User login
Healthcare pricing transparency may have pros and cons

Credit: Rhoda Baer
Searching a health service pricing website prior to receiving medical care can reduce patients’ payments, but it may have negative effects as well, researchers have reported in JAMA.
Their study showed that searching the website allowed patients to pay lower prices for clinical services such as advanced imaging and lab tests.
However, the researchers suggested that knowing the price of services ahead of time may prompt some patients to forgo care.
And although cost savings from price shopping might lead to improved treatment adherence, it might also lead to overuse of services.
Neeraj Sood, PhD, of the University of Southern California in Los Angeles, and his colleagues examined the association between price availability and the total claims payments (the total amount paid by patient and insurer) for lab tests, advanced imaging services, and clinician office visits.
The researchers compared payments made by patients who searched a pricing website before using a service to patients who had not researched pricing. The team analyzed medical claims data from 2010 to 2013. This included 502,949 patients who were insured in the US by 18 employers who provided a price transparency platform to their employees.
Patients with access to the pricing website 14 days before receiving care had lower claim payments than those who did not. Adjusted payments were approximately 14% lower for lab tests, 13% lower for advanced imaging, and 1% lower for clinician office visits.
The relative differences translated into lower absolute dollar payments of $3.45 for lab tests, $124.74 for advanced imaging, and $1.18 for clinician office visits.
In the period before either group had access to the pricing website, payments for searchers were about 4% higher for lab tests and 6% higher for advanced imaging but 0.26% lower for office visits than for nonsearchers.
The researchers said future studies should evaluate services beyond those examined in this study. They should also examine how the use of care is affected to better understand the broader effect of price transparency on healthcare spending and population health.
This study was published alongside a related editorial. ![]()

Credit: Rhoda Baer
Searching a health service pricing website prior to receiving medical care can reduce patients’ payments, but it may have negative effects as well, researchers have reported in JAMA.
Their study showed that searching the website allowed patients to pay lower prices for clinical services such as advanced imaging and lab tests.
However, the researchers suggested that knowing the price of services ahead of time may prompt some patients to forgo care.
And although cost savings from price shopping might lead to improved treatment adherence, it might also lead to overuse of services.
Neeraj Sood, PhD, of the University of Southern California in Los Angeles, and his colleagues examined the association between price availability and the total claims payments (the total amount paid by patient and insurer) for lab tests, advanced imaging services, and clinician office visits.
The researchers compared payments made by patients who searched a pricing website before using a service to patients who had not researched pricing. The team analyzed medical claims data from 2010 to 2013. This included 502,949 patients who were insured in the US by 18 employers who provided a price transparency platform to their employees.
Patients with access to the pricing website 14 days before receiving care had lower claim payments than those who did not. Adjusted payments were approximately 14% lower for lab tests, 13% lower for advanced imaging, and 1% lower for clinician office visits.
The relative differences translated into lower absolute dollar payments of $3.45 for lab tests, $124.74 for advanced imaging, and $1.18 for clinician office visits.
In the period before either group had access to the pricing website, payments for searchers were about 4% higher for lab tests and 6% higher for advanced imaging but 0.26% lower for office visits than for nonsearchers.
The researchers said future studies should evaluate services beyond those examined in this study. They should also examine how the use of care is affected to better understand the broader effect of price transparency on healthcare spending and population health.
This study was published alongside a related editorial. ![]()

Credit: Rhoda Baer
Searching a health service pricing website prior to receiving medical care can reduce patients’ payments, but it may have negative effects as well, researchers have reported in JAMA.
Their study showed that searching the website allowed patients to pay lower prices for clinical services such as advanced imaging and lab tests.
However, the researchers suggested that knowing the price of services ahead of time may prompt some patients to forgo care.
And although cost savings from price shopping might lead to improved treatment adherence, it might also lead to overuse of services.
Neeraj Sood, PhD, of the University of Southern California in Los Angeles, and his colleagues examined the association between price availability and the total claims payments (the total amount paid by patient and insurer) for lab tests, advanced imaging services, and clinician office visits.
The researchers compared payments made by patients who searched a pricing website before using a service to patients who had not researched pricing. The team analyzed medical claims data from 2010 to 2013. This included 502,949 patients who were insured in the US by 18 employers who provided a price transparency platform to their employees.
Patients with access to the pricing website 14 days before receiving care had lower claim payments than those who did not. Adjusted payments were approximately 14% lower for lab tests, 13% lower for advanced imaging, and 1% lower for clinician office visits.
The relative differences translated into lower absolute dollar payments of $3.45 for lab tests, $124.74 for advanced imaging, and $1.18 for clinician office visits.
In the period before either group had access to the pricing website, payments for searchers were about 4% higher for lab tests and 6% higher for advanced imaging but 0.26% lower for office visits than for nonsearchers.
The researchers said future studies should evaluate services beyond those examined in this study. They should also examine how the use of care is affected to better understand the broader effect of price transparency on healthcare spending and population health.
This study was published alongside a related editorial. ![]()
Supercomputers can predict drugs’ side effects

Credit: FDA
Scientists have found they can use supercomputers to identify proteins that cause adverse drug reactions.
The team noted that, during the drug development process, researchers often miss side effects that kill at least 100,000 patients a year.
In PLOS ONE, Montiago LaBute, PhD, of Lawrence Livermore National Laboratory in California, and his colleagues explained how we might use high-performance computers to solve this problem.
Side effects go undetected during drug development
A typical drug discovery process begins with identifying which proteins are associated with a specific disease. Candidate drug compounds are combined with target proteins to determine the drug’s efficacy and toxicity.
While this method allows researchers to identify side effects with many target proteins, there are myriad unknown, off-target proteins that may bind to the candidate drug and could cause unanticipated side effects.
Because it is cost-prohibitive to experimentally test a drug candidate against a potentially large set of proteins—and the list of possible off-targets is not known ahead of time—pharmaceutical companies usually only test a minimal set of off-target proteins during the early stages of drug discovery.
So certain adverse drug reactions remain undetected through the later stages of drug development, and the drugs may make it to the marketplace before these reactions are detected.
There have been several highly publicized medications with off-target protein side effects that have reached the marketplace. For example, Avandia, an anti-diabetic drug, caused heart attacks in some patients.
And Vioxx, an anti-inflammatory medication, caused heart attacks and strokes in certain patient populations. Both drugs were recalled because of their side effects.
“There were no indications of side effects of these medications in early testing or clinical trials,” Dr LaBute said. “We need a way to determine the safety of such therapeutics before they reach patients. Our work can help direct such drugs to patients who will benefit the most from them with the least amount of side effects.”
Supercomputers predict adverse drug reactions
Dr LaBute and colleagues tackled the problem by using supercomputers and information from public databases of drug compounds and proteins.
The databases included DrugBank, UniProt, and Protein Data Bank (PDB), as well as drug databases from the US Food and Drug Administration (FDA) and SIDER, which contain FDA-approved drugs with adverse drug reactions.
The team examined 4020 off-target proteins from DrugBank and UniProt. Those proteins were indexed against the PDB, which whittled the number down to 409 off-proteins that have high-quality 3D crystallographic X-ray diffraction structures essential for analysis in a computational setting.
The researchers fed the 409 off-target proteins into high-performance computer software known as VinaLC, along with 906 FDA-approved drug compounds. VinaLC used a molecular docking matrix that bound the drugs to the proteins. A score was given to each combination to assess whether effective binding occurred.
The team fed binding scores into another computer program and combined them with 560 FDA-approved drugs with known side effects. They used an algorithm to determine which proteins were associated with certain side effects.
In two categories of disorders—vascular disorders and neoplasms—the researchers’ computational model of predicting side effects was more predictive than current statistical methods that do not include binding scores.
In addition, the team’s calculations predicted new potential side effects. For example, they predicted a connection between a protein normally associated with cancer metastasis to vascular disorders like aneurysms.
“We have discovered a very viable way to find off-target proteins that are important for side effects,” Dr LaBute said. “This approach using [high-powered computers] and molecular docking to find [adverse drug reactions] never really existed before.”
The team’s findings provide drug companies with a cost-effective and reliable method to screen for side effects, according to Dr LaBute. Now, his group’s goal is to expand their computational pharmaceutical research to include more off-target proteins for testing and eventually screen every protein in the body.
“If we can do that, the drugs of tomorrow will have less side effects that can potentially lead to fatalities,” Dr Labute said. “Optimistically, we could be a decade away from our ultimate goal. However, we need help from pharmaceutical companies, healthcare providers, and the FDA to provide us with patient and therapeutic data.” ![]()

