User login
New formulation improves chemo drug

Credit: Larry Ostby
A new formulation of the chemotherapy drug cisplatin can significantly increase the drug’s ability to target and destroy cancer cells, a new study suggests.
Scientists constructed a modified version of cisplatin called Platin-M, which is designed to overcome treatment resistance by attacking mitochondria within cancer cells.
“You can think of mitochondria as a kind of powerhouse for the cell, generating the energy it needs to grow and reproduce,” said Shanta Dhar, PhD, of the University of Georgia in Athens, Georgia.
“This prodrug delivers cisplatin directly to the mitochondria in cancerous cells. Without that essential powerhouse, the cell cannot survive.”
Dr Dhar and her colleagues described the creation of this prodrug in the Proceedings of the National Academy of Sciences.
Sean Marrache, a graduate student in Dr Dhar’s lab, entrapped Platin-M in a specially designed nanoparticle that seeks out the mitochondria and releases the drug. Once inside, Platin-M interferes with the mitochondria’s DNA, triggering cell death.
The researchers tested Platin-M on neuroblastoma cells. In experiments using a cisplatin-resistant cell culture, Platin-M nanoparticles were roughly 17 times more active than cisplatin alone.
“This technique could become a treatment for a number of cancers, but it may prove most useful for more aggressive forms of cancer that are resistant to current therapies,” said Rakesh Pathak, PhD, a postdoctoral researcher in Dr Dhar’s lab.
However, the researchers cautioned that these results are preliminary, and more work is necessary before Platin-M enters clinical trials. Still, their early results in mouse models are encouraging, and they are currently developing safety trials in larger animals.
“Cisplatin is a well-studied chemotherapy, so we hope our unique formulation will enhance its efficacy,” Dr Dhar said. “We are excited about these early results, which look very promising.” ![]()

Credit: Larry Ostby
A new formulation of the chemotherapy drug cisplatin can significantly increase the drug’s ability to target and destroy cancer cells, a new study suggests.
Scientists constructed a modified version of cisplatin called Platin-M, which is designed to overcome treatment resistance by attacking mitochondria within cancer cells.
“You can think of mitochondria as a kind of powerhouse for the cell, generating the energy it needs to grow and reproduce,” said Shanta Dhar, PhD, of the University of Georgia in Athens, Georgia.
“This prodrug delivers cisplatin directly to the mitochondria in cancerous cells. Without that essential powerhouse, the cell cannot survive.”
Dr Dhar and her colleagues described the creation of this prodrug in the Proceedings of the National Academy of Sciences.
Sean Marrache, a graduate student in Dr Dhar’s lab, entrapped Platin-M in a specially designed nanoparticle that seeks out the mitochondria and releases the drug. Once inside, Platin-M interferes with the mitochondria’s DNA, triggering cell death.
The researchers tested Platin-M on neuroblastoma cells. In experiments using a cisplatin-resistant cell culture, Platin-M nanoparticles were roughly 17 times more active than cisplatin alone.
“This technique could become a treatment for a number of cancers, but it may prove most useful for more aggressive forms of cancer that are resistant to current therapies,” said Rakesh Pathak, PhD, a postdoctoral researcher in Dr Dhar’s lab.
However, the researchers cautioned that these results are preliminary, and more work is necessary before Platin-M enters clinical trials. Still, their early results in mouse models are encouraging, and they are currently developing safety trials in larger animals.
“Cisplatin is a well-studied chemotherapy, so we hope our unique formulation will enhance its efficacy,” Dr Dhar said. “We are excited about these early results, which look very promising.” ![]()

Credit: Larry Ostby
A new formulation of the chemotherapy drug cisplatin can significantly increase the drug’s ability to target and destroy cancer cells, a new study suggests.
Scientists constructed a modified version of cisplatin called Platin-M, which is designed to overcome treatment resistance by attacking mitochondria within cancer cells.
“You can think of mitochondria as a kind of powerhouse for the cell, generating the energy it needs to grow and reproduce,” said Shanta Dhar, PhD, of the University of Georgia in Athens, Georgia.
“This prodrug delivers cisplatin directly to the mitochondria in cancerous cells. Without that essential powerhouse, the cell cannot survive.”
Dr Dhar and her colleagues described the creation of this prodrug in the Proceedings of the National Academy of Sciences.
Sean Marrache, a graduate student in Dr Dhar’s lab, entrapped Platin-M in a specially designed nanoparticle that seeks out the mitochondria and releases the drug. Once inside, Platin-M interferes with the mitochondria’s DNA, triggering cell death.
The researchers tested Platin-M on neuroblastoma cells. In experiments using a cisplatin-resistant cell culture, Platin-M nanoparticles were roughly 17 times more active than cisplatin alone.
“This technique could become a treatment for a number of cancers, but it may prove most useful for more aggressive forms of cancer that are resistant to current therapies,” said Rakesh Pathak, PhD, a postdoctoral researcher in Dr Dhar’s lab.
However, the researchers cautioned that these results are preliminary, and more work is necessary before Platin-M enters clinical trials. Still, their early results in mouse models are encouraging, and they are currently developing safety trials in larger animals.
“Cisplatin is a well-studied chemotherapy, so we hope our unique formulation will enhance its efficacy,” Dr Dhar said. “We are excited about these early results, which look very promising.” ![]()
‘Herculean study’ reveals key regulators of malaria

lab’s mosquito insectory
The University of Nottingham
A researcher who battled malaria infection as a child is now fighting the disease in her lab and has made a discovery that may bring us closer to successfully disrupting the malaria parasite life-cycle.
Rita Tewari, PhD, of The University of Nottingham in the UK, and her colleagues have completed what she calls a “Herculean study” investigating the roles that 30 protein phosphatases and 72 kinases play as the malaria parasite develops.
Dr Tewari and her colleagues reported the results of this study in Cell Host and Microbe.
“This latest study identifies how protein phosphatases regulate parasite development and differentiation,” she said. “Our research provides a systematic functional analysis for all the 30 phosphatases in Plasmodium berghei, the parasite responsible for causing malaria in rodents.”
“These enzymes work in tandem with the protein kinases identified by the same team in a complementary study carried out in 2010. If we can find out what proteins are essential for these parasites to develop and divide, maybe we can target those proteins and arrest them with drugs or vaccines.”
Born and raised in Delhi, India, Dr Tewari had malaria 7 times as a child. She now leads her own malaria research lab at The University of Nottingham, complete with her own mosquito insectary.
It has taken her team, together with collaborators at Imperial College London, 8 years to identify every one of the protein phosphatases and protein kinases responsible for malaria parasite development.
Protein kinases and phosphatases are crucial for many stages of the malaria parasite lifecycle. And Dr Tewari’s group has been investigating protein kinases and phosphatases to better understand the basic developmental biology of malaria parasites.
Using a number of molecular cell biology and biochemical techniques, the researchers found that 16 of the 30 phosphatase genes they identified could not be knocked out. This suggests some of these genes could be future drug targets, as their presence is critical to parasite growth.
“Interestingly, out of the genes that could be knocked out [14], 6 were found to be crucial for sexual development and, hence, could be drug targets for parasite transmission to and from the mosquito,” Dr Tewari said.
“The research gathered here using the mouse malaria parasite can be directly related to the human malaria parasite, as many of the genes share a very similar homology, and symptoms of the diseases are very similar.” ![]()

