User login
Functional Outcomes in Localized Prostate Cancer: Treatment Choice, Time, Prognosis All Matter
New research published Jan. 23 in JAMA parses functional outcome results from a population-based study of men diagnosed with localized prostate cancer. For their research, Bashir Al Hussein Al Awamlh, MD, of Vanderbilt University in Nashville, Tennessee, and his colleagues, looked at sexual function, urinary health, bowel function, hormonal function, and other outcomes in this cohort at 10 years’ follow-up.
Among 2455 patients for whom 10-year data were available, 1877 were deemed at baseline to have a favorable prognosis (defined as cT1-cT2bN0M0, prostate-specific antigen level less than 20 ng/mL, and grade group 1-2) and 568 had unfavorable-prognosis prostate cancer (defined as cT2cN0M0, prostate-specific antigen level of 20-50 ng/mL, or grade group 3-5). Follow-up data were collected by questionnaire through February 1, 2022. The men in the study were all younger than 80 years, and three-quarters of them were White.
At 10 years, outcomes differed based on the amount of time that had passed since diagnosis (they found different results at 3 and 5 year follow up, for example) and which treatment a patient received.
Among men with favorable prognoses at diagnosis, 20% underwent active surveillance for at least 1 year, while 56% received radical prostatectomy, 19% had external beam radiotherapy (EBRT) without ADT, and 5% had brachytherapy. Nearly a third of men originally opting for surveillance went on to undergo a therapeutic intervention by 10 years.
Dr. Al Hussein Al Awamlh and his colleagues found that while 3- and 5-year follow-up studies in this cohort had shown declines in sexual function among men who underwent surgery compared with those who had radiation or active surveillance, by 10 years those differences had faded, with no clinically meaningful differences in sexual function scores between the surgery and surveillance groups. In an interview, Dr. Al Hussein Al Awamlh said that this finding likely reflected mainly age-related declines in function across the study population — though it could also reflect declines after converting from surveillance to surgery or gradual decline with radiation treatment, he acknowledged.
Men with favorable prognoses at baseline who underwent surgery saw significantly worse urinary incontinence at 10 years compared with those started on radiotherapy or active surveillance. And EBRT was associated with fewer incontinence issues compared with active surveillance.
Among the group of men with an unfavorable prognosis at baseline, 64% of whom underwent radical prostatectomy and 36% EBRT with ADT, surgery was associated with worse urinary incontinence but not worse sexual function throughout 10 years of follow up, compared to radiotherapy with androgen deprivation therapy.
Radiation-treated patients with unfavorable prognoses, meanwhile, saw significantly worse bowel function and hormone function at 10 years compared with patients who had undergone surgery.
Dr. Al Hussein Al Awamlh said that a strength of this study was that “we had enough patients to stratify functional outcomes based on disease prognosis.” Another key finding was that some of the outcomes changed over time. “For example, among the patients with unfavorable prognoses, at 10-year follow-up there was slightly worse bowel and hormone function seen associated with radiation with ADT compared with surgery,” he said — something not seen at earlier follow-up points.
The findings may help offer a more nuanced way to counsel patients, Dr. Al Hussein Al Awamlh noted. For example, the side effects associated with sexual function “are not as relevant for those with unfavorable disease,” he said.
While current prostate cancer guidelines do address quality of life in shared decision-making, he said, “hopefully this data may provide more insight on that.” For patients with favorable prognosis, the findings reinforce that “active surveillance is a great option because it avoids the effects associated with those other treatments.”
Ultimately, Dr. Al Hussein Al Awamlh said, “this is a patient preference issue. It’s important for patients to understand how different functions are affected and to decide what is better for them — what they can live with and what they cannot, provided all the options are oncologically safe.”
The study authors disclosed as limitations of their study its observational design, the potential for response bias among study participants, and small numbers for some of the measured outcomes.
In an interview, urologist Mark S. Litwin, MD, of the University of California Los Angeles, characterized the study as “a well-conducted very-long-term longitudinal cohort that tracked men long past the initial diagnosis and treatment. That empowered the Vanderbilt team to find differences in quality of life many years later and compare them to other older men who had not received treatment.”
The new findings, Dr. Litwin said, “are critical in showing that most men with prostate cancer do not die from it; hence, the quality-of-life effects end up being the key issues for decision-making.”
Dr. Al Hussein Al Awamlh and colleagues’ study was funded by grants from the National Institutes of Health, the Agency for Healthcare Research and Quality, and the Patient-Centered Outcomes Research Institute. Several coauthors disclosed funding from pharmaceutical and/or device manufacturers. Dr. Litwin disclosed no conflicts of interest related to his comment.
New research published Jan. 23 in JAMA parses functional outcome results from a population-based study of men diagnosed with localized prostate cancer. For their research, Bashir Al Hussein Al Awamlh, MD, of Vanderbilt University in Nashville, Tennessee, and his colleagues, looked at sexual function, urinary health, bowel function, hormonal function, and other outcomes in this cohort at 10 years’ follow-up.
Among 2455 patients for whom 10-year data were available, 1877 were deemed at baseline to have a favorable prognosis (defined as cT1-cT2bN0M0, prostate-specific antigen level less than 20 ng/mL, and grade group 1-2) and 568 had unfavorable-prognosis prostate cancer (defined as cT2cN0M0, prostate-specific antigen level of 20-50 ng/mL, or grade group 3-5). Follow-up data were collected by questionnaire through February 1, 2022. The men in the study were all younger than 80 years, and three-quarters of them were White.
At 10 years, outcomes differed based on the amount of time that had passed since diagnosis (they found different results at 3 and 5 year follow up, for example) and which treatment a patient received.
Among men with favorable prognoses at diagnosis, 20% underwent active surveillance for at least 1 year, while 56% received radical prostatectomy, 19% had external beam radiotherapy (EBRT) without ADT, and 5% had brachytherapy. Nearly a third of men originally opting for surveillance went on to undergo a therapeutic intervention by 10 years.
Dr. Al Hussein Al Awamlh and his colleagues found that while 3- and 5-year follow-up studies in this cohort had shown declines in sexual function among men who underwent surgery compared with those who had radiation or active surveillance, by 10 years those differences had faded, with no clinically meaningful differences in sexual function scores between the surgery and surveillance groups. In an interview, Dr. Al Hussein Al Awamlh said that this finding likely reflected mainly age-related declines in function across the study population — though it could also reflect declines after converting from surveillance to surgery or gradual decline with radiation treatment, he acknowledged.
Men with favorable prognoses at baseline who underwent surgery saw significantly worse urinary incontinence at 10 years compared with those started on radiotherapy or active surveillance. And EBRT was associated with fewer incontinence issues compared with active surveillance.
Among the group of men with an unfavorable prognosis at baseline, 64% of whom underwent radical prostatectomy and 36% EBRT with ADT, surgery was associated with worse urinary incontinence but not worse sexual function throughout 10 years of follow up, compared to radiotherapy with androgen deprivation therapy.
Radiation-treated patients with unfavorable prognoses, meanwhile, saw significantly worse bowel function and hormone function at 10 years compared with patients who had undergone surgery.
Dr. Al Hussein Al Awamlh said that a strength of this study was that “we had enough patients to stratify functional outcomes based on disease prognosis.” Another key finding was that some of the outcomes changed over time. “For example, among the patients with unfavorable prognoses, at 10-year follow-up there was slightly worse bowel and hormone function seen associated with radiation with ADT compared with surgery,” he said — something not seen at earlier follow-up points.
The findings may help offer a more nuanced way to counsel patients, Dr. Al Hussein Al Awamlh noted. For example, the side effects associated with sexual function “are not as relevant for those with unfavorable disease,” he said.
While current prostate cancer guidelines do address quality of life in shared decision-making, he said, “hopefully this data may provide more insight on that.” For patients with favorable prognosis, the findings reinforce that “active surveillance is a great option because it avoids the effects associated with those other treatments.”
Ultimately, Dr. Al Hussein Al Awamlh said, “this is a patient preference issue. It’s important for patients to understand how different functions are affected and to decide what is better for them — what they can live with and what they cannot, provided all the options are oncologically safe.”
The study authors disclosed as limitations of their study its observational design, the potential for response bias among study participants, and small numbers for some of the measured outcomes.
In an interview, urologist Mark S. Litwin, MD, of the University of California Los Angeles, characterized the study as “a well-conducted very-long-term longitudinal cohort that tracked men long past the initial diagnosis and treatment. That empowered the Vanderbilt team to find differences in quality of life many years later and compare them to other older men who had not received treatment.”
The new findings, Dr. Litwin said, “are critical in showing that most men with prostate cancer do not die from it; hence, the quality-of-life effects end up being the key issues for decision-making.”
Dr. Al Hussein Al Awamlh and colleagues’ study was funded by grants from the National Institutes of Health, the Agency for Healthcare Research and Quality, and the Patient-Centered Outcomes Research Institute. Several coauthors disclosed funding from pharmaceutical and/or device manufacturers. Dr. Litwin disclosed no conflicts of interest related to his comment.
New research published Jan. 23 in JAMA parses functional outcome results from a population-based study of men diagnosed with localized prostate cancer. For their research, Bashir Al Hussein Al Awamlh, MD, of Vanderbilt University in Nashville, Tennessee, and his colleagues, looked at sexual function, urinary health, bowel function, hormonal function, and other outcomes in this cohort at 10 years’ follow-up.
Among 2455 patients for whom 10-year data were available, 1877 were deemed at baseline to have a favorable prognosis (defined as cT1-cT2bN0M0, prostate-specific antigen level less than 20 ng/mL, and grade group 1-2) and 568 had unfavorable-prognosis prostate cancer (defined as cT2cN0M0, prostate-specific antigen level of 20-50 ng/mL, or grade group 3-5). Follow-up data were collected by questionnaire through February 1, 2022. The men in the study were all younger than 80 years, and three-quarters of them were White.
At 10 years, outcomes differed based on the amount of time that had passed since diagnosis (they found different results at 3 and 5 year follow up, for example) and which treatment a patient received.
Among men with favorable prognoses at diagnosis, 20% underwent active surveillance for at least 1 year, while 56% received radical prostatectomy, 19% had external beam radiotherapy (EBRT) without ADT, and 5% had brachytherapy. Nearly a third of men originally opting for surveillance went on to undergo a therapeutic intervention by 10 years.
Dr. Al Hussein Al Awamlh and his colleagues found that while 3- and 5-year follow-up studies in this cohort had shown declines in sexual function among men who underwent surgery compared with those who had radiation or active surveillance, by 10 years those differences had faded, with no clinically meaningful differences in sexual function scores between the surgery and surveillance groups. In an interview, Dr. Al Hussein Al Awamlh said that this finding likely reflected mainly age-related declines in function across the study population — though it could also reflect declines after converting from surveillance to surgery or gradual decline with radiation treatment, he acknowledged.
Men with favorable prognoses at baseline who underwent surgery saw significantly worse urinary incontinence at 10 years compared with those started on radiotherapy or active surveillance. And EBRT was associated with fewer incontinence issues compared with active surveillance.
Among the group of men with an unfavorable prognosis at baseline, 64% of whom underwent radical prostatectomy and 36% EBRT with ADT, surgery was associated with worse urinary incontinence but not worse sexual function throughout 10 years of follow up, compared to radiotherapy with androgen deprivation therapy.
Radiation-treated patients with unfavorable prognoses, meanwhile, saw significantly worse bowel function and hormone function at 10 years compared with patients who had undergone surgery.
Dr. Al Hussein Al Awamlh said that a strength of this study was that “we had enough patients to stratify functional outcomes based on disease prognosis.” Another key finding was that some of the outcomes changed over time. “For example, among the patients with unfavorable prognoses, at 10-year follow-up there was slightly worse bowel and hormone function seen associated with radiation with ADT compared with surgery,” he said — something not seen at earlier follow-up points.
The findings may help offer a more nuanced way to counsel patients, Dr. Al Hussein Al Awamlh noted. For example, the side effects associated with sexual function “are not as relevant for those with unfavorable disease,” he said.
While current prostate cancer guidelines do address quality of life in shared decision-making, he said, “hopefully this data may provide more insight on that.” For patients with favorable prognosis, the findings reinforce that “active surveillance is a great option because it avoids the effects associated with those other treatments.”
Ultimately, Dr. Al Hussein Al Awamlh said, “this is a patient preference issue. It’s important for patients to understand how different functions are affected and to decide what is better for them — what they can live with and what they cannot, provided all the options are oncologically safe.”
The study authors disclosed as limitations of their study its observational design, the potential for response bias among study participants, and small numbers for some of the measured outcomes.
In an interview, urologist Mark S. Litwin, MD, of the University of California Los Angeles, characterized the study as “a well-conducted very-long-term longitudinal cohort that tracked men long past the initial diagnosis and treatment. That empowered the Vanderbilt team to find differences in quality of life many years later and compare them to other older men who had not received treatment.”
The new findings, Dr. Litwin said, “are critical in showing that most men with prostate cancer do not die from it; hence, the quality-of-life effects end up being the key issues for decision-making.”
Dr. Al Hussein Al Awamlh and colleagues’ study was funded by grants from the National Institutes of Health, the Agency for Healthcare Research and Quality, and the Patient-Centered Outcomes Research Institute. Several coauthors disclosed funding from pharmaceutical and/or device manufacturers. Dr. Litwin disclosed no conflicts of interest related to his comment.
FROM JAMA
Analysis of Nail Excision Practice Patterns in the Medicare Provider Utilization and Payment Database 2012-2017
To the Editor:
Partial or total nail plate excisions commonly are used for the treatment of onychocryptosis and nail spicules. Procedures involving the nail unit require advanced technical skills to achieve optimal functional and aesthetic outcomes, avoid complications, and minimize health care costs. Data on the frequency of nail plate excisions performed by dermatologists and their relative frequency compared to other medical providers are limited. The objective of our study was to analyze trends in nail excision practice patterns among medical providers in the United States.
A retrospective analysis on nail excisions using the Current Procedural Terminology (CPT) code 11750 (excision of nail and nail matrix, partial or complete [eg, ingrown or deformed nail] for permanent removal), which is distinct from code 11755 (biopsy of nail unit [eg, plate, bed, matrix, hyponychium, proximal and lateral nail folds][separate procedure]), was performed using data from the Medicare Provider Utilization and Payment Database 2012-2017.1,2 This file also is used by Peck et al3 in an article submitted to the Journal of the American Podiatric Medical Association and currently under consideration for publication. Procedures were recorded by year and provider type—dermatologist, podiatrist, physician assistant (PA)/nurse practitioner (NP), nondermatologist physician—and subcategorized by provider specialty (Table). Practice locations subcategorized by provider type were mapped using Tableau Software (Salesforce)(Figure). Descriptive statistics including number of providers, mean and median excisions per provider, and minimum/maximum nail excisions were calculated (Table). Practice types of PAs/NPs and specialization of nondermatologist physicians were determined using provider name, identification number, and practice address. This study did not require institutional review board review, as only publicly available data were utilized in our analysis.
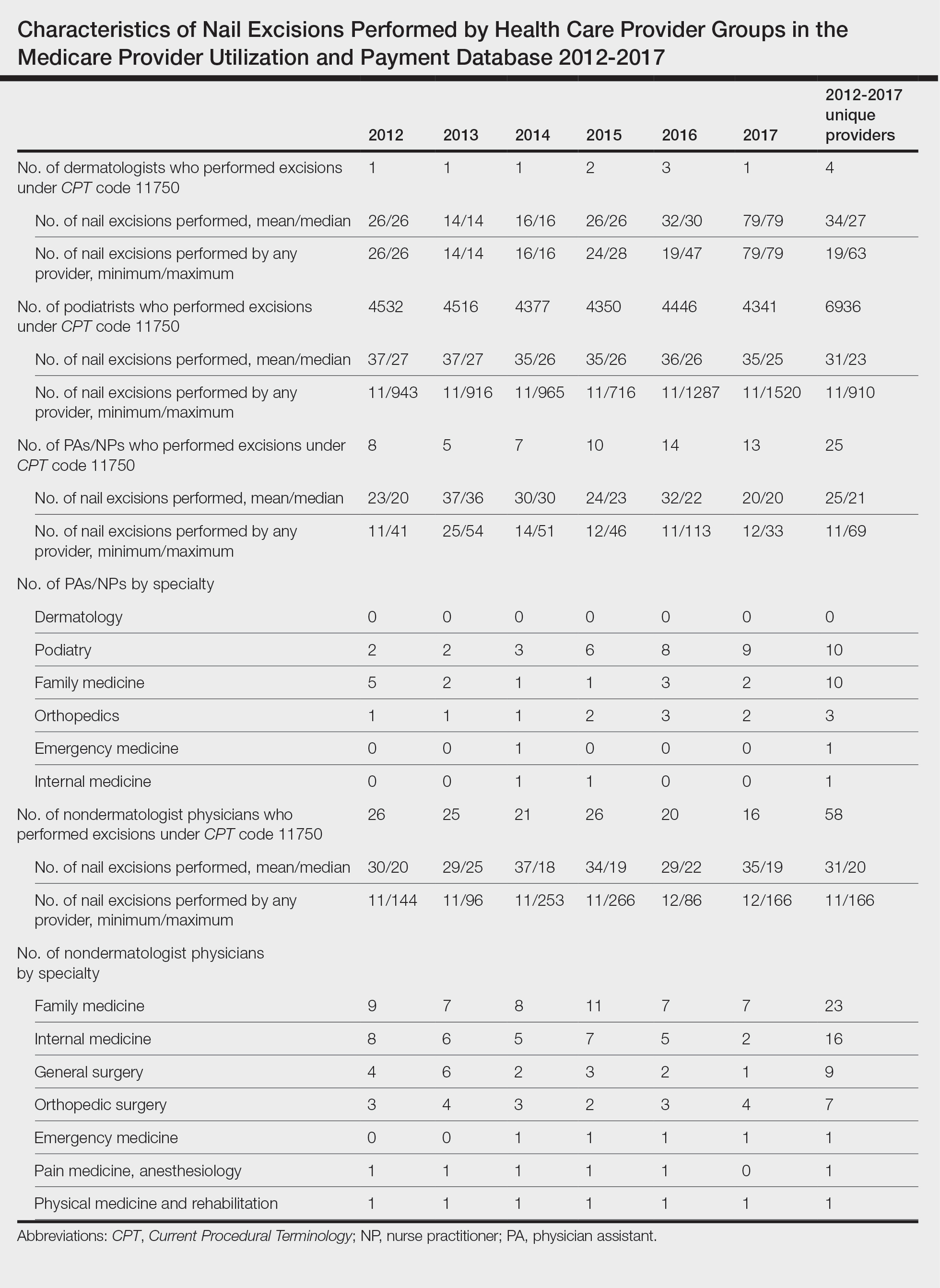
A total of 6936 podiatrists, 58 nondermatologist physicians, 25 PAs/NPs, and 4 dermatologists performed 10 or more nail excisions annually under CPT code 11750 from January 2012 to December 2017 with annual means of 31, 31, 25, and 34, respectively (Table). No PAs/NPs included in the dataset worked in dermatology practices during the study period. Physician assistants and NPs most often practiced in podiatry and family medicine (FM) settings (both 40% [10/25]). Nondermatologist physicians most often specialized in FM (40% [23/58])(Table). The greatest number of providers practiced in 3 of the 4 most-populous states: California, Texas, and Florida; the fewest number practiced in 3 of the 10 least-populous states: Alaska, Hawaii, and Vermont. Vermont, Wyoming, and North Dakota—3 of the 5 least-populous states—had the fewest practitioners among the contiguous United States (Figure).