Credit: FDA
Scientists have found they can use supercomputers to identify proteins that cause adverse drug reactions.
The team noted that, during the drug development process, researchers often miss side effects that kill at least 100,000 patients a year.
In PLOS ONE, Montiago LaBute, PhD, of Lawrence Livermore National Laboratory in California, and his colleagues explained how we might use high-performance computers to solve this problem.
Side effects go undetected during drug development
A typical drug discovery process begins with identifying which proteins are associated with a specific disease. Candidate drug compounds are combined with target proteins to determine the drug’s efficacy and toxicity.
While this method allows researchers to identify side effects with many target proteins, there are myriad unknown, off-target proteins that may bind to the candidate drug and could cause unanticipated side effects.
Because it is cost-prohibitive to experimentally test a drug candidate against a potentially large set of proteins—and the list of possible off-targets is not known ahead of time—pharmaceutical companies usually only test a minimal set of off-target proteins during the early stages of drug discovery.
So certain adverse drug reactions remain undetected through the later stages of drug development, and the drugs may make it to the marketplace before these reactions are detected.
There have been several highly publicized medications with off-target protein side effects that have reached the marketplace. For example, Avandia, an anti-diabetic drug, caused heart attacks in some patients.
And Vioxx, an anti-inflammatory medication, caused heart attacks and strokes in certain patient populations. Both drugs were recalled because of their side effects.
“There were no indications of side effects of these medications in early testing or clinical trials,” Dr LaBute said. “We need a way to determine the safety of such therapeutics before they reach patients. Our work can help direct such drugs to patients who will benefit the most from them with the least amount of side effects.”
Supercomputers predict adverse drug reactions
Dr LaBute and colleagues tackled the problem by using supercomputers and information from public databases of drug compounds and proteins.
The databases included DrugBank, UniProt, and Protein Data Bank (PDB), as well as drug databases from the US Food and Drug Administration (FDA) and SIDER, which contain FDA-approved drugs with adverse drug reactions.
The team examined 4020 off-target proteins from DrugBank and UniProt. Those proteins were indexed against the PDB, which whittled the number down to 409 off-proteins that have high-quality 3D crystallographic X-ray diffraction structures essential for analysis in a computational setting.
The researchers fed the 409 off-target proteins into high-performance computer software known as VinaLC, along with 906 FDA-approved drug compounds. VinaLC used a molecular docking matrix that bound the drugs to the proteins. A score was given to each combination to assess whether effective binding occurred.
The team fed binding scores into another computer program and combined them with 560 FDA-approved drugs with known side effects. They used an algorithm to determine which proteins were associated with certain side effects.
In two categories of disorders—vascular disorders and neoplasms—the researchers’ computational model of predicting side effects was more predictive than current statistical methods that do not include binding scores.
In addition, the team’s calculations predicted new potential side effects. For example, they predicted a connection between a protein normally associated with cancer metastasis to vascular disorders like aneurysms.
“We have discovered a very viable way to find off-target proteins that are important for side effects,” Dr LaBute said. “This approach using [high-powered computers] and molecular docking to find [adverse drug reactions] never really existed before.”
The team’s findings provide drug companies with a cost-effective and reliable method to screen for side effects, according to Dr LaBute. Now, his group’s goal is to expand their computational pharmaceutical research to include more off-target proteins for testing and eventually screen every protein in the body.
“If we can do that, the drugs of tomorrow will have less side effects that can potentially lead to fatalities,” Dr Labute said. “Optimistically, we could be a decade away from our ultimate goal. However, we need help from pharmaceutical companies, healthcare providers, and the FDA to provide us with patient and therapeutic data.” ![]()

Credit: FDA
Scientists have found they can use supercomputers to identify proteins that cause adverse drug reactions.
The team noted that, during the drug development process, researchers often miss side effects that kill at least 100,000 patients a year.
In PLOS ONE, Montiago LaBute, PhD, of Lawrence Livermore National Laboratory in California, and his colleagues explained how we might use high-performance computers to solve this problem.
Side effects go undetected during drug development
A typical drug discovery process begins with identifying which proteins are associated with a specific disease. Candidate drug compounds are combined with target proteins to determine the drug’s efficacy and toxicity.
While this method allows researchers to identify side effects with many target proteins, there are myriad unknown, off-target proteins that may bind to the candidate drug and could cause unanticipated side effects.
Because it is cost-prohibitive to experimentally test a drug candidate against a potentially large set of proteins—and the list of possible off-targets is not known ahead of time—pharmaceutical companies usually only test a minimal set of off-target proteins during the early stages of drug discovery.
So certain adverse drug reactions remain undetected through the later stages of drug development, and the drugs may make it to the marketplace before these reactions are detected.
There have been several highly publicized medications with off-target protein side effects that have reached the marketplace. For example, Avandia, an anti-diabetic drug, caused heart attacks in some patients.
And Vioxx, an anti-inflammatory medication, caused heart attacks and strokes in certain patient populations. Both drugs were recalled because of their side effects.
“There were no indications of side effects of these medications in early testing or clinical trials,” Dr LaBute said. “We need a way to determine the safety of such therapeutics before they reach patients. Our work can help direct such drugs to patients who will benefit the most from them with the least amount of side effects.”
Supercomputers predict adverse drug reactions
Dr LaBute and colleagues tackled the problem by using supercomputers and information from public databases of drug compounds and proteins.
The databases included DrugBank, UniProt, and Protein Data Bank (PDB), as well as drug databases from the US Food and Drug Administration (FDA) and SIDER, which contain FDA-approved drugs with adverse drug reactions.
The team examined 4020 off-target proteins from DrugBank and UniProt. Those proteins were indexed against the PDB, which whittled the number down to 409 off-proteins that have high-quality 3D crystallographic X-ray diffraction structures essential for analysis in a computational setting.
The researchers fed the 409 off-target proteins into high-performance computer software known as VinaLC, along with 906 FDA-approved drug compounds. VinaLC used a molecular docking matrix that bound the drugs to the proteins. A score was given to each combination to assess whether effective binding occurred.
The team fed binding scores into another computer program and combined them with 560 FDA-approved drugs with known side effects. They used an algorithm to determine which proteins were associated with certain side effects.
In two categories of disorders—vascular disorders and neoplasms—the researchers’ computational model of predicting side effects was more predictive than current statistical methods that do not include binding scores.
In addition, the team’s calculations predicted new potential side effects. For example, they predicted a connection between a protein normally associated with cancer metastasis to vascular disorders like aneurysms.
“We have discovered a very viable way to find off-target proteins that are important for side effects,” Dr LaBute said. “This approach using [high-powered computers] and molecular docking to find [adverse drug reactions] never really existed before.”
The team’s findings provide drug companies with a cost-effective and reliable method to screen for side effects, according to Dr LaBute. Now, his group’s goal is to expand their computational pharmaceutical research to include more off-target proteins for testing and eventually screen every protein in the body.
“If we can do that, the drugs of tomorrow will have less side effects that can potentially lead to fatalities,” Dr Labute said. “Optimistically, we could be a decade away from our ultimate goal. However, we need help from pharmaceutical companies, healthcare providers, and the FDA to provide us with patient and therapeutic data.” ![]()
Collaborative cancer care cuts readmission rates

while another looks on
Credit: NCI
A “co-rounding” partnership between medical oncologists and palliative care specialists has shown improvements in health-system and patient-related outcomes.
The first year of the partnership, which was tested in Duke University Hospital’s solid tumor oncology unit, brought significant decreases in the average length of hospital stay and in readmission rates, compared to a previous year in which the partnership did not exist.
There was a decrease in intensive care unit transfers and a trend toward increased hospice referrals as well, although these differences were not significant.
“The integration of palliative care, as a necessary and essential component of cancer care, is one that has been increasingly endorsed," said Richard Riedel, MD, of Duke University Hospital in Durham, North Carolina.
“The benefits of palliative care have been shown in the outpatient and consultative settings, but we didn’t know its impact on daily inpatient care. Now, we have successfully partnered with our palliative care colleagues to bring their unique skill sets and expertise directly to our admitted patients, and have shown it to be beneficial.”
Dr Riedel described this research (abstract 3*) in a presscast prior to the 2014 Palliative Care in Oncology Symposium, which is scheduled to take place October 24-25 at the Westin Boston Waterfront in Boston.
The co-rounding partnership involves 3 formal meetings each day in which members of the team, including both the attending medical oncologist and the attending palliative care physician, discuss all patients in the solid tumor unit.
The team decides which attending physician oversees direct care for a patient depending on his or her needs. For example, patients with higher symptom burden are typically assigned to the palliative care specialists.
The hospital support staff (eg, internal medicine house staff, physician assistants, and pharmacists) round with both attending physicians, and this care model allows for both formal and informal consultation between specialties.
To evaluate the effects of this model, the researchers assessed outcomes among the 731 patients admitted before the intervention began and 783 admitted in the first year of the intervention. About three-quarters of patients in both groups had metastatic cancer.
The team found a significant decrease in the average length of hospital stay from the pre-intervention period to the post-intervention period—4.51 days and 4.16 days, respectively (P=0.02).
Likewise, there was a significant decrease in readmission rates. There was 23% relative reduction in 7-day readmission rates (P<0.0001) and a 12% relative reduction in 30-day readmission rates (P=0.048).
Patient transfers to the intensive care unit decreased by 15% post-intervention, and hospice referrals increased by 17%, but these effects were not statistically significant (P=0.64 and 0.09, respectively).
The researchers said these results emphasize the value of implementing palliative medicine soon after a cancer diagnosis, rather than waiting until later in the disease’s progression.
Due to positive results with the co-rounding partnership, Duke University Hospital has established new outpatient palliative care clinics in oncology and general medicine.
The researchers are planning future studies to assess longer-term effects of the intervention on both patient and health-system outcomes, evaluate patient satisfaction, and explore potential cost savings associated with this intervention. ![]()
*Data presented differ from data in the abstract.