lab’s mosquito insectory
The University of Nottingham
A researcher who battled malaria infection as a child is now fighting the disease in her lab and has made a discovery that may bring us closer to successfully disrupting the malaria parasite life-cycle.
Rita Tewari, PhD, of The University of Nottingham in the UK, and her colleagues have completed what she calls a “Herculean study” investigating the roles that 30 protein phosphatases and 72 kinases play as the malaria parasite develops.
Dr Tewari and her colleagues reported the results of this study in Cell Host and Microbe.
“This latest study identifies how protein phosphatases regulate parasite development and differentiation,” she said. “Our research provides a systematic functional analysis for all the 30 phosphatases in Plasmodium berghei, the parasite responsible for causing malaria in rodents.”
“These enzymes work in tandem with the protein kinases identified by the same team in a complementary study carried out in 2010. If we can find out what proteins are essential for these parasites to develop and divide, maybe we can target those proteins and arrest them with drugs or vaccines.”
Born and raised in Delhi, India, Dr Tewari had malaria 7 times as a child. She now leads her own malaria research lab at The University of Nottingham, complete with her own mosquito insectary.
It has taken her team, together with collaborators at Imperial College London, 8 years to identify every one of the protein phosphatases and protein kinases responsible for malaria parasite development.
Protein kinases and phosphatases are crucial for many stages of the malaria parasite lifecycle. And Dr Tewari’s group has been investigating protein kinases and phosphatases to better understand the basic developmental biology of malaria parasites.
Using a number of molecular cell biology and biochemical techniques, the researchers found that 16 of the 30 phosphatase genes they identified could not be knocked out. This suggests some of these genes could be future drug targets, as their presence is critical to parasite growth.
“Interestingly, out of the genes that could be knocked out [14], 6 were found to be crucial for sexual development and, hence, could be drug targets for parasite transmission to and from the mosquito,” Dr Tewari said.
“The research gathered here using the mouse malaria parasite can be directly related to the human malaria parasite, as many of the genes share a very similar homology, and symptoms of the diseases are very similar.” ![]()

lab’s mosquito insectory
The University of Nottingham
A researcher who battled malaria infection as a child is now fighting the disease in her lab and has made a discovery that may bring us closer to successfully disrupting the malaria parasite life-cycle.
Rita Tewari, PhD, of The University of Nottingham in the UK, and her colleagues have completed what she calls a “Herculean study” investigating the roles that 30 protein phosphatases and 72 kinases play as the malaria parasite develops.
Dr Tewari and her colleagues reported the results of this study in Cell Host and Microbe.
“This latest study identifies how protein phosphatases regulate parasite development and differentiation,” she said. “Our research provides a systematic functional analysis for all the 30 phosphatases in Plasmodium berghei, the parasite responsible for causing malaria in rodents.”
“These enzymes work in tandem with the protein kinases identified by the same team in a complementary study carried out in 2010. If we can find out what proteins are essential for these parasites to develop and divide, maybe we can target those proteins and arrest them with drugs or vaccines.”
Born and raised in Delhi, India, Dr Tewari had malaria 7 times as a child. She now leads her own malaria research lab at The University of Nottingham, complete with her own mosquito insectary.
It has taken her team, together with collaborators at Imperial College London, 8 years to identify every one of the protein phosphatases and protein kinases responsible for malaria parasite development.
Protein kinases and phosphatases are crucial for many stages of the malaria parasite lifecycle. And Dr Tewari’s group has been investigating protein kinases and phosphatases to better understand the basic developmental biology of malaria parasites.
Using a number of molecular cell biology and biochemical techniques, the researchers found that 16 of the 30 phosphatase genes they identified could not be knocked out. This suggests some of these genes could be future drug targets, as their presence is critical to parasite growth.
“Interestingly, out of the genes that could be knocked out [14], 6 were found to be crucial for sexual development and, hence, could be drug targets for parasite transmission to and from the mosquito,” Dr Tewari said.
“The research gathered here using the mouse malaria parasite can be directly related to the human malaria parasite, as many of the genes share a very similar homology, and symptoms of the diseases are very similar.” ![]()
Increasing AYA enrollment in cancer trials

patient and her father
Credit: Rhoda Baer
Age limits on clinical trials must be more flexible to allow more adolescent and young adult (AYA) cancer patients the opportunity to access new treatments, according to a report published in The Lancet Oncology.
The report’s authors discovered that expanding age eligibility criteria for cancer trials increased the enrollment of AYA patients and patients belonging to other age groups. But there is still room for improvement, according to the authors.
“[R]ight now, too many of our young patients are needlessly falling through the gap between pediatric and adult cancer trials,” said Lorna Fern, PhD, of University College London Hospitals in the UK.
“By encouraging doctors to take into account the full age range of patients affected by individual types of cancer, we’ve shown that it’s possible to design trials that include teenage cancer patients and, importantly, that better match the underlying biology of the disease and the people affected.”
To assess AYA enrollment in cancer trials, Dr Fern and her colleagues looked at 68,275 cancer patients aged 0 to 59 years. They were diagnosed with leukemias, lymphomas, or solid tumor malignancies between April 1, 2005, and March 31, 2010.
During this 6-year period, trial participation increased among all age groups. There was a 13% increase in participation among 15- to 19-year-olds (from 24% to 37%), a 5% increase among 20- to 24-year-olds (from 13% to 18%), and a 6% increase among 0- to 14-year-olds (from 52% to 58%).
Dr Fern and her colleagues said the rise in enrollment, particularly among AYAs, was due to increased availability and access to trials; increased awareness from healthcare professionals, patients, and the public about research; and the opening of trials with broader age limits that allow AYAs to enter trials.
In light of this study, Cancer Research UK has started asking researchers to justify age restrictions on new studies, in an effort to recruit more AYA cancer patients onto its trials.
“[I]t’s vital that effective treatments are being developed to tackle cancer across all age brackets,” said Kate Law, Cancer Research UK’s director of clinical trials.
“We now only accept age limits on our clinical trials if they are backed up by hard evidence, which will hopefully mean more young cancer patients get the chance to contribute to research and have the latest experimental treatments.” ![]()

patient and her father
Credit: Rhoda Baer
Age limits on clinical trials must be more flexible to allow more adolescent and young adult (AYA) cancer patients the opportunity to access new treatments, according to a report published in The Lancet Oncology.
The report’s authors discovered that expanding age eligibility criteria for cancer trials increased the enrollment of AYA patients and patients belonging to other age groups. But there is still room for improvement, according to the authors.
“[R]ight now, too many of our young patients are needlessly falling through the gap between pediatric and adult cancer trials,” said Lorna Fern, PhD, of University College London Hospitals in the UK.
“By encouraging doctors to take into account the full age range of patients affected by individual types of cancer, we’ve shown that it’s possible to design trials that include teenage cancer patients and, importantly, that better match the underlying biology of the disease and the people affected.”
To assess AYA enrollment in cancer trials, Dr Fern and her colleagues looked at 68,275 cancer patients aged 0 to 59 years. They were diagnosed with leukemias, lymphomas, or solid tumor malignancies between April 1, 2005, and March 31, 2010.
During this 6-year period, trial participation increased among all age groups. There was a 13% increase in participation among 15- to 19-year-olds (from 24% to 37%), a 5% increase among 20- to 24-year-olds (from 13% to 18%), and a 6% increase among 0- to 14-year-olds (from 52% to 58%).
Dr Fern and her colleagues said the rise in enrollment, particularly among AYAs, was due to increased availability and access to trials; increased awareness from healthcare professionals, patients, and the public about research; and the opening of trials with broader age limits that allow AYAs to enter trials.
In light of this study, Cancer Research UK has started asking researchers to justify age restrictions on new studies, in an effort to recruit more AYA cancer patients onto its trials.
“[I]t’s vital that effective treatments are being developed to tackle cancer across all age brackets,” said Kate Law, Cancer Research UK’s director of clinical trials.
“We now only accept age limits on our clinical trials if they are backed up by hard evidence, which will hopefully mean more young cancer patients get the chance to contribute to research and have the latest experimental treatments.” ![]()