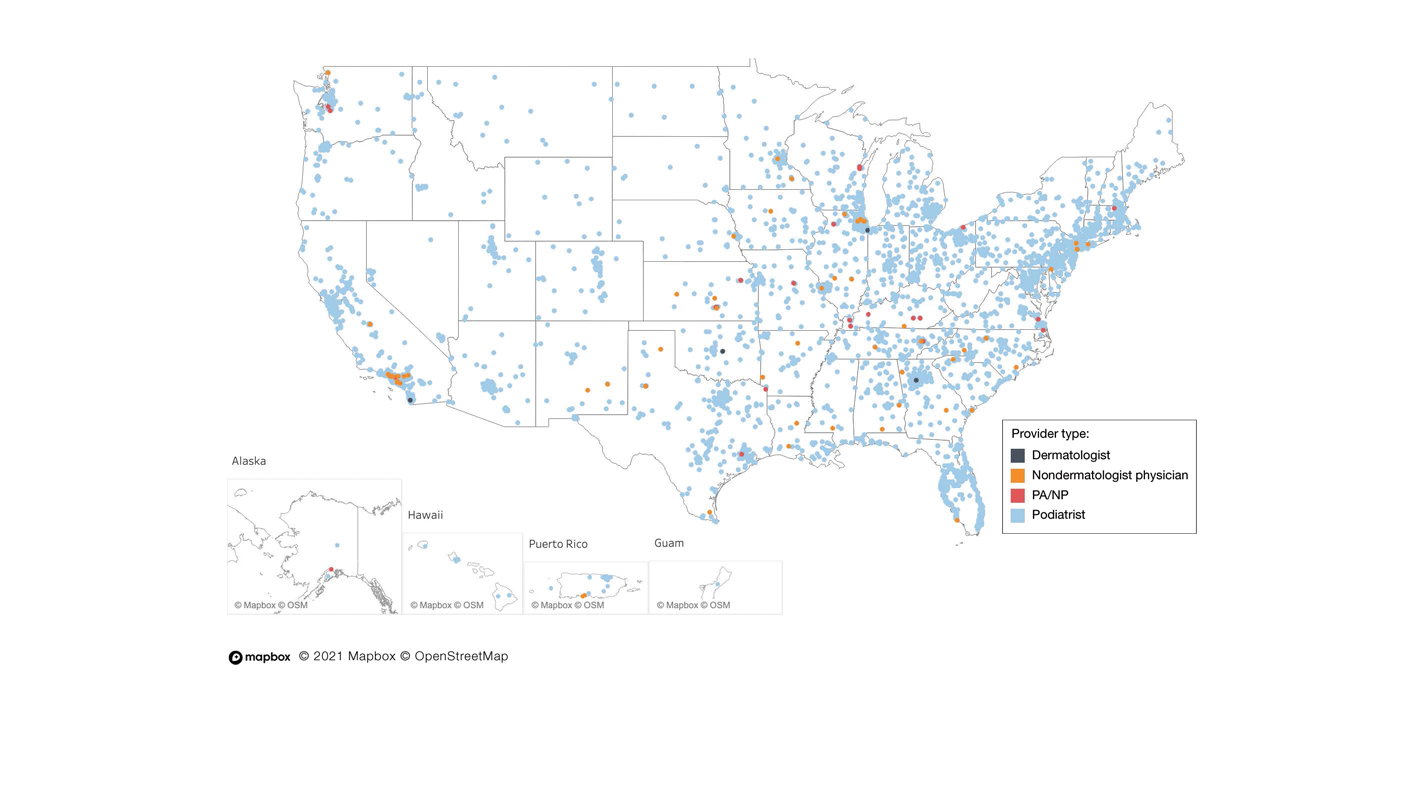
Our study showed that from January 2012 to December 2017, fewer dermatologists performed nail excisions than any other provider type (0.06%, 4 dermatologists of 7023 total providers), and dermatologists performed 1734-fold fewer nail excisions than podiatrists (99%, 6936 podiatrists of 7023 total providers). Only dermatologists practicing in California, Georgia, Indiana, and Oklahoma performed nail excisions. Conversely, podiatrists were more geographically distributed across the United States and other territories, with representation in all 50 states as well as the District of Columbia, Puerto Rico, and Guam.
Reasons for these large discrepancies in practice between dermatologists and other providers likely are multifactorial, encompassing a lack of emphasis on nail procedures in dermatology training, patient perception of the scope of dermatologic practice, and nail excision reimbursement patterns. Most dermatologists likely lack experience in performing nail procedures. The Accreditation Council for Graduate Medical Education requirements mandate that dermatology residents observe or perform 3 nail procedures over 3 years of residency, including 1 that may be performed on a human cadaver.4 In contrast, podiatry trainees must gain competency in toenail avulsion (both partial and complete), participate in anesthesia workshops, and become proficient in administering lower extremity blocks by the end of their training.5 Therefore, incorporating aspects of podiatric surgical training into dermatology residency requirements may increase the competency and comfort of dermatologists in performing nail excisions and practicing as nail experts as attending physicians.
It is likely that US patients do not perceive dermatologists as nail specialists and instead primarily consult podiatrists or FM and/or internal medicine physicians for treatment; for example, nail disease was one of the least common reasons for consulting a dermatologist (5%) in a German nationwide survey-based study (N=1015).6 Therefore, increased efforts are needed to educate the general public about the expertise of dermatologists in the diagnosis and management of nail conditions.
Reimbursement also may be a barrier to dermatologists performing nail procedures as part of their scope of practice; for example, in a retrospective study of nail biopsies using the Medicare Provider Utilization and Payment Database, there was no statistically significant difference in reimbursements for nail biopsies vs skin biopsies from 2012 to 2017 (P=0.69).7 Similar to nail biopsies, nail excisions typically are much more time consuming and technically demanding than skin biopsies, which may discourage dermatologists from routinely performing nail excision procedures.
Our study is subject to a number of limitations. The data reflected only US-based practice patterns and may not be applicable to nail procedures globally. There also is the potential for miscoding of procedures in the Medicare database. The data included only Part B Medicare fee-for-service and excludes non-Medicare insured, uninsured, and self-pay patients, as well as aggregated records from 10 or fewer Medicare beneficiaries.
Dermatologists rarely perform nail excisions and perform fewer nail excisions than any other provider type in the United States. There currently is an unmet need for comprehensive nail surgery education in US-based dermatology residency programs. We hope that our study fosters interdisciplinary collegiality and training between podiatrists and dermatologists and promotes expanded access to care across the United States to serve patients with nail disorders.
- Centers for Medicare & Medicaid Services. Medicare Fee-For-Service Provider Utilization & Payment Data Physician and Other Supplier Public Use File: A Methodological Overview . Updated September 22, 2020. Accessed January 5, 2024. https://www.cms.gov/research-statistics-data-and-systems/statistics-trends-and-reports/medicare-provider-charge-data/downloads/medicare-physician-and-other-supplier-puf-methodology.pdf
- Centers for Medicare and Medicaid Services. Billing and Coding: Surgical Treatment of Nails. Updated November 9, 2023. Accessed January 8, 2024. https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleID=52998#:~:text=The%20description%20of%20CPT%20codes,date%20of%20service%20(DOS).
- Peck GM, Vlahovic TC, Hill R, et al. Senior podiatrists in solo practice are high performers of nail excisions. JAPMA. In press.
- Accreditation Council for Graduate Medical Education. Case log minimums. review committee for dermatology. Published May 2019. Accessed January 5, 2024. https://www.acgme.org/Portals/0/PFAssets/ProgramResources/CaseLogMinimums.pdf?ver=2018-04-03-102751-650
- Council on Podiatric Medical Education. Standards and Requirements for Approval of Podiatric Medicine and Surgery Residencies. Published July 2023. Accessed January 17, 2024. https://www.cpme.org/files/320%20Council%20Approved%20October%202022%20-%20April%202023%20edits.pdf
- Augustin M, Eissing L, Elsner P, et al. Perception and image of dermatology in the German general population 2002-2014. J Eur Acad Dermatol Venereol. 2017;31:2124-2130.
- Wang Y, Lipner SR. Retrospective analysis of nail biopsies performed using the Medicare provider utilization and payment database 2012 to 2017. Dermatol Ther. 2021;34:E14928.
To the Editor:
Partial or total nail plate excisions commonly are used for the treatment of onychocryptosis and nail spicules. Procedures involving the nail unit require advanced technical skills to achieve optimal functional and aesthetic outcomes, avoid complications, and minimize health care costs. Data on the frequency of nail plate excisions performed by dermatologists and their relative frequency compared to other medical providers are limited. The objective of our study was to analyze trends in nail excision practice patterns among medical providers in the United States.
A retrospective analysis on nail excisions using the Current Procedural Terminology (CPT) code 11750 (excision of nail and nail matrix, partial or complete [eg, ingrown or deformed nail] for permanent removal), which is distinct from code 11755 (biopsy of nail unit [eg, plate, bed, matrix, hyponychium, proximal and lateral nail folds][separate procedure]), was performed using data from the Medicare Provider Utilization and Payment Database 2012-2017.1,2 This file also is used by Peck et al3 in an article submitted to the Journal of the American Podiatric Medical Association and currently under consideration for publication. Procedures were recorded by year and provider type—dermatologist, podiatrist, physician assistant (PA)/nurse practitioner (NP), nondermatologist physician—and subcategorized by provider specialty (Table). Practice locations subcategorized by provider type were mapped using Tableau Software (Salesforce)(Figure). Descriptive statistics including number of providers, mean and median excisions per provider, and minimum/maximum nail excisions were calculated (Table). Practice types of PAs/NPs and specialization of nondermatologist physicians were determined using provider name, identification number, and practice address. This study did not require institutional review board review, as only publicly available data were utilized in our analysis.

A total of 6936 podiatrists, 58 nondermatologist physicians, 25 PAs/NPs, and 4 dermatologists performed 10 or more nail excisions annually under CPT code 11750 from January 2012 to December 2017 with annual means of 31, 31, 25, and 34, respectively (Table). No PAs/NPs included in the dataset worked in dermatology practices during the study period. Physician assistants and NPs most often practiced in podiatry and family medicine (FM) settings (both 40% [10/25]). Nondermatologist physicians most often specialized in FM (40% [23/58])(Table). The greatest number of providers practiced in 3 of the 4 most-populous states: California, Texas, and Florida; the fewest number practiced in 3 of the 10 least-populous states: Alaska, Hawaii, and Vermont. Vermont, Wyoming, and North Dakota—3 of the 5 least-populous states—had the fewest practitioners among the contiguous United States (Figure).

Our study showed that from January 2012 to December 2017, fewer dermatologists performed nail excisions than any other provider type (0.06%, 4 dermatologists of 7023 total providers), and dermatologists performed 1734-fold fewer nail excisions than podiatrists (99%, 6936 podiatrists of 7023 total providers). Only dermatologists practicing in California, Georgia, Indiana, and Oklahoma performed nail excisions. Conversely, podiatrists were more geographically distributed across the United States and other territories, with representation in all 50 states as well as the District of Columbia, Puerto Rico, and Guam.
Reasons for these large discrepancies in practice between dermatologists and other providers likely are multifactorial, encompassing a lack of emphasis on nail procedures in dermatology training, patient perception of the scope of dermatologic practice, and nail excision reimbursement patterns. Most dermatologists likely lack experience in performing nail procedures. The Accreditation Council for Graduate Medical Education requirements mandate that dermatology residents observe or perform 3 nail procedures over 3 years of residency, including 1 that may be performed on a human cadaver.4 In contrast, podiatry trainees must gain competency in toenail avulsion (both partial and complete), participate in anesthesia workshops, and become proficient in administering lower extremity blocks by the end of their training.5 Therefore, incorporating aspects of podiatric surgical training into dermatology residency requirements may increase the competency and comfort of dermatologists in performing nail excisions and practicing as nail experts as attending physicians.
It is likely that US patients do not perceive dermatologists as nail specialists and instead primarily consult podiatrists or FM and/or internal medicine physicians for treatment; for example, nail disease was one of the least common reasons for consulting a dermatologist (5%) in a German nationwide survey-based study (N=1015).6 Therefore, increased efforts are needed to educate the general public about the expertise of dermatologists in the diagnosis and management of nail conditions.
Reimbursement also may be a barrier to dermatologists performing nail procedures as part of their scope of practice; for example, in a retrospective study of nail biopsies using the Medicare Provider Utilization and Payment Database, there was no statistically significant difference in reimbursements for nail biopsies vs skin biopsies from 2012 to 2017 (P=0.69).7 Similar to nail biopsies, nail excisions typically are much more time consuming and technically demanding than skin biopsies, which may discourage dermatologists from routinely performing nail excision procedures.
Our study is subject to a number of limitations. The data reflected only US-based practice patterns and may not be applicable to nail procedures globally. There also is the potential for miscoding of procedures in the Medicare database. The data included only Part B Medicare fee-for-service and excludes non-Medicare insured, uninsured, and self-pay patients, as well as aggregated records from 10 or fewer Medicare beneficiaries.
Dermatologists rarely perform nail excisions and perform fewer nail excisions than any other provider type in the United States. There currently is an unmet need for comprehensive nail surgery education in US-based dermatology residency programs. We hope that our study fosters interdisciplinary collegiality and training between podiatrists and dermatologists and promotes expanded access to care across the United States to serve patients with nail disorders.
To the Editor:
Partial or total nail plate excisions commonly are used for the treatment of onychocryptosis and nail spicules. Procedures involving the nail unit require advanced technical skills to achieve optimal functional and aesthetic outcomes, avoid complications, and minimize health care costs. Data on the frequency of nail plate excisions performed by dermatologists and their relative frequency compared to other medical providers are limited. The objective of our study was to analyze trends in nail excision practice patterns among medical providers in the United States.
A retrospective analysis on nail excisions using the Current Procedural Terminology (CPT) code 11750 (excision of nail and nail matrix, partial or complete [eg, ingrown or deformed nail] for permanent removal), which is distinct from code 11755 (biopsy of nail unit [eg, plate, bed, matrix, hyponychium, proximal and lateral nail folds][separate procedure]), was performed using data from the Medicare Provider Utilization and Payment Database 2012-2017.1,2 This file also is used by Peck et al3 in an article submitted to the Journal of the American Podiatric Medical Association and currently under consideration for publication. Procedures were recorded by year and provider type—dermatologist, podiatrist, physician assistant (PA)/nurse practitioner (NP), nondermatologist physician—and subcategorized by provider specialty (Table). Practice locations subcategorized by provider type were mapped using Tableau Software (Salesforce)(Figure). Descriptive statistics including number of providers, mean and median excisions per provider, and minimum/maximum nail excisions were calculated (Table). Practice types of PAs/NPs and specialization of nondermatologist physicians were determined using provider name, identification number, and practice address. This study did not require institutional review board review, as only publicly available data were utilized in our analysis.

A total of 6936 podiatrists, 58 nondermatologist physicians, 25 PAs/NPs, and 4 dermatologists performed 10 or more nail excisions annually under CPT code 11750 from January 2012 to December 2017 with annual means of 31, 31, 25, and 34, respectively (Table). No PAs/NPs included in the dataset worked in dermatology practices during the study period. Physician assistants and NPs most often practiced in podiatry and family medicine (FM) settings (both 40% [10/25]). Nondermatologist physicians most often specialized in FM (40% [23/58])(Table). The greatest number of providers practiced in 3 of the 4 most-populous states: California, Texas, and Florida; the fewest number practiced in 3 of the 10 least-populous states: Alaska, Hawaii, and Vermont. Vermont, Wyoming, and North Dakota—3 of the 5 least-populous states—had the fewest practitioners among the contiguous United States (Figure).

Our study showed that from January 2012 to December 2017, fewer dermatologists performed nail excisions than any other provider type (0.06%, 4 dermatologists of 7023 total providers), and dermatologists performed 1734-fold fewer nail excisions than podiatrists (99%, 6936 podiatrists of 7023 total providers). Only dermatologists practicing in California, Georgia, Indiana, and Oklahoma performed nail excisions. Conversely, podiatrists were more geographically distributed across the United States and other territories, with representation in all 50 states as well as the District of Columbia, Puerto Rico, and Guam.
Reasons for these large discrepancies in practice between dermatologists and other providers likely are multifactorial, encompassing a lack of emphasis on nail procedures in dermatology training, patient perception of the scope of dermatologic practice, and nail excision reimbursement patterns. Most dermatologists likely lack experience in performing nail procedures. The Accreditation Council for Graduate Medical Education requirements mandate that dermatology residents observe or perform 3 nail procedures over 3 years of residency, including 1 that may be performed on a human cadaver.4 In contrast, podiatry trainees must gain competency in toenail avulsion (both partial and complete), participate in anesthesia workshops, and become proficient in administering lower extremity blocks by the end of their training.5 Therefore, incorporating aspects of podiatric surgical training into dermatology residency requirements may increase the competency and comfort of dermatologists in performing nail excisions and practicing as nail experts as attending physicians.
It is likely that US patients do not perceive dermatologists as nail specialists and instead primarily consult podiatrists or FM and/or internal medicine physicians for treatment; for example, nail disease was one of the least common reasons for consulting a dermatologist (5%) in a German nationwide survey-based study (N=1015).6 Therefore, increased efforts are needed to educate the general public about the expertise of dermatologists in the diagnosis and management of nail conditions.
Reimbursement also may be a barrier to dermatologists performing nail procedures as part of their scope of practice; for example, in a retrospective study of nail biopsies using the Medicare Provider Utilization and Payment Database, there was no statistically significant difference in reimbursements for nail biopsies vs skin biopsies from 2012 to 2017 (P=0.69).7 Similar to nail biopsies, nail excisions typically are much more time consuming and technically demanding than skin biopsies, which may discourage dermatologists from routinely performing nail excision procedures.
Our study is subject to a number of limitations. The data reflected only US-based practice patterns and may not be applicable to nail procedures globally. There also is the potential for miscoding of procedures in the Medicare database. The data included only Part B Medicare fee-for-service and excludes non-Medicare insured, uninsured, and self-pay patients, as well as aggregated records from 10 or fewer Medicare beneficiaries.
Dermatologists rarely perform nail excisions and perform fewer nail excisions than any other provider type in the United States. There currently is an unmet need for comprehensive nail surgery education in US-based dermatology residency programs. We hope that our study fosters interdisciplinary collegiality and training between podiatrists and dermatologists and promotes expanded access to care across the United States to serve patients with nail disorders.
- Centers for Medicare & Medicaid Services. Medicare Fee-For-Service Provider Utilization & Payment Data Physician and Other Supplier Public Use File: A Methodological Overview . Updated September 22, 2020. Accessed January 5, 2024. https://www.cms.gov/research-statistics-data-and-systems/statistics-trends-and-reports/medicare-provider-charge-data/downloads/medicare-physician-and-other-supplier-puf-methodology.pdf
- Centers for Medicare and Medicaid Services. Billing and Coding: Surgical Treatment of Nails. Updated November 9, 2023. Accessed January 8, 2024. https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleID=52998#:~:text=The%20description%20of%20CPT%20codes,date%20of%20service%20(DOS).
- Peck GM, Vlahovic TC, Hill R, et al. Senior podiatrists in solo practice are high performers of nail excisions. JAPMA. In press.
- Accreditation Council for Graduate Medical Education. Case log minimums. review committee for dermatology. Published May 2019. Accessed January 5, 2024. https://www.acgme.org/Portals/0/PFAssets/ProgramResources/CaseLogMinimums.pdf?ver=2018-04-03-102751-650
- Council on Podiatric Medical Education. Standards and Requirements for Approval of Podiatric Medicine and Surgery Residencies. Published July 2023. Accessed January 17, 2024. https://www.cpme.org/files/320%20Council%20Approved%20October%202022%20-%20April%202023%20edits.pdf
- Augustin M, Eissing L, Elsner P, et al. Perception and image of dermatology in the German general population 2002-2014. J Eur Acad Dermatol Venereol. 2017;31:2124-2130.
- Wang Y, Lipner SR. Retrospective analysis of nail biopsies performed using the Medicare provider utilization and payment database 2012 to 2017. Dermatol Ther. 2021;34:E14928.
- Centers for Medicare & Medicaid Services. Medicare Fee-For-Service Provider Utilization & Payment Data Physician and Other Supplier Public Use File: A Methodological Overview . Updated September 22, 2020. Accessed January 5, 2024. https://www.cms.gov/research-statistics-data-and-systems/statistics-trends-and-reports/medicare-provider-charge-data/downloads/medicare-physician-and-other-supplier-puf-methodology.pdf
- Centers for Medicare and Medicaid Services. Billing and Coding: Surgical Treatment of Nails. Updated November 9, 2023. Accessed January 8, 2024. https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleID=52998#:~:text=The%20description%20of%20CPT%20codes,date%20of%20service%20(DOS).