while another looks on
Credit: NCI
A “co-rounding” partnership between medical oncologists and palliative care specialists has shown improvements in health-system and patient-related outcomes.
The first year of the partnership, which was tested in Duke University Hospital’s solid tumor oncology unit, brought significant decreases in the average length of hospital stay and in readmission rates, compared to a previous year in which the partnership did not exist.
There was a decrease in intensive care unit transfers and a trend toward increased hospice referrals as well, although these differences were not significant.
“The integration of palliative care, as a necessary and essential component of cancer care, is one that has been increasingly endorsed," said Richard Riedel, MD, of Duke University Hospital in Durham, North Carolina.
“The benefits of palliative care have been shown in the outpatient and consultative settings, but we didn’t know its impact on daily inpatient care. Now, we have successfully partnered with our palliative care colleagues to bring their unique skill sets and expertise directly to our admitted patients, and have shown it to be beneficial.”
Dr Riedel described this research (abstract 3*) in a presscast prior to the 2014 Palliative Care in Oncology Symposium, which is scheduled to take place October 24-25 at the Westin Boston Waterfront in Boston.
The co-rounding partnership involves 3 formal meetings each day in which members of the team, including both the attending medical oncologist and the attending palliative care physician, discuss all patients in the solid tumor unit.
The team decides which attending physician oversees direct care for a patient depending on his or her needs. For example, patients with higher symptom burden are typically assigned to the palliative care specialists.
The hospital support staff (eg, internal medicine house staff, physician assistants, and pharmacists) round with both attending physicians, and this care model allows for both formal and informal consultation between specialties.
To evaluate the effects of this model, the researchers assessed outcomes among the 731 patients admitted before the intervention began and 783 admitted in the first year of the intervention. About three-quarters of patients in both groups had metastatic cancer.
The team found a significant decrease in the average length of hospital stay from the pre-intervention period to the post-intervention period—4.51 days and 4.16 days, respectively (P=0.02).
Likewise, there was a significant decrease in readmission rates. There was 23% relative reduction in 7-day readmission rates (P<0.0001) and a 12% relative reduction in 30-day readmission rates (P=0.048).
Patient transfers to the intensive care unit decreased by 15% post-intervention, and hospice referrals increased by 17%, but these effects were not statistically significant (P=0.64 and 0.09, respectively).
The researchers said these results emphasize the value of implementing palliative medicine soon after a cancer diagnosis, rather than waiting until later in the disease’s progression.
Due to positive results with the co-rounding partnership, Duke University Hospital has established new outpatient palliative care clinics in oncology and general medicine.
The researchers are planning future studies to assess longer-term effects of the intervention on both patient and health-system outcomes, evaluate patient satisfaction, and explore potential cost savings associated with this intervention. ![]()
*Data presented differ from data in the abstract.

while another looks on
Credit: NCI
A “co-rounding” partnership between medical oncologists and palliative care specialists has shown improvements in health-system and patient-related outcomes.
The first year of the partnership, which was tested in Duke University Hospital’s solid tumor oncology unit, brought significant decreases in the average length of hospital stay and in readmission rates, compared to a previous year in which the partnership did not exist.
There was a decrease in intensive care unit transfers and a trend toward increased hospice referrals as well, although these differences were not significant.
“The integration of palliative care, as a necessary and essential component of cancer care, is one that has been increasingly endorsed," said Richard Riedel, MD, of Duke University Hospital in Durham, North Carolina.
“The benefits of palliative care have been shown in the outpatient and consultative settings, but we didn’t know its impact on daily inpatient care. Now, we have successfully partnered with our palliative care colleagues to bring their unique skill sets and expertise directly to our admitted patients, and have shown it to be beneficial.”
Dr Riedel described this research (abstract 3*) in a presscast prior to the 2014 Palliative Care in Oncology Symposium, which is scheduled to take place October 24-25 at the Westin Boston Waterfront in Boston.
The co-rounding partnership involves 3 formal meetings each day in which members of the team, including both the attending medical oncologist and the attending palliative care physician, discuss all patients in the solid tumor unit.
The team decides which attending physician oversees direct care for a patient depending on his or her needs. For example, patients with higher symptom burden are typically assigned to the palliative care specialists.
The hospital support staff (eg, internal medicine house staff, physician assistants, and pharmacists) round with both attending physicians, and this care model allows for both formal and informal consultation between specialties.
To evaluate the effects of this model, the researchers assessed outcomes among the 731 patients admitted before the intervention began and 783 admitted in the first year of the intervention. About three-quarters of patients in both groups had metastatic cancer.
The team found a significant decrease in the average length of hospital stay from the pre-intervention period to the post-intervention period—4.51 days and 4.16 days, respectively (P=0.02).
Likewise, there was a significant decrease in readmission rates. There was 23% relative reduction in 7-day readmission rates (P<0.0001) and a 12% relative reduction in 30-day readmission rates (P=0.048).
Patient transfers to the intensive care unit decreased by 15% post-intervention, and hospice referrals increased by 17%, but these effects were not statistically significant (P=0.64 and 0.09, respectively).
The researchers said these results emphasize the value of implementing palliative medicine soon after a cancer diagnosis, rather than waiting until later in the disease’s progression.
Due to positive results with the co-rounding partnership, Duke University Hospital has established new outpatient palliative care clinics in oncology and general medicine.
The researchers are planning future studies to assess longer-term effects of the intervention on both patient and health-system outcomes, evaluate patient satisfaction, and explore potential cost savings associated with this intervention. ![]()
*Data presented differ from data in the abstract.
LOY linked to higher risk of cancer, mortality in men

Credit: William Weinert
SAN DIEGO—Age-related loss of the Y chromosome (LOY) from blood cells is associated with an elevated risk of cancer and mortality, a new study indicates.
This finding could help explain why men tend to have a shorter life span and higher rates of non-sex-specific cancers than women, said Lars Forsberg, PhD, of Uppsala University in Sweden.
He and his colleagues presented this research at the American Society of Human Genetics 2014 Annual Meeting and described it
in a letter to Nature Genetics.
LOY, which occurs occasionally as a man’s blood cells replicate, was first reported nearly 50 years ago and remains largely unexplained in both its causes and effects. Recent advances have allowed researchers to use a blood test to detect when only a small fraction of a man’s blood cells have undergone LOY.
Dr Forsberg and his colleagues studied the relationship between LOY, cancer, and mortality using blood samples from 1153 men aged 70 to 84 years who were followed for up to 40 years.
In survival analyses, the investigators studied 982 participants who did not have cancer prior to sampling. The team adjusted their analyses for age, hypertension, exercise, smoking, diabetes, body mass index, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol, and ancestry.
The researchers calculated the degree of LOY for each subject from the median log R ratio values for approximately 2560 probes in the male-specific region of chromosome Y (mLRR-Y).
In a primary analysis, the investigators found that men with a higher degree of LOY had an increased risk of all-cause mortality (hazard ratio [HR]=2.13, P=0.029).
And LOY was a key risk factor for cancer-related mortality (HR=3.76, P=0.022), but it was not significantly associated with non-cancer-related mortality (P=0.245).
The researchers then scored participants on the basis of a defined threshold of mLRR-Y. Men with an mLRR-Y of –0.4 or less were scored as 1, and other subjects were scored as 0.
This analysis confirmed the effect of LOY on the risk of all-cause mortality (HR=1.91, P=0.010). It also showed that median survival times in men with LOY were 5.5 years shorter than for the other subjects, representing half the survival time.
In addition, the analysis confirmed the effect of LOY on the risk of cancer-related mortality (HR=3.29, P=0.003) and death from non-hematologic cancers (HR=3.62, P=0.003).
The investigators could not test the effect of LOY on mortality related to hematologic malignancies, as only one man with an mLRR-Y of –0.4 or less died from a hematologic malignancy.
However, the team did find that the risk of any cancer diagnosis was higher in men with an mLRR-Y of −0.4 or less (HR=2.47, P=0.014). And the same was true for the risk of developing a non-hematologic cancer (HR=2.68, P=0.008).
“Many people think the Y chromosome only contains genes involved in sex determination and sperm production,” said Jan Dumanski, MD, PhD, also of Uppsala University. “In fact, these genes have other important functions, such as possibly playing a role in preventing tumors.”
The researchers noted that LOY in blood cells is associated with many different cancers, and this may be because Y chromosome genes enable blood cells to assist with immunosurveillance.
“Our hypothesis is that LOY disrupts the immunosurveillance normally conducted by blood cells, allowing tumors to grow unchecked and develop into cancer,” Dr Forsberg said.
These findings suggest a new approach to early detection of cancer risk in men: a blood test to assess LOY.
“LOY is not very dangerous in a small fraction of blood cells but becomes increasingly predictive of cancer as more cells lose their Y chromosome,” Dr Forsberg explained. “This takes years, so you’d have a window of time to do something to reduce your risk.”
The investigators are currently exploring LOY in more detail, including the effects of various lifestyle factors and other health conditions on LOY. They are also examining the frequency and consequences of LOY in different types of cells and throughout life. ![]()