patient and her father
Credit: Rhoda Baer
Age limits on clinical trials must be more flexible to allow more adolescent and young adult (AYA) cancer patients the opportunity to access new treatments, according to a report published in The Lancet Oncology.
The report’s authors discovered that expanding age eligibility criteria for cancer trials increased the enrollment of AYA patients and patients belonging to other age groups. But there is still room for improvement, according to the authors.
“[R]ight now, too many of our young patients are needlessly falling through the gap between pediatric and adult cancer trials,” said Lorna Fern, PhD, of University College London Hospitals in the UK.
“By encouraging doctors to take into account the full age range of patients affected by individual types of cancer, we’ve shown that it’s possible to design trials that include teenage cancer patients and, importantly, that better match the underlying biology of the disease and the people affected.”
To assess AYA enrollment in cancer trials, Dr Fern and her colleagues looked at 68,275 cancer patients aged 0 to 59 years. They were diagnosed with leukemias, lymphomas, or solid tumor malignancies between April 1, 2005, and March 31, 2010.
During this 6-year period, trial participation increased among all age groups. There was a 13% increase in participation among 15- to 19-year-olds (from 24% to 37%), a 5% increase among 20- to 24-year-olds (from 13% to 18%), and a 6% increase among 0- to 14-year-olds (from 52% to 58%).
Dr Fern and her colleagues said the rise in enrollment, particularly among AYAs, was due to increased availability and access to trials; increased awareness from healthcare professionals, patients, and the public about research; and the opening of trials with broader age limits that allow AYAs to enter trials.
In light of this study, Cancer Research UK has started asking researchers to justify age restrictions on new studies, in an effort to recruit more AYA cancer patients onto its trials.
“[I]t’s vital that effective treatments are being developed to tackle cancer across all age brackets,” said Kate Law, Cancer Research UK’s director of clinical trials.
“We now only accept age limits on our clinical trials if they are backed up by hard evidence, which will hopefully mean more young cancer patients get the chance to contribute to research and have the latest experimental treatments.” ![]()
Adipose-derived SCs can resist methotrexate

A new study indicates that adipose-derived stem cells (ASCs) are highly resistant to the chemotherapy drug methotrexate (MTX).
Cultured ASCs and tissue samples that included ASCs were able to withstand exposure to MTX quite well. The drug had little or no effect on ASC viability, division, senescence, or differentiation.
The researchers believe these findings could prove significant for cancer patients, particularly children with acute lymphoblastic leukemia.
“Kids undergo chemotherapy at such an important time, when they should be growing, but, instead, they are introduced to this very harsh environment where bone cells are damaged with these drugs,” said study author Olivia Beane, a graduate student at Brown University in Providence, Rhode Island.
“That leads to major long-term side effects, including osteoporosis and bone defects. If we found a stem cell that was resistant to the chemotherapeutic agent and could promote bone growth by becoming bone itself, then maybe they wouldn’t have these issues.”
Beane’s work, which appears in Experimental Cell Research, grew out of more basic research. She was originally looking for chemicals that could help purify ASCs from mixed cell cultures to encourage their proliferation.
Among other things, she tried chemotherapy drugs, speculating that ASCs might withstand a drug that other cells could not. The idea that this could help cancer patients did not come until later.
To explore potential cancer applications, Beane and her colleagues exposed pure human ASC cultures, stromal vascular fraction (SVF) tissue samples (which include ASCs and several other cell types), and cultures of human fibroblast cells to medically relevant concentrations of chemotherapy drugs for 24 hours.
The researchers then measured how those cell populations fared over the next 10 days. They also measured the ability of MTX-exposed ASCs, both alone and in SVF, to proliferate and differentiate.
In contrast to the fibroblast controls, the ASCs withstood a variety of MTX doses. The drug had little or no effect on ASC viability, cell division, senescence, or differentiation. ASCs also resisted vincristine to an extent, but they could not withstand exposure to cytarabine or etoposide.
The SVF tissue samples withstood MTX doses well too. That is significant, according to the researchers, because the tissue would be clinically useful if an ASC-based therapy were ever developed for cancer patients. Hypothetically, fresh SVF could be harvested from the fat of a donor and injected into bone tissue, delivering ASCs to the site.
To understand why ASCs resist MTX, the researchers conducted further tests. MTX shuts down DNA biosynthesis by binding the protein dihydrofolate reductase so it is unavailable to assist in that essential task.
The testing showed that ASCs ramped up dihydrofolate reductase levels upon exposure to the drug. They produced enough to overcome a clinically relevant dose of MTX.
Now, the researchers are eager to see if they can translate these findings to deliver a medical benefit for cancer patients. To that end, the team is planning several more experiments.
One is to test ASC survival and performance after 48- and 72-hour exposures to MTX. Another is to begin examining how the cells fare in mouse models of chemotherapy. The researchers plan to directly compare ASCs and bone marrow-derived stem cells exposed to various chemotherapies. ![]()

A new study indicates that adipose-derived stem cells (ASCs) are highly resistant to the chemotherapy drug methotrexate (MTX).
Cultured ASCs and tissue samples that included ASCs were able to withstand exposure to MTX quite well. The drug had little or no effect on ASC viability, division, senescence, or differentiation.
The researchers believe these findings could prove significant for cancer patients, particularly children with acute lymphoblastic leukemia.
“Kids undergo chemotherapy at such an important time, when they should be growing, but, instead, they are introduced to this very harsh environment where bone cells are damaged with these drugs,” said study author Olivia Beane, a graduate student at Brown University in Providence, Rhode Island.
“That leads to major long-term side effects, including osteoporosis and bone defects. If we found a stem cell that was resistant to the chemotherapeutic agent and could promote bone growth by becoming bone itself, then maybe they wouldn’t have these issues.”
Beane’s work, which appears in Experimental Cell Research, grew out of more basic research. She was originally looking for chemicals that could help purify ASCs from mixed cell cultures to encourage their proliferation.
Among other things, she tried chemotherapy drugs, speculating that ASCs might withstand a drug that other cells could not. The idea that this could help cancer patients did not come until later.
To explore potential cancer applications, Beane and her colleagues exposed pure human ASC cultures, stromal vascular fraction (SVF) tissue samples (which include ASCs and several other cell types), and cultures of human fibroblast cells to medically relevant concentrations of chemotherapy drugs for 24 hours.
The researchers then measured how those cell populations fared over the next 10 days. They also measured the ability of MTX-exposed ASCs, both alone and in SVF, to proliferate and differentiate.
In contrast to the fibroblast controls, the ASCs withstood a variety of MTX doses. The drug had little or no effect on ASC viability, cell division, senescence, or differentiation. ASCs also resisted vincristine to an extent, but they could not withstand exposure to cytarabine or etoposide.
The SVF tissue samples withstood MTX doses well too. That is significant, according to the researchers, because the tissue would be clinically useful if an ASC-based therapy were ever developed for cancer patients. Hypothetically, fresh SVF could be harvested from the fat of a donor and injected into bone tissue, delivering ASCs to the site.
To understand why ASCs resist MTX, the researchers conducted further tests. MTX shuts down DNA biosynthesis by binding the protein dihydrofolate reductase so it is unavailable to assist in that essential task.
The testing showed that ASCs ramped up dihydrofolate reductase levels upon exposure to the drug. They produced enough to overcome a clinically relevant dose of MTX.
Now, the researchers are eager to see if they can translate these findings to deliver a medical benefit for cancer patients. To that end, the team is planning several more experiments.
One is to test ASC survival and performance after 48- and 72-hour exposures to MTX. Another is to begin examining how the cells fare in mouse models of chemotherapy. The researchers plan to directly compare ASCs and bone marrow-derived stem cells exposed to various chemotherapies. ![]()