- Peck GM, Vlahovic TC, Hill R, et al. Senior podiatrists in solo practice are high performers of nail excisions. JAPMA. In press.
- Accreditation Council for Graduate Medical Education. Case log minimums. review committee for dermatology. Published May 2019. Accessed January 5, 2024. https://www.acgme.org/Portals/0/PFAssets/ProgramResources/CaseLogMinimums.pdf?ver=2018-04-03-102751-650
- Council on Podiatric Medical Education. Standards and Requirements for Approval of Podiatric Medicine and Surgery Residencies. Published July 2023. Accessed January 17, 2024. https://www.cpme.org/files/320%20Council%20Approved%20October%202022%20-%20April%202023%20edits.pdf
- Augustin M, Eissing L, Elsner P, et al. Perception and image of dermatology in the German general population 2002-2014. J Eur Acad Dermatol Venereol. 2017;31:2124-2130.
- Wang Y, Lipner SR. Retrospective analysis of nail biopsies performed using the Medicare provider utilization and payment database 2012 to 2017. Dermatol Ther. 2021;34:E14928.
Practice Points
- Dermatologists are considered nail experts but perform nail excisions less frequently than their podiatric counterparts and physicians in other specialties.
- Aspects of podiatric surgical training should be incorporated into dermatology residency to increase competency and comfort of dermatologists in nail excision procedures.
- Dermatologists may not be perceived as nail experts by the public, indicating a need for increased community education on the role of dermatologists in treating nail disease.
The Case for Biomarker Testing in Gastroesophageal Cancer
For patients to fully benefit from the latest targeted therapies, biomarker testing needs to improve, explained Yelena Janjigian, MD, chief of gastrointestinal oncology at the Memorial Sloan Kettering Cancer Center in New York City.
“The biomarker revolution in this disease has been quite remarkable in the last 10 years, so it’s very important to routinely test for these biomarkers,” Dr. Janjigian said in a presentation at the 2024 ASCO Gastrointestinal Cancers Symposium.
Dr. Janjigian suspected that inertia and logistics are the main reasons biomarker testing rates have lagged. “Even at tertiary cancer centers like ours, we fall short,” she said. For practices that don’t see many patients with gastroesophageal cancer, the rates are probably worse.
Biomarker testing, however, is readily available, Dr. Janjigian said, and overall, it’s about “being obsessive about doing it and following up on it and training your staff.”
As for how to prioritize biomarker testing for treatment selection, Dr. Janjigian provided her top three picks.
Microsatellite instability (MSI) is the most important biomarker, followed by human epidermal growth factor receptor 2 (HER2) as well as tumors expressing programmed death–ligand 1 (PD-L1) with a combined positive score (CPS) of 5 or higher.
Claudin 18.2 testing is “a great newcomer” worth mentioning as well, she noted. Claudin 18.2 is “very druggable,” and several claudin-targeting drugs are currently being assessed, including zolbetuximab.
MSI testing earned the top spot for Dr. Janjigian given the overall survival results from the CHECKMATE 649 trial.
The trial, which Dr. Janjigian led, assessed treatment with first-line nivolumab plus chemotherapy, nivolumab plus ipilimumab, or chemotherapy alone in patients with advanced gastric cancer, gastroesophageal junction cancer, or esophageal adenocarcinoma.
Median overall survival among the small subset of patients with high MSI who received nivolumab plus chemotherapy (n = 23) was more than three times longer than that among those who received chemotherapy alone (n = 21) — 38.7 months vs 12.3 months. Median overall survival was not reached in patients with high MSI who received nivolumab plus ipilimumab at the trial’s 36-month follow-up.
Dr. Janjigian’s case for a PD-L1 CPS of 5 or higher also came, in part, from the CHECKMATE 649 trial. In a subgroup analysis, patients with a CPS of 5 or higher receiving nivolumab plus chemotherapy had a significantly higher median overall survival of 14.4 months vs 11.1 months with chemotherapy alone.
Dr. Janjigian made the case for HER2 testing based on outcomes from the KEYNOTE 811 trial.
This trial, also led by Dr. Janjigian, randomized HER2-positive patients with unresectable advanced gastroesophageal junction adenocarcinoma irrespective of PDL-1 status to pembrolizumab plus trastuzumab and chemotherapy or trastuzumab and chemotherapy alone.
Past studies have reported that targeting HER2 by itself is not a good idea, Dr. Janjigian said, but this trial demonstrated that dual PD-L1/HER2 blockade improves survival outcomes.
Median overall survival in HER2-positive patients with a PD-L1 CPS of 1 or more was 20.0 months vs 15.7 months (hazard ratio [HR], 0.81; 95% CI, 0.67-0.98) compared with 20.0 vs 16.8 months in the overall cohort (HR, 0.84; 95% CI, 0.70-1.01). However, patients with PD-L1 CPS below 1 showed limited benefit from pembrolizumab (HR, 1.41 for overall survival; 95% CI, 0.90-2.20).
To take advantage of the benefit, HER2 testing is “critical,” Dr. Janjigian said.
Overall, when it comes to targeted therapy for advanced disease, the evolution has been rapid. But “we are not done yet,” she said. “We need to be smarter about patient selection” by using biomarker testing.
Dr. Janjigian reported a range of industry ties, including travel expenses, honoraria, and research funding from nivolumab maker Bristol Myers Squibb and Merck, the maker of pembrolizumab. She also advises both companies.
A version of this article first appeared on Medscape.com.
For patients to fully benefit from the latest targeted therapies, biomarker testing needs to improve, explained Yelena Janjigian, MD, chief of gastrointestinal oncology at the Memorial Sloan Kettering Cancer Center in New York City.
“The biomarker revolution in this disease has been quite remarkable in the last 10 years, so it’s very important to routinely test for these biomarkers,” Dr. Janjigian said in a presentation at the 2024 ASCO Gastrointestinal Cancers Symposium.
Dr. Janjigian suspected that inertia and logistics are the main reasons biomarker testing rates have lagged. “Even at tertiary cancer centers like ours, we fall short,” she said. For practices that don’t see many patients with gastroesophageal cancer, the rates are probably worse.
Biomarker testing, however, is readily available, Dr. Janjigian said, and overall, it’s about “being obsessive about doing it and following up on it and training your staff.”
As for how to prioritize biomarker testing for treatment selection, Dr. Janjigian provided her top three picks.
Microsatellite instability (MSI) is the most important biomarker, followed by human epidermal growth factor receptor 2 (HER2) as well as tumors expressing programmed death–ligand 1 (PD-L1) with a combined positive score (CPS) of 5 or higher.
Claudin 18.2 testing is “a great newcomer” worth mentioning as well, she noted. Claudin 18.2 is “very druggable,” and several claudin-targeting drugs are currently being assessed, including zolbetuximab.
MSI testing earned the top spot for Dr. Janjigian given the overall survival results from the CHECKMATE 649 trial.
The trial, which Dr. Janjigian led, assessed treatment with first-line nivolumab plus chemotherapy, nivolumab plus ipilimumab, or chemotherapy alone in patients with advanced gastric cancer, gastroesophageal junction cancer, or esophageal adenocarcinoma.
Median overall survival among the small subset of patients with high MSI who received nivolumab plus chemotherapy (n = 23) was more than three times longer than that among those who received chemotherapy alone (n = 21) — 38.7 months vs 12.3 months. Median overall survival was not reached in patients with high MSI who received nivolumab plus ipilimumab at the trial’s 36-month follow-up.
Dr. Janjigian’s case for a PD-L1 CPS of 5 or higher also came, in part, from the CHECKMATE 649 trial. In a subgroup analysis, patients with a CPS of 5 or higher receiving nivolumab plus chemotherapy had a significantly higher median overall survival of 14.4 months vs 11.1 months with chemotherapy alone.
Dr. Janjigian made the case for HER2 testing based on outcomes from the KEYNOTE 811 trial.
This trial, also led by Dr. Janjigian, randomized HER2-positive patients with unresectable advanced gastroesophageal junction adenocarcinoma irrespective of PDL-1 status to pembrolizumab plus trastuzumab and chemotherapy or trastuzumab and chemotherapy alone.
Past studies have reported that targeting HER2 by itself is not a good idea, Dr. Janjigian said, but this trial demonstrated that dual PD-L1/HER2 blockade improves survival outcomes.
Median overall survival in HER2-positive patients with a PD-L1 CPS of 1 or more was 20.0 months vs 15.7 months (hazard ratio [HR], 0.81; 95% CI, 0.67-0.98) compared with 20.0 vs 16.8 months in the overall cohort (HR, 0.84; 95% CI, 0.70-1.01). However, patients with PD-L1 CPS below 1 showed limited benefit from pembrolizumab (HR, 1.41 for overall survival; 95% CI, 0.90-2.20).
To take advantage of the benefit, HER2 testing is “critical,” Dr. Janjigian said.
Overall, when it comes to targeted therapy for advanced disease, the evolution has been rapid. But “we are not done yet,” she said. “We need to be smarter about patient selection” by using biomarker testing.
Dr. Janjigian reported a range of industry ties, including travel expenses, honoraria, and research funding from nivolumab maker Bristol Myers Squibb and Merck, the maker of pembrolizumab. She also advises both companies.
A version of this article first appeared on Medscape.com.
For patients to fully benefit from the latest targeted therapies, biomarker testing needs to improve, explained Yelena Janjigian, MD, chief of gastrointestinal oncology at the Memorial Sloan Kettering Cancer Center in New York City.
“The biomarker revolution in this disease has been quite remarkable in the last 10 years, so it’s very important to routinely test for these biomarkers,” Dr. Janjigian said in a presentation at the 2024 ASCO Gastrointestinal Cancers Symposium.
Dr. Janjigian suspected that inertia and logistics are the main reasons biomarker testing rates have lagged. “Even at tertiary cancer centers like ours, we fall short,” she said. For practices that don’t see many patients with gastroesophageal cancer, the rates are probably worse.
Biomarker testing, however, is readily available, Dr. Janjigian said, and overall, it’s about “being obsessive about doing it and following up on it and training your staff.”
As for how to prioritize biomarker testing for treatment selection, Dr. Janjigian provided her top three picks.
Microsatellite instability (MSI) is the most important biomarker, followed by human epidermal growth factor receptor 2 (HER2) as well as tumors expressing programmed death–ligand 1 (PD-L1) with a combined positive score (CPS) of 5 or higher.
Claudin 18.2 testing is “a great newcomer” worth mentioning as well, she noted. Claudin 18.2 is “very druggable,” and several claudin-targeting drugs are currently being assessed, including zolbetuximab.
MSI testing earned the top spot for Dr. Janjigian given the overall survival results from the CHECKMATE 649 trial.
The trial, which Dr. Janjigian led, assessed treatment with first-line nivolumab plus chemotherapy, nivolumab plus ipilimumab, or chemotherapy alone in patients with advanced gastric cancer, gastroesophageal junction cancer, or esophageal adenocarcinoma.
Median overall survival among the small subset of patients with high MSI who received nivolumab plus chemotherapy (n = 23) was more than three times longer than that among those who received chemotherapy alone (n = 21) — 38.7 months vs 12.3 months. Median overall survival was not reached in patients with high MSI who received nivolumab plus ipilimumab at the trial’s 36-month follow-up.
Dr. Janjigian’s case for a PD-L1 CPS of 5 or higher also came, in part, from the CHECKMATE 649 trial. In a subgroup analysis, patients with a CPS of 5 or higher receiving nivolumab plus chemotherapy had a significantly higher median overall survival of 14.4 months vs 11.1 months with chemotherapy alone.
Dr. Janjigian made the case for HER2 testing based on outcomes from the KEYNOTE 811 trial.
This trial, also led by Dr. Janjigian, randomized HER2-positive patients with unresectable advanced gastroesophageal junction adenocarcinoma irrespective of PDL-1 status to pembrolizumab plus trastuzumab and chemotherapy or trastuzumab and chemotherapy alone.
Past studies have reported that targeting HER2 by itself is not a good idea, Dr. Janjigian said, but this trial demonstrated that dual PD-L1/HER2 blockade improves survival outcomes.
Median overall survival in HER2-positive patients with a PD-L1 CPS of 1 or more was 20.0 months vs 15.7 months (hazard ratio [HR], 0.81; 95% CI, 0.67-0.98) compared with 20.0 vs 16.8 months in the overall cohort (HR, 0.84; 95% CI, 0.70-1.01). However, patients with PD-L1 CPS below 1 showed limited benefit from pembrolizumab (HR, 1.41 for overall survival; 95% CI, 0.90-2.20).
To take advantage of the benefit, HER2 testing is “critical,” Dr. Janjigian said.
Overall, when it comes to targeted therapy for advanced disease, the evolution has been rapid. But “we are not done yet,” she said. “We need to be smarter about patient selection” by using biomarker testing.
Dr. Janjigian reported a range of industry ties, including travel expenses, honoraria, and research funding from nivolumab maker Bristol Myers Squibb and Merck, the maker of pembrolizumab. She also advises both companies.
A version of this article first appeared on Medscape.com.
FROM ASCO GI 2024
Hepatic infusion pumps: New enthusiasm for an old technology
Dutch investigators reported a 3-year overall survival of 33% in patients with advanced, unresectable cholangiocarcinoma confined to the liver who received the infusion chemotherapy vs 3% in historical controls treated with standard systemic gemcitabine/cisplatin.
The response with the pump is “clearly superior” to systemic treatment, said investigator Bas Groot Koerkamp, MD, who presented the findings at the ASCO Gastrointestinal Cancers Symposium.
“I do share the enthusiasm of my colleagues about immunotherapy and targeted treatments for intrahepatic cholangiocarcinoma,” said Dr. Koerkamp, a hepato-pancreato-biliary surgeon at Erasmus University Medical Center, Rotterdam, the Netherlands. But “none of these treatments has shown a 3-year overall survival of one in three with advanced disease.”
The hepatic arterial infusion pump, a hockey puck-sized device that essentially bathes liver tumors in floxuridine for about 2 weeks, is not a new technology. The pump has been around since at least the 1990s, developed largely at Memorial Sloan Kettering Cancer Center, New York City, where Dr. Koerkamp trained.
Three previous small studies in cholangiocarcinoma reported outcomes similar to Dr. Koerkamp’s. Despite the strong survival outcomes, uptake of these pumps has lagged.
A key reason is likely the lack of phase 3 trials evaluating the technology, Laleh Melstrom, MD, chief of surgical oncology at City of Hope, outside of Los Angeles, Duarte, California, told this news organization.
Dr. Melstrom, who moderated Dr. Koerkamp’s presentation, also noted that using the pump requires special attention to bilirubin levels to prevent biliary toxicity and knowledge of pump placement.
The pump, placed subcutaneously on one side of the lower abdomen, is connected to a side branch of the hepatic artery and then filled with the chemotherapy agent floxuridine. Delivering floxuridine directly to the hepatic artery increases liver lesion exposure 200-fold over systemic delivery. The pump needs to be refilled after 2 weeks.
“It’s not difficult to place the pump, even doing it robotically,” which was how it was placed in over 40% of patients in the study, Dr. Koerkamp said.
As for biliary toxicity, only one patient in the current study developed biliary sclerosis, which was easily handled with a stent. “You just put in a stent and continue,” Dr. Koerkamp said.
The current single-arm phase 2 study included 50 patients implanted with the hepatic pump at three centers in the Netherlands. All patients had advanced, unresectable cholangiocarcinoma confined to the liver.
Ultimately, 48 of 50 patients received treatment after one patient died of unrelated causes and another had an arterial dissection.
Overall, 38 received gemcitabine/cisplatin concurrently, and the remaining had the pump treatment alone, having already received the systemic combination. Most (84%) received at least four cycles of chemotherapy infusion.
Almost half of patients (46%) had a partial response to treatment, and 88% exhibited disease control at 6 months. Four patients who responded underwent a liver resection, one of whom had a complete pathologic response.
Median overall survival was 22 months vs 12 months in historical controls. One-year median overall survival was 80% in the treatment group vs 47% in controls, and 3-year median overall survival was 33% in the pump group vs 3% in controls.
An audience member noted that similar results have been reported for transarterial Yttrium-90 radioembolization, another and newer option to treat intrahepatic cholangiocarcinoma.
“The Y90 results are quite impressive,” Dr. Koerkamp said, adding that he’d like to see a head-to-head comparison.
“The main advantage of the pump is that it treats the entire liver,” as opposed to one lesion at a time, “so if you have 10 lesions [the pump] makes a lot more sense,” he said.
There is “definitely a movement” to “reinvigorate” the hepatic artery infusion pump approach, Dr. Melstrom said.
The study was funded by the Dutch Cancer Society. Dr. Koerkamp disclosed research funding from Tricumed, a maker of implantable infusion pumps. Dr. Melstrom didn’t have any disclosures.
A version of this article first appeared on Medscape.com.
Dutch investigators reported a 3-year overall survival of 33% in patients with advanced, unresectable cholangiocarcinoma confined to the liver who received the infusion chemotherapy vs 3% in historical controls treated with standard systemic gemcitabine/cisplatin.
The response with the pump is “clearly superior” to systemic treatment, said investigator Bas Groot Koerkamp, MD, who presented the findings at the ASCO Gastrointestinal Cancers Symposium.
“I do share the enthusiasm of my colleagues about immunotherapy and targeted treatments for intrahepatic cholangiocarcinoma,” said Dr. Koerkamp, a hepato-pancreato-biliary surgeon at Erasmus University Medical Center, Rotterdam, the Netherlands. But “none of these treatments has shown a 3-year overall survival of one in three with advanced disease.”
The hepatic arterial infusion pump, a hockey puck-sized device that essentially bathes liver tumors in floxuridine for about 2 weeks, is not a new technology. The pump has been around since at least the 1990s, developed largely at Memorial Sloan Kettering Cancer Center, New York City, where Dr. Koerkamp trained.
Three previous small studies in cholangiocarcinoma reported outcomes similar to Dr. Koerkamp’s. Despite the strong survival outcomes, uptake of these pumps has lagged.
A key reason is likely the lack of phase 3 trials evaluating the technology, Laleh Melstrom, MD, chief of surgical oncology at City of Hope, outside of Los Angeles, Duarte, California, told this news organization.
Dr. Melstrom, who moderated Dr. Koerkamp’s presentation, also noted that using the pump requires special attention to bilirubin levels to prevent biliary toxicity and knowledge of pump placement.
The pump, placed subcutaneously on one side of the lower abdomen, is connected to a side branch of the hepatic artery and then filled with the chemotherapy agent floxuridine. Delivering floxuridine directly to the hepatic artery increases liver lesion exposure 200-fold over systemic delivery. The pump needs to be refilled after 2 weeks.
“It’s not difficult to place the pump, even doing it robotically,” which was how it was placed in over 40% of patients in the study, Dr. Koerkamp said.
As for biliary toxicity, only one patient in the current study developed biliary sclerosis, which was easily handled with a stent. “You just put in a stent and continue,” Dr. Koerkamp said.
The current single-arm phase 2 study included 50 patients implanted with the hepatic pump at three centers in the Netherlands. All patients had advanced, unresectable cholangiocarcinoma confined to the liver.
Ultimately, 48 of 50 patients received treatment after one patient died of unrelated causes and another had an arterial dissection.
Overall, 38 received gemcitabine/cisplatin concurrently, and the remaining had the pump treatment alone, having already received the systemic combination. Most (84%) received at least four cycles of chemotherapy infusion.
Almost half of patients (46%) had a partial response to treatment, and 88% exhibited disease control at 6 months. Four patients who responded underwent a liver resection, one of whom had a complete pathologic response.
Median overall survival was 22 months vs 12 months in historical controls. One-year median overall survival was 80% in the treatment group vs 47% in controls, and 3-year median overall survival was 33% in the pump group vs 3% in controls.
An audience member noted that similar results have been reported for transarterial Yttrium-90 radioembolization, another and newer option to treat intrahepatic cholangiocarcinoma.