Credit: William Weinert
SAN DIEGO—Age-related loss of the Y chromosome (LOY) from blood cells is associated with an elevated risk of cancer and mortality, a new study indicates.
This finding could help explain why men tend to have a shorter life span and higher rates of non-sex-specific cancers than women, said Lars Forsberg, PhD, of Uppsala University in Sweden.
He and his colleagues presented this research at the American Society of Human Genetics 2014 Annual Meeting and described it
in a letter to Nature Genetics.
LOY, which occurs occasionally as a man’s blood cells replicate, was first reported nearly 50 years ago and remains largely unexplained in both its causes and effects. Recent advances have allowed researchers to use a blood test to detect when only a small fraction of a man’s blood cells have undergone LOY.
Dr Forsberg and his colleagues studied the relationship between LOY, cancer, and mortality using blood samples from 1153 men aged 70 to 84 years who were followed for up to 40 years.
In survival analyses, the investigators studied 982 participants who did not have cancer prior to sampling. The team adjusted their analyses for age, hypertension, exercise, smoking, diabetes, body mass index, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol, and ancestry.
The researchers calculated the degree of LOY for each subject from the median log R ratio values for approximately 2560 probes in the male-specific region of chromosome Y (mLRR-Y).
In a primary analysis, the investigators found that men with a higher degree of LOY had an increased risk of all-cause mortality (hazard ratio [HR]=2.13, P=0.029).
And LOY was a key risk factor for cancer-related mortality (HR=3.76, P=0.022), but it was not significantly associated with non-cancer-related mortality (P=0.245).
The researchers then scored participants on the basis of a defined threshold of mLRR-Y. Men with an mLRR-Y of –0.4 or less were scored as 1, and other subjects were scored as 0.
This analysis confirmed the effect of LOY on the risk of all-cause mortality (HR=1.91, P=0.010). It also showed that median survival times in men with LOY were 5.5 years shorter than for the other subjects, representing half the survival time.
In addition, the analysis confirmed the effect of LOY on the risk of cancer-related mortality (HR=3.29, P=0.003) and death from non-hematologic cancers (HR=3.62, P=0.003).
The investigators could not test the effect of LOY on mortality related to hematologic malignancies, as only one man with an mLRR-Y of –0.4 or less died from a hematologic malignancy.
However, the team did find that the risk of any cancer diagnosis was higher in men with an mLRR-Y of −0.4 or less (HR=2.47, P=0.014). And the same was true for the risk of developing a non-hematologic cancer (HR=2.68, P=0.008).
“Many people think the Y chromosome only contains genes involved in sex determination and sperm production,” said Jan Dumanski, MD, PhD, also of Uppsala University. “In fact, these genes have other important functions, such as possibly playing a role in preventing tumors.”
The researchers noted that LOY in blood cells is associated with many different cancers, and this may be because Y chromosome genes enable blood cells to assist with immunosurveillance.
“Our hypothesis is that LOY disrupts the immunosurveillance normally conducted by blood cells, allowing tumors to grow unchecked and develop into cancer,” Dr Forsberg said.
These findings suggest a new approach to early detection of cancer risk in men: a blood test to assess LOY.
“LOY is not very dangerous in a small fraction of blood cells but becomes increasingly predictive of cancer as more cells lose their Y chromosome,” Dr Forsberg explained. “This takes years, so you’d have a window of time to do something to reduce your risk.”
The investigators are currently exploring LOY in more detail, including the effects of various lifestyle factors and other health conditions on LOY. They are also examining the frequency and consequences of LOY in different types of cells and throughout life. ![]()

Credit: William Weinert
SAN DIEGO—Age-related loss of the Y chromosome (LOY) from blood cells is associated with an elevated risk of cancer and mortality, a new study indicates.
This finding could help explain why men tend to have a shorter life span and higher rates of non-sex-specific cancers than women, said Lars Forsberg, PhD, of Uppsala University in Sweden.
He and his colleagues presented this research at the American Society of Human Genetics 2014 Annual Meeting and described it
in a letter to Nature Genetics.
LOY, which occurs occasionally as a man’s blood cells replicate, was first reported nearly 50 years ago and remains largely unexplained in both its causes and effects. Recent advances have allowed researchers to use a blood test to detect when only a small fraction of a man’s blood cells have undergone LOY.
Dr Forsberg and his colleagues studied the relationship between LOY, cancer, and mortality using blood samples from 1153 men aged 70 to 84 years who were followed for up to 40 years.
In survival analyses, the investigators studied 982 participants who did not have cancer prior to sampling. The team adjusted their analyses for age, hypertension, exercise, smoking, diabetes, body mass index, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol, and ancestry.
The researchers calculated the degree of LOY for each subject from the median log R ratio values for approximately 2560 probes in the male-specific region of chromosome Y (mLRR-Y).
In a primary analysis, the investigators found that men with a higher degree of LOY had an increased risk of all-cause mortality (hazard ratio [HR]=2.13, P=0.029).
And LOY was a key risk factor for cancer-related mortality (HR=3.76, P=0.022), but it was not significantly associated with non-cancer-related mortality (P=0.245).
The researchers then scored participants on the basis of a defined threshold of mLRR-Y. Men with an mLRR-Y of –0.4 or less were scored as 1, and other subjects were scored as 0.
This analysis confirmed the effect of LOY on the risk of all-cause mortality (HR=1.91, P=0.010). It also showed that median survival times in men with LOY were 5.5 years shorter than for the other subjects, representing half the survival time.
In addition, the analysis confirmed the effect of LOY on the risk of cancer-related mortality (HR=3.29, P=0.003) and death from non-hematologic cancers (HR=3.62, P=0.003).
The investigators could not test the effect of LOY on mortality related to hematologic malignancies, as only one man with an mLRR-Y of –0.4 or less died from a hematologic malignancy.
However, the team did find that the risk of any cancer diagnosis was higher in men with an mLRR-Y of −0.4 or less (HR=2.47, P=0.014). And the same was true for the risk of developing a non-hematologic cancer (HR=2.68, P=0.008).
“Many people think the Y chromosome only contains genes involved in sex determination and sperm production,” said Jan Dumanski, MD, PhD, also of Uppsala University. “In fact, these genes have other important functions, such as possibly playing a role in preventing tumors.”
The researchers noted that LOY in blood cells is associated with many different cancers, and this may be because Y chromosome genes enable blood cells to assist with immunosurveillance.
“Our hypothesis is that LOY disrupts the immunosurveillance normally conducted by blood cells, allowing tumors to grow unchecked and develop into cancer,” Dr Forsberg said.
These findings suggest a new approach to early detection of cancer risk in men: a blood test to assess LOY.
“LOY is not very dangerous in a small fraction of blood cells but becomes increasingly predictive of cancer as more cells lose their Y chromosome,” Dr Forsberg explained. “This takes years, so you’d have a window of time to do something to reduce your risk.”
The investigators are currently exploring LOY in more detail, including the effects of various lifestyle factors and other health conditions on LOY. They are also examining the frequency and consequences of LOY in different types of cells and throughout life. ![]()
Hospital acquisitions lead to increased patient costs
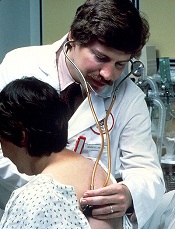
Credit: NCI
The trend of hospitals consolidating medical groups and physician practices is increasing the cost of patient care, new research suggests.
The study was conducted using 4 years of data from nearly 160 medical groups in California.
Results showed that hospital-owned physician organizations incurred higher expenditures than physician-owned organizations for services to patients covered by commercial health maintenance organization (HMO) insurance.
The findings, published in JAMA, come as a growing number of local hospitals and large, multihospital systems in the US are acquiring physician groups and medical practices.
“This consolidation is meant to better coordinate care and to have a stronger bargaining position with insurance plans,” said James Robinson, PhD, of the University of California, Berkeley School of Public Health.
“The movement also aligns with the goals of the Affordable Care Act, since physicians and hospitals working together in ‘accountable care organizations’ can provide care better than the traditional fee-for-service and solo-practice models. The intent of consolidation is to reduce costs and improve quality, but the problem with all this is that hospitals are very expensive and complex organizations, and they are not known for their efficiency and low prices.”
Dr Robinson teamed up with Kelly Miller, of Integrated Healthcare Association in Oakland, California, to analyze data on 158 major medical groups. The data spanned the period from 2009 to 2012.
Of the 158 organizations, 118 (75%) were physician-owned and provided care for 3,065,551 patients, 19 (12%) were owned by local hospitals and provided care for 728,608 patients, and 21 (13%) were owned by multihospital systems and provided care for 693,254 patients.
The patients were covered by commercial HMO insurance. The data did not include patients covered by commercial preferred provider organization (PPO) insurance, Medicare, or Medicaid.
The researchers assessed costs related to physician visits, inpatient hospital admissions, outpatient surgery and diagnostic procedures, drugs, and all other forms of medical care except mental health services.
Results revealed that the average expenditure per patient across all physician organizations increased by 16.5% between 2009 and 2012, from $2954 to $3443.
By 2012, expenditures per patient had increased to an average of $3066 in physician-owned organizations, $4312 in local hospital-owned organizations, and $4776 in multihospital system-owned organizations.
This represents a 40.6% relative difference in expenditures per patient associated with hospital ownership and a 55.8% relative difference associated with ownership by a multihospital system compared with ownership by member physicians.
After adjusting for patient severity and other factors over the period, local hospital-owned physician organizations incurred expenditures per patient 10.3% higher than physician-owned organizations. And organizations owned by multihospital systems incurred expenditures 19.8% higher than physician-owned organizations.
Dr Robinson said these findings might be explained by the fact that, once a medical group has been acquired by a multihospital system, physicians in those groups are expected to admit their patients to the high-priced hospital.
“Hospital-owned medical groups usually are expected to conduct ambulatory surgery and diagnostic procedures in the outpatient departments of their parent hospital, but hospital outpatient departments are much more costly and charge much higher prices than freestanding, non-hospital ambulatory centers,” he said.
Dr Robinson added that public policy should not encourage mergers and acquisitions as a means of promoting collaboration. Instead, policymakers should consider supporting the use of bundled payments for hospitals and physicians to improve the coordination of care.
“Hospitals are an essential part of the healthcare system, but they should not be the center of the delivery system,” he said. “Rather, physician-led organizations based in ambulatory and community settings are likely to be more efficient and provide cheaper care.”
The researchers noted that their findings are limited to California, and further studies should be conducted using data from other states.
“Nevertheless, these findings are important,” Dr Robinson said, “since California is the nation’s leader in terms of having physicians participate in large medical groups that already perform the functions ascribed to ‘accountable care organizations’ by the Obama administration.” ![]()

