boston.
“We found that many cancer survivors, particularly those who are younger or from underserved populations, experience financial or work-related hardship—even when insured and years out from treatment,” said lead study author Robin Whitney, RN, a cancer survivor and PhD student at the Betty Irene Moore School of Nursing at the University of California, Davis.
“Addressing these challenges is an important aspect of providing quality cancer care, because they can substantially impact quality of life and health outcomes.”
Whitney and her colleagues focused this study on a subset of individuals surveyed in a larger study (2011 Medical Expenditures Panel Survey Experiences with Cancer Survivorship Supplement).
Among the 1592 survivors surveyed, 47% were younger than 65 years of age, 56% were female, 88% were white, and 4% were uninsured. Fourteen percent were in active treatment, 46% were less than 5 years post-treatment, and 39% were 5 years or more post-treatment.
Overall, 27% of those surveyed reported at least one financial difficulty, such as debt, bankruptcy, and worrying about medical bills. Patients in active treatment reported 120% more financial difficulties than survivors who were less than 5 years post-treatment.
Individuals younger than 65 reported 130% more financial difficulties than older survivors. Survivors without insurance had 67% more difficulties than those with insurance. And minorities had 42% more financial difficulties than whites.
In all, 37% of survivors reported making at least one work modification due to their cancer diagnosis, such as changing to a flexible schedule or less demanding job, early or delayed retirement, and extended or unpaid time off.
Women were significantly more likely than men to make at least one work modification. Patients in active treatment made 120% more work modifications than survivors who were less than 5 years post-treatment. And minorities made 57% more modifications than whites.
According to the researchers, these findings are generalizable to the US population and point to the urgent need for screening and support for financial and work challenges across the cancer survivorship trajectory, from diagnosis to long-term survivorship.
*Information presented differs from that in the abstract.

chemotherapy
Credit: Rhoda Baer
Many US cancer survivors may be experiencing financial or work-related hardship, a new survey suggests.
Twenty-seven percent of the nearly 1600 survivors surveyed reported at least one financial problem, such as debt or bankruptcy.
And 37% reported having to modify work plans, such as taking extended time off or delaying retirement.
Women, younger survivors, racial/ethnic minorities, and uninsured survivors were all disproportionally burdened by these challenges.
This research (abstract 238*) was presented in a presscast prior to the 2014 Palliative Care in Oncology Symposium, which is scheduled to take place October 24-25 at the Westin Boston Waterfront in Boston.
“We found that many cancer survivors, particularly those who are younger or from underserved populations, experience financial or work-related hardship—even when insured and years out from treatment,” said lead study author Robin Whitney, RN, a cancer survivor and PhD student at the Betty Irene Moore School of Nursing at the University of California, Davis.
“Addressing these challenges is an important aspect of providing quality cancer care, because they can substantially impact quality of life and health outcomes.”
Whitney and her colleagues focused this study on a subset of individuals surveyed in a larger study (2011 Medical Expenditures Panel Survey Experiences with Cancer Survivorship Supplement).
Among the 1592 survivors surveyed, 47% were younger than 65 years of age, 56% were female, 88% were white, and 4% were uninsured. Fourteen percent were in active treatment, 46% were less than 5 years post-treatment, and 39% were 5 years or more post-treatment.
Overall, 27% of those surveyed reported at least one financial difficulty, such as debt, bankruptcy, and worrying about medical bills. Patients in active treatment reported 120% more financial difficulties than survivors who were less than 5 years post-treatment.
Individuals younger than 65 reported 130% more financial difficulties than older survivors. Survivors without insurance had 67% more difficulties than those with insurance. And minorities had 42% more financial difficulties than whites.
In all, 37% of survivors reported making at least one work modification due to their cancer diagnosis, such as changing to a flexible schedule or less demanding job, early or delayed retirement, and extended or unpaid time off.
Women were significantly more likely than men to make at least one work modification. Patients in active treatment made 120% more work modifications than survivors who were less than 5 years post-treatment. And minorities made 57% more modifications than whites.
According to the researchers, these findings are generalizable to the US population and point to the urgent need for screening and support for financial and work challenges across the cancer survivorship trajectory, from diagnosis to long-term survivorship.
*Information presented differs from that in the abstract.

chemotherapy
Credit: Rhoda Baer
Many US cancer survivors may be experiencing financial or work-related hardship, a new survey suggests.
Twenty-seven percent of the nearly 1600 survivors surveyed reported at least one financial problem, such as debt or bankruptcy.
And 37% reported having to modify work plans, such as taking extended time off or delaying retirement.
Women, younger survivors, racial/ethnic minorities, and uninsured survivors were all disproportionally burdened by these challenges.
This research (abstract 238*) was presented in a presscast prior to the 2014 Palliative Care in Oncology Symposium, which is scheduled to take place October 24-25 at the Westin Boston Waterfront in Boston.
“We found that many cancer survivors, particularly those who are younger or from underserved populations, experience financial or work-related hardship—even when insured and years out from treatment,” said lead study author Robin Whitney, RN, a cancer survivor and PhD student at the Betty Irene Moore School of Nursing at the University of California, Davis.
“Addressing these challenges is an important aspect of providing quality cancer care, because they can substantially impact quality of life and health outcomes.”
Whitney and her colleagues focused this study on a subset of individuals surveyed in a larger study (2011 Medical Expenditures Panel Survey Experiences with Cancer Survivorship Supplement).
Among the 1592 survivors surveyed, 47% were younger than 65 years of age, 56% were female, 88% were white, and 4% were uninsured. Fourteen percent were in active treatment, 46% were less than 5 years post-treatment, and 39% were 5 years or more post-treatment.
Overall, 27% of those surveyed reported at least one financial difficulty, such as debt, bankruptcy, and worrying about medical bills. Patients in active treatment reported 120% more financial difficulties than survivors who were less than 5 years post-treatment.
Individuals younger than 65 reported 130% more financial difficulties than older survivors. Survivors without insurance had 67% more difficulties than those with insurance. And minorities had 42% more financial difficulties than whites.
In all, 37% of survivors reported making at least one work modification due to their cancer diagnosis, such as changing to a flexible schedule or less demanding job, early or delayed retirement, and extended or unpaid time off.
Women were significantly more likely than men to make at least one work modification. Patients in active treatment made 120% more work modifications than survivors who were less than 5 years post-treatment. And minorities made 57% more modifications than whites.
According to the researchers, these findings are generalizable to the US population and point to the urgent need for screening and support for financial and work challenges across the cancer survivorship trajectory, from diagnosis to long-term survivorship.
*Information presented differs from that in the abstract.