“The Y90 results are quite impressive,” Dr. Koerkamp said, adding that he’d like to see a head-to-head comparison.
“The main advantage of the pump is that it treats the entire liver,” as opposed to one lesion at a time, “so if you have 10 lesions [the pump] makes a lot more sense,” he said.
There is “definitely a movement” to “reinvigorate” the hepatic artery infusion pump approach, Dr. Melstrom said.
The study was funded by the Dutch Cancer Society. Dr. Koerkamp disclosed research funding from Tricumed, a maker of implantable infusion pumps. Dr. Melstrom didn’t have any disclosures.
A version of this article first appeared on Medscape.com.
Dutch investigators reported a 3-year overall survival of 33% in patients with advanced, unresectable cholangiocarcinoma confined to the liver who received the infusion chemotherapy vs 3% in historical controls treated with standard systemic gemcitabine/cisplatin.
The response with the pump is “clearly superior” to systemic treatment, said investigator Bas Groot Koerkamp, MD, who presented the findings at the ASCO Gastrointestinal Cancers Symposium.
“I do share the enthusiasm of my colleagues about immunotherapy and targeted treatments for intrahepatic cholangiocarcinoma,” said Dr. Koerkamp, a hepato-pancreato-biliary surgeon at Erasmus University Medical Center, Rotterdam, the Netherlands. But “none of these treatments has shown a 3-year overall survival of one in three with advanced disease.”
The hepatic arterial infusion pump, a hockey puck-sized device that essentially bathes liver tumors in floxuridine for about 2 weeks, is not a new technology. The pump has been around since at least the 1990s, developed largely at Memorial Sloan Kettering Cancer Center, New York City, where Dr. Koerkamp trained.
Three previous small studies in cholangiocarcinoma reported outcomes similar to Dr. Koerkamp’s. Despite the strong survival outcomes, uptake of these pumps has lagged.
A key reason is likely the lack of phase 3 trials evaluating the technology, Laleh Melstrom, MD, chief of surgical oncology at City of Hope, outside of Los Angeles, Duarte, California, told this news organization.
Dr. Melstrom, who moderated Dr. Koerkamp’s presentation, also noted that using the pump requires special attention to bilirubin levels to prevent biliary toxicity and knowledge of pump placement.
The pump, placed subcutaneously on one side of the lower abdomen, is connected to a side branch of the hepatic artery and then filled with the chemotherapy agent floxuridine. Delivering floxuridine directly to the hepatic artery increases liver lesion exposure 200-fold over systemic delivery. The pump needs to be refilled after 2 weeks.
“It’s not difficult to place the pump, even doing it robotically,” which was how it was placed in over 40% of patients in the study, Dr. Koerkamp said.
As for biliary toxicity, only one patient in the current study developed biliary sclerosis, which was easily handled with a stent. “You just put in a stent and continue,” Dr. Koerkamp said.
The current single-arm phase 2 study included 50 patients implanted with the hepatic pump at three centers in the Netherlands. All patients had advanced, unresectable cholangiocarcinoma confined to the liver.
Ultimately, 48 of 50 patients received treatment after one patient died of unrelated causes and another had an arterial dissection.
Overall, 38 received gemcitabine/cisplatin concurrently, and the remaining had the pump treatment alone, having already received the systemic combination. Most (84%) received at least four cycles of chemotherapy infusion.
Almost half of patients (46%) had a partial response to treatment, and 88% exhibited disease control at 6 months. Four patients who responded underwent a liver resection, one of whom had a complete pathologic response.
Median overall survival was 22 months vs 12 months in historical controls. One-year median overall survival was 80% in the treatment group vs 47% in controls, and 3-year median overall survival was 33% in the pump group vs 3% in controls.
An audience member noted that similar results have been reported for transarterial Yttrium-90 radioembolization, another and newer option to treat intrahepatic cholangiocarcinoma.
“The Y90 results are quite impressive,” Dr. Koerkamp said, adding that he’d like to see a head-to-head comparison.
“The main advantage of the pump is that it treats the entire liver,” as opposed to one lesion at a time, “so if you have 10 lesions [the pump] makes a lot more sense,” he said.
There is “definitely a movement” to “reinvigorate” the hepatic artery infusion pump approach, Dr. Melstrom said.
The study was funded by the Dutch Cancer Society. Dr. Koerkamp disclosed research funding from Tricumed, a maker of implantable infusion pumps. Dr. Melstrom didn’t have any disclosures.
A version of this article first appeared on Medscape.com.
FROM ASCO GI 2024
Blue to Slate Gray Discoloration of the Proximal Fingernails
The Diagnosis: Argyria-Induced Azure Lunulae
Argyria is an acquired condition resulting from excessive exogenous exposure to silver with subsequent gastrointestinal absorption and pigmentary tissue deposition. Upon further questioning, our patient disclosed a lifetime history of colloidal silver use, both as a topical antiseptic agent and intraorally for aphthous ulcers. Silver has a predilection for granular deposition in stromal tissues and basement membranes with sparing of the epidermis, manifesting as progressive, permanent, blue to slate gray discoloration of sunexposed skin, mucous membranes, and nail beds.1 The patient was advised to discontinue use of colloidal silver to avoid development of further pigmentary changes. The appearance of his nails remained unchanged in the months following initial presentation, as expected, since argyria pigmentation is not anticipated to reverse upon colloidal silver cessation.
Nail involvement may be an early presentation of generalized argyria or may be found in isolation, as seen in our patient. Early recognition and patient education are essential to minimize cumulative silver deposition. Although dyspigmentation may impact psychosocial well-being secondary to aesthetic concerns, there is limited research supporting adverse systemic effects of argyria confined to the nail beds. Similarly, the majority of generalized cases are not associated with systemic complications; however, potential toxicities, as described in isolated case reports without conclusive causal relationships, include nyctalopia, renal or hepatic toxicity, pulmonary fibrosis, and neuropsychiatric events.1-6 Successful treatment of cutaneous argyria has been reported with the 1064-nm Q-switched Nd:YAG laser; however, there have been no reported treatments for nail bed involvement.7 Due to the absence of systemic symptoms, additional mucocutaneous dyspigmentation, or cosmetic concerns regarding nail bed lunulae discoloration in our patient, no further intervention was pursued, except for continued colloidal silver cessation.
The differential diagnosis of blue-gray nail bed dyspigmentation is broad and includes cyanosis secondary to cardiopulmonary disease, drug-induced dyspigmentation, Wilson disease, argyria, chrysiasis, hereditary acrolabial telangiectasia, and pseudomonal infection or chloronychia.1,8,9 Etiologic insight may be provided from a thorough review of prescription and over-the-counter medications as well as careful attention to the distribution of dyspigmentation. Medications commonly associated with bluish nail bed dyspigmentation include antimalarials, amiodarone, minocycline, clofazimine, chlorpromazine/phenothiazines, and various chemotherapeutic drugs; our patient was not taking any of these.1,9
Cyanotic nail bed dyspigmentation secondary to cardiopulmonary disease likely manifests with more diffuse nail bed dyspigmentation and is not confined solely to the lunulae. Only drug-induced dyspigmentation, classically due to phenolphthalein-containing laxatives; Wilson disease; and argyria have a tendency to spare the distal nail bed, which is a presentation termed azure lunulae.8 The toenails typically are spared in argyria, while toenail involvement is variable in Wilson disease, and additional systemic symptoms—including hepatic, ophthalmologic, and neuropsychiatric—as well as potential family history would be expected.8 Phenolphthalein is no longer available in over-the-counter laxatives, as it was formally banned by the US Food and Drug Administration in 1999 due to concerns of carcinogenicity.10
Hereditary acrolabial telangiectasia is a familial condition with autosomal-dominant inheritance that can manifest similarly to argyria with blue-gray discoloration of the proximal nail bed; however, this condition also would demonstrate involvement of the vermilion border and nipple areolae, often with associated telangiectasia and migraine headaches.11
Chloronychia (also known as green nail syndrome) is an infection of the nail bed with Pseudomonas aeruginosa that more commonly presents with greenblack discoloration with variable involvement of the fingernails and toenails. Chloronychia, often with associated onycholysis, typically is found in individuals with repeated exposure to water, soaps, and detergents.12 Our patient’s long-standing and unwavering nail bed appearance, involvement of all fingernail lunulae, lack of additional symptoms, and disclosed use of over-the-counter colloidal silver supported a clinical diagnosis of argyriainduced azure lunulae.
Argyria-induced azure lunulae secondary to colloidal silver exposure is an uncommon yet clinically significant cause of nail bed dyspigmentation. Prompt identification and cessation of the offending agent can prevent progression of mucocutaneous dyspigmentation and avoid potential long-term sequelae from systemic deposition.
- Mota L, Dinis-Oliveira RJ. Clinical and forensic aspects of the different subtypes of argyria. J Clin Med. 2021;10:2086. doi:10.3390/ jcm10102086
- Osin´ska J, Poborc-Godlewska J, Kiec´-Swierczyn´ska M, et al. 6 cases of argyria among workers engaged in silverplating radio subunits. Med Pr. 1982;33:361-364.
- Mayr M, Kim MJ, Wanner D, et al. Argyria and decreased kidney function: are silver compounds toxic to the kidney? Am J Kidney Dis. 2009;53:890-894. doi:10.1053/j.ajkd.2008.08.028
- Trop M, Novak M, Rodl S, et al. Silver-coated dressing acticoat caused raised liver enzymes and argyria-like symptoms in burn patient. J Trauma. 2006;60:648-652. doi:10.1097/01.ta.0000208126 .22089.b6
- Mirsattari SM, Hammond RR, Sharpe MD, et al. Myoclonic status epilepticus following repeated oral ingestion of colloidal silver. Neurology. 2004;62:1408-1410. doi:10.1212/01.wnl.0000120671.73335.ec
- Barrie HJ, Harding HE. Argyro-siderosis of the lungs in silver finishers. Br J Ind Med. 1947;4:225-229. doi:10.1136/oem.4.4.225
- Griffith RD, Simmons BJ, Bray FN, et al. 1064 nm Q-switched Nd:YAG laser for the treatment of argyria: a systematic review. J Eur Acad Dermatol Venereol. 2015;29:2100-2103. doi:10.111 1/jdv.13117
- Rubin AI, Jellinek NJ, Daniel CR III, et al, eds. Scher and Daniel’s Nails: Diagnosis, Surgery, Therapy. 4th ed. Springer; 2018.
- Slater K, Sommariva E, Kartono F. A case study of argyria of the nails secondary to colloidal silver ingestion [published online October 28, 2022]. Cureus. 2022;14:E30818. doi:10.7759/cureus.30818
- Hubbard WK. Laxative drug products for over-the-counter human use. Fed Register. 1999;64:4535-4540. Accessed January 5, 2024. https://www.govinfo.gov/content/pkg/FR-1999-01-29/html/99-1938.htm
- Millns JL, Dicken CH. Hereditary acrolabial telangiectasia. a report of familial blue lips, nails, and nipples. Arch Dermatol. 1979;115:474-478. doi:10.1001/archderm.115.4.474
- Chiriac A, Brzezinski P, Foia L, et al. Chloronychia: green nail syndrome caused by Pseudomonas aeruginosa in elderly persons [published online January 14, 2015]. Clin Interv Aging. 2015;10:265-267. doi:10.2147/CIA.S75525
The Diagnosis: Argyria-Induced Azure Lunulae
Argyria is an acquired condition resulting from excessive exogenous exposure to silver with subsequent gastrointestinal absorption and pigmentary tissue deposition. Upon further questioning, our patient disclosed a lifetime history of colloidal silver use, both as a topical antiseptic agent and intraorally for aphthous ulcers. Silver has a predilection for granular deposition in stromal tissues and basement membranes with sparing of the epidermis, manifesting as progressive, permanent, blue to slate gray discoloration of sunexposed skin, mucous membranes, and nail beds.1 The patient was advised to discontinue use of colloidal silver to avoid development of further pigmentary changes. The appearance of his nails remained unchanged in the months following initial presentation, as expected, since argyria pigmentation is not anticipated to reverse upon colloidal silver cessation.
Nail involvement may be an early presentation of generalized argyria or may be found in isolation, as seen in our patient. Early recognition and patient education are essential to minimize cumulative silver deposition. Although dyspigmentation may impact psychosocial well-being secondary to aesthetic concerns, there is limited research supporting adverse systemic effects of argyria confined to the nail beds. Similarly, the majority of generalized cases are not associated with systemic complications; however, potential toxicities, as described in isolated case reports without conclusive causal relationships, include nyctalopia, renal or hepatic toxicity, pulmonary fibrosis, and neuropsychiatric events.1-6 Successful treatment of cutaneous argyria has been reported with the 1064-nm Q-switched Nd:YAG laser; however, there have been no reported treatments for nail bed involvement.7 Due to the absence of systemic symptoms, additional mucocutaneous dyspigmentation, or cosmetic concerns regarding nail bed lunulae discoloration in our patient, no further intervention was pursued, except for continued colloidal silver cessation.
The differential diagnosis of blue-gray nail bed dyspigmentation is broad and includes cyanosis secondary to cardiopulmonary disease, drug-induced dyspigmentation, Wilson disease, argyria, chrysiasis, hereditary acrolabial telangiectasia, and pseudomonal infection or chloronychia.1,8,9 Etiologic insight may be provided from a thorough review of prescription and over-the-counter medications as well as careful attention to the distribution of dyspigmentation. Medications commonly associated with bluish nail bed dyspigmentation include antimalarials, amiodarone, minocycline, clofazimine, chlorpromazine/phenothiazines, and various chemotherapeutic drugs; our patient was not taking any of these.1,9
Cyanotic nail bed dyspigmentation secondary to cardiopulmonary disease likely manifests with more diffuse nail bed dyspigmentation and is not confined solely to the lunulae. Only drug-induced dyspigmentation, classically due to phenolphthalein-containing laxatives; Wilson disease; and argyria have a tendency to spare the distal nail bed, which is a presentation termed azure lunulae.8 The toenails typically are spared in argyria, while toenail involvement is variable in Wilson disease, and additional systemic symptoms—including hepatic, ophthalmologic, and neuropsychiatric—as well as potential family history would be expected.8 Phenolphthalein is no longer available in over-the-counter laxatives, as it was formally banned by the US Food and Drug Administration in 1999 due to concerns of carcinogenicity.10
Hereditary acrolabial telangiectasia is a familial condition with autosomal-dominant inheritance that can manifest similarly to argyria with blue-gray discoloration of the proximal nail bed; however, this condition also would demonstrate involvement of the vermilion border and nipple areolae, often with associated telangiectasia and migraine headaches.11
Chloronychia (also known as green nail syndrome) is an infection of the nail bed with Pseudomonas aeruginosa that more commonly presents with greenblack discoloration with variable involvement of the fingernails and toenails. Chloronychia, often with associated onycholysis, typically is found in individuals with repeated exposure to water, soaps, and detergents.12 Our patient’s long-standing and unwavering nail bed appearance, involvement of all fingernail lunulae, lack of additional symptoms, and disclosed use of over-the-counter colloidal silver supported a clinical diagnosis of argyriainduced azure lunulae.
Argyria-induced azure lunulae secondary to colloidal silver exposure is an uncommon yet clinically significant cause of nail bed dyspigmentation. Prompt identification and cessation of the offending agent can prevent progression of mucocutaneous dyspigmentation and avoid potential long-term sequelae from systemic deposition.
The Diagnosis: Argyria-Induced Azure Lunulae
Argyria is an acquired condition resulting from excessive exogenous exposure to silver with subsequent gastrointestinal absorption and pigmentary tissue deposition. Upon further questioning, our patient disclosed a lifetime history of colloidal silver use, both as a topical antiseptic agent and intraorally for aphthous ulcers. Silver has a predilection for granular deposition in stromal tissues and basement membranes with sparing of the epidermis, manifesting as progressive, permanent, blue to slate gray discoloration of sunexposed skin, mucous membranes, and nail beds.1 The patient was advised to discontinue use of colloidal silver to avoid development of further pigmentary changes. The appearance of his nails remained unchanged in the months following initial presentation, as expected, since argyria pigmentation is not anticipated to reverse upon colloidal silver cessation.
Nail involvement may be an early presentation of generalized argyria or may be found in isolation, as seen in our patient. Early recognition and patient education are essential to minimize cumulative silver deposition. Although dyspigmentation may impact psychosocial well-being secondary to aesthetic concerns, there is limited research supporting adverse systemic effects of argyria confined to the nail beds. Similarly, the majority of generalized cases are not associated with systemic complications; however, potential toxicities, as described in isolated case reports without conclusive causal relationships, include nyctalopia, renal or hepatic toxicity, pulmonary fibrosis, and neuropsychiatric events.1-6 Successful treatment of cutaneous argyria has been reported with the 1064-nm Q-switched Nd:YAG laser; however, there have been no reported treatments for nail bed involvement.7 Due to the absence of systemic symptoms, additional mucocutaneous dyspigmentation, or cosmetic concerns regarding nail bed lunulae discoloration in our patient, no further intervention was pursued, except for continued colloidal silver cessation.
The differential diagnosis of blue-gray nail bed dyspigmentation is broad and includes cyanosis secondary to cardiopulmonary disease, drug-induced dyspigmentation, Wilson disease, argyria, chrysiasis, hereditary acrolabial telangiectasia, and pseudomonal infection or chloronychia.1,8,9 Etiologic insight may be provided from a thorough review of prescription and over-the-counter medications as well as careful attention to the distribution of dyspigmentation. Medications commonly associated with bluish nail bed dyspigmentation include antimalarials, amiodarone, minocycline, clofazimine, chlorpromazine/phenothiazines, and various chemotherapeutic drugs; our patient was not taking any of these.1,9
Cyanotic nail bed dyspigmentation secondary to cardiopulmonary disease likely manifests with more diffuse nail bed dyspigmentation and is not confined solely to the lunulae. Only drug-induced dyspigmentation, classically due to phenolphthalein-containing laxatives; Wilson disease; and argyria have a tendency to spare the distal nail bed, which is a presentation termed azure lunulae.8 The toenails typically are spared in argyria, while toenail involvement is variable in Wilson disease, and additional systemic symptoms—including hepatic, ophthalmologic, and neuropsychiatric—as well as potential family history would be expected.8 Phenolphthalein is no longer available in over-the-counter laxatives, as it was formally banned by the US Food and Drug Administration in 1999 due to concerns of carcinogenicity.10
Hereditary acrolabial telangiectasia is a familial condition with autosomal-dominant inheritance that can manifest similarly to argyria with blue-gray discoloration of the proximal nail bed; however, this condition also would demonstrate involvement of the vermilion border and nipple areolae, often with associated telangiectasia and migraine headaches.11
Chloronychia (also known as green nail syndrome) is an infection of the nail bed with Pseudomonas aeruginosa that more commonly presents with greenblack discoloration with variable involvement of the fingernails and toenails. Chloronychia, often with associated onycholysis, typically is found in individuals with repeated exposure to water, soaps, and detergents.12 Our patient’s long-standing and unwavering nail bed appearance, involvement of all fingernail lunulae, lack of additional symptoms, and disclosed use of over-the-counter colloidal silver supported a clinical diagnosis of argyriainduced azure lunulae.
Argyria-induced azure lunulae secondary to colloidal silver exposure is an uncommon yet clinically significant cause of nail bed dyspigmentation. Prompt identification and cessation of the offending agent can prevent progression of mucocutaneous dyspigmentation and avoid potential long-term sequelae from systemic deposition.
- Mota L, Dinis-Oliveira RJ. Clinical and forensic aspects of the different subtypes of argyria. J Clin Med. 2021;10:2086. doi:10.3390/ jcm10102086
- Osin´ska J, Poborc-Godlewska J, Kiec´-Swierczyn´ska M, et al. 6 cases of argyria among workers engaged in silverplating radio subunits. Med Pr. 1982;33:361-364.