Credit: NCI
The trend of hospitals consolidating medical groups and physician practices is increasing the cost of patient care, new research suggests.
The study was conducted using 4 years of data from nearly 160 medical groups in California.
Results showed that hospital-owned physician organizations incurred higher expenditures than physician-owned organizations for services to patients covered by commercial health maintenance organization (HMO) insurance.
The findings, published in JAMA, come as a growing number of local hospitals and large, multihospital systems in the US are acquiring physician groups and medical practices.
“This consolidation is meant to better coordinate care and to have a stronger bargaining position with insurance plans,” said James Robinson, PhD, of the University of California, Berkeley School of Public Health.
“The movement also aligns with the goals of the Affordable Care Act, since physicians and hospitals working together in ‘accountable care organizations’ can provide care better than the traditional fee-for-service and solo-practice models. The intent of consolidation is to reduce costs and improve quality, but the problem with all this is that hospitals are very expensive and complex organizations, and they are not known for their efficiency and low prices.”
Dr Robinson teamed up with Kelly Miller, of Integrated Healthcare Association in Oakland, California, to analyze data on 158 major medical groups. The data spanned the period from 2009 to 2012.
Of the 158 organizations, 118 (75%) were physician-owned and provided care for 3,065,551 patients, 19 (12%) were owned by local hospitals and provided care for 728,608 patients, and 21 (13%) were owned by multihospital systems and provided care for 693,254 patients.
The patients were covered by commercial HMO insurance. The data did not include patients covered by commercial preferred provider organization (PPO) insurance, Medicare, or Medicaid.
The researchers assessed costs related to physician visits, inpatient hospital admissions, outpatient surgery and diagnostic procedures, drugs, and all other forms of medical care except mental health services.
Results revealed that the average expenditure per patient across all physician organizations increased by 16.5% between 2009 and 2012, from $2954 to $3443.
By 2012, expenditures per patient had increased to an average of $3066 in physician-owned organizations, $4312 in local hospital-owned organizations, and $4776 in multihospital system-owned organizations.
This represents a 40.6% relative difference in expenditures per patient associated with hospital ownership and a 55.8% relative difference associated with ownership by a multihospital system compared with ownership by member physicians.
After adjusting for patient severity and other factors over the period, local hospital-owned physician organizations incurred expenditures per patient 10.3% higher than physician-owned organizations. And organizations owned by multihospital systems incurred expenditures 19.8% higher than physician-owned organizations.
Dr Robinson said these findings might be explained by the fact that, once a medical group has been acquired by a multihospital system, physicians in those groups are expected to admit their patients to the high-priced hospital.
“Hospital-owned medical groups usually are expected to conduct ambulatory surgery and diagnostic procedures in the outpatient departments of their parent hospital, but hospital outpatient departments are much more costly and charge much higher prices than freestanding, non-hospital ambulatory centers,” he said.
Dr Robinson added that public policy should not encourage mergers and acquisitions as a means of promoting collaboration. Instead, policymakers should consider supporting the use of bundled payments for hospitals and physicians to improve the coordination of care.
“Hospitals are an essential part of the healthcare system, but they should not be the center of the delivery system,” he said. “Rather, physician-led organizations based in ambulatory and community settings are likely to be more efficient and provide cheaper care.”
The researchers noted that their findings are limited to California, and further studies should be conducted using data from other states.
“Nevertheless, these findings are important,” Dr Robinson said, “since California is the nation’s leader in terms of having physicians participate in large medical groups that already perform the functions ascribed to ‘accountable care organizations’ by the Obama administration.” ![]()

Credit: NCI
The trend of hospitals consolidating medical groups and physician practices is increasing the cost of patient care, new research suggests.
The study was conducted using 4 years of data from nearly 160 medical groups in California.
Results showed that hospital-owned physician organizations incurred higher expenditures than physician-owned organizations for services to patients covered by commercial health maintenance organization (HMO) insurance.
The findings, published in JAMA, come as a growing number of local hospitals and large, multihospital systems in the US are acquiring physician groups and medical practices.
“This consolidation is meant to better coordinate care and to have a stronger bargaining position with insurance plans,” said James Robinson, PhD, of the University of California, Berkeley School of Public Health.
“The movement also aligns with the goals of the Affordable Care Act, since physicians and hospitals working together in ‘accountable care organizations’ can provide care better than the traditional fee-for-service and solo-practice models. The intent of consolidation is to reduce costs and improve quality, but the problem with all this is that hospitals are very expensive and complex organizations, and they are not known for their efficiency and low prices.”
Dr Robinson teamed up with Kelly Miller, of Integrated Healthcare Association in Oakland, California, to analyze data on 158 major medical groups. The data spanned the period from 2009 to 2012.
Of the 158 organizations, 118 (75%) were physician-owned and provided care for 3,065,551 patients, 19 (12%) were owned by local hospitals and provided care for 728,608 patients, and 21 (13%) were owned by multihospital systems and provided care for 693,254 patients.
The patients were covered by commercial HMO insurance. The data did not include patients covered by commercial preferred provider organization (PPO) insurance, Medicare, or Medicaid.
The researchers assessed costs related to physician visits, inpatient hospital admissions, outpatient surgery and diagnostic procedures, drugs, and all other forms of medical care except mental health services.
Results revealed that the average expenditure per patient across all physician organizations increased by 16.5% between 2009 and 2012, from $2954 to $3443.
By 2012, expenditures per patient had increased to an average of $3066 in physician-owned organizations, $4312 in local hospital-owned organizations, and $4776 in multihospital system-owned organizations.
This represents a 40.6% relative difference in expenditures per patient associated with hospital ownership and a 55.8% relative difference associated with ownership by a multihospital system compared with ownership by member physicians.
After adjusting for patient severity and other factors over the period, local hospital-owned physician organizations incurred expenditures per patient 10.3% higher than physician-owned organizations. And organizations owned by multihospital systems incurred expenditures 19.8% higher than physician-owned organizations.
Dr Robinson said these findings might be explained by the fact that, once a medical group has been acquired by a multihospital system, physicians in those groups are expected to admit their patients to the high-priced hospital.
“Hospital-owned medical groups usually are expected to conduct ambulatory surgery and diagnostic procedures in the outpatient departments of their parent hospital, but hospital outpatient departments are much more costly and charge much higher prices than freestanding, non-hospital ambulatory centers,” he said.
Dr Robinson added that public policy should not encourage mergers and acquisitions as a means of promoting collaboration. Instead, policymakers should consider supporting the use of bundled payments for hospitals and physicians to improve the coordination of care.
“Hospitals are an essential part of the healthcare system, but they should not be the center of the delivery system,” he said. “Rather, physician-led organizations based in ambulatory and community settings are likely to be more efficient and provide cheaper care.”
The researchers noted that their findings are limited to California, and further studies should be conducted using data from other states.
“Nevertheless, these findings are important,” Dr Robinson said, “since California is the nation’s leader in terms of having physicians participate in large medical groups that already perform the functions ascribed to ‘accountable care organizations’ by the Obama administration.” ![]()
Less competition equals higher healthcare costs

Credit: Petr Kratochvil
Medical practices in less competitive markets charge more for their services, according to a study published in JAMA.
The study, based on US healthcare data from 2010, provides new information about the effects of competition on prices for office visits paid by preferred provider organizations (PPOs).
“The research comes out of trying to understand some dramatic changes that have occurred in the healthcare system over a couple of decades,” said Laurence Baker, PhD, of the Stanford University School of Medicine in California.
One such change is the shift from practices with one or two doctors toward larger, more complex organizations with many physicians. An impact of this can be reduced competition among physician practices.
Dr Baker and his colleagues sought to understand how variation in the amount of competition within a region affects the amounts doctors are paid.
The researchers assessed the relationship between competition and prices paid by PPOs for the most commonly billed services within 10 prominent physician specialties—internal medicine, family practice, cardiology, dermatology, gastroenterology, neurology, general surgery, orthopedics, urology, and otolaryngology.
To establish what prices various medical practices were paid for services, the team used Truven Analytics MarketScan Commercial Claims and Encounters database, which contains the prices paid to physicians for more than 49 million privately insured people from all over the US. They obtained the number of claims and the mean price paid for each service in 1058 counties representing all 50 states.
To measure competitiveness, the researchers drew inspiration from the business world. Using Medicare data, they adapted a standard economic competition measure to track physician practice competition for different US regions.
The Hirschman-Herfindahl Index (HHI) uses the relative sizes of practices to measure market concentration. A higher HHI indicates a less competitive market, and a lower HHI indicates higher competition.
Less competition, higher prices
The researchers found that less competition among physician practices was associated with higher prices paid by private PPOs for office visits.
Across 10 types of office visits, the difference in the HHI was associated with average prices for office visits 8.3% to 16.1% higher. In a more conservative model, the difference in the HHI was associated with 3.5% to 5.4% higher average prices.
The researchers pointed out that, in 2011, privately insured individuals in the US spent nearly $250 billion on physician services. In that context, these small percentage increases could translate to tens of billions of dollars in extra spending.
The team also found that, between 2003 and 2010, prices increased more rapidly in areas that were less competitive. Even when there is no change in HHI, practices in less competitive areas could continue to drive up prices.
“These larger organizations might have better processes in place to optimize care,” said Kate Bundorf, PhD, also of the Stanford University School of Medicine.
“But our research also points out [that we] have to think about the effect on prices and try to balance those two things when we think about how to form policy about these organizations.”
Dr Baker echoed that sentiment.
“Sometimes, it can be tempting to say our goals for the healthcare system should be only about taking care of patients and doing it as well as possible,” he said. “We don’t want to worry about the economics. But the truth is, we do have to worry about the prices because the bill does come, even if you wish it wouldn’t.” ![]()