A new study indicates that adipose-derived stem cells (ASCs) are highly resistant to the chemotherapy drug methotrexate (MTX).
Cultured ASCs and tissue samples that included ASCs were able to withstand exposure to MTX quite well. The drug had little or no effect on ASC viability, division, senescence, or differentiation.
The researchers believe these findings could prove significant for cancer patients, particularly children with acute lymphoblastic leukemia.
“Kids undergo chemotherapy at such an important time, when they should be growing, but, instead, they are introduced to this very harsh environment where bone cells are damaged with these drugs,” said study author Olivia Beane, a graduate student at Brown University in Providence, Rhode Island.
“That leads to major long-term side effects, including osteoporosis and bone defects. If we found a stem cell that was resistant to the chemotherapeutic agent and could promote bone growth by becoming bone itself, then maybe they wouldn’t have these issues.”
Beane’s work, which appears in Experimental Cell Research, grew out of more basic research. She was originally looking for chemicals that could help purify ASCs from mixed cell cultures to encourage their proliferation.
Among other things, she tried chemotherapy drugs, speculating that ASCs might withstand a drug that other cells could not. The idea that this could help cancer patients did not come until later.
To explore potential cancer applications, Beane and her colleagues exposed pure human ASC cultures, stromal vascular fraction (SVF) tissue samples (which include ASCs and several other cell types), and cultures of human fibroblast cells to medically relevant concentrations of chemotherapy drugs for 24 hours.
The researchers then measured how those cell populations fared over the next 10 days. They also measured the ability of MTX-exposed ASCs, both alone and in SVF, to proliferate and differentiate.
In contrast to the fibroblast controls, the ASCs withstood a variety of MTX doses. The drug had little or no effect on ASC viability, cell division, senescence, or differentiation. ASCs also resisted vincristine to an extent, but they could not withstand exposure to cytarabine or etoposide.
The SVF tissue samples withstood MTX doses well too. That is significant, according to the researchers, because the tissue would be clinically useful if an ASC-based therapy were ever developed for cancer patients. Hypothetically, fresh SVF could be harvested from the fat of a donor and injected into bone tissue, delivering ASCs to the site.
To understand why ASCs resist MTX, the researchers conducted further tests. MTX shuts down DNA biosynthesis by binding the protein dihydrofolate reductase so it is unavailable to assist in that essential task.
The testing showed that ASCs ramped up dihydrofolate reductase levels upon exposure to the drug. They produced enough to overcome a clinically relevant dose of MTX.
Now, the researchers are eager to see if they can translate these findings to deliver a medical benefit for cancer patients. To that end, the team is planning several more experiments.
One is to test ASC survival and performance after 48- and 72-hour exposures to MTX. Another is to begin examining how the cells fare in mouse models of chemotherapy. The researchers plan to directly compare ASCs and bone marrow-derived stem cells exposed to various chemotherapies. ![]()
Circadian disruption negatively affects RBCs

Credit: NHLBI
MANCHESTER—Preclinical research indicates that circadian disruption has severe adverse effects on red blood cells (RBCs), a finding that might possibly explain the high incidence of heart disease observed in shift workers.
The study also showed the negative effects could be reduced under hypoxic conditions. Hypoxia in combination with circadian disruption produced fresh RBCs.
And this, according to researchers, suggests blood donations might help decrease the risk of cardiovascular disease in shift workers.
This research was presented at the 2014 Annual Main Meeting of the Society for Experimental Biology (SEB). It was also published in Chronobiology International.
The researchers, led by Margit Egg, PhD, of the University of Innsbruck in Austria, set out to investigate the impact of circadian disruption on hypoxic signaling and the cardiovascular system.
The team used zebrafish, a model organism that, like humans, is active during the day. To disrupt circadian rhythms, the researchers subjected the fish to alternate short days (7 hours) and long days (21 hours), resembling shift patterns common in industry.
Results showed that circadian disruption increased the number of aged RBCs that accumulated in the blood vessels.
“Normally, there is a balance between newly produced red blood cells and old ones which are removed from the blood,” Dr Egg noted.
Old cells are less flexible and become stuck in the spleen and liver, where they are engulfed by white blood cells. Circadian disruption appears to inhibit this removal process, but the researchers are unsure why this is the case.
They do know that having large aggregates of old RBCs in the vessels increases the chance of a clot that could lead to a heart attack. This may explain why shift workers have a 30% higher risk of cardiovascular disease. In addition, the decreased functionality of the aged cells reduces the oxygen-carrying capacity of the blood.
However, the researchers also found that zebrafish were less affected by circadian disruption if they were simultaneously exposed to hypoxic conditions. This is because hypoxia stimulates the production of fresh RBCs.
The team noted that the cell signaling pathways that regulate circadian rhythms and the hypoxic response are intrinsically linked. This is based on the observation that genes activated by hypoxia, such as erythropoietin, normally show a daily rhythm of activity that becomes disturbed under hypoxic conditions.
“In zebrafish, hypoxia in combination with jetlag led to the production of fresh red blood cells, counteracting the harmful consequences of jetlag and reducing mortality by 10%,” Dr Egg noted.
“Blood donations in humans also stimulate the generation of new fresh erythrocytes. Therefore, blood donations on a regular basis might be a very simple measure to help decrease the cardiovascular risk in human shift workers.”
Dr Egg and her colleagues are currently investigating whether circadian disruption affects any other physiological processes, apart from the cardiovascular system. ![]()

Credit: NHLBI
MANCHESTER—Preclinical research indicates that circadian disruption has severe adverse effects on red blood cells (RBCs), a finding that might possibly explain the high incidence of heart disease observed in shift workers.
The study also showed the negative effects could be reduced under hypoxic conditions. Hypoxia in combination with circadian disruption produced fresh RBCs.
And this, according to researchers, suggests blood donations might help decrease the risk of cardiovascular disease in shift workers.
This research was presented at the 2014 Annual Main Meeting of the Society for Experimental Biology (SEB). It was also published in Chronobiology International.
The researchers, led by Margit Egg, PhD, of the University of Innsbruck in Austria, set out to investigate the impact of circadian disruption on hypoxic signaling and the cardiovascular system.
The team used zebrafish, a model organism that, like humans, is active during the day. To disrupt circadian rhythms, the researchers subjected the fish to alternate short days (7 hours) and long days (21 hours), resembling shift patterns common in industry.
Results showed that circadian disruption increased the number of aged RBCs that accumulated in the blood vessels.
“Normally, there is a balance between newly produced red blood cells and old ones which are removed from the blood,” Dr Egg noted.
Old cells are less flexible and become stuck in the spleen and liver, where they are engulfed by white blood cells. Circadian disruption appears to inhibit this removal process, but the researchers are unsure why this is the case.
They do know that having large aggregates of old RBCs in the vessels increases the chance of a clot that could lead to a heart attack. This may explain why shift workers have a 30% higher risk of cardiovascular disease. In addition, the decreased functionality of the aged cells reduces the oxygen-carrying capacity of the blood.
However, the researchers also found that zebrafish were less affected by circadian disruption if they were simultaneously exposed to hypoxic conditions. This is because hypoxia stimulates the production of fresh RBCs.
The team noted that the cell signaling pathways that regulate circadian rhythms and the hypoxic response are intrinsically linked. This is based on the observation that genes activated by hypoxia, such as erythropoietin, normally show a daily rhythm of activity that becomes disturbed under hypoxic conditions.
“In zebrafish, hypoxia in combination with jetlag led to the production of fresh red blood cells, counteracting the harmful consequences of jetlag and reducing mortality by 10%,” Dr Egg noted.
“Blood donations in humans also stimulate the generation of new fresh erythrocytes. Therefore, blood donations on a regular basis might be a very simple measure to help decrease the cardiovascular risk in human shift workers.”
Dr Egg and her colleagues are currently investigating whether circadian disruption affects any other physiological processes, apart from the cardiovascular system. ![]()