- Mayr M, Kim MJ, Wanner D, et al. Argyria and decreased kidney function: are silver compounds toxic to the kidney? Am J Kidney Dis. 2009;53:890-894. doi:10.1053/j.ajkd.2008.08.028
- Trop M, Novak M, Rodl S, et al. Silver-coated dressing acticoat caused raised liver enzymes and argyria-like symptoms in burn patient. J Trauma. 2006;60:648-652. doi:10.1097/01.ta.0000208126 .22089.b6
- Mirsattari SM, Hammond RR, Sharpe MD, et al. Myoclonic status epilepticus following repeated oral ingestion of colloidal silver. Neurology. 2004;62:1408-1410. doi:10.1212/01.wnl.0000120671.73335.ec
- Barrie HJ, Harding HE. Argyro-siderosis of the lungs in silver finishers. Br J Ind Med. 1947;4:225-229. doi:10.1136/oem.4.4.225
- Griffith RD, Simmons BJ, Bray FN, et al. 1064 nm Q-switched Nd:YAG laser for the treatment of argyria: a systematic review. J Eur Acad Dermatol Venereol. 2015;29:2100-2103. doi:10.111 1/jdv.13117
- Rubin AI, Jellinek NJ, Daniel CR III, et al, eds. Scher and Daniel’s Nails: Diagnosis, Surgery, Therapy. 4th ed. Springer; 2018.
- Slater K, Sommariva E, Kartono F. A case study of argyria of the nails secondary to colloidal silver ingestion [published online October 28, 2022]. Cureus. 2022;14:E30818. doi:10.7759/cureus.30818
- Hubbard WK. Laxative drug products for over-the-counter human use. Fed Register. 1999;64:4535-4540. Accessed January 5, 2024. https://www.govinfo.gov/content/pkg/FR-1999-01-29/html/99-1938.htm
- Millns JL, Dicken CH. Hereditary acrolabial telangiectasia. a report of familial blue lips, nails, and nipples. Arch Dermatol. 1979;115:474-478. doi:10.1001/archderm.115.4.474
- Chiriac A, Brzezinski P, Foia L, et al. Chloronychia: green nail syndrome caused by Pseudomonas aeruginosa in elderly persons [published online January 14, 2015]. Clin Interv Aging. 2015;10:265-267. doi:10.2147/CIA.S75525
- Mota L, Dinis-Oliveira RJ. Clinical and forensic aspects of the different subtypes of argyria. J Clin Med. 2021;10:2086. doi:10.3390/ jcm10102086
- Osin´ska J, Poborc-Godlewska J, Kiec´-Swierczyn´ska M, et al. 6 cases of argyria among workers engaged in silverplating radio subunits. Med Pr. 1982;33:361-364.
- Mayr M, Kim MJ, Wanner D, et al. Argyria and decreased kidney function: are silver compounds toxic to the kidney? Am J Kidney Dis. 2009;53:890-894. doi:10.1053/j.ajkd.2008.08.028
- Trop M, Novak M, Rodl S, et al. Silver-coated dressing acticoat caused raised liver enzymes and argyria-like symptoms in burn patient. J Trauma. 2006;60:648-652. doi:10.1097/01.ta.0000208126 .22089.b6
- Mirsattari SM, Hammond RR, Sharpe MD, et al. Myoclonic status epilepticus following repeated oral ingestion of colloidal silver. Neurology. 2004;62:1408-1410. doi:10.1212/01.wnl.0000120671.73335.ec
- Barrie HJ, Harding HE. Argyro-siderosis of the lungs in silver finishers. Br J Ind Med. 1947;4:225-229. doi:10.1136/oem.4.4.225
- Griffith RD, Simmons BJ, Bray FN, et al. 1064 nm Q-switched Nd:YAG laser for the treatment of argyria: a systematic review. J Eur Acad Dermatol Venereol. 2015;29:2100-2103. doi:10.111 1/jdv.13117
- Rubin AI, Jellinek NJ, Daniel CR III, et al, eds. Scher and Daniel’s Nails: Diagnosis, Surgery, Therapy. 4th ed. Springer; 2018.
- Slater K, Sommariva E, Kartono F. A case study of argyria of the nails secondary to colloidal silver ingestion [published online October 28, 2022]. Cureus. 2022;14:E30818. doi:10.7759/cureus.30818
- Hubbard WK. Laxative drug products for over-the-counter human use. Fed Register. 1999;64:4535-4540. Accessed January 5, 2024. https://www.govinfo.gov/content/pkg/FR-1999-01-29/html/99-1938.htm
- Millns JL, Dicken CH. Hereditary acrolabial telangiectasia. a report of familial blue lips, nails, and nipples. Arch Dermatol. 1979;115:474-478. doi:10.1001/archderm.115.4.474
- Chiriac A, Brzezinski P, Foia L, et al. Chloronychia: green nail syndrome caused by Pseudomonas aeruginosa in elderly persons [published online January 14, 2015]. Clin Interv Aging. 2015;10:265-267. doi:10.2147/CIA.S75525
An 88-year-old man presented with asymptomatic and unchanging discoloration of the proximal fingernails of both hands of 50 years’ duration. Physical examination revealed blue to slate gray, subungual pigmentary changes of the fingernails of both hands sparing the nail bed distal to the lunulae. There was no overlying plate dystrophy, toenail involvement, or additional mucocutaneous abnormalities. His medical history was notable for heart failure, obstructive sleep apnea, and type 2 diabetes mellitus. He had no history of hepatic, ophthalmologic, or neurologic dysfunction.
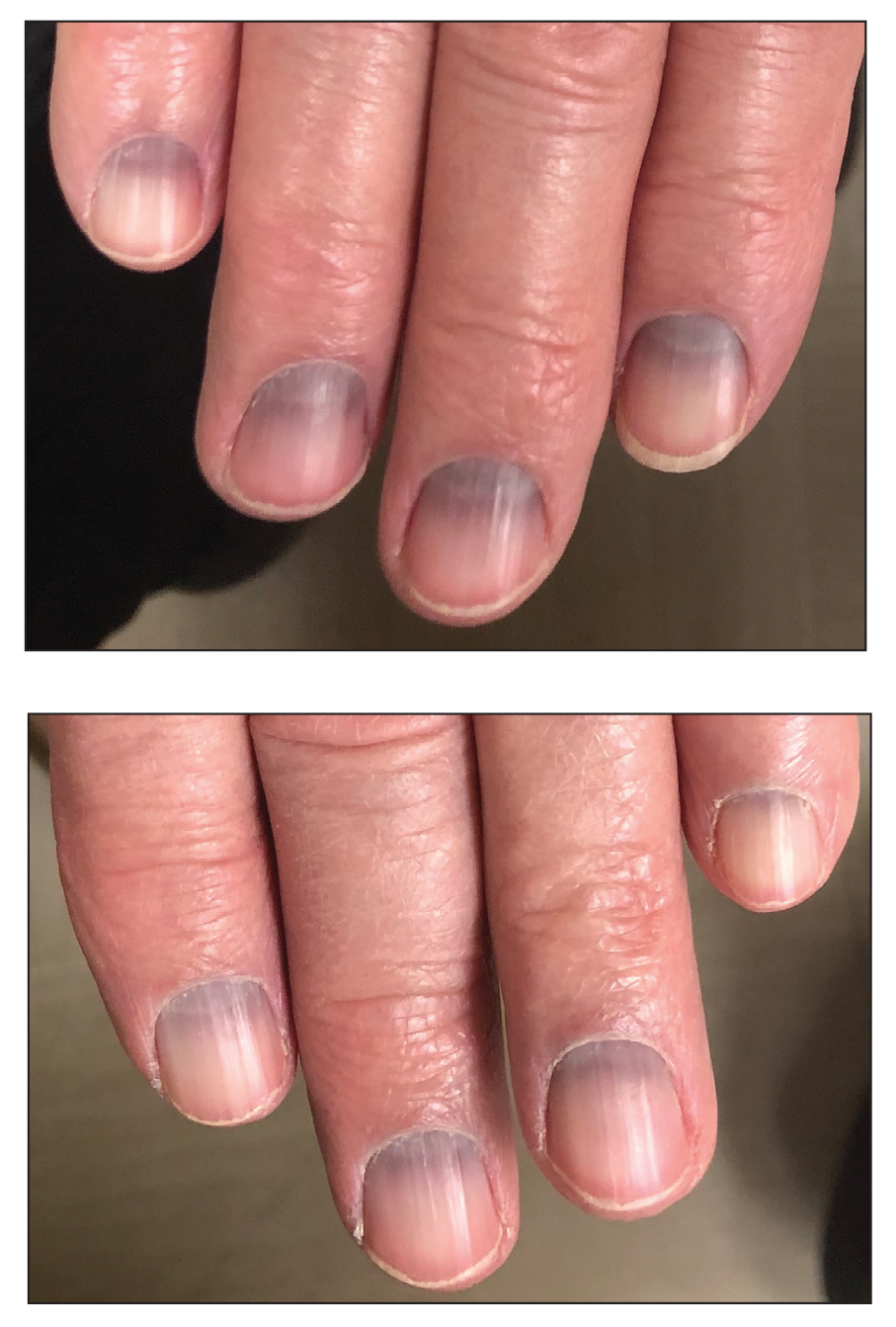
Targeted Colorectal Cancer Combo Improves QoL
Dominik Modest, MD, presented these new results of the phase 3 CodeBreaK 300 trial at the 2024 ASCO Gastrointestinal Cancers Symposium.
The KRAS G12C mutation occurs in 3%-4% of metastatic colorectal cancer cases, according to Dr. Modest and the other authors of a paper published in the New England Journal of Medicine describing the primary outcome of the trial. The study included 160 patients who were randomized to once daily sotorasib (960 mg) plus panitumumab (Soto960), once daily sotorasib (240 mg) plus panitumumab (Soto240), or investigator’s choice of trifluridine–tipiracil or regorafenib.
The December 2023 paper described improvements in median progression-free survival, progression or death, and objective response (OR). The authors described statistically significant improvements in disease progression or death in the Soto960 group (hazard ratio [HR], 0.49; P = .006) and the Soto240 group (HR, 0.58; P = .03). The objective response rate was highest in the Soto960 group (26.4%; 95% CI, 15.3%-40.3%), followed by the Soto240 group (5.7%; 95% CI, 1.2%-15.7%), and the control group (0%; 95% CI, 0.0%-6.6%). Grade 3 or higher treatment-related adverse events were generally similar at 35.8% (Soto960), 30.2% (Soto240), and 43.1% (control) in each group. The most common adverse events associated with sotorasib-panitumumab were skin-related toxicity and hypomagnesemia.
The new analysis showed that both doses of sotorasib also improved patient-reported outcomes from baseline to week 8, Dr. Modest, professor of medicine at Charité University of Medicine in Berlin, said at the meeting.
Compared with the chemotherapy group, there were statistically significant differences in least square mean change from baseline to week 8 for: pain at its worst in the Soto240 group (Brief Pain Inventory [BPI], –1.18; 95% CI, –2.05 to –0.32) and the Soto960 group (BPI, –1.49; 95% CI, –2.36 to –0.61); and physical functioning, as measured by the European Organisation for Research and Treatment of Cancer Core 30-item Quality of Life questionnaire, in the Soto240 (7.95; 95% CI, 2.39-13.51) and Soto960 (6.73; 95% CI, 1.05-12.41) groups. Nearly all other measures trended toward favoring the sotorasib/panitumumab groups, but did not reach statistical significance. A similar pattern was seen in time to deterioration measures. Among adverse events, diarrhea trended toward being more frequent in the intervention arms.
At week 9, 63% of patients in Soto960 and 84% in Soto240 reported improvement in the Patient Global Impression of Change score (PGI-C), versus 37% in the chemotherapy arm. At week 17, the percentages were 77%, 59%, and 21%, respectively.
“The clinical benefits and the better quality of life outcomes associated with sotorasib at the high dose of 960 milligrams plus panitumumab establishes this combination as a potential new standard [therapy] for patients with chemorefractory KRAS G12C mutant colorectal cancer, and I think it’s quite reassuring that even if you compare two active drugs versus one active drug, this does not necessarily translate into impaired quality of life assessments by the patients,” Dr. Modest said during his presentation.
CodeBreaK 300 may point the way to other dual therapies involving kinase inhibitors, according to Rona Yaeger, MD, who wrote an accompanying editorial to the NEJM paper. Dr. Yaeger noted that clinical and preclinical studies had shown that targeted oncogenes like KRAS G12C and BRAF V600E alone would be insufficient in colorectal cancer.
When combined with KRAS G12C inhibitors, EGFR inhibitors prevent EGFR from participating in negative feedback loops that can otherwise lead to drug resistance. “Whether targeting [receptor tyrosine kinases like EGFR] in epithelial tumors other than those associated with colorectal cancers would improve the incidence of response to KRAS G12C inhibitors remains unknown,” wrote Dr. Yaeger, a medical oncologist at Memorial Sloan Kettering Cancer Center in New York. There is an ongoing clinical trial evaluating KRAS G12C inhibitors combined with EGFR antibodies in both lung and pancreatic cancer.
She noted that colorectal tumors have high levels of receptor tyrosine kinases, and argued that this will require higher doses of KRAS G12C inhibitors or novel drugs with higher activity. This is supported by the higher frequency of response and longer PFS at the higher dose in CodeBreaK 300, but could present a challenge: “Lowering the drug dose to manage toxic effects may limit the efficacy of the drug against some cancers,” she wrote.
Dr. Yaeger highlighted the KRYSTAL-10 phase 3 randomized trial, which is assessing the KRAS G12C inhibitor adagrasib in combination with the EGFR antibody cetuximab versus chemotherapy in advanced solid tumors with the KRAS G12C mutation.
“The CodeBreaK 300 trial is an exciting first step for targeting KRAS in colorectal cancer,” Dr. Yaeger wrote.
Dr. Modest has financial relationships with Amgen, AstraZeneca/MedImmune, Bristol-Myers Squibb, Incyte, Lily, Merck Serono, Merck Sharp & Dohme, Onkowissen, Pierre Fabre, Roche, and SERVIER. Dr. Yaeger has financial relationships with Amgen, Boehringer Ingelheim, Daiichi Sankyo, Mirati, Pfizer, and Zai Lab.
Dominik Modest, MD, presented these new results of the phase 3 CodeBreaK 300 trial at the 2024 ASCO Gastrointestinal Cancers Symposium.
The KRAS G12C mutation occurs in 3%-4% of metastatic colorectal cancer cases, according to Dr. Modest and the other authors of a paper published in the New England Journal of Medicine describing the primary outcome of the trial. The study included 160 patients who were randomized to once daily sotorasib (960 mg) plus panitumumab (Soto960), once daily sotorasib (240 mg) plus panitumumab (Soto240), or investigator’s choice of trifluridine–tipiracil or regorafenib.
The December 2023 paper described improvements in median progression-free survival, progression or death, and objective response (OR). The authors described statistically significant improvements in disease progression or death in the Soto960 group (hazard ratio [HR], 0.49; P = .006) and the Soto240 group (HR, 0.58; P = .03). The objective response rate was highest in the Soto960 group (26.4%; 95% CI, 15.3%-40.3%), followed by the Soto240 group (5.7%; 95% CI, 1.2%-15.7%), and the control group (0%; 95% CI, 0.0%-6.6%). Grade 3 or higher treatment-related adverse events were generally similar at 35.8% (Soto960), 30.2% (Soto240), and 43.1% (control) in each group. The most common adverse events associated with sotorasib-panitumumab were skin-related toxicity and hypomagnesemia.
The new analysis showed that both doses of sotorasib also improved patient-reported outcomes from baseline to week 8, Dr. Modest, professor of medicine at Charité University of Medicine in Berlin, said at the meeting.
Compared with the chemotherapy group, there were statistically significant differences in least square mean change from baseline to week 8 for: pain at its worst in the Soto240 group (Brief Pain Inventory [BPI], –1.18; 95% CI, –2.05 to –0.32) and the Soto960 group (BPI, –1.49; 95% CI, –2.36 to –0.61); and physical functioning, as measured by the European Organisation for Research and Treatment of Cancer Core 30-item Quality of Life questionnaire, in the Soto240 (7.95; 95% CI, 2.39-13.51) and Soto960 (6.73; 95% CI, 1.05-12.41) groups. Nearly all other measures trended toward favoring the sotorasib/panitumumab groups, but did not reach statistical significance. A similar pattern was seen in time to deterioration measures. Among adverse events, diarrhea trended toward being more frequent in the intervention arms.
At week 9, 63% of patients in Soto960 and 84% in Soto240 reported improvement in the Patient Global Impression of Change score (PGI-C), versus 37% in the chemotherapy arm. At week 17, the percentages were 77%, 59%, and 21%, respectively.
“The clinical benefits and the better quality of life outcomes associated with sotorasib at the high dose of 960 milligrams plus panitumumab establishes this combination as a potential new standard [therapy] for patients with chemorefractory KRAS G12C mutant colorectal cancer, and I think it’s quite reassuring that even if you compare two active drugs versus one active drug, this does not necessarily translate into impaired quality of life assessments by the patients,” Dr. Modest said during his presentation.
CodeBreaK 300 may point the way to other dual therapies involving kinase inhibitors, according to Rona Yaeger, MD, who wrote an accompanying editorial to the NEJM paper. Dr. Yaeger noted that clinical and preclinical studies had shown that targeted oncogenes like KRAS G12C and BRAF V600E alone would be insufficient in colorectal cancer.
When combined with KRAS G12C inhibitors, EGFR inhibitors prevent EGFR from participating in negative feedback loops that can otherwise lead to drug resistance. “Whether targeting [receptor tyrosine kinases like EGFR] in epithelial tumors other than those associated with colorectal cancers would improve the incidence of response to KRAS G12C inhibitors remains unknown,” wrote Dr. Yaeger, a medical oncologist at Memorial Sloan Kettering Cancer Center in New York. There is an ongoing clinical trial evaluating KRAS G12C inhibitors combined with EGFR antibodies in both lung and pancreatic cancer.
She noted that colorectal tumors have high levels of receptor tyrosine kinases, and argued that this will require higher doses of KRAS G12C inhibitors or novel drugs with higher activity. This is supported by the higher frequency of response and longer PFS at the higher dose in CodeBreaK 300, but could present a challenge: “Lowering the drug dose to manage toxic effects may limit the efficacy of the drug against some cancers,” she wrote.
Dr. Yaeger highlighted the KRYSTAL-10 phase 3 randomized trial, which is assessing the KRAS G12C inhibitor adagrasib in combination with the EGFR antibody cetuximab versus chemotherapy in advanced solid tumors with the KRAS G12C mutation.
“The CodeBreaK 300 trial is an exciting first step for targeting KRAS in colorectal cancer,” Dr. Yaeger wrote.
Dr. Modest has financial relationships with Amgen, AstraZeneca/MedImmune, Bristol-Myers Squibb, Incyte, Lily, Merck Serono, Merck Sharp & Dohme, Onkowissen, Pierre Fabre, Roche, and SERVIER. Dr. Yaeger has financial relationships with Amgen, Boehringer Ingelheim, Daiichi Sankyo, Mirati, Pfizer, and Zai Lab.
Dominik Modest, MD, presented these new results of the phase 3 CodeBreaK 300 trial at the 2024 ASCO Gastrointestinal Cancers Symposium.
The KRAS G12C mutation occurs in 3%-4% of metastatic colorectal cancer cases, according to Dr. Modest and the other authors of a paper published in the New England Journal of Medicine describing the primary outcome of the trial. The study included 160 patients who were randomized to once daily sotorasib (960 mg) plus panitumumab (Soto960), once daily sotorasib (240 mg) plus panitumumab (Soto240), or investigator’s choice of trifluridine–tipiracil or regorafenib.
The December 2023 paper described improvements in median progression-free survival, progression or death, and objective response (OR). The authors described statistically significant improvements in disease progression or death in the Soto960 group (hazard ratio [HR], 0.49; P = .006) and the Soto240 group (HR, 0.58; P = .03). The objective response rate was highest in the Soto960 group (26.4%; 95% CI, 15.3%-40.3%), followed by the Soto240 group (5.7%; 95% CI, 1.2%-15.7%), and the control group (0%; 95% CI, 0.0%-6.6%). Grade 3 or higher treatment-related adverse events were generally similar at 35.8% (Soto960), 30.2% (Soto240), and 43.1% (control) in each group. The most common adverse events associated with sotorasib-panitumumab were skin-related toxicity and hypomagnesemia.