Credit: Petr Kratochvil
Medical practices in less competitive markets charge more for their services, according to a study published in JAMA.
The study, based on US healthcare data from 2010, provides new information about the effects of competition on prices for office visits paid by preferred provider organizations (PPOs).
“The research comes out of trying to understand some dramatic changes that have occurred in the healthcare system over a couple of decades,” said Laurence Baker, PhD, of the Stanford University School of Medicine in California.
One such change is the shift from practices with one or two doctors toward larger, more complex organizations with many physicians. An impact of this can be reduced competition among physician practices.
Dr Baker and his colleagues sought to understand how variation in the amount of competition within a region affects the amounts doctors are paid.
The researchers assessed the relationship between competition and prices paid by PPOs for the most commonly billed services within 10 prominent physician specialties—internal medicine, family practice, cardiology, dermatology, gastroenterology, neurology, general surgery, orthopedics, urology, and otolaryngology.
To establish what prices various medical practices were paid for services, the team used Truven Analytics MarketScan Commercial Claims and Encounters database, which contains the prices paid to physicians for more than 49 million privately insured people from all over the US. They obtained the number of claims and the mean price paid for each service in 1058 counties representing all 50 states.
To measure competitiveness, the researchers drew inspiration from the business world. Using Medicare data, they adapted a standard economic competition measure to track physician practice competition for different US regions.
The Hirschman-Herfindahl Index (HHI) uses the relative sizes of practices to measure market concentration. A higher HHI indicates a less competitive market, and a lower HHI indicates higher competition.
Less competition, higher prices
The researchers found that less competition among physician practices was associated with higher prices paid by private PPOs for office visits.
Across 10 types of office visits, the difference in the HHI was associated with average prices for office visits 8.3% to 16.1% higher. In a more conservative model, the difference in the HHI was associated with 3.5% to 5.4% higher average prices.
The researchers pointed out that, in 2011, privately insured individuals in the US spent nearly $250 billion on physician services. In that context, these small percentage increases could translate to tens of billions of dollars in extra spending.
The team also found that, between 2003 and 2010, prices increased more rapidly in areas that were less competitive. Even when there is no change in HHI, practices in less competitive areas could continue to drive up prices.
“These larger organizations might have better processes in place to optimize care,” said Kate Bundorf, PhD, also of the Stanford University School of Medicine.
“But our research also points out [that we] have to think about the effect on prices and try to balance those two things when we think about how to form policy about these organizations.”
Dr Baker echoed that sentiment.
“Sometimes, it can be tempting to say our goals for the healthcare system should be only about taking care of patients and doing it as well as possible,” he said. “We don’t want to worry about the economics. But the truth is, we do have to worry about the prices because the bill does come, even if you wish it wouldn’t.” ![]()

Credit: Petr Kratochvil
Medical practices in less competitive markets charge more for their services, according to a study published in JAMA.
The study, based on US healthcare data from 2010, provides new information about the effects of competition on prices for office visits paid by preferred provider organizations (PPOs).
“The research comes out of trying to understand some dramatic changes that have occurred in the healthcare system over a couple of decades,” said Laurence Baker, PhD, of the Stanford University School of Medicine in California.
One such change is the shift from practices with one or two doctors toward larger, more complex organizations with many physicians. An impact of this can be reduced competition among physician practices.
Dr Baker and his colleagues sought to understand how variation in the amount of competition within a region affects the amounts doctors are paid.
The researchers assessed the relationship between competition and prices paid by PPOs for the most commonly billed services within 10 prominent physician specialties—internal medicine, family practice, cardiology, dermatology, gastroenterology, neurology, general surgery, orthopedics, urology, and otolaryngology.
To establish what prices various medical practices were paid for services, the team used Truven Analytics MarketScan Commercial Claims and Encounters database, which contains the prices paid to physicians for more than 49 million privately insured people from all over the US. They obtained the number of claims and the mean price paid for each service in 1058 counties representing all 50 states.
To measure competitiveness, the researchers drew inspiration from the business world. Using Medicare data, they adapted a standard economic competition measure to track physician practice competition for different US regions.
The Hirschman-Herfindahl Index (HHI) uses the relative sizes of practices to measure market concentration. A higher HHI indicates a less competitive market, and a lower HHI indicates higher competition.
Less competition, higher prices
The researchers found that less competition among physician practices was associated with higher prices paid by private PPOs for office visits.
Across 10 types of office visits, the difference in the HHI was associated with average prices for office visits 8.3% to 16.1% higher. In a more conservative model, the difference in the HHI was associated with 3.5% to 5.4% higher average prices.
The researchers pointed out that, in 2011, privately insured individuals in the US spent nearly $250 billion on physician services. In that context, these small percentage increases could translate to tens of billions of dollars in extra spending.
The team also found that, between 2003 and 2010, prices increased more rapidly in areas that were less competitive. Even when there is no change in HHI, practices in less competitive areas could continue to drive up prices.
“These larger organizations might have better processes in place to optimize care,” said Kate Bundorf, PhD, also of the Stanford University School of Medicine.
“But our research also points out [that we] have to think about the effect on prices and try to balance those two things when we think about how to form policy about these organizations.”
Dr Baker echoed that sentiment.
“Sometimes, it can be tempting to say our goals for the healthcare system should be only about taking care of patients and doing it as well as possible,” he said. “We don’t want to worry about the economics. But the truth is, we do have to worry about the prices because the bill does come, even if you wish it wouldn’t.” ![]()
Docs often don’t know about patients’ CVCs
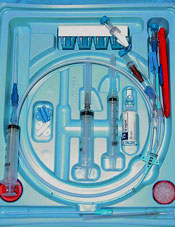
A multicenter study showed that roughly 1 in 5 physicians did not know when a hospitalized patient had a central venous catheter (CVC) in place.
Hospitalists were the least likely to know of a CVC’s presence, followed by general medicine teaching attendings, interns, and residents.
These findings raise questions about patient safety, as CVCs pose a risk of bloodstream infection and thrombosis, both of which can be prevented by removing catheters that are no longer necessary.
“We know that central venous catheters are invaluable for the safe and comprehensive care of some hospitalized patients, but just as they are helpful, they can be harmful,” said study author Vineet Chopra, MD, of the University of Michigan Health System in Ann Arbor.
“The key to preventing complications is to remove devices when they are no longer necessary, but that requires knowing they are there in the first place. Our findings suggest that patient safety may be jeopardized if medical providers don’t improve their practices regarding device awareness.”
Dr Chopra and his colleagues reported their findings in the Annals of Internal Medicine.
The study included 990 patients and 1881 clinical assessments at 3 academic medical centers in the US. Responses from interns (n=454), residents and physician extenders (n=513), general medicine teaching attendings (n=245), subspecialty attendings (n=176), intensivists (n=95), and hospitalists (n=398) were included.
The overall prevalence of CVCs was 21.1%, 60.3% of which were peripherally inserted central catheters (PICCs). The remaining CVCs were triple-lumen catheters inserted in the neck (19.6%), chest (11.5%), or groin (8.6%).
In all, 21.2% of clinicians interviewed did not know when a patient had a CVC in place. And 5.6% of clinicians said a patient had a CVC when there was no device in place.
Hospitalists were most likely to be unaware of a CVC (30.5%), followed by general medicine teaching attendings (25.8%), interns (19.1%), and residents (13.8%).
When assessed by service, critical care physicians were the least likely to be unaware of a CVC (12.6%), compared to general medicine teaching attendings/hospitalists (26.2%) and clinicians in other subspecialties (22.5%). Awareness was best among specialties that used CVCs often, such as cardiology and oncology.
Lack of awareness was greatest for PICCs; 25.1% of clinicians were unaware of a PICC’s presence, and 15.6% were unaware of a triple lumen catheter’s presence.
“These findings have important patient safety and policy implications for health systems nationwide,” Dr Chopra said, “because they suggest that removal of clinically unnecessary catheters may be limited by lack of awareness by providers, especially in non-intensive care settings.” ![]()