Credit: NHLBI
MANCHESTER—Preclinical research indicates that circadian disruption has severe adverse effects on red blood cells (RBCs), a finding that might possibly explain the high incidence of heart disease observed in shift workers.
The study also showed the negative effects could be reduced under hypoxic conditions. Hypoxia in combination with circadian disruption produced fresh RBCs.
And this, according to researchers, suggests blood donations might help decrease the risk of cardiovascular disease in shift workers.
This research was presented at the 2014 Annual Main Meeting of the Society for Experimental Biology (SEB). It was also published in Chronobiology International.
The researchers, led by Margit Egg, PhD, of the University of Innsbruck in Austria, set out to investigate the impact of circadian disruption on hypoxic signaling and the cardiovascular system.
The team used zebrafish, a model organism that, like humans, is active during the day. To disrupt circadian rhythms, the researchers subjected the fish to alternate short days (7 hours) and long days (21 hours), resembling shift patterns common in industry.
Results showed that circadian disruption increased the number of aged RBCs that accumulated in the blood vessels.
“Normally, there is a balance between newly produced red blood cells and old ones which are removed from the blood,” Dr Egg noted.
Old cells are less flexible and become stuck in the spleen and liver, where they are engulfed by white blood cells. Circadian disruption appears to inhibit this removal process, but the researchers are unsure why this is the case.
They do know that having large aggregates of old RBCs in the vessels increases the chance of a clot that could lead to a heart attack. This may explain why shift workers have a 30% higher risk of cardiovascular disease. In addition, the decreased functionality of the aged cells reduces the oxygen-carrying capacity of the blood.
However, the researchers also found that zebrafish were less affected by circadian disruption if they were simultaneously exposed to hypoxic conditions. This is because hypoxia stimulates the production of fresh RBCs.
The team noted that the cell signaling pathways that regulate circadian rhythms and the hypoxic response are intrinsically linked. This is based on the observation that genes activated by hypoxia, such as erythropoietin, normally show a daily rhythm of activity that becomes disturbed under hypoxic conditions.
“In zebrafish, hypoxia in combination with jetlag led to the production of fresh red blood cells, counteracting the harmful consequences of jetlag and reducing mortality by 10%,” Dr Egg noted.
“Blood donations in humans also stimulate the generation of new fresh erythrocytes. Therefore, blood donations on a regular basis might be a very simple measure to help decrease the cardiovascular risk in human shift workers.”
Dr Egg and her colleagues are currently investigating whether circadian disruption affects any other physiological processes, apart from the cardiovascular system. ![]()
New compound blocks essential enzyme

Credit: Peter H. Seeberger
A novel compound can inhibit an enzyme that is essential for malaria parasite survival, according to research published in PLOS Biology.
Researchers believe that creating this compound, WEHI-916, is the first step toward developing a new class of antimalarial drugs that could cure and prevent malaria infections caused by all species of the parasite, including those resistant to existing drugs.
The group developed WEHI-916 to block the enzyme Plasmepsin V. They previously showed Plasmepsin V is responsible for controlling the transport of proteins in and out of the malaria parasite.
Now, they’ve used WEHI-916 to prove the importance of Plasmepsin V to the survival of both Plasmodium vivax and Plasmodium falciparum.
“Researchers, including us, had been trying, without success, to learn more about Plasmepsin V using standard genetic techniques,” said study author Just Boddey, PhD, of The Walter and Eliza Hall Institute of Medical Research in Parkville, Victoria, Australia.
“Our idea was to create a drug-like compound that would block Plasmepsin V so we could investigate its importance. We found that blocking Plasmepsin V kills malaria parasites and delivered a new and effective potential drug at the same time.”
Plasmepsin V was an ideal drug target because its inhibition effectively halted the transport of hundreds of malaria proteins, Dr Boddey noted.
“The Plasmodium parasite needs to produce and deliver over 300 different proteins to the red blood cell to survive in the body and hide from the host’s immune system,” he said. “Instead of targeting individual proteins, we can block Plasmepsin V and prevent all of those proteins from leaving the parasite.”
The researchers believe these findings could aid the development of drugs that are effective in curing malaria caused by all 5 species of Plasmodium parasite.
“Our study has shown that Plasmepsin V is a key enzyme in [P vivax and P falciparum], and WEHI-916 can inhibit Plasmepsin V isolated from both of them,” said study author Brad Sleebs, PhD, also of The Walter and Eliza Hall Institute.
“Not only does this compound enable us to prove Plasmepsin V is an excellent drug target, it is a starting point for a research program that could lead to a new class of antimalarial drugs.”
Now, the researchers have turned their attention to developing WEHI-916 and related compounds for human use.
“We are now examining in our insectary whether Plasmepsin V could be a target during other stages of the malaria lifecycle,” Dr Boddey said. “The enzyme is present in the parasites that first infect humans in the liver, as well as in parasite forms that exit humans and infect mosquitoes.”
“If WEHI-916 kills the parasite during these stages as well, it will mean any drugs that target Plasmepsin V can be used as a preventative as well as a cure.” ![]()

Credit: Peter H. Seeberger
A novel compound can inhibit an enzyme that is essential for malaria parasite survival, according to research published in PLOS Biology.
Researchers believe that creating this compound, WEHI-916, is the first step toward developing a new class of antimalarial drugs that could cure and prevent malaria infections caused by all species of the parasite, including those resistant to existing drugs.
The group developed WEHI-916 to block the enzyme Plasmepsin V. They previously showed Plasmepsin V is responsible for controlling the transport of proteins in and out of the malaria parasite.
Now, they’ve used WEHI-916 to prove the importance of Plasmepsin V to the survival of both Plasmodium vivax and Plasmodium falciparum.
“Researchers, including us, had been trying, without success, to learn more about Plasmepsin V using standard genetic techniques,” said study author Just Boddey, PhD, of The Walter and Eliza Hall Institute of Medical Research in Parkville, Victoria, Australia.
“Our idea was to create a drug-like compound that would block Plasmepsin V so we could investigate its importance. We found that blocking Plasmepsin V kills malaria parasites and delivered a new and effective potential drug at the same time.”
Plasmepsin V was an ideal drug target because its inhibition effectively halted the transport of hundreds of malaria proteins, Dr Boddey noted.
“The Plasmodium parasite needs to produce and deliver over 300 different proteins to the red blood cell to survive in the body and hide from the host’s immune system,” he said. “Instead of targeting individual proteins, we can block Plasmepsin V and prevent all of those proteins from leaving the parasite.”
The researchers believe these findings could aid the development of drugs that are effective in curing malaria caused by all 5 species of Plasmodium parasite.
“Our study has shown that Plasmepsin V is a key enzyme in [P vivax and P falciparum], and WEHI-916 can inhibit Plasmepsin V isolated from both of them,” said study author Brad Sleebs, PhD, also of The Walter and Eliza Hall Institute.
“Not only does this compound enable us to prove Plasmepsin V is an excellent drug target, it is a starting point for a research program that could lead to a new class of antimalarial drugs.”
Now, the researchers have turned their attention to developing WEHI-916 and related compounds for human use.
“We are now examining in our insectary whether Plasmepsin V could be a target during other stages of the malaria lifecycle,” Dr Boddey said. “The enzyme is present in the parasites that first infect humans in the liver, as well as in parasite forms that exit humans and infect mosquitoes.”
“If WEHI-916 kills the parasite during these stages as well, it will mean any drugs that target Plasmepsin V can be used as a preventative as well as a cure.” ![]()