The new analysis showed that both doses of sotorasib also improved patient-reported outcomes from baseline to week 8, Dr. Modest, professor of medicine at Charité University of Medicine in Berlin, said at the meeting.
Compared with the chemotherapy group, there were statistically significant differences in least square mean change from baseline to week 8 for: pain at its worst in the Soto240 group (Brief Pain Inventory [BPI], –1.18; 95% CI, –2.05 to –0.32) and the Soto960 group (BPI, –1.49; 95% CI, –2.36 to –0.61); and physical functioning, as measured by the European Organisation for Research and Treatment of Cancer Core 30-item Quality of Life questionnaire, in the Soto240 (7.95; 95% CI, 2.39-13.51) and Soto960 (6.73; 95% CI, 1.05-12.41) groups. Nearly all other measures trended toward favoring the sotorasib/panitumumab groups, but did not reach statistical significance. A similar pattern was seen in time to deterioration measures. Among adverse events, diarrhea trended toward being more frequent in the intervention arms.
At week 9, 63% of patients in Soto960 and 84% in Soto240 reported improvement in the Patient Global Impression of Change score (PGI-C), versus 37% in the chemotherapy arm. At week 17, the percentages were 77%, 59%, and 21%, respectively.
“The clinical benefits and the better quality of life outcomes associated with sotorasib at the high dose of 960 milligrams plus panitumumab establishes this combination as a potential new standard [therapy] for patients with chemorefractory KRAS G12C mutant colorectal cancer, and I think it’s quite reassuring that even if you compare two active drugs versus one active drug, this does not necessarily translate into impaired quality of life assessments by the patients,” Dr. Modest said during his presentation.
CodeBreaK 300 may point the way to other dual therapies involving kinase inhibitors, according to Rona Yaeger, MD, who wrote an accompanying editorial to the NEJM paper. Dr. Yaeger noted that clinical and preclinical studies had shown that targeted oncogenes like KRAS G12C and BRAF V600E alone would be insufficient in colorectal cancer.
When combined with KRAS G12C inhibitors, EGFR inhibitors prevent EGFR from participating in negative feedback loops that can otherwise lead to drug resistance. “Whether targeting [receptor tyrosine kinases like EGFR] in epithelial tumors other than those associated with colorectal cancers would improve the incidence of response to KRAS G12C inhibitors remains unknown,” wrote Dr. Yaeger, a medical oncologist at Memorial Sloan Kettering Cancer Center in New York. There is an ongoing clinical trial evaluating KRAS G12C inhibitors combined with EGFR antibodies in both lung and pancreatic cancer.
She noted that colorectal tumors have high levels of receptor tyrosine kinases, and argued that this will require higher doses of KRAS G12C inhibitors or novel drugs with higher activity. This is supported by the higher frequency of response and longer PFS at the higher dose in CodeBreaK 300, but could present a challenge: “Lowering the drug dose to manage toxic effects may limit the efficacy of the drug against some cancers,” she wrote.
Dr. Yaeger highlighted the KRYSTAL-10 phase 3 randomized trial, which is assessing the KRAS G12C inhibitor adagrasib in combination with the EGFR antibody cetuximab versus chemotherapy in advanced solid tumors with the KRAS G12C mutation.
“The CodeBreaK 300 trial is an exciting first step for targeting KRAS in colorectal cancer,” Dr. Yaeger wrote.
Dr. Modest has financial relationships with Amgen, AstraZeneca/MedImmune, Bristol-Myers Squibb, Incyte, Lily, Merck Serono, Merck Sharp & Dohme, Onkowissen, Pierre Fabre, Roche, and SERVIER. Dr. Yaeger has financial relationships with Amgen, Boehringer Ingelheim, Daiichi Sankyo, Mirati, Pfizer, and Zai Lab.
FROM ASCO GI
Immunotherapy Combo Wins Big on PFS in First-Line Mets CRC
SAN FRANCISCO —
Findings from the CHECKMATE-8HW trial revealed that first-line nivolumab plus ipilimumab led to a significant improvement in progression-free survival (PFS) compared with chemotherapy among patients with metastatic CRC.
More specifically, at 2 years, PFS was 72% among patients with microsatellite instability–high (MSI-H) or deficient mismatch repair (dMMR) randomized to the immunotherapy combination compared with just 14% among those randomized to chemotherapy with or without targeted therapy.
The magnitude of the benefit was unexpected, especially considering patients received only four cycles of the immunotherapy combination in the trial. “It’s a good surprise,” said lead investigator Thierry Andre, MD, who presented the findings at the 2024 ASCO Gastrointestinal Cancers Symposium.
The findings indicate that nivolumab plus ipilimumab should really be “a new standard,” said Andre, a medical oncologist at Sorbonne University, Paris.
The combination as well as nivolumab alone has received US Food and Drug Administration’s (FDA’s) approval to treat MSI-H or dMMR metastatic CRC in the second line, following chemotherapy failure.
The FDA also approved pembrolizumab as first-line monotherapy for this CRC indication in 2020. The KEYNOTE-177 trial, which led to the pembrolizumab approval, reported a 2-year PFS of 48% among patients receiving the monotherapy. Andre was the lead investigator on KEYNOTE-177.
To compare PFS results for pembrolizumab and nivolumab alone, the CHECKMATE-8HW trial included a nivolumab monotherapy arm, but these results are pending, as are the overall survival findings, Andre said.
Overall, CHECKMATE-8HW must be taken into context with KEYNOTE-177, and “we need a little bit more trial data” for oncologists to decide between the two options, said Neil Newman, MD, a radiation oncologist at the University of Texas Health Science Center, San Antonio, Texas, who co-moderated Dr. Andre’s presentation.
Andre noted, however, that if the nivolumab and pembrolizumab monotherapy results are similar, most patients will likely receive the nivolumab/ipilimumab combination, given the improved PFS outcomes.
In CHECKMATE-8HW, patients were randomized to three regimens. The 202 patients in the combination arm received nivolumab 240 mg plus ipilimumab 1 mg/kg every 3 weeks for four doses, followed by nivolumab 480 mg every 4 weeks. The 101 patients in the chemotherapy group received investigator’s choice of mFOLFOX6 or FOLFIRI with or without bevacizumab or cetuximab. And the nivolumab monotherapy arm received nivolumab 240 mg every 2 weeks for six doses, followed by nivolumab 480 mg every 4 weeks.
Treatment continued until disease progression or unacceptable toxicity over a maximum of 2 years. The median duration of treatment was 13.5 months in the nivolumab/ipilimumab arm vs 4 months in the chemotherapy arm.
PFS curves started to separate between nivolumab/ipilimumab and chemotherapy at about 3 months.
Patients receiving the combination exhibited a 79% reduction in the risk for disease progression or death at 2 years (72% vs 14%; hazard ratio, 0.21; P < .0001). The median PFS was not reached with the combination vs 5.9 months with chemotherapy. The PFS benefit of nivolumab/ipilimumab held across various subgroups, including patients with KRAS or NRAS mutations and baseline lung, liver, or peritoneal metastases.
The incidence of grade 3/4 treatment-related adverse events was 23% with nivolumab/ipilimumab vs 48% in the chemotherapy arm. The most common grade 3/4 events with nivolumab/ipilimumab were diarrhea/colitis (5%), adrenal insufficiency (4%), hepatitis (3%), and inflammation of the pituitary gland (3%).
Two treatment-related deaths occurred in the combination arm — one from pneumonitis and the second from myocarditis — and none occurred in the chemotherapy arm.
Mark A. Lewis, MD, a gastrointestinal oncologist at Intermountain Healthcare in Murray, Utah, was impressed with the CHECKMATE-8HW findings. The data are shaping up to make nivolumab/ipilimumab “the next great step in metastatic CRC management beyond KEYNOTE-177,” Dr. Lewis said.
Dr. Lewis noted that the new trial makes it “imperative” to standardize testing for immunotherapy candidacy upfront. “It is completely unacceptable for any patient with metastatic CRC to not have their MMR/MSI status assessed,” he said. “Much as no oncologist would dare treat breast cancer without testing ER, PR, HER2 status, biomarkers cannot be a later-line afterthought in stage IV CRC.”
Drugmaker Bristol-Myers Squibb told this news organization that the company will be seeking a first-line indication for the combination, and anticipates approval early next year or possibly sooner, if the FDA grants a priority review.
The work was funded by Bristol-Myers Squibb and the ONO Pharmaceutical Company. Dr. Andre had numerous industry ties, including being a consultant for both BMS and Merck. He also reported honoraria from both companies. Dr. Newman and Dr. Lewis didn’t have any disclosures.
A version of this article appeared on Medscape.com.
SAN FRANCISCO —
Findings from the CHECKMATE-8HW trial revealed that first-line nivolumab plus ipilimumab led to a significant improvement in progression-free survival (PFS) compared with chemotherapy among patients with metastatic CRC.
More specifically, at 2 years, PFS was 72% among patients with microsatellite instability–high (MSI-H) or deficient mismatch repair (dMMR) randomized to the immunotherapy combination compared with just 14% among those randomized to chemotherapy with or without targeted therapy.
The magnitude of the benefit was unexpected, especially considering patients received only four cycles of the immunotherapy combination in the trial. “It’s a good surprise,” said lead investigator Thierry Andre, MD, who presented the findings at the 2024 ASCO Gastrointestinal Cancers Symposium.
The findings indicate that nivolumab plus ipilimumab should really be “a new standard,” said Andre, a medical oncologist at Sorbonne University, Paris.
The combination as well as nivolumab alone has received US Food and Drug Administration’s (FDA’s) approval to treat MSI-H or dMMR metastatic CRC in the second line, following chemotherapy failure.
The FDA also approved pembrolizumab as first-line monotherapy for this CRC indication in 2020. The KEYNOTE-177 trial, which led to the pembrolizumab approval, reported a 2-year PFS of 48% among patients receiving the monotherapy. Andre was the lead investigator on KEYNOTE-177.
To compare PFS results for pembrolizumab and nivolumab alone, the CHECKMATE-8HW trial included a nivolumab monotherapy arm, but these results are pending, as are the overall survival findings, Andre said.
Overall, CHECKMATE-8HW must be taken into context with KEYNOTE-177, and “we need a little bit more trial data” for oncologists to decide between the two options, said Neil Newman, MD, a radiation oncologist at the University of Texas Health Science Center, San Antonio, Texas, who co-moderated Dr. Andre’s presentation.
Andre noted, however, that if the nivolumab and pembrolizumab monotherapy results are similar, most patients will likely receive the nivolumab/ipilimumab combination, given the improved PFS outcomes.
In CHECKMATE-8HW, patients were randomized to three regimens. The 202 patients in the combination arm received nivolumab 240 mg plus ipilimumab 1 mg/kg every 3 weeks for four doses, followed by nivolumab 480 mg every 4 weeks. The 101 patients in the chemotherapy group received investigator’s choice of mFOLFOX6 or FOLFIRI with or without bevacizumab or cetuximab. And the nivolumab monotherapy arm received nivolumab 240 mg every 2 weeks for six doses, followed by nivolumab 480 mg every 4 weeks.
Treatment continued until disease progression or unacceptable toxicity over a maximum of 2 years. The median duration of treatment was 13.5 months in the nivolumab/ipilimumab arm vs 4 months in the chemotherapy arm.
PFS curves started to separate between nivolumab/ipilimumab and chemotherapy at about 3 months.
Patients receiving the combination exhibited a 79% reduction in the risk for disease progression or death at 2 years (72% vs 14%; hazard ratio, 0.21; P < .0001). The median PFS was not reached with the combination vs 5.9 months with chemotherapy. The PFS benefit of nivolumab/ipilimumab held across various subgroups, including patients with KRAS or NRAS mutations and baseline lung, liver, or peritoneal metastases.
The incidence of grade 3/4 treatment-related adverse events was 23% with nivolumab/ipilimumab vs 48% in the chemotherapy arm. The most common grade 3/4 events with nivolumab/ipilimumab were diarrhea/colitis (5%), adrenal insufficiency (4%), hepatitis (3%), and inflammation of the pituitary gland (3%).
Two treatment-related deaths occurred in the combination arm — one from pneumonitis and the second from myocarditis — and none occurred in the chemotherapy arm.
Mark A. Lewis, MD, a gastrointestinal oncologist at Intermountain Healthcare in Murray, Utah, was impressed with the CHECKMATE-8HW findings. The data are shaping up to make nivolumab/ipilimumab “the next great step in metastatic CRC management beyond KEYNOTE-177,” Dr. Lewis said.
Dr. Lewis noted that the new trial makes it “imperative” to standardize testing for immunotherapy candidacy upfront. “It is completely unacceptable for any patient with metastatic CRC to not have their MMR/MSI status assessed,” he said. “Much as no oncologist would dare treat breast cancer without testing ER, PR, HER2 status, biomarkers cannot be a later-line afterthought in stage IV CRC.”
Drugmaker Bristol-Myers Squibb told this news organization that the company will be seeking a first-line indication for the combination, and anticipates approval early next year or possibly sooner, if the FDA grants a priority review.
The work was funded by Bristol-Myers Squibb and the ONO Pharmaceutical Company. Dr. Andre had numerous industry ties, including being a consultant for both BMS and Merck. He also reported honoraria from both companies. Dr. Newman and Dr. Lewis didn’t have any disclosures.
A version of this article appeared on Medscape.com.
SAN FRANCISCO —
Findings from the CHECKMATE-8HW trial revealed that first-line nivolumab plus ipilimumab led to a significant improvement in progression-free survival (PFS) compared with chemotherapy among patients with metastatic CRC.
More specifically, at 2 years, PFS was 72% among patients with microsatellite instability–high (MSI-H) or deficient mismatch repair (dMMR) randomized to the immunotherapy combination compared with just 14% among those randomized to chemotherapy with or without targeted therapy.
The magnitude of the benefit was unexpected, especially considering patients received only four cycles of the immunotherapy combination in the trial. “It’s a good surprise,” said lead investigator Thierry Andre, MD, who presented the findings at the 2024 ASCO Gastrointestinal Cancers Symposium.
The findings indicate that nivolumab plus ipilimumab should really be “a new standard,” said Andre, a medical oncologist at Sorbonne University, Paris.
The combination as well as nivolumab alone has received US Food and Drug Administration’s (FDA’s) approval to treat MSI-H or dMMR metastatic CRC in the second line, following chemotherapy failure.
The FDA also approved pembrolizumab as first-line monotherapy for this CRC indication in 2020. The KEYNOTE-177 trial, which led to the pembrolizumab approval, reported a 2-year PFS of 48% among patients receiving the monotherapy. Andre was the lead investigator on KEYNOTE-177.
To compare PFS results for pembrolizumab and nivolumab alone, the CHECKMATE-8HW trial included a nivolumab monotherapy arm, but these results are pending, as are the overall survival findings, Andre said.
Overall, CHECKMATE-8HW must be taken into context with KEYNOTE-177, and “we need a little bit more trial data” for oncologists to decide between the two options, said Neil Newman, MD, a radiation oncologist at the University of Texas Health Science Center, San Antonio, Texas, who co-moderated Dr. Andre’s presentation.
Andre noted, however, that if the nivolumab and pembrolizumab monotherapy results are similar, most patients will likely receive the nivolumab/ipilimumab combination, given the improved PFS outcomes.
In CHECKMATE-8HW, patients were randomized to three regimens. The 202 patients in the combination arm received nivolumab 240 mg plus ipilimumab 1 mg/kg every 3 weeks for four doses, followed by nivolumab 480 mg every 4 weeks. The 101 patients in the chemotherapy group received investigator’s choice of mFOLFOX6 or FOLFIRI with or without bevacizumab or cetuximab. And the nivolumab monotherapy arm received nivolumab 240 mg every 2 weeks for six doses, followed by nivolumab 480 mg every 4 weeks.
Treatment continued until disease progression or unacceptable toxicity over a maximum of 2 years. The median duration of treatment was 13.5 months in the nivolumab/ipilimumab arm vs 4 months in the chemotherapy arm.
PFS curves started to separate between nivolumab/ipilimumab and chemotherapy at about 3 months.
Patients receiving the combination exhibited a 79% reduction in the risk for disease progression or death at 2 years (72% vs 14%; hazard ratio, 0.21; P < .0001). The median PFS was not reached with the combination vs 5.9 months with chemotherapy. The PFS benefit of nivolumab/ipilimumab held across various subgroups, including patients with KRAS or NRAS mutations and baseline lung, liver, or peritoneal metastases.
The incidence of grade 3/4 treatment-related adverse events was 23% with nivolumab/ipilimumab vs 48% in the chemotherapy arm. The most common grade 3/4 events with nivolumab/ipilimumab were diarrhea/colitis (5%), adrenal insufficiency (4%), hepatitis (3%), and inflammation of the pituitary gland (3%).
Two treatment-related deaths occurred in the combination arm — one from pneumonitis and the second from myocarditis — and none occurred in the chemotherapy arm.
Mark A. Lewis, MD, a gastrointestinal oncologist at Intermountain Healthcare in Murray, Utah, was impressed with the CHECKMATE-8HW findings. The data are shaping up to make nivolumab/ipilimumab “the next great step in metastatic CRC management beyond KEYNOTE-177,” Dr. Lewis said.
Dr. Lewis noted that the new trial makes it “imperative” to standardize testing for immunotherapy candidacy upfront. “It is completely unacceptable for any patient with metastatic CRC to not have their MMR/MSI status assessed,” he said. “Much as no oncologist would dare treat breast cancer without testing ER, PR, HER2 status, biomarkers cannot be a later-line afterthought in stage IV CRC.”
Drugmaker Bristol-Myers Squibb told this news organization that the company will be seeking a first-line indication for the combination, and anticipates approval early next year or possibly sooner, if the FDA grants a priority review.
The work was funded by Bristol-Myers Squibb and the ONO Pharmaceutical Company. Dr. Andre had numerous industry ties, including being a consultant for both BMS and Merck. He also reported honoraria from both companies. Dr. Newman and Dr. Lewis didn’t have any disclosures.
A version of this article appeared on Medscape.com.
FROM ASCO-GI 2024
T-ALL: Cranial Radiotherapy Yields Little Benefit
“Overall, comparison of these cohorts provides a strong indication that CRT provides minimal benefit to patients with CNS-3 disease at diagnosis,” first author Ajay Vora, MD, a consultant hematologist with Great Ormond Street Hospital, in London, and his colleagues report in a research letter published recently in Blood Advances.
“Given the high rates of neurocognitive impairment and secondary CNS malignancies, we believe strong consideration should be given to eliminating CRT in first-line treatment for all patients with T-ALL,” they wrote.
More aggressive than B-cell ALL, T-ALL is characterized by a higher likelihood of infiltration of the CNS at diagnosis, which increases the risk of relapse after treatment.
Until recently, treatment of T-ALL long entailed CNS-directed therapy using prophylactic CRT. Now, however, due to the risks of significant toxicity, including neurocognitive defects and secondary cancers, CRT is usually either omitted or limited to key subgroups, such as those with CNS-3 disease. As an alternative, intrathecal chemotherapy is used, the authors explain.
In a 2023 study evaluating the consecutive Children’s Oncology Group (COG) AALL0434 and AALL1231 phase 3 trials of 2,164 patients with T-ALL, patients with CNS-3 at diagnosis were found to have worse outcomes, compared with CNS-1 and 2.
Importantly, the outcomes in both of those two trials were similar, despite the use of CRT in more than 90% of patients in the AALL0434 trial--but in only 10% of patients AALL1231 trial (mainly those with CNS-3 and at high-risk). These outcomes suggested that CRT can safely be eliminated for CNS-1 and 2 patients.
With CRT used in both trials among patients with CNS-3, conclusions about eliminating CRT among those patients could not be drawn. However, with other large groups (including the Dutch Childhood Oncology Group), eliminating CRT in the frontline treatment of all patients with T-ALL, including those with CNS-3, is what Dr. Vora and colleagues sought to further investigate.