A multicenter study showed that roughly 1 in 5 physicians did not know when a hospitalized patient had a central venous catheter (CVC) in place.
Hospitalists were the least likely to know of a CVC’s presence, followed by general medicine teaching attendings, interns, and residents.
These findings raise questions about patient safety, as CVCs pose a risk of bloodstream infection and thrombosis, both of which can be prevented by removing catheters that are no longer necessary.
“We know that central venous catheters are invaluable for the safe and comprehensive care of some hospitalized patients, but just as they are helpful, they can be harmful,” said study author Vineet Chopra, MD, of the University of Michigan Health System in Ann Arbor.
“The key to preventing complications is to remove devices when they are no longer necessary, but that requires knowing they are there in the first place. Our findings suggest that patient safety may be jeopardized if medical providers don’t improve their practices regarding device awareness.”
Dr Chopra and his colleagues reported their findings in the Annals of Internal Medicine.
The study included 990 patients and 1881 clinical assessments at 3 academic medical centers in the US. Responses from interns (n=454), residents and physician extenders (n=513), general medicine teaching attendings (n=245), subspecialty attendings (n=176), intensivists (n=95), and hospitalists (n=398) were included.
The overall prevalence of CVCs was 21.1%, 60.3% of which were peripherally inserted central catheters (PICCs). The remaining CVCs were triple-lumen catheters inserted in the neck (19.6%), chest (11.5%), or groin (8.6%).
In all, 21.2% of clinicians interviewed did not know when a patient had a CVC in place. And 5.6% of clinicians said a patient had a CVC when there was no device in place.
Hospitalists were most likely to be unaware of a CVC (30.5%), followed by general medicine teaching attendings (25.8%), interns (19.1%), and residents (13.8%).
When assessed by service, critical care physicians were the least likely to be unaware of a CVC (12.6%), compared to general medicine teaching attendings/hospitalists (26.2%) and clinicians in other subspecialties (22.5%). Awareness was best among specialties that used CVCs often, such as cardiology and oncology.
Lack of awareness was greatest for PICCs; 25.1% of clinicians were unaware of a PICC’s presence, and 15.6% were unaware of a triple lumen catheter’s presence.
“These findings have important patient safety and policy implications for health systems nationwide,” Dr Chopra said, “because they suggest that removal of clinically unnecessary catheters may be limited by lack of awareness by providers, especially in non-intensive care settings.” ![]()

A multicenter study showed that roughly 1 in 5 physicians did not know when a hospitalized patient had a central venous catheter (CVC) in place.
Hospitalists were the least likely to know of a CVC’s presence, followed by general medicine teaching attendings, interns, and residents.
These findings raise questions about patient safety, as CVCs pose a risk of bloodstream infection and thrombosis, both of which can be prevented by removing catheters that are no longer necessary.
“We know that central venous catheters are invaluable for the safe and comprehensive care of some hospitalized patients, but just as they are helpful, they can be harmful,” said study author Vineet Chopra, MD, of the University of Michigan Health System in Ann Arbor.
“The key to preventing complications is to remove devices when they are no longer necessary, but that requires knowing they are there in the first place. Our findings suggest that patient safety may be jeopardized if medical providers don’t improve their practices regarding device awareness.”
Dr Chopra and his colleagues reported their findings in the Annals of Internal Medicine.
The study included 990 patients and 1881 clinical assessments at 3 academic medical centers in the US. Responses from interns (n=454), residents and physician extenders (n=513), general medicine teaching attendings (n=245), subspecialty attendings (n=176), intensivists (n=95), and hospitalists (n=398) were included.
The overall prevalence of CVCs was 21.1%, 60.3% of which were peripherally inserted central catheters (PICCs). The remaining CVCs were triple-lumen catheters inserted in the neck (19.6%), chest (11.5%), or groin (8.6%).
In all, 21.2% of clinicians interviewed did not know when a patient had a CVC in place. And 5.6% of clinicians said a patient had a CVC when there was no device in place.
Hospitalists were most likely to be unaware of a CVC (30.5%), followed by general medicine teaching attendings (25.8%), interns (19.1%), and residents (13.8%).
When assessed by service, critical care physicians were the least likely to be unaware of a CVC (12.6%), compared to general medicine teaching attendings/hospitalists (26.2%) and clinicians in other subspecialties (22.5%). Awareness was best among specialties that used CVCs often, such as cardiology and oncology.
Lack of awareness was greatest for PICCs; 25.1% of clinicians were unaware of a PICC’s presence, and 15.6% were unaware of a triple lumen catheter’s presence.
“These findings have important patient safety and policy implications for health systems nationwide,” Dr Chopra said, “because they suggest that removal of clinically unnecessary catheters may be limited by lack of awareness by providers, especially in non-intensive care settings.”
Hemorrhage control system gets expanded approval

Control System
The US Food and Drug Administration has expanded the indication for the iTClamp® Hemorrhage Control System.
It is now approved to provide temporary control of severe bleeding of the neck. The product was already approved for use on the extremities, axilla, inguinal areas, and the scalp.
The iTClamp is a temporary wound closure device designed to control severe bleeding in seconds.
It seals the edges of a wound closed to create a temporary pool of blood under pressure. This forms a stable clot that mitigates further blood
loss until the wound can be surgically repaired.
Each iTClamp measures less than 2 by 2 inches and weighs less than 3 ounces. It requires only minimal training and gross motor skills to use, according to iTraumaCare, the company that makes the product.
“Addressing difficult-to-control hemorrhage in the neck has been a consistent problem with few solutions,” said Dennis Filips, MD, founder and chief medical officer of iTraumaCare.
“This expanded indication for the iTClamp will allow first responders, medical professionals, and tactical and battlefield medics to use the device in even more meaningful ways to improve patient care.”

Control System
The US Food and Drug Administration has expanded the indication for the iTClamp® Hemorrhage Control System.
It is now approved to provide temporary control of severe bleeding of the neck. The product was already approved for use on the extremities, axilla, inguinal areas, and the scalp.
The iTClamp is a temporary wound closure device designed to control severe bleeding in seconds.
It seals the edges of a wound closed to create a temporary pool of blood under pressure. This forms a stable clot that mitigates further blood
loss until the wound can be surgically repaired.
Each iTClamp measures less than 2 by 2 inches and weighs less than 3 ounces. It requires only minimal training and gross motor skills to use, according to iTraumaCare, the company that makes the product.
“Addressing difficult-to-control hemorrhage in the neck has been a consistent problem with few solutions,” said Dennis Filips, MD, founder and chief medical officer of iTraumaCare.
“This expanded indication for the iTClamp will allow first responders, medical professionals, and tactical and battlefield medics to use the device in even more meaningful ways to improve patient care.”

Control System
The US Food and Drug Administration has expanded the indication for the iTClamp® Hemorrhage Control System.
It is now approved to provide temporary control of severe bleeding of the neck. The product was already approved for use on the extremities, axilla, inguinal areas, and the scalp.
The iTClamp is a temporary wound closure device designed to control severe bleeding in seconds.
It seals the edges of a wound closed to create a temporary pool of blood under pressure. This forms a stable clot that mitigates further blood
loss until the wound can be surgically repaired.
Each iTClamp measures less than 2 by 2 inches and weighs less than 3 ounces. It requires only minimal training and gross motor skills to use, according to iTraumaCare, the company that makes the product.
“Addressing difficult-to-control hemorrhage in the neck has been a consistent problem with few solutions,” said Dennis Filips, MD, founder and chief medical officer of iTraumaCare.
“This expanded indication for the iTClamp will allow first responders, medical professionals, and tactical and battlefield medics to use the device in even more meaningful ways to improve patient care.”
Megakaryocytes can control HSCs, team finds

to a megakaryocyte (red)
Credit: Meng Zhao
For the first time, researchers have shown that hematopoietic stem cells (HSCs) can be directly controlled by their own progeny, megakaryocytes.
Preclinical experiments revealed that megakaryocytes maintain HSC quiescence during homeostasis and promote HSC regeneration after chemotherapeutic stress.
The discovery suggests megakaryocytes might be used to treat patients with low blood cell counts and to expand HSCs for transplant.
The researchers described these findings in Nature Medicine.
The team examined the relationship between megakaryocytes and HSCs in mouse bone marrow. And they discovered that, as a terminally differentiated progeny, megakaryocytes regulate HSCs by performing two previously unknown functions.
“Megakaryocytes can directly regulate the amount of hematopoietic stem cells by telling the cells when they need to keep in the quiescent stage and when they need to start proliferating to meet increased demand,” said study author Meng Zhao, PhD, of the Stowers Institute for Medical Research in Kansas City, Missouri.
The researchers found that the protein transforming growth factor B1 (TGF-B1), contained in megakaryocytes, signaled quiescence.
And, when under stress from chemotherapy, megakaryocytes signaled fibroblast growth factor 1 (FGF1), to stimulate HSC proliferation.
“Our findings suggest that megakaryocytes are required for the recovery of hematopoietic stem cells post-chemotherapy,” said Linheng Li, PhD, also of the Stowers Institute.
The discovery could provide insight for using megakaryocyte-derived factors, such as TGF-B1 and FGF1, clinically to facilitate the regeneration of HSCs, he added.
Engineering a megakaryocyte niche that supports the growth of HSCs in culture is the next step for the researchers. They are also investigating whether a megakaryocyte niche can be used to help expand human HSCs in vitro for transplant.
These findings are supported by similar research also reported in Nature Medicine.