Credit: Peter H. Seeberger
A novel compound can inhibit an enzyme that is essential for malaria parasite survival, according to research published in PLOS Biology.
Researchers believe that creating this compound, WEHI-916, is the first step toward developing a new class of antimalarial drugs that could cure and prevent malaria infections caused by all species of the parasite, including those resistant to existing drugs.
The group developed WEHI-916 to block the enzyme Plasmepsin V. They previously showed Plasmepsin V is responsible for controlling the transport of proteins in and out of the malaria parasite.
Now, they’ve used WEHI-916 to prove the importance of Plasmepsin V to the survival of both Plasmodium vivax and Plasmodium falciparum.
“Researchers, including us, had been trying, without success, to learn more about Plasmepsin V using standard genetic techniques,” said study author Just Boddey, PhD, of The Walter and Eliza Hall Institute of Medical Research in Parkville, Victoria, Australia.
“Our idea was to create a drug-like compound that would block Plasmepsin V so we could investigate its importance. We found that blocking Plasmepsin V kills malaria parasites and delivered a new and effective potential drug at the same time.”
Plasmepsin V was an ideal drug target because its inhibition effectively halted the transport of hundreds of malaria proteins, Dr Boddey noted.
“The Plasmodium parasite needs to produce and deliver over 300 different proteins to the red blood cell to survive in the body and hide from the host’s immune system,” he said. “Instead of targeting individual proteins, we can block Plasmepsin V and prevent all of those proteins from leaving the parasite.”
The researchers believe these findings could aid the development of drugs that are effective in curing malaria caused by all 5 species of Plasmodium parasite.
“Our study has shown that Plasmepsin V is a key enzyme in [P vivax and P falciparum], and WEHI-916 can inhibit Plasmepsin V isolated from both of them,” said study author Brad Sleebs, PhD, also of The Walter and Eliza Hall Institute.
“Not only does this compound enable us to prove Plasmepsin V is an excellent drug target, it is a starting point for a research program that could lead to a new class of antimalarial drugs.”
Now, the researchers have turned their attention to developing WEHI-916 and related compounds for human use.
“We are now examining in our insectary whether Plasmepsin V could be a target during other stages of the malaria lifecycle,” Dr Boddey said. “The enzyme is present in the parasites that first infect humans in the liver, as well as in parasite forms that exit humans and infect mosquitoes.”
“If WEHI-916 kills the parasite during these stages as well, it will mean any drugs that target Plasmepsin V can be used as a preventative as well as a cure.” ![]()
Unsuspected aspect of immune regulation revealed

Immunologists may have discovered an additional role for B cells. Their research suggests the cells participate in the development of regulatory T cells (Tregs).
Until now, the only non-thymic cells known to aid Treg production were dendritic cells, which travel to the thymus to deliver antigens.
The new research, published in the Journal of Immunology, suggests B cells can do the same thing.
B cells were previously thought to specialize only in antibody production. With their newly discovered role, the cells become much more interesting and complex characters, according to the researchers.
The findings mean B cells could have useful applications for treating transplant patients and those with autoimmune disorders.
“Regulatory T cells are critical in the outcome of an immune response, so anything that regulates them becomes very interesting to immunologists,” said study author Shane Grey, PhD, of the Garvan Institute of Medical Research in Darlinghurst, New South Wales, Australia.
“Right now, there are clinical trials around the world looking to expand populations of these cells in patients. Researchers are also working on ways to grow regulatory cells in the laboratory—to infuse into patients as therapy. Our finding suggests it should be possible to set up systems that harness B cells to expand regulatory cells.”
Dr Grey and his colleagues worked with mice genetically modified to express high levels of BAFF, which increases B-cell survival. The higher number of B cells overall allowed researchers to track the activity of B cells in the thymus.
“It has been known for years that some B cells travel to the thymus, but no one has understood why,” said study author Stacey Walters, also of the Garvan Institute of Medical Research.
“Our experiments showed clearly that B cells participated in the creation of regulatory T cells. The more B cells that were in the thymus, the higher the number of regulatory cells generated. That direct correlation raises interesting possibilities. One possibility is using BAFF, a non-toxic substance, to ramp up the B-cell count of patients before transplant procedures.”
Research has suggested that Tregs can reduce the risk of graft-vs-host disease, promote enhanced immune reconstitution, and decrease the incidence of infectious complications in stem cell transplant recipients. And several studies have shown that high levels of Tregs can prevent graft rejection after solid organ transplant. ![]()

Immunologists may have discovered an additional role for B cells. Their research suggests the cells participate in the development of regulatory T cells (Tregs).
Until now, the only non-thymic cells known to aid Treg production were dendritic cells, which travel to the thymus to deliver antigens.
The new research, published in the Journal of Immunology, suggests B cells can do the same thing.
B cells were previously thought to specialize only in antibody production. With their newly discovered role, the cells become much more interesting and complex characters, according to the researchers.
The findings mean B cells could have useful applications for treating transplant patients and those with autoimmune disorders.
“Regulatory T cells are critical in the outcome of an immune response, so anything that regulates them becomes very interesting to immunologists,” said study author Shane Grey, PhD, of the Garvan Institute of Medical Research in Darlinghurst, New South Wales, Australia.
“Right now, there are clinical trials around the world looking to expand populations of these cells in patients. Researchers are also working on ways to grow regulatory cells in the laboratory—to infuse into patients as therapy. Our finding suggests it should be possible to set up systems that harness B cells to expand regulatory cells.”
Dr Grey and his colleagues worked with mice genetically modified to express high levels of BAFF, which increases B-cell survival. The higher number of B cells overall allowed researchers to track the activity of B cells in the thymus.
“It has been known for years that some B cells travel to the thymus, but no one has understood why,” said study author Stacey Walters, also of the Garvan Institute of Medical Research.
“Our experiments showed clearly that B cells participated in the creation of regulatory T cells. The more B cells that were in the thymus, the higher the number of regulatory cells generated. That direct correlation raises interesting possibilities. One possibility is using BAFF, a non-toxic substance, to ramp up the B-cell count of patients before transplant procedures.”
Research has suggested that Tregs can reduce the risk of graft-vs-host disease, promote enhanced immune reconstitution, and decrease the incidence of infectious complications in stem cell transplant recipients. And several studies have shown that high levels of Tregs can prevent graft rejection after solid organ transplant. ![]()

Immunologists may have discovered an additional role for B cells. Their research suggests the cells participate in the development of regulatory T cells (Tregs).
Until now, the only non-thymic cells known to aid Treg production were dendritic cells, which travel to the thymus to deliver antigens.
The new research, published in the Journal of Immunology, suggests B cells can do the same thing.
B cells were previously thought to specialize only in antibody production. With their newly discovered role, the cells become much more interesting and complex characters, according to the researchers.
The findings mean B cells could have useful applications for treating transplant patients and those with autoimmune disorders.
“Regulatory T cells are critical in the outcome of an immune response, so anything that regulates them becomes very interesting to immunologists,” said study author Shane Grey, PhD, of the Garvan Institute of Medical Research in Darlinghurst, New South Wales, Australia.
“Right now, there are clinical trials around the world looking to expand populations of these cells in patients. Researchers are also working on ways to grow regulatory cells in the laboratory—to infuse into patients as therapy. Our finding suggests it should be possible to set up systems that harness B cells to expand regulatory cells.”
Dr Grey and his colleagues worked with mice genetically modified to express high levels of BAFF, which increases B-cell survival. The higher number of B cells overall allowed researchers to track the activity of B cells in the thymus.
“It has been known for years that some B cells travel to the thymus, but no one has understood why,” said study author Stacey Walters, also of the Garvan Institute of Medical Research.
“Our experiments showed clearly that B cells participated in the creation of regulatory T cells. The more B cells that were in the thymus, the higher the number of regulatory cells generated. That direct correlation raises interesting possibilities. One possibility is using BAFF, a non-toxic substance, to ramp up the B-cell count of patients before transplant procedures.”
Research has suggested that Tregs can reduce the risk of graft-vs-host disease, promote enhanced immune reconstitution, and decrease the incidence of infectious complications in stem cell transplant recipients. And several studies have shown that high levels of Tregs can prevent graft rejection after solid organ transplant.
Mixing meds and supplements to dangerous effect