For the current study, they evaluated outcomes in the UKALL2003 and UKALL2011 trials conducted by the UK National Cancer Research Institute, in which CRT was eliminated for all patients — including those with CNS-3 — and compared them with the COG AALL0434 and AALL1231 trials.
In the UK trials, involving 665 patients with T-ALL aged 1 to 24, treatment included a dexamethasone-based backbone chemotherapy consisting of a 4-drug induction, Berlin-Frankfurt-Münster (BFM) consolidation, interim maintenance, delayed intensification, and maintenance therapy, with the treatment stratified based on morphological early response and minimal residual disease at the end of induction.
While the UKALL2003 trial initially recommended CRT for patients with CNS-3, that practice ended in 2009, and CNS-directed therapy subsequently consisted of intrathecal methotrexate (MTX) at regular intervals throughout treatment. Additional weekly intrathecal MTX treatments were recommended throughout induction for patients with CNS-3.
In the UKALL2011 trial, the weekly intrathecal MTX treatments were recommended for patients with CNS-2, as well as CNS-3.
Overall, among those with CNS data available, 557 patients had CNS-1 (87.4%), 44 CNS-2 (6.9%), and 36 CNS-3 (5.7%).
For the outcomes of 4-year cumulative incidence of relapse (CIR), event-free survival (EFS) and overall survival (OS) in the combined cohort of the 2 UK trials, there were no significant differences between CNS-1, 2 or 3 groups.
Specifically, the mean rates of 4-year CIR in the CNS-1, 2, and 3 groups were 13.6%, 25.9% and 24.6%, respectively (P = .241); mean EFS rates were 82.9%, 74.1% and 77.8% (P = .623), and OS rates were 88.6%, 80.9% and 91.8%, (P = .453).
“Most importantly, outcomes are not significantly different for the patients with CNS-3, despite omission of CRT in the UK cohort,” the authors underscored.
Comparatively, in the cohort of the 2 COG trials, there were significant differences based on CNS status for 4-year CIR (P = .0002); EFS (P = .0004) and OS (P = .005).
The 4-year relapse rates among those with CNS-3 in the UK cohort were slightly higher compared with those in the COG cohort (24.6% UK vs 17.9%, COG). However, the difference did not translate to poorer long-term survival in the UK cohort (91.8% vs 82.7%, respectively).
Those findings are consistent with a previous meta-analysis that Dr. Vora and his colleagues conducted of more than 16,000 patients with mainly B-cell ALL, which showed that CRT reduced the risk of isolated and combined CNS relapse in patients with CNS-3. However, that risk had no impact on EFS and OS.
Of note, patients in the UK cohort with CNS-2 had worse outcomes compared with the COG group, with double the rate of relapse and lower EFS and OS. However, the authors speculate that factors including a lower proportion of patients with CNS-2 in the UK cohort and differences in methodologies may explain those different outcomes and may preclude their generalizability to other groups.
Overall, “these findings corroborate those of earlier studies that CRT has marginal, if any benefit, for any sub-group of ALL, especially as part of contemporary treatment,” Dr. Vora said in an interview.
In terms of therapies that do appear to make a difference in the treatment of CNS-3, Dr. Vora noted that the addition of nelarabine in the COG AALL0434 trial showed “remarkable benefit” in the CNS-3 group, with a 93.1% rate of disease-free survival in those patients versus 70.2% without nelarabine.
Importantly, those patients did also receive CRT. However, Dr. Vora and colleagues underscore that “the improvement is impressive and raises the question of whether nelarabine would have a similar beneficial effect in the absence of CRT.”
In an editorial published with the COG trials, Josep-Maria Ribera, MD, of the Josep Carreras Leukemia Research Institute, in Barcelona, Spain, agrees that “better approaches clearly are needed to treat CNS-3 T-ALL, especially if omission of CRT is a priority.”
Noting the improvements observed with nelarabine, as well as Capizzi escalating-dose methotrexate (C-MTX), and dexamethasone in reducing the risk of CNS relapse, he speculates that “it is possible that the additional use of C-MTX and induction dexamethasone could eliminate the need for CRT in these patients.”
The authors and Dr. Ribera had no disclosures to report.
“Overall, comparison of these cohorts provides a strong indication that CRT provides minimal benefit to patients with CNS-3 disease at diagnosis,” first author Ajay Vora, MD, a consultant hematologist with Great Ormond Street Hospital, in London, and his colleagues report in a research letter published recently in Blood Advances.
“Given the high rates of neurocognitive impairment and secondary CNS malignancies, we believe strong consideration should be given to eliminating CRT in first-line treatment for all patients with T-ALL,” they wrote.
More aggressive than B-cell ALL, T-ALL is characterized by a higher likelihood of infiltration of the CNS at diagnosis, which increases the risk of relapse after treatment.
Until recently, treatment of T-ALL long entailed CNS-directed therapy using prophylactic CRT. Now, however, due to the risks of significant toxicity, including neurocognitive defects and secondary cancers, CRT is usually either omitted or limited to key subgroups, such as those with CNS-3 disease. As an alternative, intrathecal chemotherapy is used, the authors explain.
In a 2023 study evaluating the consecutive Children’s Oncology Group (COG) AALL0434 and AALL1231 phase 3 trials of 2,164 patients with T-ALL, patients with CNS-3 at diagnosis were found to have worse outcomes, compared with CNS-1 and 2.
Importantly, the outcomes in both of those two trials were similar, despite the use of CRT in more than 90% of patients in the AALL0434 trial--but in only 10% of patients AALL1231 trial (mainly those with CNS-3 and at high-risk). These outcomes suggested that CRT can safely be eliminated for CNS-1 and 2 patients.
With CRT used in both trials among patients with CNS-3, conclusions about eliminating CRT among those patients could not be drawn. However, with other large groups (including the Dutch Childhood Oncology Group), eliminating CRT in the frontline treatment of all patients with T-ALL, including those with CNS-3, is what Dr. Vora and colleagues sought to further investigate.
For the current study, they evaluated outcomes in the UKALL2003 and UKALL2011 trials conducted by the UK National Cancer Research Institute, in which CRT was eliminated for all patients — including those with CNS-3 — and compared them with the COG AALL0434 and AALL1231 trials.
In the UK trials, involving 665 patients with T-ALL aged 1 to 24, treatment included a dexamethasone-based backbone chemotherapy consisting of a 4-drug induction, Berlin-Frankfurt-Münster (BFM) consolidation, interim maintenance, delayed intensification, and maintenance therapy, with the treatment stratified based on morphological early response and minimal residual disease at the end of induction.
While the UKALL2003 trial initially recommended CRT for patients with CNS-3, that practice ended in 2009, and CNS-directed therapy subsequently consisted of intrathecal methotrexate (MTX) at regular intervals throughout treatment. Additional weekly intrathecal MTX treatments were recommended throughout induction for patients with CNS-3.
In the UKALL2011 trial, the weekly intrathecal MTX treatments were recommended for patients with CNS-2, as well as CNS-3.
Overall, among those with CNS data available, 557 patients had CNS-1 (87.4%), 44 CNS-2 (6.9%), and 36 CNS-3 (5.7%).
For the outcomes of 4-year cumulative incidence of relapse (CIR), event-free survival (EFS) and overall survival (OS) in the combined cohort of the 2 UK trials, there were no significant differences between CNS-1, 2 or 3 groups.
Specifically, the mean rates of 4-year CIR in the CNS-1, 2, and 3 groups were 13.6%, 25.9% and 24.6%, respectively (P = .241); mean EFS rates were 82.9%, 74.1% and 77.8% (P = .623), and OS rates were 88.6%, 80.9% and 91.8%, (P = .453).
“Most importantly, outcomes are not significantly different for the patients with CNS-3, despite omission of CRT in the UK cohort,” the authors underscored.
Comparatively, in the cohort of the 2 COG trials, there were significant differences based on CNS status for 4-year CIR (P = .0002); EFS (P = .0004) and OS (P = .005).
The 4-year relapse rates among those with CNS-3 in the UK cohort were slightly higher compared with those in the COG cohort (24.6% UK vs 17.9%, COG). However, the difference did not translate to poorer long-term survival in the UK cohort (91.8% vs 82.7%, respectively).
Those findings are consistent with a previous meta-analysis that Dr. Vora and his colleagues conducted of more than 16,000 patients with mainly B-cell ALL, which showed that CRT reduced the risk of isolated and combined CNS relapse in patients with CNS-3. However, that risk had no impact on EFS and OS.
Of note, patients in the UK cohort with CNS-2 had worse outcomes compared with the COG group, with double the rate of relapse and lower EFS and OS. However, the authors speculate that factors including a lower proportion of patients with CNS-2 in the UK cohort and differences in methodologies may explain those different outcomes and may preclude their generalizability to other groups.
Overall, “these findings corroborate those of earlier studies that CRT has marginal, if any benefit, for any sub-group of ALL, especially as part of contemporary treatment,” Dr. Vora said in an interview.
In terms of therapies that do appear to make a difference in the treatment of CNS-3, Dr. Vora noted that the addition of nelarabine in the COG AALL0434 trial showed “remarkable benefit” in the CNS-3 group, with a 93.1% rate of disease-free survival in those patients versus 70.2% without nelarabine.
Importantly, those patients did also receive CRT. However, Dr. Vora and colleagues underscore that “the improvement is impressive and raises the question of whether nelarabine would have a similar beneficial effect in the absence of CRT.”
In an editorial published with the COG trials, Josep-Maria Ribera, MD, of the Josep Carreras Leukemia Research Institute, in Barcelona, Spain, agrees that “better approaches clearly are needed to treat CNS-3 T-ALL, especially if omission of CRT is a priority.”
Noting the improvements observed with nelarabine, as well as Capizzi escalating-dose methotrexate (C-MTX), and dexamethasone in reducing the risk of CNS relapse, he speculates that “it is possible that the additional use of C-MTX and induction dexamethasone could eliminate the need for CRT in these patients.”
The authors and Dr. Ribera had no disclosures to report.
“Overall, comparison of these cohorts provides a strong indication that CRT provides minimal benefit to patients with CNS-3 disease at diagnosis,” first author Ajay Vora, MD, a consultant hematologist with Great Ormond Street Hospital, in London, and his colleagues report in a research letter published recently in Blood Advances.
“Given the high rates of neurocognitive impairment and secondary CNS malignancies, we believe strong consideration should be given to eliminating CRT in first-line treatment for all patients with T-ALL,” they wrote.
More aggressive than B-cell ALL, T-ALL is characterized by a higher likelihood of infiltration of the CNS at diagnosis, which increases the risk of relapse after treatment.
Until recently, treatment of T-ALL long entailed CNS-directed therapy using prophylactic CRT. Now, however, due to the risks of significant toxicity, including neurocognitive defects and secondary cancers, CRT is usually either omitted or limited to key subgroups, such as those with CNS-3 disease. As an alternative, intrathecal chemotherapy is used, the authors explain.
In a 2023 study evaluating the consecutive Children’s Oncology Group (COG) AALL0434 and AALL1231 phase 3 trials of 2,164 patients with T-ALL, patients with CNS-3 at diagnosis were found to have worse outcomes, compared with CNS-1 and 2.
Importantly, the outcomes in both of those two trials were similar, despite the use of CRT in more than 90% of patients in the AALL0434 trial--but in only 10% of patients AALL1231 trial (mainly those with CNS-3 and at high-risk). These outcomes suggested that CRT can safely be eliminated for CNS-1 and 2 patients.
With CRT used in both trials among patients with CNS-3, conclusions about eliminating CRT among those patients could not be drawn. However, with other large groups (including the Dutch Childhood Oncology Group), eliminating CRT in the frontline treatment of all patients with T-ALL, including those with CNS-3, is what Dr. Vora and colleagues sought to further investigate.
For the current study, they evaluated outcomes in the UKALL2003 and UKALL2011 trials conducted by the UK National Cancer Research Institute, in which CRT was eliminated for all patients — including those with CNS-3 — and compared them with the COG AALL0434 and AALL1231 trials.
In the UK trials, involving 665 patients with T-ALL aged 1 to 24, treatment included a dexamethasone-based backbone chemotherapy consisting of a 4-drug induction, Berlin-Frankfurt-Münster (BFM) consolidation, interim maintenance, delayed intensification, and maintenance therapy, with the treatment stratified based on morphological early response and minimal residual disease at the end of induction.
While the UKALL2003 trial initially recommended CRT for patients with CNS-3, that practice ended in 2009, and CNS-directed therapy subsequently consisted of intrathecal methotrexate (MTX) at regular intervals throughout treatment. Additional weekly intrathecal MTX treatments were recommended throughout induction for patients with CNS-3.
In the UKALL2011 trial, the weekly intrathecal MTX treatments were recommended for patients with CNS-2, as well as CNS-3.
Overall, among those with CNS data available, 557 patients had CNS-1 (87.4%), 44 CNS-2 (6.9%), and 36 CNS-3 (5.7%).
For the outcomes of 4-year cumulative incidence of relapse (CIR), event-free survival (EFS) and overall survival (OS) in the combined cohort of the 2 UK trials, there were no significant differences between CNS-1, 2 or 3 groups.
Specifically, the mean rates of 4-year CIR in the CNS-1, 2, and 3 groups were 13.6%, 25.9% and 24.6%, respectively (P = .241); mean EFS rates were 82.9%, 74.1% and 77.8% (P = .623), and OS rates were 88.6%, 80.9% and 91.8%, (P = .453).
“Most importantly, outcomes are not significantly different for the patients with CNS-3, despite omission of CRT in the UK cohort,” the authors underscored.
Comparatively, in the cohort of the 2 COG trials, there were significant differences based on CNS status for 4-year CIR (P = .0002); EFS (P = .0004) and OS (P = .005).
The 4-year relapse rates among those with CNS-3 in the UK cohort were slightly higher compared with those in the COG cohort (24.6% UK vs 17.9%, COG). However, the difference did not translate to poorer long-term survival in the UK cohort (91.8% vs 82.7%, respectively).
Those findings are consistent with a previous meta-analysis that Dr. Vora and his colleagues conducted of more than 16,000 patients with mainly B-cell ALL, which showed that CRT reduced the risk of isolated and combined CNS relapse in patients with CNS-3. However, that risk had no impact on EFS and OS.
Of note, patients in the UK cohort with CNS-2 had worse outcomes compared with the COG group, with double the rate of relapse and lower EFS and OS. However, the authors speculate that factors including a lower proportion of patients with CNS-2 in the UK cohort and differences in methodologies may explain those different outcomes and may preclude their generalizability to other groups.
Overall, “these findings corroborate those of earlier studies that CRT has marginal, if any benefit, for any sub-group of ALL, especially as part of contemporary treatment,” Dr. Vora said in an interview.
In terms of therapies that do appear to make a difference in the treatment of CNS-3, Dr. Vora noted that the addition of nelarabine in the COG AALL0434 trial showed “remarkable benefit” in the CNS-3 group, with a 93.1% rate of disease-free survival in those patients versus 70.2% without nelarabine.
Importantly, those patients did also receive CRT. However, Dr. Vora and colleagues underscore that “the improvement is impressive and raises the question of whether nelarabine would have a similar beneficial effect in the absence of CRT.”
In an editorial published with the COG trials, Josep-Maria Ribera, MD, of the Josep Carreras Leukemia Research Institute, in Barcelona, Spain, agrees that “better approaches clearly are needed to treat CNS-3 T-ALL, especially if omission of CRT is a priority.”
Noting the improvements observed with nelarabine, as well as Capizzi escalating-dose methotrexate (C-MTX), and dexamethasone in reducing the risk of CNS relapse, he speculates that “it is possible that the additional use of C-MTX and induction dexamethasone could eliminate the need for CRT in these patients.”
The authors and Dr. Ribera had no disclosures to report.
FROM BLOOD ADVANCES
Positive Phase 3 Results for Novel Antipsychotic in Schizophrenia
in the phase 3 EMERGENT-2 trial, a new study shows.
Xanomeline-trospium treatment was not associated with weight gain compared with placebo, and the incidences of extrapyramidal motor symptoms or akathisia were low and similar between treatment groups.
The EMERGENT-2 results “support the potential for KarXT to represent a new class of effective and well-tolerated antipsychotic medicines based on activating muscarinic receptors, not the D2 dopamine receptor-blocking mechanism of all current antipsychotic medications,” write the authors, led by Inder Kaul, MD, with Karuna Therapeutics, Boston, Massachusetts.
The US Food and Drug Administration has accepted the company’s new drug application for KarXT for the treatment of schizophrenia in adults. The Prescription Drug User Fee Act action date is September 26, 2024.
Results of the EMERGENT-2 trial were published online on December 14, 2023, in The Lancet.
Beyond the Dopamine System
Evidence suggests the muscarinic cholinergic system is involved in the pathophysiology of schizophrenia.
Xanomeline is an oral muscarinic cholinergic receptor agonist that does not have direct effects on the dopamine receptor. Combining it with trospium chloride, an oral pan-muscarinic receptor antagonist, is thought to reduce side effects associated with xanomeline’s activation of peripheral muscarinic receptors in peripheral tissues.
EMERGENT-2 was a multicenter, double-blind, placebo-controlled trial that enrolled 252 adults with schizophrenia who recently experienced a worsening of psychotic symptoms warranting hospitalization.
Patients were treated for 5 weeks, with xanomeline-trospium titrated from 50 mg/20 mg twice daily to 125 mg/30 mg twice daily. Efficacy and safety analyses were conducted in those who had received at least one dose of the study drug.
The primary endpoint was change in baseline to week 5 in Positive and Negative Syndrome Scale (PANSS) total score (range, 30-210, with higher scores indicating more severe symptoms).
At the end of the treatment period, xanomeline-trospium was associated with a significant 9.6-point reduction in PANSS total scores relative to placebo. PANSS total scores fell by 21.2 points with xanomeline-trospium vs 11.6 points with placebo (P < .0001; Cohen d effect size, 0.61).
All secondary endpoints were also met, with active treatment demonstrating statistically significant reductions compared with placebo at week 5 (P < .05).
These secondary endpoints included change in PANSS positive subscale, PANSS negative subscale, PANSS Marder negative factor, Clinical Global Impression-Severity score, and percentage of participants achieving at least a 30% reduction from baseline to week 5 in PANSS total score.
Rates of discontinuation related to side effects were similar with active treatment and placebo (7% and 6%, respectively). The most common side effects with xanomeline-trospium were constipation (21%), dyspepsia (19%), nausea (19%), vomiting (14%), headache (14%), hypertension (10%), dizziness (9%), and gastroesophageal reflux disease (6%).
Xanomeline-trospium demonstrated a “distinctive safety and tolerability profile and was not associated with many of the adverse events typically associated with current antipsychotic treatments, including extrapyramidal motor symptoms, weight gain, changes in lipid and glucose parameters, and somnolence,” the authors report.
Potential ‘Game-Changer’
Xanomeline-trospium is a potential “game-changer” for patients with schizophrenia, Ann Shinn, MD, MPH, director of clinical research, Schizophrenia and Bipolar Disorder Research Program, McLean Hospital, and assistant professor of psychiatry, Harvard Medical School, told this news organization.
There was a “clear separation between the people who were randomized to KarXT vs placebo. It’s not just a statistically significant but also a clinically significant difference in the reduction in symptoms of psychosis,” said Dr. Shinn, who wasn’t involved in the study.
“What’s really exciting” is that the drug did not cause weight gain or extrapyramidal symptoms compared with placebo. “Both from an efficacy and side-effect perspective, I think more patients with schizophrenia are going to be willing to take medication,” Dr. Shinn noted.
Also commenting on this research for this news organization, René Kahn, MD, PhD, professor and chair of psychiatry at the Icahn School of Medicine at Mount Sinai in New York, noted that current antipsychotic medications for schizophrenia work “directly on the dopamine system — either as dopamine antagonists or partial agonist.”
Xanomeline-trospium provides a “new mechanism of action, a new system that’s being targeted in the treatment of schizophrenia, and the effect size was rather large, so the drug didn’t just squeak by,” Dr. Kahn said.
Nonetheless, “we’ll have to wait and see whether it’s as effective or more effective than drugs currently on the market. The proof of the pudding will come when it’s marketed and used on thousands and thousands of patients,” Dr. Kahn added.