to a megakaryocyte (red)
Credit: Meng Zhao
For the first time, researchers have shown that hematopoietic stem cells (HSCs) can be directly controlled by their own progeny, megakaryocytes.
Preclinical experiments revealed that megakaryocytes maintain HSC quiescence during homeostasis and promote HSC regeneration after chemotherapeutic stress.
The discovery suggests megakaryocytes might be used to treat patients with low blood cell counts and to expand HSCs for transplant.
The researchers described these findings in Nature Medicine.
The team examined the relationship between megakaryocytes and HSCs in mouse bone marrow. And they discovered that, as a terminally differentiated progeny, megakaryocytes regulate HSCs by performing two previously unknown functions.
“Megakaryocytes can directly regulate the amount of hematopoietic stem cells by telling the cells when they need to keep in the quiescent stage and when they need to start proliferating to meet increased demand,” said study author Meng Zhao, PhD, of the Stowers Institute for Medical Research in Kansas City, Missouri.
The researchers found that the protein transforming growth factor B1 (TGF-B1), contained in megakaryocytes, signaled quiescence.
And, when under stress from chemotherapy, megakaryocytes signaled fibroblast growth factor 1 (FGF1), to stimulate HSC proliferation.
“Our findings suggest that megakaryocytes are required for the recovery of hematopoietic stem cells post-chemotherapy,” said Linheng Li, PhD, also of the Stowers Institute.
The discovery could provide insight for using megakaryocyte-derived factors, such as TGF-B1 and FGF1, clinically to facilitate the regeneration of HSCs, he added.
Engineering a megakaryocyte niche that supports the growth of HSCs in culture is the next step for the researchers. They are also investigating whether a megakaryocyte niche can be used to help expand human HSCs in vitro for transplant.
These findings are supported by similar research also reported in Nature Medicine.

to a megakaryocyte (red)
Credit: Meng Zhao
For the first time, researchers have shown that hematopoietic stem cells (HSCs) can be directly controlled by their own progeny, megakaryocytes.
Preclinical experiments revealed that megakaryocytes maintain HSC quiescence during homeostasis and promote HSC regeneration after chemotherapeutic stress.
The discovery suggests megakaryocytes might be used to treat patients with low blood cell counts and to expand HSCs for transplant.
The researchers described these findings in Nature Medicine.
The team examined the relationship between megakaryocytes and HSCs in mouse bone marrow. And they discovered that, as a terminally differentiated progeny, megakaryocytes regulate HSCs by performing two previously unknown functions.
“Megakaryocytes can directly regulate the amount of hematopoietic stem cells by telling the cells when they need to keep in the quiescent stage and when they need to start proliferating to meet increased demand,” said study author Meng Zhao, PhD, of the Stowers Institute for Medical Research in Kansas City, Missouri.
The researchers found that the protein transforming growth factor B1 (TGF-B1), contained in megakaryocytes, signaled quiescence.
And, when under stress from chemotherapy, megakaryocytes signaled fibroblast growth factor 1 (FGF1), to stimulate HSC proliferation.
“Our findings suggest that megakaryocytes are required for the recovery of hematopoietic stem cells post-chemotherapy,” said Linheng Li, PhD, also of the Stowers Institute.
The discovery could provide insight for using megakaryocyte-derived factors, such as TGF-B1 and FGF1, clinically to facilitate the regeneration of HSCs, he added.
Engineering a megakaryocyte niche that supports the growth of HSCs in culture is the next step for the researchers. They are also investigating whether a megakaryocyte niche can be used to help expand human HSCs in vitro for transplant.
These findings are supported by similar research also reported in Nature Medicine.
Trio-CES produces higher molecular diagnostic yield

Calvin, who was diagnosed
with Pitt-Hopkins Syndrome
via trio-CES
Credit: Lapidus family
A 3-pronged approach to clinical exome sequencing (CES) can provide a higher diagnostic yield than traditional molecular diagnostic methods, results of a new study suggest.
Investigators found that sequencing a patient’s exome together with his or her parents’—a method known as trio-CES—greatly improved the ability to reach a firm diagnosis in children with suspected genetic conditions.
This research was published in JAMA. It was released to coincide with a presentation at the American Society of Human Genetics Annual Meeting in San Diego.
The researchers performed CES on 814 patients with undiagnosed, suspected genetic conditions between January 2012 and August 2014. Sequencing was conducted as trio-CES or as proband-CES (only the affected individual sequenced) when parental samples were not available.
The team funneled the raw data through an informatics pipeline to identify variants from the standard human genome. Next, they applied a series of filters to the data based on the patient’s family history and other relevant aspects of his or her condition.
The investigators then hunted for all genes and mutations linked by medical literature to the patient’s symptoms. And a multidisciplinary team of experts reviewed the findings to reach a diagnosis.
Overall, 26% of patients (213/814) received a molecular diagnosis, with the causative variant(s) identified in a well-established clinical gene.
There was a significantly higher molecular diagnostic yield from cases performed as trio-CES relative to proband-CES—31% (127/410) and 22% (74/338), respectively.
In cases of developmental delay in children younger than 5 years (n=138), the molecular diagnosis rate was 41% (45/ 109) for trio-CES cases and 9% (2/23) for proband-CES cases.
The typical turnaround time for exome sequencing is less than 8 weeks, though test results have been returned to physicians within 10 days in medically urgent situations.
With preauthorization, many insurance providers cover the cost to sequence a child and both parents. If not, the out-of-pocket fee is about $6650.
“All families deserve a clear diagnosis of their child’s condition,” said study author Wayne Grody, MD, PhD, of the University of California, Los Angeles.
“Exome sequencing plays an important role in identifying the precise cause of a child’s illness. This is immediately useful to families and physicians in understanding how the disease occurred, preventing unnecessary testing, and developing the best strategies to treat it.”
The researchers noted, however, that the clinical implications of their findings should be better understood before trio- or proband-CES are routinely adopted.

Calvin, who was diagnosed
with Pitt-Hopkins Syndrome
via trio-CES
Credit: Lapidus family
A 3-pronged approach to clinical exome sequencing (CES) can provide a higher diagnostic yield than traditional molecular diagnostic methods, results of a new study suggest.
Investigators found that sequencing a patient’s exome together with his or her parents’—a method known as trio-CES—greatly improved the ability to reach a firm diagnosis in children with suspected genetic conditions.
This research was published in JAMA. It was released to coincide with a presentation at the American Society of Human Genetics Annual Meeting in San Diego.
The researchers performed CES on 814 patients with undiagnosed, suspected genetic conditions between January 2012 and August 2014. Sequencing was conducted as trio-CES or as proband-CES (only the affected individual sequenced) when parental samples were not available.
The team funneled the raw data through an informatics pipeline to identify variants from the standard human genome. Next, they applied a series of filters to the data based on the patient’s family history and other relevant aspects of his or her condition.
The investigators then hunted for all genes and mutations linked by medical literature to the patient’s symptoms. And a multidisciplinary team of experts reviewed the findings to reach a diagnosis.
Overall, 26% of patients (213/814) received a molecular diagnosis, with the causative variant(s) identified in a well-established clinical gene.
There was a significantly higher molecular diagnostic yield from cases performed as trio-CES relative to proband-CES—31% (127/410) and 22% (74/338), respectively.
In cases of developmental delay in children younger than 5 years (n=138), the molecular diagnosis rate was 41% (45/ 109) for trio-CES cases and 9% (2/23) for proband-CES cases.
The typical turnaround time for exome sequencing is less than 8 weeks, though test results have been returned to physicians within 10 days in medically urgent situations.
With preauthorization, many insurance providers cover the cost to sequence a child and both parents. If not, the out-of-pocket fee is about $6650.
“All families deserve a clear diagnosis of their child’s condition,” said study author Wayne Grody, MD, PhD, of the University of California, Los Angeles.
“Exome sequencing plays an important role in identifying the precise cause of a child’s illness. This is immediately useful to families and physicians in understanding how the disease occurred, preventing unnecessary testing, and developing the best strategies to treat it.”
The researchers noted, however, that the clinical implications of their findings should be better understood before trio- or proband-CES are routinely adopted.

Calvin, who was diagnosed
with Pitt-Hopkins Syndrome
via trio-CES
Credit: Lapidus family
A 3-pronged approach to clinical exome sequencing (CES) can provide a higher diagnostic yield than traditional molecular diagnostic methods, results of a new study suggest.
Investigators found that sequencing a patient’s exome together with his or her parents’—a method known as trio-CES—greatly improved the ability to reach a firm diagnosis in children with suspected genetic conditions.
This research was published in JAMA. It was released to coincide with a presentation at the American Society of Human Genetics Annual Meeting in San Diego.
The researchers performed CES on 814 patients with undiagnosed, suspected genetic conditions between January 2012 and August 2014. Sequencing was conducted as trio-CES or as proband-CES (only the affected individual sequenced) when parental samples were not available.
The team funneled the raw data through an informatics pipeline to identify variants from the standard human genome. Next, they applied a series of filters to the data based on the patient’s family history and other relevant aspects of his or her condition.
The investigators then hunted for all genes and mutations linked by medical literature to the patient’s symptoms. And a multidisciplinary team of experts reviewed the findings to reach a diagnosis.
Overall, 26% of patients (213/814) received a molecular diagnosis, with the causative variant(s) identified in a well-established clinical gene.
There was a significantly higher molecular diagnostic yield from cases performed as trio-CES relative to proband-CES—31% (127/410) and 22% (74/338), respectively.
In cases of developmental delay in children younger than 5 years (n=138), the molecular diagnosis rate was 41% (45/ 109) for trio-CES cases and 9% (2/23) for proband-CES cases.
The typical turnaround time for exome sequencing is less than 8 weeks, though test results have been returned to physicians within 10 days in medically urgent situations.
With preauthorization, many insurance providers cover the cost to sequence a child and both parents. If not, the out-of-pocket fee is about $6650.
“All families deserve a clear diagnosis of their child’s condition,” said study author Wayne Grody, MD, PhD, of the University of California, Los Angeles.
“Exome sequencing plays an important role in identifying the precise cause of a child’s illness. This is immediately useful to families and physicians in understanding how the disease occurred, preventing unnecessary testing, and developing the best strategies to treat it.”
The researchers noted, however, that the clinical implications of their findings should be better understood before trio- or proband-CES are routinely adopted.