Credit: CDC
A new study indicates that a fair share of patients may be mixing the herbal supplement St. John’s wort with prescribed medications, which can have dangerous results.
St. John’s wort can reduce the concentration of numerous drugs in the body, including anticoagulants and chemotherapeutic agents. And this can result in impaired effectiveness and treatment failure.
But the supplement can also interact with medications to produce serious adverse events.
“Patients may have a false sense of safety with so-called ‘natural’ treatments like St. John’s wort,” said study author Sarah Taylor, MD, of Wake Forest Baptist Medical Center in Winston-Salem, North Carolina.
“And it is crucial for physicians to know the dangers of ‘natural’ treatments and to communicate the risks to patients effectively.”
Dr Taylor and her colleagues investigated the use of St. John’s wort and reported their findings in The Journal of Alternative and Complementary Medicine.
To determine how often the supplement was being prescribed or taken with other medications, the researchers conducted a retrospective analysis of nationally representative data collected by the National Ambulatory Medical Care Survey from 1993 to 2010.
The team found the use of St. John’s wort in potentially harmful combinations in 28% of the cases reviewed. The drugs involved were warfarin, selective serotonin reuptake inhibitors, benzodiazepines, statins, verapamil, digoxin, and oral contraceptives.
Possible drug interactions include serotonin syndrome (a potentially fatal condition that causes high levels of the chemical serotonin to accumulate in the body), heart disease due to impaired efficacy of blood pressure medications, or unplanned pregnancy due to contraceptive failure, Dr Taylor said.
A key limitation of this study is that only medications recorded by the physician were analyzed. And Dr Taylor said the rate of St. John’s wort interactions may actually be underestimated because the database did not include patients who were using St. John’s wort but did not tell their doctor.
“Labeling requirements for helpful supplements such as St. John’s wort need to provide appropriate cautions and risk information,” Dr Taylor said, adding that France has banned the use of St. John’s wort products, and several other countries, including Japan, the UK, and Canada, are in the process of including drug-herb interaction warnings on St. John’s wort products.
“Doctors also need to be trained to always ask if the patient is taking any supplements, vitamins, minerals or herbs, especially before prescribing any of the common drugs that might interact with St. John’s wort.”

Credit: CDC
A new study indicates that a fair share of patients may be mixing the herbal supplement St. John’s wort with prescribed medications, which can have dangerous results.
St. John’s wort can reduce the concentration of numerous drugs in the body, including anticoagulants and chemotherapeutic agents. And this can result in impaired effectiveness and treatment failure.
But the supplement can also interact with medications to produce serious adverse events.
“Patients may have a false sense of safety with so-called ‘natural’ treatments like St. John’s wort,” said study author Sarah Taylor, MD, of Wake Forest Baptist Medical Center in Winston-Salem, North Carolina.
“And it is crucial for physicians to know the dangers of ‘natural’ treatments and to communicate the risks to patients effectively.”
Dr Taylor and her colleagues investigated the use of St. John’s wort and reported their findings in The Journal of Alternative and Complementary Medicine.
To determine how often the supplement was being prescribed or taken with other medications, the researchers conducted a retrospective analysis of nationally representative data collected by the National Ambulatory Medical Care Survey from 1993 to 2010.
The team found the use of St. John’s wort in potentially harmful combinations in 28% of the cases reviewed. The drugs involved were warfarin, selective serotonin reuptake inhibitors, benzodiazepines, statins, verapamil, digoxin, and oral contraceptives.
Possible drug interactions include serotonin syndrome (a potentially fatal condition that causes high levels of the chemical serotonin to accumulate in the body), heart disease due to impaired efficacy of blood pressure medications, or unplanned pregnancy due to contraceptive failure, Dr Taylor said.
A key limitation of this study is that only medications recorded by the physician were analyzed. And Dr Taylor said the rate of St. John’s wort interactions may actually be underestimated because the database did not include patients who were using St. John’s wort but did not tell their doctor.
“Labeling requirements for helpful supplements such as St. John’s wort need to provide appropriate cautions and risk information,” Dr Taylor said, adding that France has banned the use of St. John’s wort products, and several other countries, including Japan, the UK, and Canada, are in the process of including drug-herb interaction warnings on St. John’s wort products.
“Doctors also need to be trained to always ask if the patient is taking any supplements, vitamins, minerals or herbs, especially before prescribing any of the common drugs that might interact with St. John’s wort.”

Credit: CDC
A new study indicates that a fair share of patients may be mixing the herbal supplement St. John’s wort with prescribed medications, which can have dangerous results.
St. John’s wort can reduce the concentration of numerous drugs in the body, including anticoagulants and chemotherapeutic agents. And this can result in impaired effectiveness and treatment failure.
But the supplement can also interact with medications to produce serious adverse events.
“Patients may have a false sense of safety with so-called ‘natural’ treatments like St. John’s wort,” said study author Sarah Taylor, MD, of Wake Forest Baptist Medical Center in Winston-Salem, North Carolina.
“And it is crucial for physicians to know the dangers of ‘natural’ treatments and to communicate the risks to patients effectively.”
Dr Taylor and her colleagues investigated the use of St. John’s wort and reported their findings in The Journal of Alternative and Complementary Medicine.
To determine how often the supplement was being prescribed or taken with other medications, the researchers conducted a retrospective analysis of nationally representative data collected by the National Ambulatory Medical Care Survey from 1993 to 2010.
The team found the use of St. John’s wort in potentially harmful combinations in 28% of the cases reviewed. The drugs involved were warfarin, selective serotonin reuptake inhibitors, benzodiazepines, statins, verapamil, digoxin, and oral contraceptives.
Possible drug interactions include serotonin syndrome (a potentially fatal condition that causes high levels of the chemical serotonin to accumulate in the body), heart disease due to impaired efficacy of blood pressure medications, or unplanned pregnancy due to contraceptive failure, Dr Taylor said.
A key limitation of this study is that only medications recorded by the physician were analyzed. And Dr Taylor said the rate of St. John’s wort interactions may actually be underestimated because the database did not include patients who were using St. John’s wort but did not tell their doctor.
“Labeling requirements for helpful supplements such as St. John’s wort need to provide appropriate cautions and risk information,” Dr Taylor said, adding that France has banned the use of St. John’s wort products, and several other countries, including Japan, the UK, and Canada, are in the process of including drug-herb interaction warnings on St. John’s wort products.
“Doctors also need to be trained to always ask if the patient is taking any supplements, vitamins, minerals or herbs, especially before prescribing any of the common drugs that might interact with St. John’s wort.”
Mosquitos can sniff out malaria-infected mice

Credit: James Gathany
Scientists have found evidence to suggest that malaria parasites change the body odor of their host to attract hungry mosquitos.
The team observed an increase in mosquito attraction to malaria-infected mice, compared to healthy controls.
And the infected mice exhibited elevations in certain components of their natural scent, which suggests the malaria parasite changes the characteristics of its host’s body odor to make the host more attractive to mosquitos.
These findings appear in Proceedings of the National Academy of Sciences.
The researchers found that mice infected with Plasmodium chabaudii were more attractive to Anopheles stephensi mosquitos than uninfected control mice. And the attraction corresponded to an overall elevation in scent emissions from the infected mice.
However, malaria infection did not appear to trigger the expression of unique scent components. Instead, it seems the malaria pathogens alter the levels of compounds already present in the scent of uninfected mice.
“There appears to be an overall elevation of several compounds that are attractive to mosquitos,” said study author Consuelo De Moraes, PhD, of the Swiss Federal Institute of Technology in Zürich (ETH Zürich).
“Since mosquitos probably don’t benefit from feeding on infected people, it may make sense for the pathogen to exaggerate existing odor cues that the insects are already using for host location,” added study author Mark Mescher, PhD, also of ETH Zürich.
What the researchers found most surprising is the fact that the malaria infection leaves its mark on body odor long-term. Even when infected mice no longer had symptoms, their body odor showed they were carriers of the pathogen.
However, not all stages of disease smelled the same. The team found the scent profile of the acutely ill differed from the profile in mice exhibiting later stages of malaria infection.
Although the findings from this study cannot be directly translated to human malaria, they suggest similar effects might be involved in the attraction of mosquitos to infected people. Drs Mescher and De Moraes are currently investigating this possibility through additional research involving human subjects in Africa.