The coauthors of an accompanying commentary say the EMERGENT-2 findings “strongly support the possibility that agonism of muscarinic receptors provides the first viable antipsychotic alternative to blocking the dopamine D2 receptor for more than 70 years, and as such encourage further research.”
However, as a regulatory trial, EMERGENT-2 does not provide comparative data on the benefits and harms of KarXT with existing alternatives.
This represents a “missed opportunity to provide patients and clinicians with the information that is clinically needed — what is the treatment of choice for a patient?” writes Andrea Cipriani, MD, PhD, with the Department of Psychiatry, University of Oxford, United Kingdom, and co-authors.
The study was funded by Karuna Therapeutics. Several authors disclosed relationships with the company. Dr. Kahn disclosed various relationships with Boehringer Ingelheim International GmbH. Dr. Cipriani received research, educational, and consultancy fees from the Italian Network for Paediatric Trials, the CARIPLO Foundation, Lundbeck, and Angelini Pharma and was chief investigator of one trial about seltorexant in adolescent depression, sponsored by Janssen. Dr. Shinn had no relevant disclosures.
A version of this article appeared on Medscape.com.
in the phase 3 EMERGENT-2 trial, a new study shows.
Xanomeline-trospium treatment was not associated with weight gain compared with placebo, and the incidences of extrapyramidal motor symptoms or akathisia were low and similar between treatment groups.
The EMERGENT-2 results “support the potential for KarXT to represent a new class of effective and well-tolerated antipsychotic medicines based on activating muscarinic receptors, not the D2 dopamine receptor-blocking mechanism of all current antipsychotic medications,” write the authors, led by Inder Kaul, MD, with Karuna Therapeutics, Boston, Massachusetts.
The US Food and Drug Administration has accepted the company’s new drug application for KarXT for the treatment of schizophrenia in adults. The Prescription Drug User Fee Act action date is September 26, 2024.
Results of the EMERGENT-2 trial were published online on December 14, 2023, in The Lancet.
Beyond the Dopamine System
Evidence suggests the muscarinic cholinergic system is involved in the pathophysiology of schizophrenia.
Xanomeline is an oral muscarinic cholinergic receptor agonist that does not have direct effects on the dopamine receptor. Combining it with trospium chloride, an oral pan-muscarinic receptor antagonist, is thought to reduce side effects associated with xanomeline’s activation of peripheral muscarinic receptors in peripheral tissues.
EMERGENT-2 was a multicenter, double-blind, placebo-controlled trial that enrolled 252 adults with schizophrenia who recently experienced a worsening of psychotic symptoms warranting hospitalization.
Patients were treated for 5 weeks, with xanomeline-trospium titrated from 50 mg/20 mg twice daily to 125 mg/30 mg twice daily. Efficacy and safety analyses were conducted in those who had received at least one dose of the study drug.
The primary endpoint was change in baseline to week 5 in Positive and Negative Syndrome Scale (PANSS) total score (range, 30-210, with higher scores indicating more severe symptoms).
At the end of the treatment period, xanomeline-trospium was associated with a significant 9.6-point reduction in PANSS total scores relative to placebo. PANSS total scores fell by 21.2 points with xanomeline-trospium vs 11.6 points with placebo (P < .0001; Cohen d effect size, 0.61).
All secondary endpoints were also met, with active treatment demonstrating statistically significant reductions compared with placebo at week 5 (P < .05).
These secondary endpoints included change in PANSS positive subscale, PANSS negative subscale, PANSS Marder negative factor, Clinical Global Impression-Severity score, and percentage of participants achieving at least a 30% reduction from baseline to week 5 in PANSS total score.
Rates of discontinuation related to side effects were similar with active treatment and placebo (7% and 6%, respectively). The most common side effects with xanomeline-trospium were constipation (21%), dyspepsia (19%), nausea (19%), vomiting (14%), headache (14%), hypertension (10%), dizziness (9%), and gastroesophageal reflux disease (6%).
Xanomeline-trospium demonstrated a “distinctive safety and tolerability profile and was not associated with many of the adverse events typically associated with current antipsychotic treatments, including extrapyramidal motor symptoms, weight gain, changes in lipid and glucose parameters, and somnolence,” the authors report.
Potential ‘Game-Changer’
Xanomeline-trospium is a potential “game-changer” for patients with schizophrenia, Ann Shinn, MD, MPH, director of clinical research, Schizophrenia and Bipolar Disorder Research Program, McLean Hospital, and assistant professor of psychiatry, Harvard Medical School, told this news organization.
There was a “clear separation between the people who were randomized to KarXT vs placebo. It’s not just a statistically significant but also a clinically significant difference in the reduction in symptoms of psychosis,” said Dr. Shinn, who wasn’t involved in the study.
“What’s really exciting” is that the drug did not cause weight gain or extrapyramidal symptoms compared with placebo. “Both from an efficacy and side-effect perspective, I think more patients with schizophrenia are going to be willing to take medication,” Dr. Shinn noted.
Also commenting on this research for this news organization, René Kahn, MD, PhD, professor and chair of psychiatry at the Icahn School of Medicine at Mount Sinai in New York, noted that current antipsychotic medications for schizophrenia work “directly on the dopamine system — either as dopamine antagonists or partial agonist.”
Xanomeline-trospium provides a “new mechanism of action, a new system that’s being targeted in the treatment of schizophrenia, and the effect size was rather large, so the drug didn’t just squeak by,” Dr. Kahn said.
Nonetheless, “we’ll have to wait and see whether it’s as effective or more effective than drugs currently on the market. The proof of the pudding will come when it’s marketed and used on thousands and thousands of patients,” Dr. Kahn added.
The coauthors of an accompanying commentary say the EMERGENT-2 findings “strongly support the possibility that agonism of muscarinic receptors provides the first viable antipsychotic alternative to blocking the dopamine D2 receptor for more than 70 years, and as such encourage further research.”
However, as a regulatory trial, EMERGENT-2 does not provide comparative data on the benefits and harms of KarXT with existing alternatives.
This represents a “missed opportunity to provide patients and clinicians with the information that is clinically needed — what is the treatment of choice for a patient?” writes Andrea Cipriani, MD, PhD, with the Department of Psychiatry, University of Oxford, United Kingdom, and co-authors.
The study was funded by Karuna Therapeutics. Several authors disclosed relationships with the company. Dr. Kahn disclosed various relationships with Boehringer Ingelheim International GmbH. Dr. Cipriani received research, educational, and consultancy fees from the Italian Network for Paediatric Trials, the CARIPLO Foundation, Lundbeck, and Angelini Pharma and was chief investigator of one trial about seltorexant in adolescent depression, sponsored by Janssen. Dr. Shinn had no relevant disclosures.
A version of this article appeared on Medscape.com.
in the phase 3 EMERGENT-2 trial, a new study shows.
Xanomeline-trospium treatment was not associated with weight gain compared with placebo, and the incidences of extrapyramidal motor symptoms or akathisia were low and similar between treatment groups.
The EMERGENT-2 results “support the potential for KarXT to represent a new class of effective and well-tolerated antipsychotic medicines based on activating muscarinic receptors, not the D2 dopamine receptor-blocking mechanism of all current antipsychotic medications,” write the authors, led by Inder Kaul, MD, with Karuna Therapeutics, Boston, Massachusetts.
The US Food and Drug Administration has accepted the company’s new drug application for KarXT for the treatment of schizophrenia in adults. The Prescription Drug User Fee Act action date is September 26, 2024.
Results of the EMERGENT-2 trial were published online on December 14, 2023, in The Lancet.
Beyond the Dopamine System
Evidence suggests the muscarinic cholinergic system is involved in the pathophysiology of schizophrenia.
Xanomeline is an oral muscarinic cholinergic receptor agonist that does not have direct effects on the dopamine receptor. Combining it with trospium chloride, an oral pan-muscarinic receptor antagonist, is thought to reduce side effects associated with xanomeline’s activation of peripheral muscarinic receptors in peripheral tissues.
EMERGENT-2 was a multicenter, double-blind, placebo-controlled trial that enrolled 252 adults with schizophrenia who recently experienced a worsening of psychotic symptoms warranting hospitalization.
Patients were treated for 5 weeks, with xanomeline-trospium titrated from 50 mg/20 mg twice daily to 125 mg/30 mg twice daily. Efficacy and safety analyses were conducted in those who had received at least one dose of the study drug.
The primary endpoint was change in baseline to week 5 in Positive and Negative Syndrome Scale (PANSS) total score (range, 30-210, with higher scores indicating more severe symptoms).
At the end of the treatment period, xanomeline-trospium was associated with a significant 9.6-point reduction in PANSS total scores relative to placebo. PANSS total scores fell by 21.2 points with xanomeline-trospium vs 11.6 points with placebo (P < .0001; Cohen d effect size, 0.61).
All secondary endpoints were also met, with active treatment demonstrating statistically significant reductions compared with placebo at week 5 (P < .05).
These secondary endpoints included change in PANSS positive subscale, PANSS negative subscale, PANSS Marder negative factor, Clinical Global Impression-Severity score, and percentage of participants achieving at least a 30% reduction from baseline to week 5 in PANSS total score.
Rates of discontinuation related to side effects were similar with active treatment and placebo (7% and 6%, respectively). The most common side effects with xanomeline-trospium were constipation (21%), dyspepsia (19%), nausea (19%), vomiting (14%), headache (14%), hypertension (10%), dizziness (9%), and gastroesophageal reflux disease (6%).
Xanomeline-trospium demonstrated a “distinctive safety and tolerability profile and was not associated with many of the adverse events typically associated with current antipsychotic treatments, including extrapyramidal motor symptoms, weight gain, changes in lipid and glucose parameters, and somnolence,” the authors report.
Potential ‘Game-Changer’
Xanomeline-trospium is a potential “game-changer” for patients with schizophrenia, Ann Shinn, MD, MPH, director of clinical research, Schizophrenia and Bipolar Disorder Research Program, McLean Hospital, and assistant professor of psychiatry, Harvard Medical School, told this news organization.
There was a “clear separation between the people who were randomized to KarXT vs placebo. It’s not just a statistically significant but also a clinically significant difference in the reduction in symptoms of psychosis,” said Dr. Shinn, who wasn’t involved in the study.
“What’s really exciting” is that the drug did not cause weight gain or extrapyramidal symptoms compared with placebo. “Both from an efficacy and side-effect perspective, I think more patients with schizophrenia are going to be willing to take medication,” Dr. Shinn noted.
Also commenting on this research for this news organization, René Kahn, MD, PhD, professor and chair of psychiatry at the Icahn School of Medicine at Mount Sinai in New York, noted that current antipsychotic medications for schizophrenia work “directly on the dopamine system — either as dopamine antagonists or partial agonist.”
Xanomeline-trospium provides a “new mechanism of action, a new system that’s being targeted in the treatment of schizophrenia, and the effect size was rather large, so the drug didn’t just squeak by,” Dr. Kahn said.
Nonetheless, “we’ll have to wait and see whether it’s as effective or more effective than drugs currently on the market. The proof of the pudding will come when it’s marketed and used on thousands and thousands of patients,” Dr. Kahn added.
The coauthors of an accompanying commentary say the EMERGENT-2 findings “strongly support the possibility that agonism of muscarinic receptors provides the first viable antipsychotic alternative to blocking the dopamine D2 receptor for more than 70 years, and as such encourage further research.”
However, as a regulatory trial, EMERGENT-2 does not provide comparative data on the benefits and harms of KarXT with existing alternatives.
This represents a “missed opportunity to provide patients and clinicians with the information that is clinically needed — what is the treatment of choice for a patient?” writes Andrea Cipriani, MD, PhD, with the Department of Psychiatry, University of Oxford, United Kingdom, and co-authors.
The study was funded by Karuna Therapeutics. Several authors disclosed relationships with the company. Dr. Kahn disclosed various relationships with Boehringer Ingelheim International GmbH. Dr. Cipriani received research, educational, and consultancy fees from the Italian Network for Paediatric Trials, the CARIPLO Foundation, Lundbeck, and Angelini Pharma and was chief investigator of one trial about seltorexant in adolescent depression, sponsored by Janssen. Dr. Shinn had no relevant disclosures.
A version of this article appeared on Medscape.com.
Deaths Linked to Substance Use, CVD on the Rise
TOPLINE:
, with the most pronounced rise among women, American Indians, younger people, rural residents, and users of cannabis and psychostimulants, results of new research suggest.
METHODOLOGY:
- From the Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research (CDC WONDER) database and using International Classification of Diseases (ICD) codes, researchers collected data on deaths within the United States where both SU and CVD (SU+CVD) were a contributing or an underlying cause and gathered information on location of death (medical facility, home, hospice, nursing home/long-term care facility), demographics (sex, race/ethnicity, age), and region (urban-rural, state).
- Researchers determined crude and age-adjusted mortality rates (AAMRs) per 100,000 population, identified trends in AAMR using annual percent change (APC) and calculated the weighted average of APCs (AAPCs).
- Between 1999 and 2019, there were 636,572 deaths related to CVD+SU, 75.6% of which were among men and 70.6% among non-Hispanic White individuals, with 65% related to alcohol, and where location of death was available, 47.7% occurred in medical facilities.
TAKEAWAY:
- The overall SU+CVD-related AAMR from 1999 to 2019 was 14.3 (95% CI, 14.3-14.3) per 100,000 individuals, with the rate being higher in men (22.5) than in women (6.8) and highest in American Indians or Alaska Natives (37.7) compared with other races/ethnicities.
- Rural areas had higher SU+CVD-related AAMR (15.2; 95% CI, 15.1-15.3) than urban areas, with the District of Columbia having the highest AAMR geographically (25.4), individuals aged 55-69 years having the highest rate agewise (25.1), and alcohol accounting for the highest rate (9.09) among substance types.
- Temporal trends show that the overall SU+CVD-related AAMR increased from 9.9 in 1999 to 21.4 in 2019, a rate that started accelerating in 2012, with an AAPC of 4.0% (95% CI, 3.7-4.3); increases were across all ethnicities and age groups and were particularly pronounced among women (4.8%; 95% CI, 4.5-5.1).
- Cannabis had the highest AAPC of all substances (12.7%), but stimulants had an APC of 21.4 (95% CI, 20.0-22.8) from 2009 to 2019, a period during which stimulants were the fastest-growing substance abuse category.
IN PRACTICE:
These new results identify high-risk groups, which “is crucial for prioritizing preventive measures aiming to reduce substance use and cardiovascular disease-related mortality in these populations,” the researchers wrote.
SOURCE:
Abdul Mannan Khan Minhas, MD, Department of Medicine, University of Mississippi Medical Center, Jackson, Mississippi, and Jakrin Kewcharoen, MD, Division of Cardiology, Loma Linda University Medical Center, Loma Linda, California, were co-first authors of the study, which was published online in the Journal of the American Heart Association.
A version of this article first appeared on Medscape.com.
TOPLINE:
, with the most pronounced rise among women, American Indians, younger people, rural residents, and users of cannabis and psychostimulants, results of new research suggest.
METHODOLOGY:
- From the Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research (CDC WONDER) database and using International Classification of Diseases (ICD) codes, researchers collected data on deaths within the United States where both SU and CVD (SU+CVD) were a contributing or an underlying cause and gathered information on location of death (medical facility, home, hospice, nursing home/long-term care facility), demographics (sex, race/ethnicity, age), and region (urban-rural, state).
- Researchers determined crude and age-adjusted mortality rates (AAMRs) per 100,000 population, identified trends in AAMR using annual percent change (APC) and calculated the weighted average of APCs (AAPCs).
- Between 1999 and 2019, there were 636,572 deaths related to CVD+SU, 75.6% of which were among men and 70.6% among non-Hispanic White individuals, with 65% related to alcohol, and where location of death was available, 47.7% occurred in medical facilities.
TAKEAWAY:
- The overall SU+CVD-related AAMR from 1999 to 2019 was 14.3 (95% CI, 14.3-14.3) per 100,000 individuals, with the rate being higher in men (22.5) than in women (6.8) and highest in American Indians or Alaska Natives (37.7) compared with other races/ethnicities.
- Rural areas had higher SU+CVD-related AAMR (15.2; 95% CI, 15.1-15.3) than urban areas, with the District of Columbia having the highest AAMR geographically (25.4), individuals aged 55-69 years having the highest rate agewise (25.1), and alcohol accounting for the highest rate (9.09) among substance types.
- Temporal trends show that the overall SU+CVD-related AAMR increased from 9.9 in 1999 to 21.4 in 2019, a rate that started accelerating in 2012, with an AAPC of 4.0% (95% CI, 3.7-4.3); increases were across all ethnicities and age groups and were particularly pronounced among women (4.8%; 95% CI, 4.5-5.1).
- Cannabis had the highest AAPC of all substances (12.7%), but stimulants had an APC of 21.4 (95% CI, 20.0-22.8) from 2009 to 2019, a period during which stimulants were the fastest-growing substance abuse category.
IN PRACTICE:
These new results identify high-risk groups, which “is crucial for prioritizing preventive measures aiming to reduce substance use and cardiovascular disease-related mortality in these populations,” the researchers wrote.
SOURCE:
Abdul Mannan Khan Minhas, MD, Department of Medicine, University of Mississippi Medical Center, Jackson, Mississippi, and Jakrin Kewcharoen, MD, Division of Cardiology, Loma Linda University Medical Center, Loma Linda, California, were co-first authors of the study, which was published online in the Journal of the American Heart Association.
A version of this article first appeared on Medscape.com.
TOPLINE:
, with the most pronounced rise among women, American Indians, younger people, rural residents, and users of cannabis and psychostimulants, results of new research suggest.
METHODOLOGY:
- From the Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research (CDC WONDER) database and using International Classification of Diseases (ICD) codes, researchers collected data on deaths within the United States where both SU and CVD (SU+CVD) were a contributing or an underlying cause and gathered information on location of death (medical facility, home, hospice, nursing home/long-term care facility), demographics (sex, race/ethnicity, age), and region (urban-rural, state).
- Researchers determined crude and age-adjusted mortality rates (AAMRs) per 100,000 population, identified trends in AAMR using annual percent change (APC) and calculated the weighted average of APCs (AAPCs).
- Between 1999 and 2019, there were 636,572 deaths related to CVD+SU, 75.6% of which were among men and 70.6% among non-Hispanic White individuals, with 65% related to alcohol, and where location of death was available, 47.7% occurred in medical facilities.
TAKEAWAY:
- The overall SU+CVD-related AAMR from 1999 to 2019 was 14.3 (95% CI, 14.3-14.3) per 100,000 individuals, with the rate being higher in men (22.5) than in women (6.8) and highest in American Indians or Alaska Natives (37.7) compared with other races/ethnicities.
- Rural areas had higher SU+CVD-related AAMR (15.2; 95% CI, 15.1-15.3) than urban areas, with the District of Columbia having the highest AAMR geographically (25.4), individuals aged 55-69 years having the highest rate agewise (25.1), and alcohol accounting for the highest rate (9.09) among substance types.
- Temporal trends show that the overall SU+CVD-related AAMR increased from 9.9 in 1999 to 21.4 in 2019, a rate that started accelerating in 2012, with an AAPC of 4.0% (95% CI, 3.7-4.3); increases were across all ethnicities and age groups and were particularly pronounced among women (4.8%; 95% CI, 4.5-5.1).
- Cannabis had the highest AAPC of all substances (12.7%), but stimulants had an APC of 21.4 (95% CI, 20.0-22.8) from 2009 to 2019, a period during which stimulants were the fastest-growing substance abuse category.
IN PRACTICE:
These new results identify high-risk groups, which “is crucial for prioritizing preventive measures aiming to reduce substance use and cardiovascular disease-related mortality in these populations,” the researchers wrote.
SOURCE:
Abdul Mannan Khan Minhas, MD, Department of Medicine, University of Mississippi Medical Center, Jackson, Mississippi, and Jakrin Kewcharoen, MD, Division of Cardiology, Loma Linda University Medical Center, Loma Linda, California, were co-first authors of the study, which was published online in the Journal of the American Heart Association.
A version of this article first appeared on Medscape.com.