Credit: James Gathany
Scientists have found evidence to suggest that malaria parasites change the body odor of their host to attract hungry mosquitos.
The team observed an increase in mosquito attraction to malaria-infected mice, compared to healthy controls.
And the infected mice exhibited elevations in certain components of their natural scent, which suggests the malaria parasite changes the characteristics of its host’s body odor to make the host more attractive to mosquitos.
These findings appear in Proceedings of the National Academy of Sciences.
The researchers found that mice infected with Plasmodium chabaudii were more attractive to Anopheles stephensi mosquitos than uninfected control mice. And the attraction corresponded to an overall elevation in scent emissions from the infected mice.
However, malaria infection did not appear to trigger the expression of unique scent components. Instead, it seems the malaria pathogens alter the levels of compounds already present in the scent of uninfected mice.
“There appears to be an overall elevation of several compounds that are attractive to mosquitos,” said study author Consuelo De Moraes, PhD, of the Swiss Federal Institute of Technology in Zürich (ETH Zürich).
“Since mosquitos probably don’t benefit from feeding on infected people, it may make sense for the pathogen to exaggerate existing odor cues that the insects are already using for host location,” added study author Mark Mescher, PhD, also of ETH Zürich.
What the researchers found most surprising is the fact that the malaria infection leaves its mark on body odor long-term. Even when infected mice no longer had symptoms, their body odor showed they were carriers of the pathogen.
However, not all stages of disease smelled the same. The team found the scent profile of the acutely ill differed from the profile in mice exhibiting later stages of malaria infection.
Although the findings from this study cannot be directly translated to human malaria, they suggest similar effects might be involved in the attraction of mosquitos to infected people. Drs Mescher and De Moraes are currently investigating this possibility through additional research involving human subjects in Africa.

Credit: James Gathany
Scientists have found evidence to suggest that malaria parasites change the body odor of their host to attract hungry mosquitos.
The team observed an increase in mosquito attraction to malaria-infected mice, compared to healthy controls.
And the infected mice exhibited elevations in certain components of their natural scent, which suggests the malaria parasite changes the characteristics of its host’s body odor to make the host more attractive to mosquitos.
These findings appear in Proceedings of the National Academy of Sciences.
The researchers found that mice infected with Plasmodium chabaudii were more attractive to Anopheles stephensi mosquitos than uninfected control mice. And the attraction corresponded to an overall elevation in scent emissions from the infected mice.
However, malaria infection did not appear to trigger the expression of unique scent components. Instead, it seems the malaria pathogens alter the levels of compounds already present in the scent of uninfected mice.
“There appears to be an overall elevation of several compounds that are attractive to mosquitos,” said study author Consuelo De Moraes, PhD, of the Swiss Federal Institute of Technology in Zürich (ETH Zürich).
“Since mosquitos probably don’t benefit from feeding on infected people, it may make sense for the pathogen to exaggerate existing odor cues that the insects are already using for host location,” added study author Mark Mescher, PhD, also of ETH Zürich.
What the researchers found most surprising is the fact that the malaria infection leaves its mark on body odor long-term. Even when infected mice no longer had symptoms, their body odor showed they were carriers of the pathogen.
However, not all stages of disease smelled the same. The team found the scent profile of the acutely ill differed from the profile in mice exhibiting later stages of malaria infection.
Although the findings from this study cannot be directly translated to human malaria, they suggest similar effects might be involved in the attraction of mosquitos to infected people. Drs Mescher and De Moraes are currently investigating this possibility through additional research involving human subjects in Africa.
Nature retracts STAP cell papers
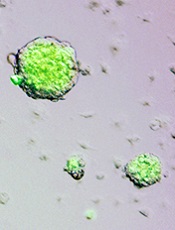
Credit: Haruko Obokata
The journal Nature has retracted the papers it published several months ago on stimulus-triggered acquisition of pluripotency (STAP) cells.
In January, Nature published an article and a letter in which researchers claimed they could create STAP cells—ie, induce pluripotency in somatic cells by exposing them to a low-pH environment.
Not long after the papers were published, however, members of the scientific community began to question the validity of the research.
They voiced concerns about published images, possible plagiarism, and an inability to replicate the experiments described.
So the Japanese institute RIKEN, where most of the study’s investigators are employed, launched an investigation.
In April, RIKEN’s investigative committee concluded that lead study author Haruko Obokata, PhD, and some of her colleagues were guilty of misconduct and/or negligence.
Dr Obokata appealed the findings, saying the acts of misconduct were simply mistakes and that STAP cells do exist.
But the committee decided another investigation is not warranted, and RIKEN called for a retraction of the Nature papers.
Today, Nature published the retractions, which can be viewed here and here. An editorial on the subject is available here.
As for the future of STAP cells, RIKEN is currently attempting to recreate Dr Obokata’s experiments and determine if the cells do exist. The organization plans to release an interim report on this attempt in late July or early August.
Other researchers said they have tried and failed to replicate Dr Obokata’s experiments. One group detailed their failed attempt in F1000Research.

Credit: Haruko Obokata
The journal Nature has retracted the papers it published several months ago on stimulus-triggered acquisition of pluripotency (STAP) cells.
In January, Nature published an article and a letter in which researchers claimed they could create STAP cells—ie, induce pluripotency in somatic cells by exposing them to a low-pH environment.
Not long after the papers were published, however, members of the scientific community began to question the validity of the research.
They voiced concerns about published images, possible plagiarism, and an inability to replicate the experiments described.
So the Japanese institute RIKEN, where most of the study’s investigators are employed, launched an investigation.
In April, RIKEN’s investigative committee concluded that lead study author Haruko Obokata, PhD, and some of her colleagues were guilty of misconduct and/or negligence.
Dr Obokata appealed the findings, saying the acts of misconduct were simply mistakes and that STAP cells do exist.
But the committee decided another investigation is not warranted, and RIKEN called for a retraction of the Nature papers.
Today, Nature published the retractions, which can be viewed here and here. An editorial on the subject is available here.
As for the future of STAP cells, RIKEN is currently attempting to recreate Dr Obokata’s experiments and determine if the cells do exist. The organization plans to release an interim report on this attempt in late July or early August.
Other researchers said they have tried and failed to replicate Dr Obokata’s experiments. One group detailed their failed attempt in F1000Research.

Credit: Haruko Obokata
The journal Nature has retracted the papers it published several months ago on stimulus-triggered acquisition of pluripotency (STAP) cells.
In January, Nature published an article and a letter in which researchers claimed they could create STAP cells—ie, induce pluripotency in somatic cells by exposing them to a low-pH environment.
Not long after the papers were published, however, members of the scientific community began to question the validity of the research.
They voiced concerns about published images, possible plagiarism, and an inability to replicate the experiments described.
So the Japanese institute RIKEN, where most of the study’s investigators are employed, launched an investigation.
In April, RIKEN’s investigative committee concluded that lead study author Haruko Obokata, PhD, and some of her colleagues were guilty of misconduct and/or negligence.
Dr Obokata appealed the findings, saying the acts of misconduct were simply mistakes and that STAP cells do exist.
But the committee decided another investigation is not warranted, and RIKEN called for a retraction of the Nature papers.
Today, Nature published the retractions, which can be viewed here and here. An editorial on the subject is available here.
As for the future of STAP cells, RIKEN is currently attempting to recreate Dr Obokata’s experiments and determine if the cells do exist. The organization plans to release an interim report on this attempt in late July or early August.
Other researchers said they have tried and failed to replicate Dr Obokata’s experiments. One group detailed their failed attempt in F1000Research.